Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question last week was
You can check out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to feature another case study with one of our clients and the case study this week is
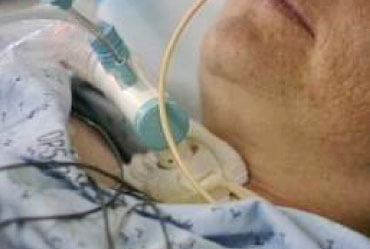
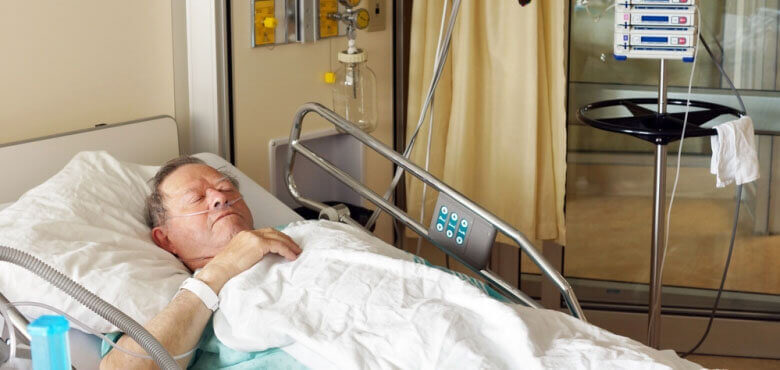
CASE STUDY: My brother is in Intensive Care after stroke and cardiac arrest, he’s off the ventilator now, will he get out of ICU alive?
This is another great case study and an excerpt from a 1:1 phone counselling and consulting session with me, where Linda, a concerned sister wants to find out if her brother is going to be OK after a lengthy and difficult stay in Intensive Care, where I can provide some insights and reassurance!
We talk about the impact of cardiac arrest and also why BIPAP ventilation might be enough to get her brother out of ICU alive!
Go and check it out yourself here.
Linda: Hello?
Patrik: Hello, is that Linda?
Linda: Yes it is.
Patrik: Good morning.
Linda: Hi, is this Patrik?
Patrik: Yes, it is. Good morning, how are you?
Linda: Hi, good morning. I could be doing better but I’m doing well. Thank you for asking. Did you get the audio recordings of the meetings we have had?
Patrik: I did, and I just listened to it and it sounds to me like your brother has a long-standing medical history on top of everything that he seems to be going through at the moment.
Linda: Yeah, I think that I went off the plane in November 30th, which I can’t believe it was only five months ago. I think he was a lot sicker than I thought. That’s why his caseworker called. It was because he was going from ER to ER and non-compliant.
Patrik: Mm-hmm (affirmative).
Linda: And you know, coming out here and seeing my mom and dad after two years, it just didn’t work out so well for my mom but my dad is still here in town.
Patrik: Sure.
Linda: But he just coded on last Thursday and we happened to be there. I would have probably found him, if it hadn’t been within the cafeteria. Give it to me straight Patrik…
Patrik: I probably have enough information to get through what I can see within the next hour or so. Also my next question is, are you the medical power of attorney for your brother?
Linda: I do have it. Right now my Dad is out of the country in Mexico, but the counsellor who had the durable one, she signed it over to me on the 12th, on Friday.
Patrik: Right, so you have decision-making authority?
Linda: I do. Temporarily, until my dad moves back and would do the notary and all that. He’s out of the country but hospital … He’s already talked to the hospital administration. Yes, I do have durable power of attorney.
Patrik: Okay great! Look, with everything that you’ve told me in the recording and also in the voicemail that you left, I’d say there are a lot of things that are not in favour of your brother. However, in order to make the call from my end, I would really need to know what are they doing at the moment. Just looking at medical history, diet, Type 2 diabetes, seizures, cardiac surgery, code on the 10th of May, hemothorax. Then he’s had the pulmonary edoema, he’s got congestive heart failure, PVD, there’s anaemia.
So there is a long list of things that are not in your brother’s favour, there’s no question around that. The questions is, and I’m not sure whether you can answer that for me, what are they doing at the moment? Do you know?
Linda: Well, I did take photographs every day of their board because I just got power of attorney on Friday, right?
