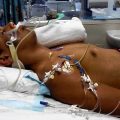
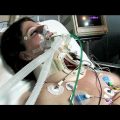
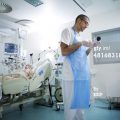
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How Can My Mom Prevent Withdrawal Symptoms or ICU Psychosis after Being On an Induced Coma?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Juan, as part of my 1:1 consulting and advocacy service! Juan’s mom is with a tracheostomy, balloon pump, and is now on VV- ECMO. Juan asks how long his critically ill mom needs to be on life support and remain sedated in the ICU.
How Long Will My Critically Ill Mom Need To Be on Life Support & Remain Sedated in the ICU?
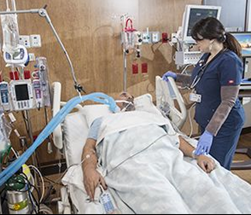
“You can also check out previous 1:1 consulting and advocacy sessions with me and Juan here.”
Patrik: Hey, Juan. How are you?
Juan: Hi, Patrik. How are you?
Patrik: Very well, thank you. How’s your mom?
Juan: She’s all right.
Patrik: That’s good.
Juan: So she has a few small fluctuations today.
Patrik: Right.
Juan: So, they’ve decided to remove the IABP tomorrow.
Patrik: Okay.
RECOMMENDED:
Juan: Instead of today.
Patrik: Okay.
Juan: They have reduced it to 1:3.
Patrik: Good.
Juan: But they said they don’t want to leave it at 1:3 at night. So they’ll keep it 1:3 in the daytime and then at night, they’ll change it back to 1:2, and then probably tomorrow they’ll remove it.
Patrik: Right. Okay. Well, it seems to be fairly strong.
Juan: Yeah. Yeah. It does seem to be strong.
Patrik: That’s good.
Recommended:
Juan: And it’s been holding the whole day, actually, since seven in the morning till now, it’s been holding up that.
Patrik: That’s great. That’s great.
Juan: Yeah. So there’s this virus type, I think I sent you the..
Patrik: Yes. The results.
Juan: So that… Yeah. They’ve introduced something called Ganciclovir.
Patrik: Ganciclovir. Okay. That’s pretty strong stuff.
Juan: So they said that she has a high viral load off it, so they’ve introduced ganciclovir and they’re hoping that should take care of it.
Patrik: Sure. Yeah.
Juan: They feel like these fluctuations might be being contributed to by that. So she’s been breathing a little bit shallow breaths today and she’s been trying to breathe more and more on her own. So they adjusted the ventilator settings. They needed to make it 1:5 from 1:2. I don’t really know what that means, but they made it so that her inhalation is quicker, I think, than her exhalation.
Patrik: Yes. Very much so.
Juan: Yeah.
Patrik: That is what they’ve done. When I look at the picture, they’ve basically increased her pressure control. I believe she’s now needing to do less work. Are they talking about wanting to wean her off? I mean, they need to wean her off ECMO first before they even talk about weaning her off the ventilator.
Recommended:
Juan: That is the plan. That is the plan. So I think they feel she needs a couple more days on the VV ECMO.
Patrik: At least.
Juan: Yeah. So that’s going on. Yesterday and day before, her chest x-rays were looking clearer.
Patrik: Right.
Juan: So the black portions were more visible.
Patrik: Good.
Juan: Today it was a little bit cloudier than yesterday.
Patrik: Right.
Juan: But one of the doctors at first thought that maybe she would like to introduce a hemofilter, but then…
Patrik: Yes.
Juan: Again. But then the head doctor said that she doesn’t want to do that. So they’re not doing that.
Patrik: Fair enough.
Juan: Because they… Yeah. I guess they want to keep that balance right. They’ve removed the Fentanyl and Midazolam and Atracurium completely. I don’t think they want to use that anymore. Instead they’ve introduced some Morphine.
Patrik: Okay.
Juan: And they’re reducing the Precedex slowly that by 0.2 every hour. So it’s probably at about 0.5 right now.
Patrik: Why are they introducing Morphine instead of keeping going with the Fentanyl? Did they tell you? Were they tell you?
Juan: So I think they feel like if it’s more calming and they need to focus on calming her right now because she’s getting quite anxious. And I think that that’s not having that effect.. I think.. Hold on.
Kevin: Yeah, I think maybe she’s also built up resistance to it because it’s been on for some time now.
Recommended:
Patrik: Right.
Kevin: So…
Patrik: Okay.
Kevin: They said they just want to switch to morphine. They’re doing a low dose of morphine and they said morphine has a… I guess, they said it’s more natural than fentanyl.
Patrik: Okay. Maybe a little bit. Yeah. Maybe a little bit.
Kevin: Yeah.
Patrik: Okay. Fair enough.
Kevin: Yeah.
Juan: So they don’t want to be using any of that anymore.
Patrik: Yeah, no, that’s good that they are not using that anymore. And the Midazolam is off at the moment, isn’t it?
Juan: Yes. It’s off and I don’t think they want to be using more of Midazolam either.
Patrik: No, no, no. Wouldn’t be.
Juan: Because yesterday they ended up giving her so many boluses that they were just a bit like, “What’s the sense?” If boluses and the regular are ongoing… As in, if there’s no difference, if you’re getting so many boluses that you’re just giving too much anyways, then it does defeats the purpose they said that they wanted to move over to something that’s more calming and less damaging for her. So they… Well, I guess right now, for now they’re looking at Morphine and they’re trying to reduce the Precedex.
Patrik: Fair enough. Fair enough. To me it sounds like..
