Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
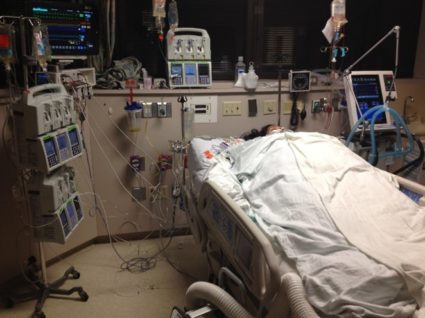
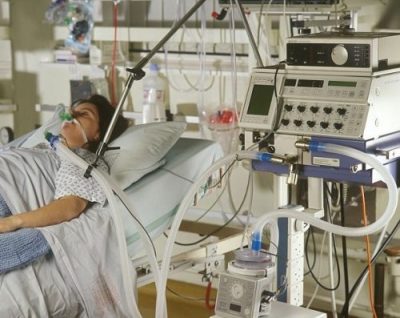
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Juan, as part of my 1:1 consulting and advocacy service! Juan’s mom is with a tracheostomy, balloon pump, and is now on VV- ECMO. John asks how his mom can prevent withdrawal symptoms or ICU psychosis after being in an induced coma.
How Can My Mom Prevent Withdrawal Symptoms or ICU Psychosis after Being in an Induced Coma?
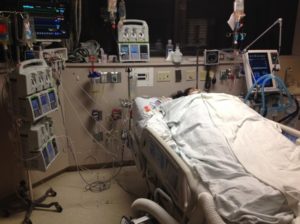
“You can also check out previous 1:1 consulting and advocacy sessions with me and Juan here.”
Juan: Patrik, how long will it take her to learn how to speak again? Once we remove the trache tube.
Patrik: Okay. Great question. So as soon as she’s off the ventilator or let’s put it that way, as soon as she can have time off the ventilator and she’s strong enough, they might try a speaking valve.
Kevin: What’s that again?
Patrik: Yeah. So when someone has a tracheostomy and has time off the ventilator, so just because someone has a tracheostomy doesn’t mean they need a ventilator all the time.
Kevin: Right.
Patrik: Okay. So let’s just say she’s coming to a point where she needs the ventilator only intermittently.
Patrik: And if she’s strong enough, they can trial a speaking valve.
Kevin: What is that?
Patrik: Yeah. So basically when you take off the ventilator of a trache, you could attach the speaking valve and then you have to deflate the tracheostomy cuff, and then you can do speaking exercises.
Kevin: Ah, okay okay.
Patrik: But I think she’s a long time away from that at the moment.
RECOMMENDED:
Kevin: Right, right, right. Okay.
Patrik: So those would be the next steps. So there is a very good chance, if all progresses as we think it’s progressing, that the speech therapies would be doing speaking exercises with her.
Kevin: Great. Okay Patrik, I have two questions. One was, since she’s been on the Midazolam and the Atracurium for quite some time now, lingering or after effects would essentially still be there. So how does that play out?
Patrik: Yeah. Great, great question. So my biggest concern with the Atracurium is that… Okay. When someone is in ICU, in an induced coma without Atracurium, deconditioning of the body happens very fast, and is real. So when then patients wake up from an induced coma, they are deconditioned, and their muscles are very weak and so forth.
Patrik: So now, on top of that, you’re having the Atracurium, which is a muscle relaxant, a paralyzing agent. So the deconditioning is even worse. I’ll come to the Midazolam in a moment, but let me ask you one question, is your mom moving at the moment? Is she moving arms, legs?
Kevin: No, no. She’s not able to move anything.
Patrik: Right. And that’s part of the deconditioning process.
Kevin: Right.
Recommended:
Patrik: So-
Kevin: I sense that there’s probably quite a lot of severe muscle weakness.
Patrik: Correct, correct.
