There are several different types of Units in Hospitals in general that offer care to those Patients that are critically ill and require Intensive Care. Usually the terms such as ‘Intensive Care Units’, ‘Coronary Care Units’, High Dependency Units’ and even ‘Specialised Intensive Care Units’ are used. Some units have all these different specialities combined.
This page aims to eliminate some of the confusion that might result from these different terms. This page will shed some light on all these terms and the page also links to conditions, treatment and equipment used in Intensive Care
- What is an Intensive Care Unit (ICU)?
- What is a Cardiothoracic Intensive Care Unit (CICU)?
- What is a Neurosurgical Intensive Care Unit (NICU)?
- What is a Coronary Care Unit (CCU)?
- What is a High Dependency Unit (HDU)?
What is an Intensive Care Unit?
Each year hundreds of thousands of patients are admitted into Intensive Care Units (ICUs) worldwide. These units are designed to deliver the highest of medical and nursing care to the most critically ill Patients. Some smaller rural and urban hospitals do not have Intensive Care units while larger metropolitan hospitals may have a number of specialised Intensive Care units.
History
Intensive Care is a relatively new concept, as only after World war II, during the 1960’s and early 1970’s doctors recognised the life-saving potential of placing Patients into specialised areas called Intensive Care Units. The purpose of these units was to provide high leverage and intensive management for Patients following major injury, illness or after major surgery.
Your first Impressions of an Intensive Care Unit
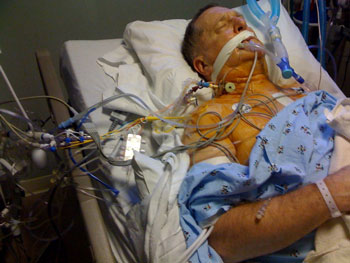
Physically, most Intensive Care Units are large areas with a concentration of specialised, technical equipment and monitors needed to care for the most critically ill Patients, including your loved one. Access to the unit is often limited, not only to Families, but also to other non-ICU staff members. The ICU has a higher ratio of doctors and nurses to Patients than found in other areas of the hospital, as it is such a highly specialised area.
Every Patient, including your loved one, in ICU has a monitor (a television-like screen) that can monitor your loved ones heart rate and rhythm, blood pressure, temperature, breathing and many other things. Most Patients will have powerful drugs given to them continuously through intravenous infusions (‘I.V’ or ‘drip’). Your loved one may also be assisted in their breathing by a machine (ventilator). They are attached to the machine by a tube (ETT) inserted into the Trachea (windpipe).
For most Families of the critically ill ICU Patients there is no previous knowledge of Intensive Care conditions, treatment, equipment and procedures. You and your Family as the visitors of your loved one in Intensive Care can be confronted by a lot of activity and noise which can make the environment alien and frightening and you are very likely feeling out of your comfort zone. One of the most concerning and confronting aspects of being in the ICU are the alarms as they seem to go off regularly and come from all around. Almost all ICU equipment uses alarms. However, it is important to remember that most alarms do not signal an emergency, but rather, they assist nursing and medical staff in providing better care by letting the staff know that the your loved one needs closer attention.
You will also find that you are out of your comfort zone and that generally other people are making decisions for you and your loved one. This can be quite confronting and you may feel powerless. INTENSIVE CARE HOTLINE’s goal is to educate and assist you with the information accessible on this website to help and guide you through one of the most difficult or even traumatic times in your life and we hope we can put things in perspective for you so that you feel less outside of your comfort zone. We also want to help you how you can negotiate with the staff in the Intensive Care Unit, as there are a lot of things going on behind the scenes that you are unaware of, but that can sometimes have an impact on you, your Family and your loved one.
Visiting Family in the Intensive Care Unit
Visiting in some units may be restricted in the interests of both your loved one’s and your family’s safety and to allow staff to continue the high intensity care required. If your loved one has children, they may be allowed to visit. We advise to discuss with a senior registered nurse or a social worker as to how this visit may affect your child. Visiting hours are usually during the daytime with some units having a ‘quiet-time’ (no visitors) during the middle of the day. Exceptions to these general rules may be made in consultation with senior ICU nursing and medical staff. At times there may be some special requirements to control infection.
Having restricted visiting times, may in some instances also hint towards the culture in a particular unit. My personal view after 13 years Intensive Care Nursing in different countries is that there shouldn’t be any restrictions. My view is that nobody should have anything to hide in Intensive Care in what they are doing. And yes, sometimes other Patients need quiet time, too. However, if you and your Family conduct yourselves appropriately, being with your loved one is very important and should not be at the discretion of the Nursing or the Medical staff. There are of course situations, where for safety, privacy and dignity reasons visiting would be detrimental, but this should not go on for a very long time and disruption of visiting times should be at a minimum.
The Cardiothoracic Intensive Care Unit (CICU)
The Cardiothoracic ICU (CICU) cares for Patients who need heart (cardiac) and chest (thoracic) surgery. Surgical procedures may include operations on the heart, the heart’s blood vessels, the chest or the lungs.
If your loved one is in a Cardiothoracic Intensive Care Unit, he or she will require continuous monitoring of the heart and may require insertion of a PA Catheter (Pulmonary Artery Catheter or Swan-Ganz Catheter) or an Intra-Aortic Balloon Pump (IABP).
Some cardiothoracic Patients, including your loved one, for a short time after their operation, may require a ventilator(breathing machine) to assist their breathing. This means they will be attached to the machine by a tube in the Patient’s mouth (or nose) to the windpipe (trachea).
