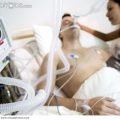
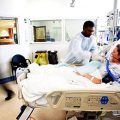
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How Can My Critically Ill Mom Survive Whilst On ECMO & Get Her Out of ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Juan, as part of my 1:1 consulting and advocacy service! Juan’s mom is with a tracheostomy and on ECMO in the ICU. Juan is asking why the ICU team is not giving them any sign that his mom can get off ECMO support.
My Critically Ill Mom is 5 weeks Now in the ICU & the ICU Team is Not Giving Us Any Sign that She can Get Off ECMO Support! Help!
“You can also check out previous 1:1 consulting and advocacy sessions with me and Juan here.”
Juan: They did mention that. Why did they say that we don’t need it?
Kevin: She’s already on the hemofilter.
Juan: Yeah, they said that she’s already on the hemofilter for now.
Patrik: Is she?
Juan: Yes. They re-introduced the hemofilter between yesterday and day before they took out some fluid.
Patrik: Okay. But as of now, she’s not on the filter, is she?
Juan: The hemofilter is still there, yeah.
Patrik: Are they using it?
Juan: Yes.
Patrik: Okay.
Juan: They don’t use it too much.
Patrik: Oh, okay. That’s good.
Juan: Yeah. You remember last week when she had it on, they removed about 6 to 7 liters that she used as she passed three liters. So now it’s much less than that. Yesterday, they removed 500ml, and then today I think a tiny bit maybe, with 10, 20ml an hour or something. So it’s not too much. They have it there. So, yeah I think that they will be seeing if the kidney situation improves now since they most suspected drugs. They want to see if that changes things, and then take a call on what needs to be done.
Patrik: Sure. Okay, well let’s see.
Juan: Yeah, let’s sleep through the night, and tomorrow maybe we’ll see.
Patrik: Yes, absolutely.
Juan: Okay.
Patrik: Okay, all right. Look, let’s reassess tomorrow, or if you need anything just yell out.
Juan: Yes, we’ll do. Thank you Patrik.
Patrik: Thank you so much. All the best for now. Thank you. Bye.
Juan: Thanks, you too. Bye.
Patrik: Bye.
RECOMMENDED:
Patrik: Hi Juan! How are you?
Juan: I’m doing good Patrik. Thank you.
Juan: Patrik, I just have a question, why do most ICU patients develop bleeding in their stomach?
Patrik: Oh okay, I’ll tell you why.
Patrik: I would argue a combination of a number of things. And I’ll tell you why I think it’s a combination of a number of things. So definitely the heparin, as you would have seen, I have highlighted today that INR and aPTT are higher than usual, so that’s definitely a risk. Now, when patients are in ICU, the risk of a GI (gastrointestinal) bleed is reasonably high.
Patrik: I’ll give you a little bit of background there so, and I don’t want to digress too much, but I think it will help you to understand sort of historically. 25 years ago in ICU, no patients were getting any feeds. They were all getting infusions and they had a lot of patients ended up with massive GI bleeds. Then, early feeding was introduced to have the stomach and the gastrointestinal tract working normally, and that reduced the risk of GI bleeds in ICU.
Patrik: The reason there is a high risk of GI bleed in ICU is it’s, it’s a mass… A lot of patients in ICU end up with gastric ulcers because of the stress. So your mom, most likely on top of the heparin, might’ve developed an ulcer, like a stomach ulcer. As part of… it’s unfortunate, it’s part of almost like ICU syndrome. Now you’ve got the added on risk with the heparin and there you go. Now, the other question then for me would be, is she absorbing her feeds?
Juan: Well, no, she’s had some trouble in the last couple of days. The diarrhea, the aspiration, and et cetera. And then last night, she aspirated a bit again, so they’ve been stopping the feeds.
Patrik: Oh, okay, so that’s all goes hand in hand.
Juan: Yeah, and then, so not getting the feed, getting the medication, and the aPTT, INR is going up like all probably combined.
Patrik: I see. I have seen in the pictures that you’ve sent, I have seen that they’ve reduced the heparin.
Juan: Yes.
Patrik: I have seen that. The other thing that doesn’t quite make sense to me is aPTT and INR are often independent of each other. It’s not, sometimes you have aPTT high and INR low and vice versa. In this situation both are high, not sure why. It’s clear why the aPTT is high because of the heparin. It’s unclear to me why INR would be high.
Recommended links:
Juan: Can you tell us, at least me, I don’t know if I’ve followed the show of it, can you explain a little bit more about, I mean, I read up about what aPTT is and I read up what INR is, but can you just explain that to me a little bit?
Patrik: So aPTT is a clotting factor.
Juan: Yeah.
