Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Isabel as part of my 1:1 consulting and advocacy service! Isabel is worried about the ICU team’s change in perspective regarding her husband’s tracheostomy procedure and she is asking why is the ICU team reluctant to do it now.
I Want My Husband To Have The Tracheostomy Now But Why is the ICU Team Reluctant To Do It?
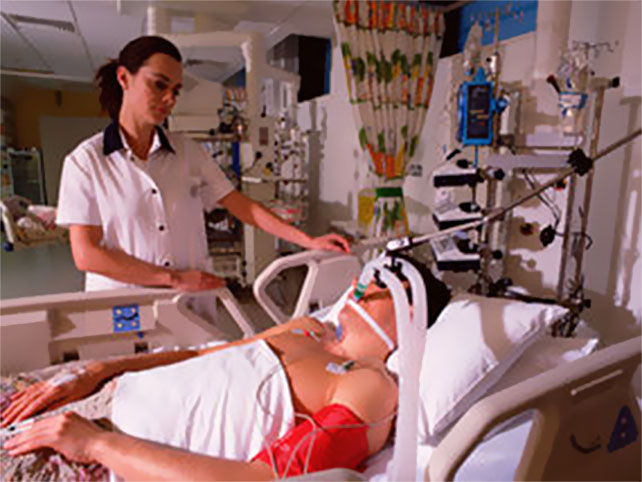
“You can also check out previous 1:1 consulting and advocacy sessions with me and Isabel here.”
Eli: Here’s the thing then, here’s my analytical thinking on that then, if that is the case and it’s 50/50 chance that that is happening, we have to act quickly on the requests that we think can put them in a better position, like the tracheostomy and the second opinion. So, as soon as we can get those in, time is of the essence I guess. We need to ask for that as soon as possible.
Helga: I agree, Eli, I agree. Getting the second opinion, getting the MRI report and then asking for the tracheostomy. Not necessarily in that order, but definitely, I feel like the tracheostomy is important because it’s going to help give them some comfort and even ability to move better. I would even say, whenever you’re calling in and talking to the night nurse to ask them, what physical therapy have you done during this round? What movement have you done?” And if depending on the answer, I would ask them, “Well, could you do it now?” If they haven’t already. Because Patrik has heard that that was physical therapy was part of brain stimuli
Eli: We have to be careful too not to ruffle the feathers and then piss them off and then we’re not able to see what’s really going on behind the scenes.
Helga: But Isabel’s asked them. I’m not saying in a reprimanded way, I’m saying, asking them, the doctor said that they’ve been doing that. We’ve never been told that at all. So Isabel always gets updates from the nurses, they’re really nice and they’ll talk to her and tell her as they’re setting up Zoom, she can ask them in a casual way like, “Hey, what movement has he had today during your care?” and see what they answer. If they say none, then she can request, “Oh, well would you please move him around.” Because that also would give him some comfort too, because if you’re lying there stiff, that’s going to hurt. You don’t get to move. So having some movement makes things a little bit more comfortable. So these we’re talking about suffering. We want to alleviate that as best as possible. The tracheostomy and movement are important.
RECOMMENDED:
Isabel: She did say that he lost a tremendous amount of weight. He lost maybe 35 pounds.
Eli: Yeah.
Isabel: And I told her I couldn’t see that from the angle that they put the camera. I could just see his face and his face looks the same. So I wasn’t able to see that weight loss from his body, but she told me this evening that he lost about 30 to 35 pounds.
Helga: Patrik, why would they bring that up? People do lose weight, right? And my brother was a little bit overweight, tiny bit.
Patrik: Sure. Did you say he lost 35 pounds? Why would they bring it up? I think it’s that you need to bring it up, number one, you should know about it. Number two, they might also highlight the fact that he’s not in a good position, right? So it could sort of underline their point of view. But as you said, most people in ICU lose weight. That’s the reality. And it doesn’t help with recovery, because part of the recovery is to regain weight and that’s difficult. People don’t go in ICU to be fit. Yes, they do get fit, but most patients lose weight.