Patrik: Right.
Linda: For instance, I can look at … just let me open it up here, what they’ve been doing and some of it I didn’t understand and I didn’t know where to maybe send you the photographs but I can show you a programme, I’ve got like a 100 drives here. Okay, there we go … let me see … all right. I have on day … let me see here … day 18 vitals, I can show you what it looks like on… day 18 would have been … hold on one moment … day 18 is right around two days ago, it would have been Saturday, okay? Today is Tuesday?
Patrik: Yep.
Linda: ‘Cause they weren’t letting me take pictures but I did anyway.
Patrik: Yep.
Linda: And she says “108” … looks like a … let me see here … hard for me to tell. I’m the younger sister, I’m only
Patrik: Right.
Linda: It says his blood pressure is 150/71 with a … looks like a heart machine, I think but we have … let me go back here.
Patrik: Right.
Linda: We have Sunday. Sunday the 14th, it’s says, “Foley 0600, Foley initial OP, 40% FIO O2.
Patrik: Yep.
Linda: And then his weight, 89.1 kilogrammes.
Patrik: Yep.
Linda: And then it says under here, “care for the patient 92 kilogrammes” … it’s kinda hard to see here.
Patrik: Do you know what medications he’s on?
Linda: I can get them. Today, I’m gonna go back to ICU!
Patrik: Right. Is he … he’s still, he’s still in an induced coma, is that correct?
Linda: No, he’s not. Yesterday they did a CPAP and I was gonna do some internet studying to find out what a BiPAP was to a CPAP, right?
Patrik: Yep, I can-
Linda: But they don’t have the tube down his throat.
Patrik: Okay.
Linda: That happened on Saturday.
Patrik: Right, that’s good. That’s encouraging. So he’s awake?
Linda: Yeah, he was awake. He couldn’t really talk too much.
Patrik: Right.
Linda: But he was doing the treatments where you did the machine that has the wet and dry.
Patrik: Right, yeah.
Linda: It has a tube and you use that thick BIPAP mask and they performed dialysis yesterday, 2700 litres, I don’t know what that means. Like I said, I hadn’t seen my brother in 20 years and when I went out and got him at the end of November I learned everything about dialysis, brand new to me.
Patrik: Yeah, absolutely.
Linda: Okay, so it said performed dialysis yesterday around five o’clock, took 2700 litres and some physical therapy and he has that thing where you have to blow with the ball in the middle.
Patrik: Yep, that’s encouraging.
Linda: He gets really excited and then I think he had a stroke, which is why he coded last Thursday.
Patrik: Mm-hmm (affirmative).
Linda: And it seems like he’s been having seizures. The caretaker, who really wasn’t supposed to keep on the case but she really liked him a lot, said that he had died so many times in Omaha and that’s why we went out there and got him was ’cause I guess he’d been to every emergency room and they were not gonna treat him anymore because-
Related article/video:
Patrik: Why?
Linda: He would get out, he just, he just go back to just doing nothing. Sadly, my brother spent quite a bit of time of his 55 years in and out of the penitentiary, starting around 20 years old, three years here, four years there, that type of thing. Then he got sober with the Siena/Francis House and that took about two-and-a-half years. Got his SSI, went to the doctor and he had about just 14 … about two years ago I have a picture of him working for Omaha painting the city mural, working and you couldn’t believe that two years ago he was very healthy and then down he went, but he continued to smoke cigarettes but I don’t think anymore ’cause he can’t even get out of bed…
Patrik: Right, but I can tell you even that I now have an understanding of your brother’s pre-medical history, and given that I now hear your brother is off the ventilator, that, to me, is very encouraging. I get from everything that I know so far what stands in your brother’s favour is probably his age, 55 years of age is not very old. That probably works in his favour even though he’s got the Type II Diabetes, he’s got the kidney failure, which sounds to me like he has been managing fairly well if he was on home dialysis.
He’s got a very long list of medications, there’s no doubt about that, but given that you’re now telling me he’s off the ventilator, they’re doing physical therapy, they’re doing the CPAP, that, to me, is very encouraging.
