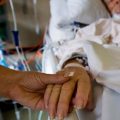
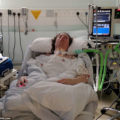
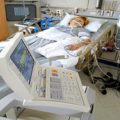
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How Can the ICU Team Start Weaning my Critically Ill Mom with COVID from ECMO in the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Juan, as part of my 1:1 consulting and advocacy service! Juan’s mom is with a tracheostomy, balloon pump, and is on ECMO. Juan is asking how they will know if their mom is ready to be weaned off ECMO.
How Do We Know If Our Critically Ill Mom in ICU Is Ready To Be Weaned Off ECMO?
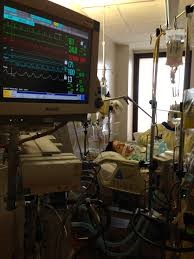
“You can also check out previous 1:1 consulting and advocacy sessions with me and Juan here.”
Juan: The PA catheter, when do they plan to remove it? Because the risk of infections. Question them about the weaning studies and get the results of that. You’ve mentioned a regular sinus rhythm. I don’t have any point to discuss. There was potassium being low. I think that’s what we have to discuss too.
Patrik: Yeah.
Juan: Third spacing could be because of the low albumin and the fluid overload. Are they managing sodium?
Patrik: Yeah. And how are they managing it? Because one way to manage a high sodium is to give water.
Juan: But that’s not something that they want to do-
Patrik: No, no.
Patrik: Definitely not.
Juan: Right. And then the pulmonary hypertension. Are they doing any kind of nebulization?
Patrik: So when I talk about pulmonary hypertension, there’s a few treatment options for pulmonary hypertension. And again, I will text that to you. For pulmonary hypertension, you can use a medication called sildenafil, which is also known as Viagra. So I’ll just quickly text you that. Viagra/sildenafil.
RECOMMENDED:
Juan: Is that what they nebulize?
Patrik: No, no, no. It’s no nebulization. Another medication that I have seen used for… Is your mom in ARDS?
Michelle: Respiratory distress syndrome. I don’t know. We’ll have to ask-
Juan: We’ll have to ask them.
Michelle: I will assume that she is. I will assume.
Patrik: Okay. I would assume so too.
Michelle: Yeah.
Patrik: In this journey, do you know whether she was ever on nitric oxide?
Juan: I don’t think she was.
Patrik: Okay. The most common drug for pulmonary hypertension is sildenafil or Viagra, but it can only be given as a tablet.
Juan: Okay. You mentioned the nitric oxide.
Patrik: Yeah. Given that she has now pulmonary fibrosis, might be too late for that, but again, you might ask.
Juan: Okay.
Patrik: Right. And definitely Epoprostenol. I’ve just texted that to you.
Juan: Okay. Okay.
Patrik: And you should be asking that too.
Juan: Sure.
Patrik: I should say Epoprostenol is a nebulizer. I should say that.
Juan: Okay.
Patrik: Epoprostenol is a nebulizer.
Juan: Okay.
Patrik: Go on.
Juan: No you can go ahead. I was just going to go to my next point that I had written down.
Patrik: No. No, please, what was your next point?
Juan: Do you think nutrition isn’t a primary issue right now.
Patrik: As long as she’s getting nutrition, you can always maximize nutrition, always. Of course you can, but it’s a dietician issue.
Juan: Okay.
Patrik: Look, not getting nutrition in ICU would be very fundamental to your mom’s recovery.
Recommended links:
Juan: She’s getting nutrition. I think that she is being… But yeah, we’ll keep that in mind and keep a regular check on it.
Patrik: That’s right. And as long as she’s absorbing her feeds, that’s all very positive.
Juan: Great. And then I have a note about when they gave the Cordarone for the atrial fibrillation.
Patrik: Correct.
Juan: Was the potassium level not being managed, and how are they managing potassium and magnesium now? Correct?
Patrik: Correct. Very much so. Very much so.
Juan: Okay. And then kind of we ask them about this roadmap exactly. The VA-ECMO, the balloon pump, the VA VV-ECMO and then what? The ventilator and kind of how they plan to proceed.
Patrik: Yeah. It’s all about the roadmap.
Suggested links:
Juan: I think that was also the intention of giving us those three options the other day. Kind of saying that, “Yes, we want to move the VA, but in order to do that, we stop with the IABP. If that doesn’t work, then the Impella, then the transplant.”
Patrik: Yeah.
Juan: Yeah. I think that’s sort of what they wanted to put out.