Eli: Yeah. Thank you, Patrik. Thank you for the insight, and the perspective, and answering all these questions.
Patrik: You’re welcome.
Helga: Yeah, thank you, Patrik.
Patrik: It’s incredibly challenging. As I said, there are no right or wrong answers. There are just right answers for you as a family.
Helga: Okay.
Eli: I think he’s turning around and we have some things that can make a big impact right now with the information that we have from the last two meetings. So, let’s take that and move with some momentum. I think we got God on our side and a lot of good information. So, I’m positive, I’m optimistic.
Aurora: Thank you, Eli. Thank you, Patrik.
Eli: Love you, Aurora.
Aurora: I apologize earlier for leaving. I break down every once in a while. And so it’s really hard to just…
Eli: We got you, Aurora.
Patrik: It’s very, very difficult.
Patrik: Yes I know you feel the pressure about getting the MRI results. You feel pressure about making a decision about the tracheostomy at the same time. If you need another two or three days, give it the time you need as a family. If you feel like you need more time, request more time from the hospital. I agree, things need to be moved forward. I agree with that, but maybe you need a little bit more time to digest.
Eli: But does he have time?
Patrik: He will have a few more days with the tracheostomy. The tracheostomy should have happened after 14 days.
Eli: Okay.
Isabel: Yeah. And that’s when they mentioned it to us at the beginning. And then they kind of shifted. I don’t know why they shifted their point of view on that.
Helga: It is because of the ECMO.
Patrik: ECMO.
Isabel: I don’t know if they had an agenda with changing their perspective, because she was very adamant about the tracheostomy and I was nervous about it, because you know, I didn’t want him to have the scar and stuff, but then when I learned more about it, I was a little bit more at ease and then it just kind of shifted.
Helga: It was no longer an option.
Isabel: Yeah. It’s like it’s out the window, when they were so adamant at first. So I don’t know why they were reluctant to proceed with it.
Eli: It’s opening another airway. That’s the COVID risk.
Patrik: The COVID risk. And number two, when he was on ECMO, he would have been on Heparin, which is a blood thinner. And doing a tracheostomy on a blood thinner is a huge risk for bleeding.
Isabel: Okay. That makes sense.
Patrik: Huge risk.
Isabel: But I think he’s still on Heparin.
Patrik: For the dialysis, yes. But it’s a minimal dose compared to ECMO. ECMO is a huge dose or a higher dose of Heparin, whereas with the dialysis sort of a low dose. They can stop that, they can do the tracheostomy and move on. But ECMO requires a higher dose. Most patients on ECMO don’t get a tracheostomy because they are on Heparin.
Isabel: Okay.
RECOMMENDED:
Aurora: Now, Isabel, you said that the COVID is leaving him. When did they tell you that? Today?
Isabel: This evening, when I brought up the plasma, when I told her that we want to transfer him to another hospital so he could get the plasma treatment. She said that the COVID wasn’t the issue anymore, and that it wasn’t going to help his situation. It was more the brain and the kidney, the renal failure that he’s having than the COVID. Excuse me.
Aurora: I was asking because yesterday it was like it was still there, and like it’s never leaving or whatever. And now today, because you asked for something else, then they say that. So it’s just like they keep…
Helga: Aurora, with his lungs improving now, that’s already a sign though, too, because-
Aurora: That’s what I thought. That’s why I’m questioning it, because yesterday that’s what I had believed from the information. And then, it turned out that, “Oh no, the COVID’s still there.” So it’s like, yes, no, yes, no. He’s okay. No, he’s not. It’s just like a teeter-totter, just bouncing back and forth. We get good news and then it’s like they come up with something else.
Isabel: I think that the COVID, even though it’s leaving his body the way she’s indicating, she did say that the COVID wreaked havoc on his lungs. It damaged them so much that he has to be dependent on some type of ventilation. For the rest of his life. That’s what she said, for the rest of his life. I don’t know why she’s saying that, lifelong ventilation. I don’t know what that means.
