Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
What Would Recovery Look Like for my Mom on ECMO After Leaving the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Juan, as part of my 1:1 consulting and advocacy service! Juan’s mom is with a tracheostomy, balloon pump, and is now on VV- ECMO. Juan is asking how he makes sure that his mom is improving and recovering whilst on ECMO in the ICU.
How Do I Make Sure That my Mom is Improving and Recovering Whilst on ECMO in the ICU?
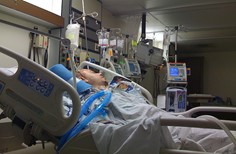
“You can also check out previous 1:1 consulting and advocacy sessions with me and Juan here.”
Patrik: Yeah. I’ll tell you how they might go around it, if they can’t turn her. They would need to use like a ceiling hoist, a hoist machine, and lift her in the ceiling, so they can take off the pressure off her back wash her back. Someone can look at her back while they are hosting her. That is the only way. And I’ve looked after many patients on ECMO that you can’t turn, because they are too unstable. And the way to manage them is, most bed spaces where I worked at and we had patients on ECMO, there was a ceiling hoist in the bed space, and we were using the hoist to lift patients up. Because you’re not changing much of their position, you’re just lifting them up, that’s how they stay hemodynamically stable, and that’s how you manage the pressure sore. Now, I don’t know whether there is a ceiling hoist where your mom is or not.
Juan: I don’t know either. We have to ask.
Kevin: We’ll ask them.
Juan: We’ll ask them.
Patrik: Yeah. You definitely have to ask them.
Juan: Okay.
Patrik: Because if she keeps improving, you don’t want the pressure sore to…
Juan: … throw that off.
Patrik: … throw that off.
Juan: Yeah, I understand. So I think we can just ask them about the hoisting, and if they have that there and how are they thinking about lifting her up.
Patrik: Yeah.
Juan: Okay, sounds good.
Patrik: Okay. All right. Let me know if you want to talk later.
Kevin: Thank you.
Patrik: Thank you.
Juan: Yeah. As soon as we have another update or something, we’ll just forward you the images as well.
Patrik: Yes please, yeah. Okay great.
Juan: Okay. Thank you Patrik.
Patrik: Thank you so much. Thank you. Bye.
Juan: Bye.
Patrik: Bye.
RECOMMENDED:
Patrik: Hi, Juan. How are you?
Juan: I’m fine, thank you, Patrik. How are you?
Patrik: I’m very well, thank you. I’m just looking through the pictures that you’ve just sent.
Juan: Yes, go ahead and take a look.
Patrik: Okay, so they’ve done specimen CMV (cytomegalovirus).
Juan: The first image is today’s results.
Patrik: Yep.
Juan: The second image is the last one.
Patrik: The last one… hang on. So, this is today… Yep. And the other one is… hang on. Oh, it’s from 8 days ago… real time interpretation. Viral load is expressed as copies… highly sensitive. Okay. So, now I’m just going back to the first one.
Juan: The load has reduced substantially.
Patrik: Yeah. Okay, that’s good. Well, the chest x-ray has improved.
Juan: Yes.
Patrik: The chest x-ray that you sent earlier has improved significantly which also is probably why the blood gas improved. Which is probably, also, why they changed the ventilator settings once again.
Juan: Yes.
Recommended:
Kevin: It changed again?
Patrik: No, no.
Juan: I just sent the latest ventilator settings.
Patrik: No, no. They haven’t changed it between now and the picture that you sent earlier, but compared to yesterday they were running it through pressure control. Whereas, today they’re running it through volume control which is probably a sign that things have improved.
Juan: Is that better for her? The volume control?
Patrik: No, I don’t think that volume control is better for her. It just means they are not a risk as they were yesterday. I think it’s riskier for her to be ventilated in pressure. It’s riskier for her to be in ventilated in volume control than it is in pressure control. Obviously, they are happy to take the risk which I see as a good sign.
Juan: Okay, okay. Does that mean that we just let them carry on in whatever mode? Should we be concerned about the mode? I’m just wondering.
Patrik: Yeah. No, that’s a great question actually. I do think swapping and changing modes all the time is not so good. Have you seen your mom today?
Juan: Yes.
Patrik: What does she look like? Is she stable? Is she waking up? Is she comfortable? Is she uncomfortable?
Juan: She’s not waking up that much. She’s looking quite like her head is looking a lot darker than yesterday. Her face is darker.
Patrik: Right.
Juan: It’s a lot more discolored. She looks more tired but her parameter seems to be improving.
Patrik: Yep.
Juan: But the Midazolam is up like one. The Atracurium’s off right now.
Patrik: Yep.
