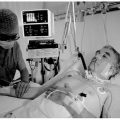
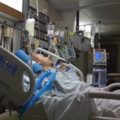
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Dustin, as part of my 1:1 consulting and advocacy service! Dustin’s father-in-law is with a breathing tube and on a ventilator in ICU. Dustin asks how his dad, with ARDS, can avoid the tracheostomy and LTAC.
How Can My Dad with ARDS Avoid Tracheostomy So He Won’t Go to LTAC?
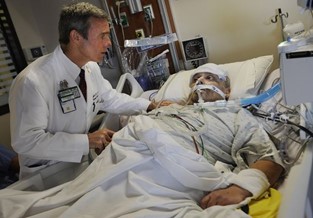
“You can also check out previous 1:1 consulting and advocacy sessions with me and Dustin here.”
Chloe: Okay.
Patrik: All right. And then it may not be avoided, but the risk is minimized I would argue, I remember doing that. You had a patient where you knew when you turn them on the side to wash their back, to change linen, all of that, you would know that they would de-saturate, so you would get them ready for that by giving them more oxygen beforehand to avoid that. Now your dad’s lungs, it may happen even if they do that. I don’t know, but it’s probably … if it does happen well, hopefully next time they’ve learned from it and pre-oxygenate, but that’s what it’s called. The technical term is pre-oxygenation.
Chloe: Okay.
Patrik: Right. It’s a bit of a catch 22, you can pre-oxygenate, and you can also sedate beforehand. Sedation often reduces the risk as well, but then again, you don’t want to give too much sedation either. Sedation again has its time and its place, but your dad is at a point where I believe sedating him would be detrimental to moving him forward.
Chloe: Okay. Yeah. Okay. All right.
Patrik: But coming back to your question, Dustin, should they be doing anything? I did ask last night about the nitric oxide about the Epoprostenol and then she mentioned the Sildenafil, look, they haven’t done the nitric oxide from what I understand, they haven’t done the Epoprostenol from what I understand, and it sounds to me like he might be on Sildenafil. Do you remember?
RECOMMENDED:
Chloe: Yeah. I think he is. Although I … How do you spell that again? I’m sorry-
Patrik: Well, don’t worry about … it’s actually Viagra. You’ve heard of Viagra.
Chloe: Oh yeah. Okay.
Patrik: Yeah. That’s what it is. That’s what it is. Sildenafil. It’s used it’s used for ARDS, Viagra.
Chloe: Wow. Okay. And you say it … when you ask if he’s on it, is that something they give him through a PICC line?
Patrik: No, they would give it … It’s a tablet and they would crush it and would give it through him … He probably has a feeding tube in his nose. They would crush it, put it in water and give it through his tube. It’s probably a 12.5 milligram dose or a 25 milligram dose.
Chloe: Okay. What do they use it again for? To …
Patrik: Yeah. It’s for pulmonary hypertension, ARDS causes pulmonary hypertension. What does that mean? Pulmonary hypertension basically stands for high pressure in the lungs. Right?
Chloe: Okay.
Patrik: And the Viagra basically opens up the vessels. It helps with the hypertension. Hypertension stands for high blood pressure in the lungs.
Chloe: Okay. I had no idea that they … I remember y’all talking about that, but I couldn’t understand between her accent and her mask. It was hard to understand her at times.
Patrik: Right. Right. So look, the Sildenafil, the Viagra all makes sense, however … Again, it looks like what they’re doing seems to work for now. It looks like they’re coming down with oxygen, the PEEP … What did she say? The PEEP is down to six.
Chloe: Yes. It still is.
Patrik: So that is a good sign. Most ARDS patients, PEEP 10, 15, wouldn’t be much higher than 15, but I’ve also seen patients in ARDS with a PEEP up to 20, but you wouldn’t go any higher than 15 or 20 ever. So those are good signs.
Recommended:
Chloe: Okay.
Patrik: I think the other thing that everybody is learning at the moment. So you’ve had ARDS before COVID and now you’ve got ARDS caused by COVID. Now nobody knows at the moment … not enough studies have been done yet. What’s the survivor rates for ARDS caused by COVID.