Now with the cardiac surgery that he had recently and also with the coding, I would really want to know what is his heart doing. Is he still on medications for his heart? What’s their outlook in terms of his heart, especially with the view of recent cardiac surgery and the code. I think that almost make or break his future.
Linda: Okay, we just found you … just like the night he coded I think, just miraculously found you on the web so we’ve only gotten to listen to My 57 Year Old Dad Has Been In Intensive Care With Cardiomyopathy And Pneumonia For 5 Weeks! He’s Still In An Induced Coma And Still Doesn’t Have A Tracheostomy, HELP! (PART 7), okay? At that point there’s a lot of poly-trauma, which you’ve kinda taught me. You said get to know the lingo and now that I’ve got the durable power of attorney I can go in there and you did say that most ICUs are concentrating on the heart no matter what kind of call they get, correct? Because the heart is really the epicentre of what makes the body work.
Patrik: It does and also, now your brother has chronic renal failure, but for example, if you have a patient who is going into heart failure and doesn’t have kidney failure, if the heart is not working, the kidneys are the first organs that fail. That’s why a lot of ICUs are focused on the heart, just to put this in perspective.
Linda: Okay, so I should start looking for what are they doing to his heart?
Patrik: Yeah, what are they doing … so with his heart, for example, ask them whether they’ve done an echocardiogram of the heart, which they probably would have.
Linda: Okay.
Patrik: And as them whether he’s still on vasopressors? Have you heard of vasopressors or inotropes?
Linda: Say that one more time?
Patrik: Vasopressors. V A S O-
Linda: I think I have. V as in Victor, vasopressors?
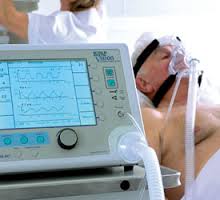
Patrik: Yeah, V A S O P R E S S O R S. So, vasopressors, it’s a form of life support. So up until a few days ago, where your brother was still on a ventilator. Ventilation obviously is life support and given that the ventilator is off now, at least with the breathing tube, that’s one form of life support taken away, okay? That’s good. That’s good news.
Now, vasopressors are another form of life support. Basically, vasopressors and mechanical ventilation are the two most commonly used forms of life support in intensive care.
Linda: Okay.
Patrik: So ask them whether he’s on any vasopressors, ask them whether they’ve done an echocardiogram and ask them what is his ejection fraction.
Linda: Injection fraction?
Patrik: Nope, ejection, E J E C T I O N.
Linda: Yeah, like injection, like a-
Patrik: But with an E at the beginning, not I N, with an E. E for Emma.
Linda: Okay.
Patrik: Ejection fraction.
Linda: Okay.
Patrik: Because that’ll give you an indication in how well his heart is working. Ejection fraction should be above, ideally above 50%. If he’s on inotropes, if he’s on vasopressors, the other term for vasopressors is inotrope, there’s a very good chance that his ejection fraction might be below 50% but you’ve gotta ask that and hopefully they’ve got the answer for that.
Linda: Okay, and what, 50% is good or not good?
Patrik: No, 50% would be relatively average, would be relatively average. Anything below 35-40 % is concerning
Linda: Okay.
Patrik: The other question that may come up, not maybe today, but down the line, just to prepare you probably … Have discussions been held about do not resuscitate or any of that? Has that been brought up?
Linda: Well he did say “no” but not really according to the hospital administration, the family did, but Peter already has it down that he wants whatever is necessary but not long-term life support.
Patrik: Okay, good.
Linda: I guess he picked full treatment but I was understanding that the DNR is something that the hospital started to probably do.
Patrik: Look, it’s a two-way street. Sometimes the hospital brings it up, sometimes families bring it up. I guess it’s good that-
Linda: I did note you did say do not ever agree to reduction in care?
Patrik: That’s right.
Linda: And then you reiterated that in videos, so I’ve got that down in my mind!
Patrik: Yeah.
Linda: So there’s a red flag there if they start go that way.
Patrik: Yeah, it’s a red flag.
Linda: Well, I’m not going to be intimidated by it and some of the people there are just awful and my sister is not in, it’s her job. It’s really hostile, it’s a hostile work environment and they did kinda treat me that way but now that I’ve got the direct power of attorney, what are they gonna do?