Juan: Atracurium is a four? We saw it… it’s off, right?
Kevin: It’s still at 4.
Juan: It’s on 4? Okay. No, sorry the Atracurium is on 4, my mistake.
Patrik: Atracurium is on 4?
Juan: Yeah.
Suggested links:
Patrik: I can’t see that in the pictures but maybe.
Juan: It’s the first image. Sorry, the name is cut off.
Patrik: Oh, that’s why. Okay. The 4 is the Atracurium is it?
Juan: Correct. Yes.
Patrik: Yeah. Of course, then she wouldn’t be waking up. Something seems to work, obviously, when you sent through the other pictures earlier she’s on antibiotics. Again, something seems to work.
Juan: Yeah.
Patrik: What are they telling you of the next steps? Are they giving you any insights?
Juan: We were going to wait for this viral loads results to come back and then meet and discuss. So, now, that it’s come back, we’re going to go talk to them after speaking with you. Well, they had already stopped at reducing the flows a little bit of the Atracurium…
Patrik: Yeah, I can see that.
Recommended:
Juan: I guess if her blood gas is not improving then I imagine they would keep going forward with that. They’re starting the feeds again slowly because she is not aspirating anymore. They are tapering off the Noradrenaline. It’s at 0.1-2 I think, if I’m not mistaken now.
Patrik: Yep. Her blood pressure is very decent.
Juan: Yep, so that’s allowing them to do that. So, I think they will continue this tapering, I imagine, for the next couple of hours. We wanted to, obviously, talk to you about this whole antibiotic, steroids business and managing at some point. We said for a while we’ve been very keen to stop the Ganciclovir, definitely, if her loads has decreased so much.
Patrik: Definitely.
Juan: We wanted to talk you about that as well. It’s been eight days, of course, which is quite a while.
Patrik: Have you asked them?
Juan: I mean we’ve expressed that multiple and they said, “Let’s look at the load. If it comes negative or if it’s reduced some we can talk about it.” That’s what we’re going talk about in the office.
Patrik: Look, with antibiotics, for an example, you usually run a course. Usually, say, five days of whatever it is… let’s do that. With the antivirals it’s a little bit more leeway. I guess, given that the viral loads seems to come down in the test, something seems to be working. But at the same token, as we discuss, obviously, the Ganciclovir has very nasty side effects.
Juan: They had said that we can do a 7-day course, or a 10-day course, or a 14-day course, or something like that. They never specified. So, we have crossed seven days.
Patrik: You have crossed a week? Sure.
Juan: And she’s exhibiting a lot of the side effects that are listed as concerns for Ganciclovir. So if it’s done its job and it’s helped… If she’s got an 8-day course. Yeah, we’ll talk to them and see what they have to say. There are lots, and lots, and lots of different options that goes specific no broad-spectrum. She’s on everything that could be possibly have been thrown at her. Yeah, we are very concerned. For every issue that she’s facing, they’re not able to pinpoint anything anymore because there’s just so much going in. Right, so…
Patrik: Right. Yes. Look, the other question that I have is on what grounds are they giving the antibiotics?
Juan: On the grounds that these cultures are showing…
Patrik: Right.
Juan: And some proactively as well.
Patrik: Right.
Juan: Symptoms are so general. She doesn’t have a fever which is one of the main symptoms that we should be seeing, but she doesn’t have a fever. She doesn’t have chills.
Recommended:
Patrik: And the x-rays improving so, something is improving.
Juan: Yeah.
Patrik: And the gases are improving. I see it as baby steps, but when you look at the reduction, in support from ECMO, it’s baby steps but it’s steps.
Juan: Yes. This afternoon they did say that. They said, “Look, her chest x-rays looking better. Her blood gas is improving. BP’s holding… we’re tapering off the Noradrenaline.
Patrik: Yes.
Juan: These are good signs. So…
Patrik: Yes.
Juan: That was where we left off. Is the edema, and the face being much discolored, something we should be concerned about it? Is it expected in her situation?
Suggested links:
Patrik: When you say the face being discolored, can you describe a bit more. Is it yellow? Is it grey? Is it…
Juan: Wait, I took a picture actually to send you.
Patrik: Right.
Patrik: The first thing that comes to mind without having seen the picture… the first thing that comes to mind is this. If you’re talking a bit about discoloration, and if we’re talking liver function and kidney function going off… is she potentially jaundiced?
Juan: So, it’s not yellow. She’s looking darker. I mean, she’s a tan woman in general.
Patrik: Then I would say it’s kidneys.