Kevin: Or myopathy, or-
Patrik: Yes, cardio, it’s… Yes, absolutely. So it’s myopathy. So that’s my concern with the Atracurium, that it should be used sparingly and only temporarily, but it sounds to me like she’s been having that consistently for the last couple of weeks, is that right?
Kevin: Yeah. Stopped it two days ago.
Patrik: Right. Okay. So that’s my concern with anyone in an induced coma, even without the Atracurium. The Atracurium is just making it worse. But she needed the Atracurium, obviously, she needed the Atracurium to be able to not fight against the ventilator. And making sure she’s not pulling out her ECMO tubes.
Kevin: Exactly.
Patrik: Right. So I know there are situations where you need the Atracurium, I’m well aware of that.
Patrik: Coming to the Midazolam, as well as the Fentanyl. So here are the disadvantages with Fentanyl and Midazolam. Both are addictive in nature. So that means when someone has been on high doses of Midazolam and Fentanyl for many weeks, they might be going through withdrawal.
Kevin: Right.
Juan: And what does that manifest like? When the withdrawal is-
Patrik: Yes. Yes. So withdrawal symptoms can manifest like an agitation, confusion, sweat, shaking, even as bad as seizures. You got to watch for that. How long has she been off the Midazolam now?
Suggested links:
Kevin: They stopped Midazolam yesterday. A couple days before-
Juan: No, on Saturday.
Kevin: Oh, on Saturday, sorry.
Juan: Today is Tuesday.
Kevin: So four days ago.
Patrik: And would you say, when you see her, there are any withdrawal symptoms?
Juan: I mean…
Kevin: She seems a bit confused. Like she moves her tongue a lot.
Juan: She’s looking blankly up into space. I don’t know if she can see or not. It doesn’t seem like she can see properly.
Patrik: Right, fair enough. Look-
Juan: She does seem a little agitated. I mean, naturally she looks a bit scared all the time, but I can’t tell if that’s normal or not.
Patrik: Right. Okay. Fair enough. Fair enough. One thing that might counteract withdrawal already is the dexmedetomidine, the Precedex. And I’ll tell you why. So dexmedetomidine or Precedex is, half of what’s in there is clonidine.
Patrik: And when someone is going through withdrawal in ICU from either Fentanyl, Morphine, or Midazolam, sometimes also Ketamine, you can counteract that with Clonidine. And given that clonidine is part of the Precedex, it might-
Kevin: Help.
Patrik: Help. It might, but it’s also a low dose of Precedex, from what I’ve seen.
Kevin: Right, right.
Patrik: You know, other symptoms when people are going through withdrawal is for example, high heart rate, low blood pressure, high blood pressure, anything. Anything you can imagine when people go through withdrawal.
Kevin: Yeah, her heart rate goes high when she’s awake.
Patrik: Right. How many weeks has she been on Midazolam for?
Kevin: Easily four weeks.
Patrik: My goodness. And how much?
Juan: It’s been varying amounts, honestly.
Kevin: Varying. From like six to five to four.
Patrik: Right. Okay. But for four weeks.
Recommended:
Kevin: Yeah.
Juan: Would you say it’s been throughout the four weeks?
Kevin: Yeah, I would say in between maybe like a couple of days it’s not there, where they only use Fentanyl and Atracurium, or they only use Fentanyl and Midazolam, and not Atracurium. So, I mean, I would give it about three and a half, four weeks.
Patrik: Yeah. But Fentanyl is just as bad. Fentanyl is very addictive in nature too.
Kevin: Yeah.
Patrik: Right. And what you will find that, you know what, I’ll tell you what you will probably find going forward. Assuming your mom will come out of this, you will probably find that she will be very confused and agitated for quite some time to come.
Patrik: It’s part of, have you heard of ICU delirium or ICU psychosis? Have you heard of that?
Suggested links:
Kevin: Yes. We did. And they’ve recommended Olanzapine for that.