Patrik: Mm-hmm (affirmative).
Linda: So those are the things you said to watch out, no reduction in treatment. They haven’t talked about a DNR and of course, Peter hasn’t because he is 50 and he has a lot of stamina.
Recommended:
Patrik: Well, it sounds like-
Linda: A lit bit stubborn. He says, “I’m gonna be walking in a week and then he has a stroke or something that they thought was just a minor event.
Patrik: No, no, that’s fine. Look, what I want to do really is I want to lay out if you want to have … so what we tend to do is like… I could also talk to the doctor and the nurses, including participating in family meetings, if that’s what you want, right?
Linda: Okay.
Patrik: We can do all of that. I guess, from my perspective, we’re just scratching the surface here, but I think you’ve got enough questions now just to ask them. The heart is going to be a very important aspect in all of this, as was just discussed because if they think his heart can recover, then I think, even though he’s got a lot of other issues, then I think he’s got a really good chance of getting out of intensive care alive. I think it’s very positive to hear that he’s awake. That’s very positive.
Linda: Yes, I think it is too.
Patrik: Very positive.
Linda: What I wanted to give you a compliment. I think that you look like Yul Brynner, but you have a dimple on your chin that’s even cuter.
Patrik: Right.
Linda: Yul Brynner is? “The King and I”?
Patrik: Say that again?
Linda: “The King and I” it’s Broadway, Yul Brynner?
Patrik: Right, yes. Oh you’re very … yeah, yeah, Oh yeah, some people have said that before, year.
Linda: You look like Yul Brynner but like the dimple in your chin is better than Yul’s. I had to tell you that ’cause I’ve seen your face a lot in your videos.
Patrik: Well you must have watched some videos then. Some people prefer to read, some people watch the videos.
Patrik: Yes.
Linda: I watched through seven so far.
Patrik: Right.
Linda: And then just picking up the lingo along the way, you know, assertive.
Patrik: You know, this is my advice. Obviously, my time is valuable but at the same time, what I keep saying to people is, if you watch the videos or read the blogs, you got all the information you need. There’s 100s of videos on the website and blog posts, questions answered over and over again, you get all the information. If you want me one-on-one, you get the answers much quicker and I can … if we spend an hour on the phone, I can tell you this, this, this, this, and this. You can go back with those questions to the doctors and I would also be very happy, I would be very happy to speak to the doctors directly, we can do a three-way call, for example, where you are on the phone as well.
As I said, I think one of the biggest leverage points that I can see is when it comes to family meetings, being there over the phone, I think that really helps, but that’s food for thought for you. Part of my 1:1 counselling, consulting advocacy package is to talk to doctors and nurses directly if you wish.
Linda: You work pretty cheap really for what you do. I not sure we’re gonna need that yet. I think I’m OK just talking to you for now as part of your engagement! You’re right, your videos … I only watched seven of them and I’m already starting to learn like the levels of acuity, how you’re speaking and the CPAP and all that and everything. So I don’t know if we’re gonna do that yet.
Patrik: Oh, that’s fine.
Recommended:
- 1:1 email counselling and consulting with Patrik
- 1:1 phone and email counselling and consulting with Patrik
Linda: Depends on how … like … but I don’t … I saw the cardiologist once and happens to be he’s the Chairman of Cardiology at Desert Springs and he’s been there for eight years, but he’s got his own practises and doing his own thing. I saw him in the hallway four days after he did my brother with the trapped lungs, and he was on the phone, but when I talked to Martin, he didn’t even look up, but I think he’s even trying to get out of there, kinda like a famous person. Again, I think the cardiologist should be consulted, you said, every time that there’s a crash or incident, right?
Patrik: Absolutely.
Linda: We were there when he crashed last time and they said, “Page Dr. Martin,” but that doesn’t necessarily mean he’s been consulted. There are so many codes in these other files that I’ve gotten from Arizona and the one from Omaha, how do you know how to figure this stuff out?
Patrik: So, do you have access to the medical notes?
Linda: I’m going to get them today.
Patrik: Right. Well, this is another thing that we do quite frequently for clients. We review medical notes.
Linda: Okay.