Chloe: Sure.
Patrik: I do believe there is a lot of experimentation going on at the moment because COVID has been around for one year now roughly, but I don’t believe anybody has any statistics in terms of, “Okay how many ARDS patients caused by COVID survive? What are the best treatment options? Does everything that we’ve done for ARDS pre-COVID still works for COVID ARDS?” I don’t think anybody knows yet.
Chloe: Yeah. Okay.
Patrik: I think it’s all experimental. Another thing that probably … Another thing that nobody knows yet either is, pre-COVID ARDS, you had, I believe probably about a 50% survival rate for ARDS roughly. Nobody knows yet. What’s the survival rate for COVID and ARDS? I believe it has yet to be decided, so that there are a lot of unknowns about that.
Chloe: Okay. Yeah, exactly.
Patrik: Just remind me Chloe, how many days is it again in ICU?
Dustin: 37.
Chloe: Yeah.
Patrik: Okay. 37. Okay. I can’t remember last night. Did they … this morning. Did they say that they’re doing physical therapy?
Chloe: Yes, sir. I asked that question. They are.
Patrik: Good.
Chloe: They are doing PT, physical and occupational therapy.
Chloe: Okay, great. That is very important. Very, very important. Nobody gets off a ventilator without physical therapy.
Chloe: Wow. Okay. Okay. I would have never felt that that was important. We have a close friend of ours who is a … He’s an occupational therapist. Yeah.
Dustin: He’s an OT.
Chloe: He’s an OT at a local hospital. And he said the same thing. He had told us that as soon as he’s actually able to respond to commands, I need to go ahead and put the orders in for that. I would have never felt that. And then of course hearing it from you really back set up. So he was telling me they have, they put the orders in and that should begin or they’ve already begun.
Patrik: Okay. I can advise you there, make sure their words match their actions. I tell you why. So let’s look ahead a little bit here. What’s happening in ICU is often … the focus is on saving lives. That’s what the focus is on. Things like physical therapy are often last on the list, because they are so busy saving lives. I guess your dad is now at a point where he’s waking up. I do believe physical therapy is going to be very important. Let’s just say, he’ll have a tracheostomy next week. Let’s just say he’ll have that. Have you got any idea of what might happen next after he has the trach? Do you have any ideas?
Chloe: No, sir. I don’t.
Suggested links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Patrik: Okay. All right. No, no, that’s good. Well, it’s good but I’ll explain to you what will probably happen next. Once he has a trach and he’s stable enough, they will try and send him to LTAC. Have you heard of-
Dustin: Oh yeah. No, we read about that. No, yeah we read about that. Actually, I read a conversation you were having with one of your other clients and he was struggling on it with his sister. I believe it is, about if he gives approval for the trach, if it means that he gives approval for them to go to LTAC and you recommended to keep them in ICU, to try and keep her in ICU after the trach. See we’ve been reading your stuff.
Chloe: Yeah. We have. I’ve been watching a lot of your videos-
Patrik: Okay. That’s nice of you.
Chloe: … and read all-
Patrik: That’s nice of you. That’s what it’s there for-
Chloe: No, no. Hey, your YouTube videos are very helpful. They really are.
Patrik: Okay. That’s nice to hear. Thank you. Thank you. So LTAC is from my experience, it’s the better version of a nursing home. The LTACs from my experience are designed to save money, not for clinical need. So your dad, depending on what health insurance he’s got would be entitled to … for simplicity, let’s just say he’s entitled to 60 days ICU. And what might happen if he ends up with a trach next week, they will probably try and send him out fairly quickly, got to be prepared for that. There’s a number of things that are concerning there, not only the level of care he will be getting an LTAC. That’s number one. Number two, LTACs are often not around the corner. I have seen patients going from one location to another for this. It’s ridiculous.
Suggested links:
Chloe: Oh my goodness.
Patrik: Ridiculous.
Chloe: Yeah.