Juan: I think, also, that they realized that she’s moving into recovery, even if it’s a little bit slow right now, I think now they want to make sure that they’re focusing and preparing for the recovery. I get the sense.
Patrik: Yeah. I mean, that makes sense. I think, as long as she is on ECMO, recovery, it’s still a long way away because at the end of the day, ECMO is one of the highest forms of life support anyone can have. I mean the progress she’s made in the last few days is significant.
Juan: Right.
Kevin: We sent you all the markers including the updated one, but the SGPT and SGOT was down significantly.
Patrik: Yes.
Kevin: The CRP is down.
Patrik: Yeah. Yeah, yeah.
Kevin: Lower. Only the platelets and the hemoglobin.
Kevin: Hemoglobin have dropped a bit.. One of the reasons is definitely because of the IABP for the platelets.
Patrik: Yes.
Kevin: And the extracorporeal support for the hemoglobin.
Patrik: Yes. Very much so. But I mean, yeah, the progress she’s made is significant, but on the other hand she still has a long way to go.
Recommended:
Kevin: Yep. Yeah. So they’re giving her a unit of blood right now.
Patrik: Yes. And I can assure you that as long as she is on ECMO, her hemoglobin will keep dropping.
Kevin: Yeah.
Patrik: Because there’s too much blood going in and out.
Kevin: Being taken out.
Patrik: Yes.
Kevin: Yeah, yeah.
Patrik: Even though it’s going back in, there is some loss there.
Juan: Yeah, they said that to us as well. I think they’re pretty clear that that’s why it’s happening.
Kevin: Yeah. The endothelium is much different than the plastic pipes of the ECMO, so that might contribute.
Patrik: Exactly, exactly.
Kevin: Yeah.
Patrik: Okay. What are they doing with a PA catheter? Why is that still there? They’ve giving you a reason why?
Juan: I think they were going to remove the PA catheter with or soon after the IABP.
Patrik: Okay.
Juan: And then I think when all of this… They’re just trying to stabilize her right now with these other changes and get the blood transfusion done. They keep saying that yeah, we’ll remove the PA catheter with, or just after the IABP.
Patrik: Right. Okay. All right. Well..
Juan: We’ve asked about it multiple times now. And I mean, they said that if it ends up being that for a few more days, then we would change the line, if they’re worried about the line..
Patrik: Sure.
Juan: Yeah.
Patrik: Look, I mean, on the one hand, it’s great to have a cardiac output. That’s fantastic, but on the other hand, the risk of the infection is just high.
Juan: Yeah. I think for today, if they’re removing the IABP tomorrow, we’ll push and see if they can remove the PA catheter as well, because it’ll have been a week, split that line then.
Suggested links:
Patrik: Yes.. Absolutely.
Juan: Yeah.
Patrik: So what are they saying? So balloon out tomorrow, and then are they giving you any timelines about VA ECMO removal?
Juan: So today when we asked them about, we mentioned during a CT scan for her to see what’s up with the lungs, because they’ve mentioned that once the VA was out, when she’s only on VV, that they could do a CT scan and they said that, “Yeah. Why not? Maybe Monday or Tuesday, early next week we’ll do a CT scan and we can take the VV there.” So I assume that the imagined VV to at least beyond till Monday then.
Patrik: Right, okay.
Juan: Unless there’s some rapid changes and improvement.
Patrik: Of course.
Juan: I don’t know, but I think they’re estimating for it to at least be on till then because naturally they don’t do big procedures or anything on a Sunday.
Patrik: Yeah.
Juan: Saturday. It just day after tomorrow.
Patrik: Yeah, no, of course not. Yeah. Of course not.
Juan: So…
Patrik: Yeah.
Juan: Yeah.
Patrik: Yeah. Okay. And, I mean, they have been cautiously optimistic and they continue to be cautiously optimistic, I guess.
Juan: Yes, yes, yes. Very much. And they said to us that, “Oh, her lungs are looking moderate.” Which means that the damage is moderate and that it’s not severe. They’re feeling like moderately confident about it, which is good. And they said that her tidal volumes are good and her PEEP pressure is looking good and she’s giving them good indication. So they’re being, like you said, cautiously optimistic, I think. But they know that her lungs still need some support, for sure.
Patrik: That’s great. I mean, that’s very positive overall.
Juan: Yeah. Yeah. They’re happy with her and her responsiveness. And again, she’s been listening to the nurses and she’s been listening to everyone. She actually told me this morning that she seems to listen in and add to everything that they’re saying. And she gets the sense that she’s very aware about all the conversations happening in the room. That’s what the nurse said to me.
Patrik: Yeah. And she’s still not moving arms or heads?
RECOMMENDED:
Juan: She moves her head. She tries to shrug her shoulders occasionally. When she’s trying to lift off her head, sometimes. She moves her tongue in her mouth a lot. A lot because you can definitely see her trying a lot to talk. She keeps trying to move her lips from left to right up and down, try and stretch her mouth. It seems like she really wants to clean her mouth and say a lot. Basically.
Patrik: Yeah. Okay.
Juan: That’s the most of it. She’s not moving her body much.
Patrik: Right. Okay. Fair enough. That’s probably a concern that she’s not moving enough yet, but hopefully that’ll come.
Juan: They’re doing some passive movements for her arms, no, for the last two days.
Patrik: Yeah.
Juan: I think that’s all why they don’t want to use the paralytics and the sedatives too much anymore. Yeah.
Patrik: Yeah. It’s terrible. It’s terrible.
Juan: Yeah.
Patrik: But I mean, there have been so many good things happening in the last few days.
Juan: Yeah, yeah.
Patrik: It’s been very, very positive seeing what’s been unfolding.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!