Patrik: Look, very rarely. If they start with the Impella, very rarely has an Impella been implanted and not working towards a transplant.
Juan: Okay. Okay. Yeah, that wasn’t mentioned, but it’s good to know. So we know that.
Patrik: Right. So the-
Juan: Can I ask, Patrik?
Patrik: Please.
Juan: With the IABP, or with the VA and the IABP, with what’s happening right now, how do we know if this is working enough to just then remove this? Or if we need to go and look at those other options?
Recommended:
Patrik: Cardiac-
Juan: I think I’m a little.
Patrik: Cardiac output. Cardiac output.
Juan: Cardiac output? Okay.
Patrik: Cardiac output will be important for you to keep an eye on.
Juan: Yeah.
Patrik: Okay.
Juan: And how quickly can Cardiac output improve?
Patrik: Fairly quickly, fairly quickly. I would argue that if you start her on Milrinone or Dobutamine, I would argue that her cardiac output could improve fairly quickly.
Juan: Is there anything that they might say about why they don’t want to use Milrinone or Dobutamine?
Patrik: That’s a missing link to me. I can’t see why they can’t use it. I can’t see it at the moment, but that’s a missing link to me. I have seen very few patients on VA-ECMO without being supported by Dobutamine or Milrinone. Very few patients that I’ve seen. I don’t understand-
Juan: So it’s standard practice?
Patrik: Yes. Yes. I would say it’s standard practice. I don’t understand why they’re not using it.
Juan: I guess because they were using vasopressin and noradrenaline, so they-
Patrik: Different classification of inotropes.
Juan: Okay. Different classification-
Patrik: Absolutely. The vasopressin and the noradrenaline are vasoconstrictors. They don’t have a direct impact on the heart. It’s an indirect impact on the heart. Whereas the-
Juan: These are direct for cardiac output.
Patrik: Correct. Dobutamine and Milrinone are directly working on the contractility of the heart.
Juan: Understood. Okay. We will bring that up tonight itself. We’re on-
Patrik: Correct.
Juan: And then the last point I have is to try and take Atracurium off ASAP. Can they increase Midazolam and Fentanyl to get rid of the Atracurium, or adding propofol to get rid of it or use Precedex clonidine.
Patrik: Very much so. Very much so. Yeah.
Juan: Okay. Excellent. These are great points. Anything that I missed?
Patrik: No, I don’t think so. One of my concerns in all of these, I mean, obviously the situation is very difficult, but one of my concerns is again, with all the lines, whether it’s the balloon pump, whether it’s the central line, whether it’s the PA catheter, infection risk.
Juan: Yeah, so getting the lines out as well-
Patrik: Getting the lines out.
Juan: with the machines coming off, I imagine, right?
Patrik: Yeah, absolutely. Absolutely.
Juan: Do you think that if they take the PA catheter out, is it safe now? Do they need it?
Patrik: I would argue that the weaning study can be done without the PA catheter. And the reason I’m saying that weaning study can be done without a PA catheter is, if they do the ECHO while they’re trying to wean her, that should give them enough information. They check the cardiac output with the ultrasound. It’s less invasive.
Juan: Yeah.
Patrik: Right? It doesn’t really have any infection rates. The advantage with a PA catheter is, the nurses can check the cardiac output. Whereas with an ultrasound, only the doctors can do it.
Juan: Got it. Yeah. Yeah. Yeah.
Recommended:
Patrik: But the infection risk with the PA catheter is high.
Juan: So they could try and get that out the earliest as well.
Patrik: That’s right. That’s right.
Juan: Okay. Any other lines we should see if they can get out ASAP or… I mean, they’re just-
RECOMMENDED:
Patrik: She’s got a central line and she’s got an arterial line, but I’m probably not worried about them with all the other major lines. She will need a central line for some time to come. She will an arterial line for some time to come. So-
Juan: So it’s safer than the other ones. Yeah.
Patrik: That’s right.
Juan: Okay. Okay. Thank you, Patrik. We’ll have this conversation and we’ll let you know how it goes and…
Patrik: Yes.
Juan: Let’s have another conversation maybe tomorrow or next week.
Patrik: Yeah, sure. Sure, sure.
Juan: Okay. Thank you very much.
Patrik: Oh, pleasure.
Michelle: Thank you.
Patrik: Oh, pleasure. You’re very welcome. Wish you all the best for now.
Juan: Thank you.
Kevin: Thank you.
Patrik: Thank you. Bye-bye. Thank you. Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!