Patrik: I have seen people going to an LTAC around the corner as well, but I’ve seen all sorts of things. But you got to be prepared that this conversation will happen. I would argue that if he ends up with a trach and he’s on … let’s just say he’s on 50% of oxygen. He’s on a PEEP of five and he’s medically stable, they will try and send him probably to LTAC.
Chloe: Okay. As long as he’s medically … What would qualify for not medically stable?
Patrik: Yes. Vasopressors in particular, what I mentioned before. If he has a low blood pressure and he ends up on vasopressors, he wouldn’t go to LTAC.
Dustin: Oh, that’s one of the two medications you were talking about with the other client, the two medications that they’re on. They have to stay in ICU.
Patrik: Yes. Yeah, very much so. Or, if he’s in an induced coma, he wouldn’t go to LTAC either. So if he is out of a coma, less than 50% of oxygen PEEP of 5, no vasopressors, no dialysis. He will … They will try and push and send him to LTAC. The problem is that your dad’s ventilation needs are so high at the moment. I can’t see that he can avoid the trach. And also I would argue that after many weeks now often induced coma, I would argue he’s too weak to be weaned off the ventilator in a few days.
Chloe: Yeah. I agree with you. I figured that myself.
Patrik: And that comes right back to the physical therapy. Comes right back to the physical therapy. It’s like, you can’t run a marathon if you’re not training for it. And it’s the same …
Chloe: Absolutely.
Patrik: It’s the same with the ventilation. You got to picture this. He’s been in an induced coma for weeks. He hasn’t moved. He’s going to wake up. His muscles are wasted. He will have difficulties just lifting his arm.
Chloe: Well, okay. Yeah, that’s one thing that my stepmother, I have not had this conversation with her. And this is another thing that she’s going to have to understand. So, I’m really glad we got a chance to talk to you because this is good. You’re giving us a lot of good insight. She’s already getting in her mind that we … she knows we haven’t won the battle and she knows we haven’t won the war, but I think she’s on the impression that once he’s done, he’s coming home.
Recommended:
Dustin: No. There’s going to be lots of rehab after … he’d got outpatient … I mean, inpatient rehab for a while.
Patrik: As much as I can help you guide with this, I certainly … Nobody has a quick fix for this. Your dad will be in for a long ride. And that could mean a prolonged weaning off the ventilator. It could be that he might never get off the ventilator, but you know that … nobody has a crystal ball there.
Chloe: Sure.
Patrik: Nobody has a crystal ball, but… I keep coming back to physical therapy, make sure their words match their actions. I don’t know how you can monitor whether he is getting physical therapy or not.
Chloe: Okay. All right. Yeah-
Dustin: Well, we could ask who the physical therapist is. I mean, get names of who the actual OT and PTs are that are going in and just ask for updates of what body parts they worked, or what did they actually do in therapy today with him. For them to explain actually what they did or to ensure there’s even a nurse assigned to him and what days the OT and PTs are. Like, just to know his schedule, understand his schedule and if they actually have.
Patrik: Yep. Yep. And also you could then ask the next question, by doing that do they see any improvement?
Dustin: Okay.
Patrik: By that, I mean, it could be as simple as … I would argue that after four weeks in a coma and being paralyzed, I would argue that if you ask him to lift his hand or his arm, I would argue that he couldn’t.
Chloe: Okay. Yeah.
Patrik: Baby steps. Unfortunately baby steps.
Dustin: Absolutely.
Patrik: Okay.
Dustin: But it’s better than nothing. It’s better than him just lying there dead.
Patrik: Absolutely. Absolutely.
Chloe: Okay.
Patrik: So that’s that. With LTAC … No, LTAC will happen without a trach. I guess you got to be prepared that if he for whatever reason … if they can’t move him to a trach, I wouldn’t be surprised if they keep coming back and change their conversation again and say, all of a sudden now he’s terminal again. All right. You got to be prepared for that. And I say it with a little bit of sarcasm because, I’ve seen so much over the years, but I see the story change all the time depending on what they need.
Chloe: Yeah. He could go down to terminal level again and then spring back up.
Patrik: All right.