Helga: I think that they’re going to put things in their life that, like Patrik said that they’re really good at using, was it euphemisms? It’s just a way to put in a sting of, “Hey, this is going to be forever. Hey, this sucks. Hey, you don’t want to live like this.” So any chance that they get to drop a thing it’s like, they’re not wanting you to visualize life, but when they do, they want to make sure that you see that it’s not going to be pretty.
Aurora: Right.
Eli: Can I say something you guys on all of that? And forgive me for giving it this perspective but, again forgive me for saying it this way, but when you over promise. Or I’m sorry, if you under promise and over deliver, the way the person reacts to that is different. So, what they may be doing is giving us worst case scenario so that we’re ready and prepared, but yet it could be better. And if it’s better, then we’re going to be a lot happier. You know what I’m saying? But if they tell us something that sounds like it’s good, because it sounds good and then the worst happens. We’re not ready for that. So, let’s change our perspective on how some of the things that are being.
Helga: But earlier the doctor that didn’t know said, “I don’t know.” And I would rather them say they don’t know than to say for sure, but even when they’re not sharing, like they’re predicting. Because that’s what it is. It’s all predictions.
Isabel: Yeah. Dani earlier, he got on the call and I let him, because I haven’t been allowing him to be on anything and I just let him. But he asked the question, “On a scale from one to 10, do you see my dad coming out of this? Ever waking up? Ever coming out of this?” And she’s like, “I don’t want to put a number on it because I can’t, but I’ll do it for you.” He said, “I want you to be matter of fact, my mom is not going matter of fact, nobody’s giving me answers. So I need you to be straightforward with me.” And she gave him a one.
Eli: Okay.
Patrik: On that note, what you said Eli in terms of under promising and over delivering. So hospital staff or ICU staff in particular, are trained to cover their downside. That downside is exactly as you said, that they could promise you something and they can’t deliver, you could drag them to the court. So everything they say is phrased in a way to cover their downside. They will never over deliver. The way I described this is, if somebody leaves ICU alive, they will tell you to cover their downside, “Oh, I think he might be back in two days.” It’s just to cover their downside.
Eli: Yeah.
Patrik: So you’ve got to read between the lines. Everything they say is to cover their downside, which is you could drag them to the court if they promise you something they can’t keep and they wouldn’t be doing that.
RECOMMENDED:
Eli: Yeah. I understand. Well again, I’m optimistic about everything and I see him looking better. I mean, something as simple as his hair today looks like it was shampooed or cleaned. And I think that that’s good. His skin, his eyes.
Aurora: I know, I keep telling them. I kept telling you.
Helga: Well, it’s funny you say that because from the very beginning, Patrik, when we first saw him, his look was so dazed and so out that he did not look like himself at all. And from last week, I don’t know when it was, but it was kind of recent. Maybe when he’s out of ECMO.
Isabel: Like when they took him off the ECMO.
Helga: His eyes. He just looked more alive. He looked different. It was really weird.
Eli: Exactly. Yep.
Patrik: When he was on ECMO, his personal care would have probably suffered, because if someone is on ECMO, it’s crazy busy just to manage ECMO, to manage ventilation, to manage medication. So once he’s come off ECMO, they probably had more time to spend on his personal care, to wash him properly. If you’re looking after someone on ECMO, you’re constantly running around, just keeping patients alive. Washing them, looking, shaving them. That’s the last on the list.
Eli: I see.
Aurora: It’s so frustrating that we can’t be there. We can’t see him. We can’t be there to comb his hair or do anything like that. When my brother was dying in the hospital, we were there for the whole week before he passed and I would comb his hair, and we cannot do that with my son and it’s so frustrating that we can’t be there.
Eli: I know, Aurora. We love him. Love you guys.
