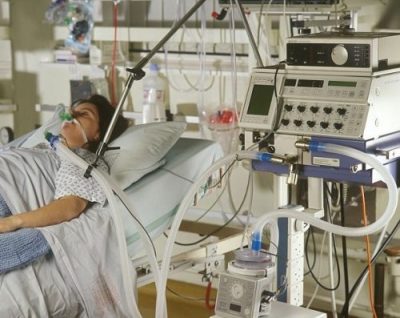
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives of Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How Long Will My Critically Ill Mom Need To Be on Life Support & Remain Sedated in the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to share this consulting session from one of my clients Juan, as part of my 1:1 consulting and advocacy service! Juan’s mom is with a tracheostomy, balloon pump, and is now on VV- ECMO. Juan is thanking Patrik for helping them to move one step forward towards the recovery of their critically ill mom in the ICU.
Thank you for Helping us Patrik to Move One Step Forward Towards the Recovery of our Critically Ill Mom in the ICU!
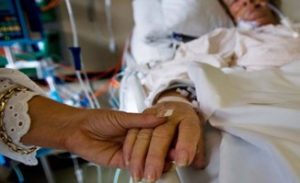
“You can also check out previous 1:1 consulting and advocacy sessions with me and Juan here.”
Juan: She moves her head. She tries to shrug her shoulders occasionally. When she’s trying to lift off her head, sometimes. She moves her tongue in her mouth a lot. A lot because you can definitely see her trying a lot to talk. She keeps trying to move her lips from left to right up and down, try and stretch her mouth. It seems like she really wants to clean her mouth and say a lot. Basically.
Patrik: Yeah. Okay.
Juan: That’s the most of it. She’s not moving her body much.
Patrik: Right. Okay. Fair enough. That’s probably a concern that she’s not moving enough yet, but hopefully that’ll come.
Juan: They’re doing some passive movements for her arms, no, for the last two days.
Patrik: Yeah.
Juan: I think that’s all why they don’t want to use the paralytics and the sedatives too much anymore. Yeah.
Patrik: Yeah. It’s terrible. It’s terrible.
Juan: Yeah.
Patrik: But I mean, there have been so many good things happening in the last few days.
Juan: Yeah, yeah.
Patrik: It’s been very, very positive seeing what’s been unfolding.
RECOMMENDED:
Juan: Yeah.
Juan: Patrik, I know it’s a big question, but I know the muscle degradation and the movement gets severely impacted. I mean, I’ve read a lot about it, so I understand that after the first couple of days, even for a normal patient, it starts to be quite rapid, the muscle degradation and then she’s on maximum support of all types, right? Maximum sedation, maximum life support. So I understand it’s quite… She’s in the most extreme situation.
Patrik: Yes, she is.
Juan: How much can we help her in terms of when we get there? Once VV is off?
Patrik: Yeah. Great question.
Juan: Once the ventilator is off?
Patrik: Yeah. So one obstacle for your mom at the moment is definitely ECMO, because if she was, “only on the ventilator without ECMO”, they could start with some physical therapy.
Juan: They told me today that she can be on the VV and still do..
Patrik: Okay.
Juan: Can’t they do some stuff, even if she’s on VV? I don’t know. Maybe.
Patrik: I would say no.
Juan: Okay.
Patrik: Simply because the risk of the cannulas moving and shifting-
Kevin: Being displaced.
Patrik: Yeah, yeah. It’s just too high.
Juan: Yeah.
Patrik: I’m all for the physical therapy as quickly as possible. I’m all for that.
Juan: Yeah, yeah.
Patrik: With VV ECMO or with any ECMO, the risk of the cannulas being dislodged, it’s simply too high.
Recommended:
Juan: I think. Yeah.
Patrik: That could cost your mom’s life. Really.
Juan: Right, right.
Patrik: The minute she’s off ECMO, they can start with some passive movements, but at the moment I’d say the best you can probably do for your mom is move her joints in terms of… But only her foot and her hands.
Juan: Okay.
Patrik: Right. That’s probably as far as you can go at the moment.
Juan: Okay. I understand. Okay.
Patrik: But I mean, if you’re looking at the positives, your mom is alive, she’s managed to get rid of VA ECMO, and hopefully she can manage to get off VV ECMO.
Juan: Yeah.
Patrik: And then only then can you take the next steps.
Juan: I understand.
Patrik: My advice for anyone in a situation like that is one day at the time.
Suggested links:
Juan: Yeah. I guess it’s just a… You understand better than anyone else, just the tradeoff between each day that you’re on the support and with the sedation and with all of it, you start counting the costs of later, but yes, I understand. She’s making big strides.