Patrik: Right. It’s another part of the service that we’re doing.
Linda: Okay, yeah, I’d like to wait till my dad gets back in the country.
Patrik: Yeah, absolutely, you make … of course. I understand that.
Linda: Some people said “I don’t think he is. Geez, he’s only 55,” and he had some drug use when he was in prison and stuff but from what I’ve told you, like I said, the guy who did it is the head of cardio. I don’t know if I’ve seen him but I’m gonna get in the files today. Like I said, on Friday I just got the durable power of attorney signed over to my dad and then he called the hospital administrator and said, “While I’m out of country, Linda is going to act as the durable power of attorney.” So I’m gonna take my husband, who’s a computer software programmer and he’s just probably gonna take… then we’ll come home and print them up ’cause we’re getting … we had to say, “Hey, can we use your Xerox machine?” ’cause they’re really not great.
The other thing was that I didn’t know anything, but the weird thing is that on March 24th my girlfriend died there, so I had be like in the same ICU room, just a couple doors down and she died of complications of emphysema, so I’m gonna quit smoking. This is it. I can’t take it anymore…
I did learn a little bit about ADs and DNRs because her daughter was so young and so that was like practise. I was like, “Jean, please don’t leave me,” and she said, “Well, the big one is gonna be coming next.” I didn’t know that he was gonna be flying up here where … you know, in an ambulance from Bullhead City Arizona right into the hospital where she was at. I’m ready to go and I love my brother a lot so I thank you so much.
Patrik: You’re most welcome. You’re most welcome. You know where I am. You can call me anytime as part of your 7 day 24/7 unlimited 1:1 phone counselling, consulting and advocacy package
Linda: Okay.
Patrik: You know where I am. You can always call me and then we can move on from there.
Linda: If I had been an RN in your field. I would have done something like this because you’re reaching and helping so many more people. I don’t know how you do it.
Patrik: I love it. I love it, absolutely love it.
Linda: You can tell. You can tell.
Patrik: That’s good.
Linda: I’ll put it this way. If you’re ever in Los Vegas, okay?
Patrik: Yep.
Linda: I have my uncle, owns this best and largest talent agency so I get tickets to a lot of cool shows and stuff.
Patrik: Okay,I’ll keep that in mind. I’ll keep that in mind. I will be in Los Vegas one day, for sure.
Linda: Oh, I’m sure you will be. You seem like a world traveller.
Patrik: I am.
Linda: I’m serious too. You look me up and hopefully, I’ll let you know.
Patrik: As I said, if you keep browsing the website, if you keep reading the newsletter, you get basically all the information for free, but if you call me, it’s just much quicker, we can cut through the chase very quickly.
Linda: All right. Like I said, also too, when my girlfriend died, one of the charge nurses that’s on my brother’s floor, his name is Bill he’s a … I believe … I don’t know, Vietnamese, just really cool. He said, “If there’s anything you need, Linda, come to me.” So I plan to take photographs of his file and bring them on into Bill and say, “Tell me about the heart part,” ’cause he does look at them but he thought that actually I was my girlfriend’s daughter because, like a lot of people, she was abandoned by … nobody cared and I was down in Georgia for a month, helping out with my brother and so I’ve got a good couple of allies there, just one of two, they took me aside and said, “If you need anything at all, I’ll help you.”
This guy was … because I came and I did see my girlfriend and no one else did and they were like, “Hey, how do you get a hold of her daughter?” and I gave them the information and they said, “Okay, well, if you can’t get power of attorney, if she shows up, if she does die, we’ll call you,” and Bill did. He just happens to be the night charge nurse for my brother so this is really good and he’s kinda helping me on the outside. So we’ll see how it goes. I’m glad that you say though that … Patrik, that everything is … sounds like it’s getting better now that he…
Patrik: It sounds like to me, but as I said, we’re only scratching the surface here. I would really … in order to be really sure about what is next, I would need to know what medication is he on. Also, what has he been getting, what does the echo show and that sort of stuff.
Linda: Okay. All right. Yeah, okay, Patrik, I will call you tomorrow at 5pm.
Patrik: Ok let’s talk then! Thank you very much, have a good night!
Linda: You too!
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!