Chloe: And this could happen a few more times. I would imagine. It’s possible. Hopefully not, but it’s possible.
Patrik: It’s possible.
Chloe: Just in a matter of a couple of weeks. How long will they stay on their path or their plan until they go, “He’s terminal again.” Is there any idea how … Is this hard to say?
Patrik: No, I wouldn’t say it’s hard to say. Again, I’m probably a little bit sarcastic here because I’ve probably been in the industry for too long. It probably depends, do they need the bed urgently? Do they have staff? Are you a pain in the bum to them? It’s all of that. It’s all of that.
Chloe: Ok.
Patrik: Look, let me say this. Their worst case scenario is … Their worst case scenario is to look after a patient indefinitely with an uncertain outcome. That’s the ICU worst case scenario.
Chloe: Right. Because they know what to do with them.
Patrik: Why would they-
Dustin: They need resources.
Patrik: Resources. Yeah, resources. I guess what’s happening at the moment … ICU beds are in high demand normally, now you’ve got COVID it’s terrible.
Recommended:
Chloe: Yeah. Yeah.
Patrik: I hear everywhere, they’re having makeshift ICUs.
Chloe: Yeah.
Patrik: And I’m wondering … Okay, you’re putting up makeshifts ICUs everywhere. Where do you get the staff from? Where do you all of a sudden get qualified ICU staff from? It takes years to train them, so it worries me. I can see the need, but I also know it takes years to train ICU nurses, train ICU … You can’t tell me you’re opening up another 10 beds and all of a sudden you’ve the staff for it. You can’t tell me that.
Chloe: Right. Exactly. Right. I agree.
Dustin: You’re getting on the job training right now.
Patrik: Yes. Very much so. I guess those people have to be looked after, of course, but I believe it comes at a price and that price is, how long do ICUs offer treatment? When do they go down the track of, “Yep, your dad is terminal,” And those timeframes I believe are getting shorter and shorter at the moment.
Chloe: Okay. Okay. Yeah. Like we said before, we’re all going to die and-
Patrik: Of course.
Chloe: And I’m willing to face that. I know it’s coming … when this happened, I just felt like something was just … none of it sounded right, the way that … The information my stepmother was getting. And then my husband with his profession, what he does, he was seeing a lot of red flags.
Patrik: The other thing I should have asked that last night, and I think I asked you yesterday, this is a reasonably small ICU.
Chloe: Yes, sir. Our place got about 150,000 people. There’s one other hospital that’s larger than this one. This one’s in a fair part of town. But it’s not a large operation.
Patrik: Right. That the reason, again, I’m bringing this up is if someone is in an eight bedded ICU, eight bed ICU, I … Let’s say an eight bed, ICU is the only ICU in a hospital. Sometimes you have hospitals that have three eight bed ICU, because they have cardiac and they have neuro and they have trauma or whatever. But if it’s only an eight bed ICU in a small hospital, I would argue they don’t have the expertise and the resources to look after the ARDS. Because if you have a 40 bed ICU in a big hospital, they’re exposed to this all the time.
RECOMMENDED:
Chloe: Right. Yeah, this is … Their daily work routine is dealing with ARDS. That’s what I was trying to give this doctor too. I was hoping to put her in a position where she had to admit that she has no other way to treat him or that he needed additional treatment that she could not provide. And I was clear with that with my stepmother. That was what I was really shooting for. I can’t prove that she can or cannot do what’s necessary for him. But I would’ve liked for her to admit to us, “Hey, I can’t do it. You may need to find another hospital for him.” Which I would have. I would have found something.
Patrik: I guess it would be difficult at the moment I would argue to find another ICU bed somewhere else. Not impossible, but I would argue it would be very difficult at the moment.
Chloe: Right. Yeah, the hospital that I would like him to go to, which has been an hour and a half from here, they said that they could possibly take him, but they said, “Go ahead and get the transfer paper.” The hospital where he is in right now, we have to go ahead and submit the transfer papers. And they may not have something available at the moment. But as soon as one gets opened, he’ll be the next in line.
Patrik: Absolutely.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!