Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM , where we INSTANTLY improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, get PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question last week was
My wife wants to die in Intensive Care after she had a lung transplant
You can check out the answer to last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer another question from one of our readers and the question this week is
HOW LONG CAN A BREATHING TUBE OR AN ENDOTRACHEAL TUBE STAY IN?
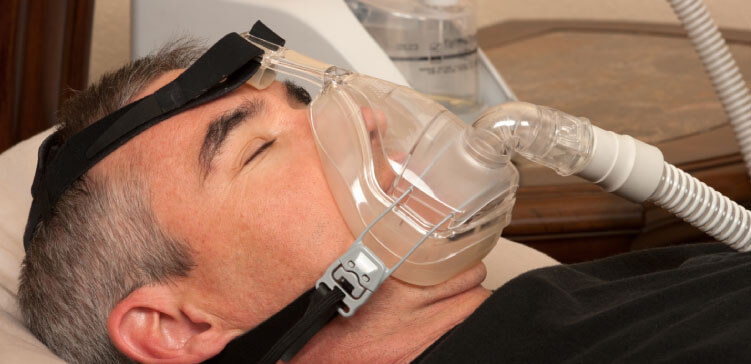
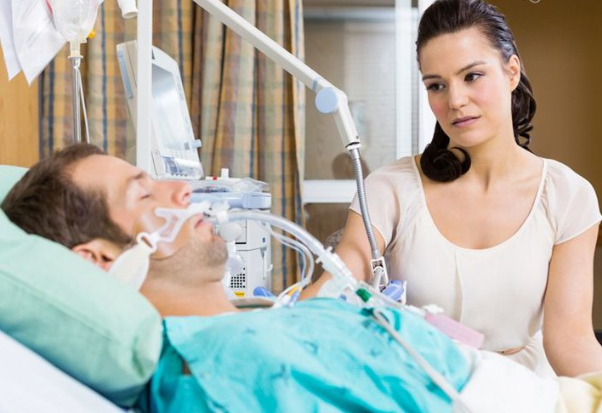
A very common question that I get asked quite frequently from family members or friends of critically ill Patients in Intensive Care is how long a breathing tube or an endotracheal tube stay in when their loved one is mechanically ventilated in Intensive Care. So lets get right into it.
Now, as a rule of thumb, a Breathing Tube or an endotracheal tube is usually staying in your loved one’s throat or Larynx for up to two weeks at the most, unless there are special and rare circumstances. I’ll come to that later.
The reality is that most critically ill Patients in Intensive Care only require mechanical ventilation with Ventilators(Breathing Machine) with a Breathing Tube or an endotracheal tube for a limited period of time.
Most mechanically ventilated Patients in Intensive Care only require ventilation with a breathing tube or an endotracheal tube for a few days at the most.
If your loved one is mechanically ventilated and on a breathing tube/endotracheal tube they will also be in an induced coma.
Related article/video:
There is always the exception to the rule of course and if your critically ill loved one requires mechanical ventilation and the breathing tube for more than a few days, potentially 7 days and longer, a tracheostomy might be a next step, but I’ll come to that later and have some more information about tracheostomy down the line!
The most common reasons for mechanical ventilation with a breathing tube or an endotracheal tube in Intensive Care is post-surgery, trauma, lung diseases such as Pneumonia, Adult Respiratory Distress Syndrome (ARDS) also known as lung failure, COPD, Acute Severe Asthma and also other admissions such as Pancreatitis, Burns, Heart Attack (Acute Myocardial Infarction) or Cardiac Arrest situations.
The list when a breathing tube/endotracheal tube and mechanical ventilation is required is not exhaustive and I only mentioned the most common scenarios in Intensive Care where mechanical ventilation with a breathing tube or an endotracheal tube is necessary.
But because the question that I get asked quite frequently is how long can a breathing tube or an endotracheal tube stay in your loved one’s throat, the answer is that it can almost stay in indefinitely. That’s certainly not a desired goal and again and normally doesn’t happen. Normally I would say that up to two weeks is the longest that I have seen it.
If a breathing tube/endotracheal tube stays in for >14 days, there are usually unusual circumstances requiring the breathing tube/endotracheal tube stay in for longer than clinically recommended such as
- Extubation(=removal of the breathing tube) is close and only a few more days away
- Anatomy of a critically ill Patient doesn’t allow for a tracheostomy to be performed I.e. short neck
- Upper airway swelling is present also known as laryngeal oedema. It basically means that the throat/larynx is swollen and if the breathing tube or endotracheal tube would be removed it would cause a stridor and your loved one wouldn’t be able to breathe. The treatment involves parenteral administration of corticosteroids, epinephrine/adreanline nebulisation and inhalation of a helium and oxygen mixture.
Usually what happens if your critically ill loved one is requiring ongoing mechanical ventilation and it is foreseeable that Extubation or removal of the breathing tube is not on the horizon due to the critical illness of your loved one, normally a formation of a Tracheostomy is the next step.
A Tracheostomy is another tube that is permanently or temporarily inserted into your loved one’s neck into the windpipe going directly into the lungs. This Tracheostomy tube is making it a lot easier for your loved one to be
- mechanically ventilated as the tube is no longer in the mouth
- weaned off the ventilator, as ventilation with a Tracheostomy doesn’t require a huge amount of sedation compared to the amount of sedation needed for when your loved one requires the breathing tube through the mouth
Related articles/videos:
- taken off the ventilator intermittently or permanently to find out how well your loved one is breathing without the ventilator
- generally looked after, as a Tracheostomy is much easier for your loved one to tolerate and is also less risky than a breathing tube or an endotracheal tube
Furthermore, a Tracheostomy tube can stay in infinitely and in fact some People have a life long Tracheostomy tube in place and they can live with it independently.
Also, by the time your critically ill loved one comes off the ventilator and the breathing tube/endotracheal tube is removed(=Extubation), they will need to be awake and have come out of the induced coma.
They need to be able to cough, breathe by themselves and they need to be able to follow simple instructions such as squeezing hands etc…
For more information how to wean your loved one off the ventilator and the breathing tube/endotracheal tube step by step click here
One of the reasons why your loved one may not be able to come off the ventilator, is that they haven’t woken up from an induced coma.
Here is more information what to do if that’s the case.
I hope that answers this common question that I get all the time and if you have any further questions, please send your questions to [email protected]
How can you make informed decisions, get PEACE OF MIND, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care! Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below!
In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care!
In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care(it’s not what you think)
Thank you for tuning into this week’s episode of “YOUR QUESTIONS ANSWERED” and I’ll see you again in another update next week!
Make sure you also check out our “BLOG” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Also check out our Products section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 consulting with me via Skype or over the phone by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!
Your Friend
Patrik Hutzel