Patrik: Yeah. Yeah. Look, I’ll tell you what I think about Olanzapine. I have seen it used for ICU psychosis. I’m not… I know it’s standard in ICU to use it. I’m not a big friend of it. Because I think it’s doping. It’s not addictive like Midazolam or Fentanyl, but it’s also, how can I describe this? It’s-
Juan: Is this another suppressant? Just give her something else to suppress something else. Yeah.
Patrik: Very much so, very much so. Yes. If you type Olanzapine into Google, it’s almost like it’s an anti-psychotic medication. Which is when people are going through a psychosis, that’s-
Juan: Yeah we don’t want to just numb her.
Patrik: Correct.
Juan: Because I truly believe that she just wants to get off all of this. I’m sure she’s dealing with withdrawal, but my mom’s a really strong person. She has a strong mind and strong willpower. So, I mean, I know there’ll be withdrawal, but I do think that we can see how to help them through that rather than just drugging her up more.
Patrik: Very much so, very much so. So, look, that’s sort of my concern with the Olanzapine. But look, if she gets off the ECMO and off the balloon pump and her lungs and her heart can recover, the next challenges for your mom are the withdrawal, and are the psychosis. And coming through this, what I would refer to, Twilight Zone.
Juan: Okay.
Patrik: But at least those challenges tend to be not life-threatening. They’re more on a recovery level. I mean, at the moment your mom’s challenges are still life-threatening. Can she get off ECMO and all of that? You know?
Juan: Yeah, yeah. So I guess we deal with the acute phase first.
Patrik: Correct.
Juan: And then we take up the mental and the physical health and strength. Both of those.
Patrik: Correct. Very much so.
Juan: So we can start looking at what drugs need to be removed and what support can be given to help with that, because obviously we are working towards recovery. And, yeah. Okay. Anything else?
Recommended:
Kevin: I have a second question.
Juan: Patrik, will you send us what we should be looking at in the arterial, ABG report?
Kevin: That’s what I was just going to ask.
Patrik: Yes.
Patrik: So let’s just quickly look at the last gas that you sent me. I’m just quickly looking through. Oh yeah, here it is. So the last gas that you sent me-
Juan: Patrik.
Patrik: You want me to send it to you again? So you can-
Juan: Sure, yeah.
Patrik: Just give me a second. Just give me a second. So I just sent it to you. Did you get it?
Juan: No, not yet. Okay, just got it, yep.
Patrik: Okay. Okay. So just have a look at this, the one that you’ve circled. If you get those numbers, that would be fantastic.
Juan: Okay. So if we get these numbers, the same ones?
Patrik: Would be fantastic. Look at the one before. I’m not worried about the top one. The two main ones that I’m looking for is the second and the third one. Everything-
Juan: The P02 and the PC02?
Patrik: P02 and PC02. Most importantly. So when you look at the one where you get the P02 of 52.9, that’s too low.
Juan: Right. And this says 159, right? 159.
Patrik: That’s 159. That’s too high, but that’s okay. You can always reduce support. And when you look at the first one there, were the P02 is 73.6, that’s also good. That’s good.
Juan: Okay. Okay. I understand.
Patrik: For simplicity, PO2 above 65, PCO2 between 35 and 45.
Juan: PCO2 between-
Patrik: I’ll text it to you. I’ll text it to you.
Juan: Okay.
Recommended:
Patrik: And then keep an eye on the lactate. Lactate has been very good. Any lactate above three would be a bit of a concern.
Juan: So under three.
Kevin: It’s actually come down even further, I think its 1.3 today, if I’m not mistaken.
Patrik: Yeah. That’s great. That’s great. So, yeah, that’s what you’d be looking for in a blood gas.
Juan: Okay. Her PO2 was 65%.
Kevin: This morning.
Patrik: Before or after V-A ECMO removal?
Kevin: After the V-A ECMO, this morning.
Patrik: After V-A ECMO removal, P02 65. No surprises there, that after V-A ECMO removal, that that would go down. No surprises there, but 65 is okay.
Kevin: Okay.
Juan: Okay.