Patrik: Look, your mom may come out of this with her brain intact with her body not being able to move. Now that’s not to say she can’t learn that again, but that might be the price she’s paying for survival. I should send you an interview that I’ve done with a gentleman a few years ago, Charlie Atkinson in America, very interesting character. He was on a ventilator for over a year. And it’s not that he was on ECMO and anything, but ventilator, tracheostomy the whole nine years and he had to relearn to walk, move. He’s quite an inspirational guy. Charlie would be now 85. And he’s still alive.
Juan: Okay.
Patrik: He’s an amazing guy. He’s got a Facebook page, where he documents his progress. The examples are out there where people recover and live and are very happy to be alive but it certainly will take time.
Juan: Yeah, yeah, no, I understand. One day at a time.
Patrik: One day at a time. That’s the best advice I can give you, as much as everybody wants to speed up things, of course, I see you as a marathon, not a sprint.
Juan: Yeah, no, I can see that.
Recommended:
Patrik: But the examples are out there that people can come out of this, not necessarily the same than they were before and recovery will take time, but I guess if you asked Charlie, he wants to be here.
Juan: Yeah, yeah, no, absolutely.
Patrik: So yeah. I’m pretty sure she will have a long road ahead.
Juan: Yeah.
Patrik: But it’s probably worth keeping at it.
Juan: Definitely.
Patrik: I’ll send you, while we’re talking, I’ll send you a link to this podcast, to this interview that I’ve done with Charlie, because I think it’ll help you just listening to him, what he’s been through. And I think it’ll help you to put things in perspective.
Juan: Sure, sure. No, I’ll listen to it today.
Patrik: But, overall, I mean, it’s a waiting game and it’s… Yeah, it’s very much a waiting game with still an uncertain outcome, but the signs are there that she hopefully can turn the corner.
Juan: Yeah. Yeah. Okay. So we’ll keep you posted, we’ll give you another update, this evening, tonight as well.
Patrik: Yeah, please, please. It’s been very positive so far. And the only other thing that I want to advise you on is, it’s often two steps forward one step back. So, so far it’s been forward really, since we started working together. So I wouldn’t be surprised if there will be some setbacks for your mom. So just be prepared for that. It’s often two steps forward. One step back.
Juan: Yeah. The week when we reached out to you, we had a lot of that, which is why we reached out to you. So strangely, when we started talking to you, it seemed to almost only be the steps one step forward at a time, but actually we reached out to you because we dealt with a whole week of one step forward, two steps back.
Patrik: Right.
Juan: Yeah.
Suggested links:
Patrik: Right. I see. If I may ask, how did you find out about the Intensive Care Hotline?
Kevin: I was just doing some research online and I came across your videos on YouTube.
Patrik: Okay.
Kevin: I watched a couple of them and I was like, “Yeah, we should definitely reach out to you.”
Juan: I mean, throughout this year we’ve been doing a lot of research and looking up a lot of different perspectives just because everything has been so… It’s been difficult to access reliable information about health and medicine and what’s happening and yeah, just, we’ve been looking for people. So yeah. I guess we stumbled upon you at the right time.
Patrik: Right. That’s interesting. Yes. And I guess, everybody has a different opinion about what’s happening with health at the moment with COVID and yeah. I think there’s so many different opinions out there. Who do you trust?
Juan: Yeah, it’s been challenging. It’s been challenging. It’s been really nice because we’ve connected with so many people around the world through the year and pretty much all of them are advising us in different ways, in different capacities right now. And it’s been very collaborative and really helpful.
Patrik: That’s good. No, that’s really good. It’s strange times. Very challenging times, but COVID..
Juan: Yeah, yeah. How are things where you are? Is your family okay? Are you okay?
Patrik: Yeah, no, we are all okay. Thank you. I appreciate that. No, we’re all okay. We are in a lockdown at the moment. I’m in Melbourne, in Australia. We are in a lockdown at the moment, but it’s… Our numbers here in Australia have been very low compared to the rest of the world. That didn’t stop us from… Or that didn’t stop the government from locking down Sydney and Melbourne.
Juan: Yeah. It has quite a strict lockdown, right?
Patrik: Yeah, very strict. Very strict.
Juan: No one entering or leaving the country.
Suggested links:
Patrik: Very strict. Well, apparently one of the strictest lockdowns in the world, apparently. We are back in lockdown at the moment, but I think people are taking it less and less serious and people are sick of the government telling them what to do.
Juan: Absolutely. I think that’s everywhere. That’s here as well.
Patrik: What’s it like there at the moment with COVID?