Patrik: And the way… a normal aPTT, if they check an aPTT on you and we are assuming that our clotting is intact would be in a range, I believe between 30 to 40. INR is another clotting factor. Basically aPTT is, it measures how long it takes the blood to form a clot.
Juan: Yeah.
Patrik: So therefore, the heparin obviously delays that. Delays for the blood to form a clot. And it’s the same for INR, it’s also a measure to see how long it takes for the blood to form a clot. Now, the difference with aPTT and INR is, you give heparin and aPTT usually is getting higher, INR you give warfarin. Have you heard of warfarin?
Juan: No.
Patrik: Warfarin is a blood thinner that can only be given via tablets. And usually it’s not… it’s sparingly used in ICU. Warfarin, it can be used in ICU but it’s sparingly used because you can only give it as a tablet, unlike heparin, it’s not an infusion. And you’ll give warfarin and your INR goes up. In this situation, your mom, as far as I’m aware, did not have any warfarin, then why is her INR going up?
Juan: She is on Ecosprin.
Patrik: Say again?
Juan: She’s on Brilinta and Ecosprin.
Patrik: Brilinta.
Kevin: Anti-platelet medication.
Patrik: Oh, Ticagrelor, okay yes, Ticagrelor. So, she’s on that on top of the heparin?
Kevin: Yes and Ecosprin as well.
Patrik: I see, wow, that’s probably why INR is high. No surprise there then. Well, on top of her starting on pantoprazole, are they stopping the Brilinta?
Juan: No one mentioned anything about it
Kevin: They only said they can’t stop the Brilinta because of the recent stenting.
Patrik: Yes, that would be correct. Have they…are they going to do a gastroscopy because of the GI bleed?
Juan: We’re going to find out now, I think they are all probably just seeing her and figuring out what they want to do.
Suggested links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Patrik: They would probably do a gastroscopy most likely.
Juan: Can I ask you Patrik, so if her INR and aPTT is going up, and that means that her blood is taking longer to clot.
Patrik: Correct.
Juan: Then does she need so much? Can they reduce the Brilinta, Ecospirin, and Heparin?
Patrik: Possibly, I would argue with that, with the stent, they can’t reduce the anti-platelet medication. With the Heparin, so they have to weigh up what’s their target range for the aPTT. So please ask them what’s their target range for the aPTT. And that target range would probably, I would think, that the target range would probably be somewhere between 50 and 60, but please ask them what it is.
Patrik: Now, what I’ve seen is that in case of a GI bleed or any bleed for that matter, they would decrease the target rate for the aPTT, temporarily. However, the risk of then her potentially having a clot is also there.
Juan: But, sorry, this is just a general question. So if her blood is doing… like if she doesn’t need that much of the Heparin…. so if her aPTT is high then isn’t the risk of clotting less?
Patrik: Yes and no. The reason she needs a higher aPTT is the risk of a blood clot, while she’s on ECMO is very high. And the reason for that is, so when you look at the ECMO machine, it runs through a filter, so the risks that the clot will form in the filter is high. If a clot forms in the filter, the risk of a clot going from the filter into the body and causing a PE (pulmonary embolism) is real, or causing a stroke is real. On top of that, because the blood is running through plastic tubes, the risk of a clot to form in a plastic tube is real.
Recommended:
Juan: Right, so it’s not that it would form in her body..
Patrik: Correct. The other thing that to a degree doesn’t surprise me, the longer someone is in ICU, again, given how sick your mom is, the risk for a long stay in such a critical condition, to have a bleed is real.
Juan: So, is not for the ICU, this is manageable? Is this like, what is what?
Patrik: So it’s definitely manageable. But think about it, so they started Pantoprazole infusion, they would stop the feeds at least for a little while, or reduce the rate, so she will get less nutrition. The other thing she will need, they probably would have checked the hemoglobin now.
Juan: Yeah, she’s getting a blood transfusion right now.
Patrik: Right, so she really develop blood transfusion. Her kidneys are already impaired. She needs the blood transfusion, but her kidneys are impacted. So it’s a catch, it’s a catch-22, she doesn’t need another complication at the moment.
Juan: Yeah. So what do you think the next steps will be?
Patrik: Well, next steps are pantoprazole infusion, a unit of blood, stop the feeds or reduce them to a degree where she can tolerate the feeds. If for whatever reason she can’t tolerate the feeds, she still needs nutrition, and then she would need TPN. Have you heard of TPN?
Recommended:
Juan: No.
Patrik: TPN is basically intravenous nutrition. What it is from my experience, it’s a clear stress response. I would argue the next step is to do a gastroscopy. Basically, putting a camera down your mom’s esophagus into the stomach, because what could happen is, she’s probably got an ulcer in her stomach and maybe they can close that ulcer once they’re going down with the camera, there are methods to do that.