Juan: Yeah, the face… it’s mostly the face that’s gotten darker. The rest of her body seems to be more normal in color. As you can see in the picture, her skin color on her shoulders and her arms. And then, her face was brighter yesterday. Honestly, until Thursday, it was brighter and then everyday it seemed to get a little darker. She got a little lighter yesterday and then it’s dark again now. The timing correlates with the Ganciclovir but whether or not it’s that I don’t know.
Patrik: Yeah. It could also be hemoglobin drop. My first guess is kidneys.
Juan: Okay.
Patrik: If she’s not jaundice, it’s kidneys.
Juan: Okay. So if the kidney function goes up then the face gets discolored, or skin gets discolored.
Patrik: Very much so, very much so. Yes, I would say so… this is kidneys.
Juan: Yes, it was nothing like yesterday.
Patrik: …even though she might be producing urine…
Juan: Yes.
Patrik: Even though she might be producing urine… because kidney’s functions are going off, she’s not excreting the toxins.
Juan: Yes, and her magnesium is really high and it’s not going down.
Patrik: Correct.
Juan: …even though we stopped the magnesium supplementation, and the steroids are not going down which obviously means than its kidneys most likely.
Recommended:
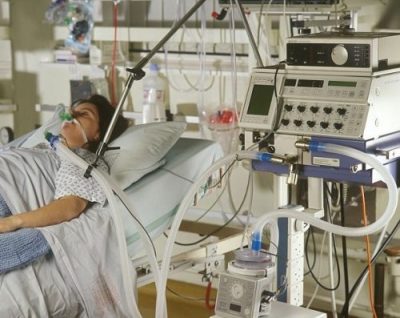
Patrik: Correct. Now, I have another concern when I see this picture. Towards the end of the ventilator circuit can you see there is this screen? So, away from your mom’s neck you can see that yellow little line?
Juan: Yeah.
Patrik: And then, next to that yellow little line is this green big filter.
Juan: Yes.
Patrik: That’s a concern and I’ll tell you why. Does she have that filter all the time?
Juan: The green and white one next to the tracheostomy thing.
Patrik: Yeah. No, I’m talking about… I wish I could circle this because I’m not good at that.
Juan: Can you shade this and then try to upload the image? There’s a little…
Patrik: So, I’m talking about… at the bottom of the picture. Not towards your mom’s face, away from your mom’s face.
Juan: Yes, the green…
Patrik: Okay. So, the green big filter at the bottom end of the picture.
Juan: Yes, we know what you’re talking about… got it.
Patrik: Does she have that all the time?
Kevin: Yes.
Juan: Yes, I think so.
Patrik: Okay. All right.
Juan: I’m going to look at old pictures to double check. But yes, I think so.
Patrik: Right. That’s a concern and I’ll tell you why. When someone is having a tracheostomy they should be on humidified oxygen. That filter is preventing your mom from humidified oxygen. Now, the research has it that those filters are providing humidification as well but it’s never as good as the humidifier never.
Juan: Okay.
Patrik: I’ll send you the picture of what she should be on and they will probably make all sorts of rationalizations and say this is just as good as the humidifier. I question that. Those filters were used in ICU 20 years ago and then people realized it’s not as good as the humidifier. The reason this is important is… So, when you and I breathe in through our noses, the air gets humidified through our nose. It’s a natural filter.
Juan: Yeah.
Patrik: Now, when someone is having a tracheostomy, obviously, they’re not breathing through the nose.
Juan: Yeah.
RECOMMENDED:
Patrik: So, therefore, air/oxygen needs to be humidified. That filter is doing some of that, but it’s not as good as a humidifier. I will send you a picture of a humidifier. It might not be as important at the moment because she’s on VV ECMO. I still think, especially with your mom’s condition, I actually think this might make a difference.
Juan: So, a humidifier is another attachment like that, that can be used-
Patrik: No, it’s not an attachment. What it is, is the… I’ll send you a picture so you know what I’m talking about. The ventilator needs to run through a humidifier so that the inhaled air/oxygen is actually humidified.
Juan: We just looked up a picture. So, it’s a little device that which gets attached to the ventilator.
Patrik: Very much so. I have to send it to you.
Juan: Okay. Yeah. I’m going to send a picture as well.
Patrik: Look, there are others… this is just one of the most common ones. There are others too but I see it every now and again and it’s just a big red flag to me. Yeah, that’s one. That’s the one that you sent. That’s what I’m talking about.
Juan: Okay.
Patrik: And enlarge that picture… it suggests it should be at 37 degrees. Right. Yeah, I worked in ICU when the filters went away to the humidifiers. In the early days, when I started in ICU, it was only the filters. And then, I actually did witness the humidifiers coming in 20 years ago. I would argue it was almost like a small revolution.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!