Helga: What I was saying wasn’t exactly his hair. I was talking about his eyes, his eyes look different. When I first saw him, I didn’t recognize him when he first went there. To recently, I recognized my brother. He actually looked like him. There was something, a look in his eyes, it wasn’t as glossed over. It wasn’t as, maybe the pupils or something, I don’t know. He just looked different. He looked more like himself. And I’m not trying to look for anything. I just was saying that, that was something I noticed that from the beginning, maybe it’s like the medicine or something. I don’t know. I couldn’t recognize him. And now I can.
Eli: Hey guys, I’m sorry to interrupt. My phone’s at 1%, it’s going to die. So I’m going to be here until it dies. But I just want to let you know if I get disconnected. I love you guys.
Aurora: Love you, Eli.
Eli: I’m still here.
Helga: Love you too brother. I think we’ve talked about everything. Wanting to support Isabel, we’re here, you can call Patrik too. When you’re on a call, we have him here and he’s been so helpful. So if they call you, you can call him. If he’s available, he’s going to answer you. Just you have that backup.
Patrik: Please do that.
Aurora: Okay. Thank you, Patrik.
Patrik: You’re welcome.
Isabel: Thank you, Patrik.
Patrik: You’re welcome. It’s very, very difficult.
Aurora: We couldn’t have done this without you, so thank you very, very much.
Helga: We don’t know your faith, Patrik, but really it was like a blessing or a godsend the night that I found your website and I’ve been telling people about you and everyone says, “I didn’t know such a thing existed.” So I’ve been sharing your information. Not that I want them to need you, but just so that they know this is something, because we’ve never heard about this here, ever.
Eli: You know what? I think that’s a huge opportunity there. Send me the link and I’ll share it online. If you don’t mind. I don’t know if you’re open to more.
Patrik: We are open to more pieces at the same time. It’s a very sort of concierge, very tailor made sort of service. It’s only so many people we can serve.
Helga: What I appreciate is just the counsel and the piece about understanding what’s happening, because I know that’s what your website talks about and you educate people with it, but experiencing it first-hand of really understanding what things mean and not being afraid to have the conversations. Because without you, without your knowledge, without that support and education, I think all of us would feel pretty paralyzed and pushed into a corner of like this is what we have to do because this is what they say. And getting that other side allows us to really analyze everything and understand what’s really happening. And so we do feel empowered and it does deliver what you say.
RECOMMENDED:
Isabel: Like that support. I recently started having Helga on the calls, because it was too much. It’s almost been a month and getting the daily updates and texting everybody the information. And then, it mentally was affecting me emotionally, and I couldn’t do it anymore by myself.
Patrik: As you can see the burden of just listening to the information and then being pushed to make a decision is huge. Just absorbing the information is massive and then. Let alone, what are the right decisions? You know? It’s huge.
Isabel: Yeah, yeah. Yeah. So thank you, Helga, for just being there for me and helping me through it. Because you know, it’s hard. It’s hard. I have cried, like I want to say 25 days straight. And honestly like my tears are just, I’m just numb now. I have no feeling in me no more. But I couldn’t do it without your help, Helga, and Aurora, and everybody. Eli too. And your brother Jonah.
Helga: And when those keep happening too, like when the calls, remember call Patrik, if he’s not able to call me, call whoever. I don’t want you to do those alone, please. I want you to have somebody there to help you, because it is a lot. Even the time that I’ve been helping you, I’ve felt it. And I’m not even in it the way you are. And it’s been a lot. So, just know we’re all here. And we have Patrik, who we trust to tell us the truth, and then we can just make our decisions together, okay? You’re not alone.
Isabel: Okay.
Helga: Okay. Was there anything else you wanted to ask, Isabel? Because I would think I’m ready to talk to you separately.
Isabel: Okay.
Helga: I just want to be respectful. I don’t know. I know that we’re not the only people Patrik helps, so I feel sensitive to making sure he’s available for other families.
RECOMMENDED:
Patrik: We can leave it here.
Helga: Okay. Sounds good. I’ll talk to you, Isabel.
Patrik: Thank you. Take care.
Isabel: Thank you. Bye-bye.
Patrik: See you, bye.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!