Juan: I mean, the government… We had one of the longest lockdowns, so one of the most serious and long lockdowns. For most of last year, and then this year it’s been on, off, on, off. In general because we’re such a populated country. You can’t actually lock people down. I think it’s mostly for media coverage and international, it’s more perception than reality. Of course, restaurants and businesses are forced to close whenever the government wants them to, but because they will just come and get harassed or fined, but by and large in villages and in populated areas, people are just carrying on life as normal, wherever they can. It’s more the educated classes that listen to the rules and the uneducated listen best, which is probably a good thing because for them it’s survival. We’ve lost way more lives because of lockdown than there is because of COVID or many other diseases as well. Hunger and poverty kills a lot of people.
Patrik: Yes.
Juan: So, pretty much… Yeah, it’s a strange situation for sure. There’s more and more anger brewing as well here because priorities just are all skewed because I think people are losing complete faith in the media and the government now.
Patrik: Yes. Very much so.
Juan: Yeah.
Patrik: Last year, we were in a lock down about a year ago and you could hardly see anyone on the streets. Whereas now we are back in that same lockdown with the same rules and regulations and there’s people everywhere.
Juan: Yeah. It’s similar here. It’s similar here. And from what we can see, it’s similar in many other parts of the world as well.
Patrik: You can’t stop life. I mean, it’s just not… People need to earn a living.
Juan: Yeah.
Patrik: It’s just not feasible.
Juan: And I think fear of disease is often worse than the disease itself. I think people are getting really, really scared is not healthy for them either.
Patrik: No, no. I can tell you that. I haven’t worked in ICU for a few years now, so it’s pretty much all I’m doing now is helping families and stuff. But the last time ICU that I worked at here in Melbourne, they had the majority of COVID patients in that particular ICU, not one staff member there, not one got infected.
Juan: Yeah, yeah, yeah. It seems similar here.
Patrik: And that was before the vaccine. That was before the vaccine.
Juan: And after?
Patrik: They wouldn’t have any COVID cases there at the moment, maybe one or two.
Juan: Right.
Patrik: So, given that they had up to 20 in that unit last year and nobody got infected, so at the moment, if they have one or two. And the majority of staff now would be vaccinated. It could be insignificant, I would argue.
Juan: Yeah, yeah, yeah.
Patrik: That goes to show to me that as long as you are doing all the right things, nothing’s going to happen.
Juan: Absolutely. I mean, when my mom was ill, there are a whole bunch of people in our house, we have kids, we have elder people, we have a lot of people, and no one else got sick, no one else got sick.
Patrik: Right.
Juan: It was my mom and everyone was looking after her and we all were together. There wasn’t really any question of isolating from each other because we all needed to help her and, I mean, everyone is fine. We’ve been coming to the hospital. I was staying in the hospital, me and my sibling, my dad comes occasionally and visits. And we’ve, touch wood, been fine including her, so.
Patrik: Right.
Recommended:
Juan: Yeah. I guess it also really depends on for mobility and your innate health as well.
Patrik: Of course. Of course. And surely that nobody is immune to COVID of course, but it really comes down to simple things like washing hands and…
Juan: Eating well.
Patrik: Eating well.
Juan: Being healthy, exercising.
Patrik: Yeah. Exactly, common sense.
Juan: Yeah. Common sense, which is lacking these days.
Patrik: Common sense. Very much lacking. So anyway, COVID will pass. We don’t know when, but it will pass eventually.
Juan: Yeah.
Patrik: It’ll probably be just like a common cold eventually.
Juan: Yeah. Yeah. I hope the COVID is like a common cold and passes as well. Let’s see.
Patrik: Same here. Same here. They’re destroying small businesses.
Juan: Yeah. Absolutely.
Patrik: And it’s terrible.
Juan: They’re making a lot of money and they’re enhancing their control. There’s a lot of that going on which I think is starting to annoy people a lot.
Patrik: Oh, yeah. Yeah, absolutely. So we will see.
RECOMMENDED:
Juan: We will get through it.
Patrik: Oh yeah, of course. Of course. It’s like when I think about it, my grandparents and I don’t know about you, but my grandparents they’ve been through world war two, some of them through world war one, I just go like, “Okay, well, COVID, won’t kill us.”
Juan: Yeah. No, definitely. Definitely. Okay. I’ll give you an update this evening.
Patrik: Very nice to talk to you. Yeah, yeah.
Juan: Patrik, what time do you go to sleep?
Patrik: So, for me, at the moment, it’s 9:30 PM, but if you need to talk, I won’t be going to sleep before midnight.
Juan: Okay.
Patrik: And even if you need something after midnight, if it’s urgent, you just call me.
Juan: Okay. All right. Will do.
Patrik: Okay.
Juan: Okay. Thank you.
Patrik: Thank you so much. Thank you. Bye-bye. Bye.
Kevin: Bye.
Juan: Bye, Patrik.
Kevin: Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!