Patrik: And I’ll tell you something. So when you look at the ventilator, okay. With a PO2 of 65, what they could do is they might be able to increase FIO2 on the ventilator to 70% in order to increase the PO2. There is no guarantee that would work because I don’t know how much oxygen is getting through the V-V ECMO.
Kevin: It’s 100% oxygen.
Patrik: Is it? Okay. If that is the case, then…
Patrik: So if that is the case, the issue there is, you can’t give any more oxygen than 100%. Okay? So therefore, the PO2 of 65 is a little bit of a concern because they can’t really do any more than that.
Kevin: Right.
Patrik: The only thing that they might be able to do is put the balloon pump back to one and one. Are you there?
Juan: Okay. So is there anything we need to ask them or raise about this?
Patrik: Oh, I would, if I was you, get another blood gas. Get another arterial blood gas and see what the numbers show.
Juan: Sure, okay.
Patrik: Other ways to potentially counteract that is to potentially increase the Milrinone and the Dobutamine. That might be another way to manage that, but you can’t give more than 100% of oxygen. That’s just not, you know.
Juan: Yeah, of course. Okay. Anything else?
Juan: Yes Patrik?
Patrik: Have they changed any other medications? As far as you’re aware?
Juan: We’re going to go and ask them again. I know they were talking about, I think one of her antibiotics… Which antibiotic ran out on Sunday?
Kevin: Polymyxin, that’s done.
Juan: Yeah, Polymyxin’s done.
Patrik: Okay.
Juan: And then-
Kevin: She’s on Zavicefta, something like that.
Patrik: Right, okay.
Juan: We’ll ask what else they’re starting. I know that they said that-
Kevin: I think she’s on one antibiotic and-
Juan: As well.
Kevin: One antibiotic and one anti-fungal.
Patrik: Okay. The other thing you might want to keep an eye on is, her APTT is 27.7. That is too low.
Juan: Okay.
Recommended:
Patrik: I do believe she’s still on heparin?
Juan: Yes.
Patrik: I would ask them, what is their plan with heparin?
Juan: They said that she’s going to need heparin for a while because of the clotting issues.
Patrik: Yep. Agreed with that. Especially if she stays on the V-A, whether she stays on ECMO or on the balloon pump, she needs heparin. I am worried with an APTT of 27 that it’s too low. Find out what their plan is.
Juan: Okay. We’ll do that.
Patrik: She’s taking steps, she’s taking steps.
Juan: Yeah. Yeah. I think the next few days will be critical.
Patrik: Yes, it will be. Yes.
Juan: And as we figure out what’s happening with the V-V, I think a lot of it will depend just on mom, and how she’s responding. I mean, my gut feeling tells me a little bit that she is quite happy to be off the V-A.
Patrik: Sure.
Juan: And she’s happy to be off some of these medications. I think that that’ll just overall help her and it’s boosted her morale. So that’s, I mean, that’s just my feeling.
Patrik: Yes. No, that’s really good. That’s really good. Is she responding to you?
Juan: She does. Today she was a little bit sleepier, but she does definitely. She moves her head, she recognizes our voices. Her heart rate goes up when we talk to her.
Patrik: That’s great.
Juan: Yeah.
RECOMMENDED:
Patrik: That’s great. It’s really important that you get those signs because it’s important for you to know that her brain is working.
Juan: Yeah.
Patrik: I think that’s really reassuring for you that you can see her brain is working.
Juan: Definitely, definitely. And she has different reactions when she hears different people’s voices. Like when she hears our voices, or when she hears my dad’s voice. You see her trying to mouth her name.
Patrik: Great. That’s really, really positive on that end.
Juan: Okay. Good. That’s good to know. All right. Thank you, Patrik. We’ll give you another update a little bit.
Patrik: Please, please.
Juan: All right. Thank you very much.
Patrik: Thank you so much.
Kevin: Thanks Patrik.
Patrik: Thank you so much. All the best for now.
Juan: Alright. Have a nice day.
Patrik: Thank you. Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!