Juan: Okay, we’ll discuss with them.
Patrik: You’ll discuss with them. And the x-ray today, I couldn’t see a lot of improvement, probably its fairly similar to the one yesterday.
Juan: Yeah.
Patrik: Have you seen your mom today?
Juan: Yes. She’s looking better.
Patrik: Okay.
Juan: She looks brighter. She’s looking, the edema has reduced definitely from yesterday. Yeah, she was just looking better.
Patrik: That’s good and when did they…
Juan: In the last couple of days as well, so I think, she’s just looking like she’s flashing up.
Patrik: Yeah. And are they giving you any sign that they can reduce ECMO support? Are they giving you any hope there?
Juan: I think we’re going to talk to them now, so they we’re getting the EEG now. As I told you the last two, just seemed a bit more, almost like it didn’t change. So we’re just waiting to see, I think these couple of complications have come in, but essentially the downs on this side are holding steady. It’s not that they are impacted and BP and heart rate has been okay. So I mean, we’ll speak to, I think the doctors are all looking at her right now.
Patrik: Sure, sure. If she’s not absorbing feeds, the other thing they could look at is medications such as Metoclopramide. I will send that to you in a text, as well as Erythromycin. I’ll text that to you. Metoclopramide also known as Maxolon, and the other one is Erythromycin. But she is passing stools isn’t she?
Juan: Yeah. It was liquid, not fully solid, but she has pass.
Patrik: It’s kind of a bit, so it’s really upper GI tract because if she start… she must be must’ve digested some food, otherwise she wouldn’t open her bowels.
Juan: Yeah.
Patrik: But then obviously upper GI tract, she’s not absorbing at the moment.
Juan: So, what does, I mean, is that the same then? The ulcer you think?
Patrik: Possibly.
Juan: Possibly.
Patrik: Ask them, are they considering a gastroscopy as a next step? But then again, if you do a gastroscopy, the risk is because she’s already…
Juan: Yeah, the one in the upper GI tract,
Patrik: Correct and she’s already at risk of bleeding.
Juan: Yeah, okay. I think the gastroenterologist is going to see her now as well.
Patrik: Oh good.
Suggested links:
Juan: They’re all just thinking and then they decide, I think, who will give us the consolidated update.
Patrik: Yeah, so it’s certainly very concerning, hopefully the pantoprazole will work.
Juan: So how does the pantoprazole work to solve this issue?
Patrik: Yep, so what happens when someone has a bleed, or prior to the bleed they often have an ulcer, and when they have an ulcer, basically what that means is the pH in the stomach, it gets very acidic. The pantoprazole is a proton pump inhibitor, which is basically a fancy name for saying it stops the stomach environment to produce more acid.
Juan: Okay, and how do these ulcers form usually?
Patrik: Oh, they form over time I mean, it’s not that just an ulcer pops up. It’s again, probably a stress response over many days or many weeks.
Juan: Okay.
Patrik: I think the gastroenterologist should have a point of view.
Juan: Yeah, I think I can see when, and she’s really nice. So I guess she…
Patrik: Right, but it is, it’s probably not helping, that plate is not helping her to get off ECMO at the moment, I would argue. Even though it’s a separate organ, it’s got nothing to do with the lungs, but it is sort of a complication you don’t want for anyone.
Juan: Yeah. Okay.
Patrik: Did this happen while you were there visiting her? Or did this happened…
Juan: We were just told right now. We’re not there.
Patrik: So how did they find out? Did they aspirate from…
Juan: We’re going to find out.
Patrik: Right. Yesterday I thought the Noradrenaline was very close to coming off completely. I would think… pardon?
Kevin: What happened was she passed 3 stools, 2 yesterday and 1 tonight. So there could what they said is a BP been a bit low could be as a result of that. A lot of fluid or extra fluid coming up.
Patrik: I think the next step is to talk to the gastroenterologist and see what they want to do as a next step.
RECOMMENDED:
Juan: Yeah we’ll speak to them. Anything else you want to say?
Patrik: Not that I can think of. The sooner they can start feeding her, the better.
Juan: Yeah, okay we’ll talk to them.
Patrik: I’m sure they know that, but the more you can go to natural feeding the better.
Juan: Yeah, I think it’s just, I guess that’s the ICU, and there’s been a combination of things. The morphine was preventing her from digesting the food. Then you have the stress, then you have the antibiotics, then you have the stomach ulcer, and one thing lead to another.
Patrik: One thing leading to another.
Juan: Okay. All right, we’ll speak to them and then we will just give you an update.
Patrik: Please, yes.
Juan: Okay. Thank you so much.
Patrik: Thank you so much, thank you. Bye, bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!