Most cardiothoracic Patients are only in the CICU for 1 – 3 days. Some Patients may need a longer stay. A few Patients may not improve as quickly and may require transfer to the general ICU for further management or they may be treated in the CICU long term.
There are very few or no cardiothoracic Intensive Care Units in rural areas. Patients requiring cardiothoracic surgery will usually be transferred to major teaching (tertiary) hospitals in metropolitan areas.
The Neurosurgical Intensive Care Unit (NICU)
The Neurosurgical Intensive Care Unit cares for Patients with brain or spinal cord conditions and occasionally other medical or surgical problems.
Many hospitals combine the specialised care of neurosurgical Patients with that of seriously ill trauma Patients and manage the Patients in the Intensive Care Unit. However, some hospitals separate Patients who have had neurosurgery into a specific area.
Reasons for admission to a NICU include conditions such as:
- head injuries(from traumas such as car accidents, assaults, falls)
- strokes (cerebrovascular accident or CVA)
- vascular (blood vessel)surgery, e.g. aneurysm (weakness or bulging of an artery) repairs and infections
The Neurosurgical ICU and Intensive Care Units that have neurosurgical services provide brain and spinal cord monitoring and treatments that are specific for the neurosurgical Patient. For example, continuous electroencephalogram (EEG) monitoring, intracranial pressure (ICP) monitoring and special spinal cord stabilization techniques are available.
In rural hospitals, many Patients with head injuries that do not require surgery are cared for in the local hospital’s ICU. Those Patients with a severe neurosurgical condition that is likely to need surgery will usually be required to transfer to a major teaching (tertiary) hospital in metropolitan areas.
What is a Coronary Care Unit (CCU) ?
The Coronary Care Unit or CCU cares for Patients who have heart disease and occasionally other medical or surgical problems.
Conditions such as myocardial infarction (heart attack), angina (chest pain), congestive heart failure (CCF) and arrhythmias (abnormal heart beats) are common reasons to be admitted to CCU.
Your loved one may have come to this unit following procedures such as cardiac angioplasty or the placement of stents in their coronary blood vessels.
The CCU provides the ability to monitor the heart’s rhythm continuously and to use specialized treatment such as thrombolytic therapy (medication that dissolves or breaks-up blood clots). Some tests such as electrocardiography (ECG) may also be performed within the CCU.
Most Patients, including your loved one, within the CCU can breath without the assistance of a machine (ventilator) – though most will require oxygen (either by nasal prongs or mask). Some may require Non- invasive ventilation with special masks that assist breathing and oxygenation (CPAP or BiPAP machine).
In most rural hospitals the Coronary Care Unit is often combined with the Intensive Care Unit and the High Dependency Unit to form a Critical Care Unit. In Metropolitan areas, where the big teaching hospitals are located, Coronary Care Units are specialised units usually separate from the Intensive Care Unit.
If your loved one is in CCU and requires an operation on their heart or heart vessels (cardiac surgery), he or she will very likely be transferred to the Intensive Care Unit (ICU) or Cardiothoracic Intensive Care Unit (CICU) after surgery. In the rural centres, this means your loved one will generally need to be transferred to a metropolitan unit prior to surgery.
What is a High Dependency Unit (HDU) ?
If your loved one has been admitted into the hospital, he or she may require a level of care that cannot be provided on a general ward but does not require admission into an Intensive Care Unit. This area is often referred to as the High Dependency Unit (HDU).
At the same time, Patients in the Intensive Care Unit who have had an improvement in their condition may also require a stay in the High Dependency Unit (HDU) before admission to a general ward.
The HDU is similar to ICU except that Patients admitted to the HDU are usually less ill or beginning to recover from their operation. There may be fewer nurses and doctors than in the ICU because the patient is not as ill and does not require as much treatment.
Similar to the ICU, Patients in the HDU are monitored frequently, assessed daily and the need for continued HDU care is continuously re-evaluated.
In most rural hospitals the HDU is a part of the ICU. In major teaching hospitals in metropolitan areas, the HDU can either be a part of the ICU or a separate unit altogether.
Related Articles:
- How long does a cardiac arrest patient stay in Intensive Care?
- Six weeks in Intensive Care after Cardiac Surgery and my mother isn’t getting any better
- How long can a breathing tube or an endotracheal tube can stay in?
- How long should a Patient be on a ventilator before having a Tracheostomy?
- How long is a Patient kept on a BIPAP machine in Intensive Care?
- What is an induced coma and why is my critically ill loved one in an induced coma?
- The 3 most dangerous mistakes that you are making but you are unaware of, if your loved one is a critically ill Patient in Intensive Care
- How to always achieve your goals whilst your loved one is critically ill in Intensive Care
- Why you must make up your own mind about your critically ill loved one’s situation in Intensive Care even if you’re not a doctor or a nurse!
- Follow this proven 5 step process on how to be in control and influential if your loved one is a long-term Patient in Intensive Care
- How to quickly take control and have real power and influence if your loved one is critically ill in Intensive Care
- Why does my loved one need a Tracheostomy in Intensive Care?
- Tracheostomy and weaning off the ventilator in Intensive Care, how long can it take?
- My sister has been in ICU for 21 weeks with Tracheostomy and still ventilated. What do we need to do?
- Severe lung failure and my aunty is not expected to survive…
- 3 quick steps on how to position and prepare yourself well mentally, whilst your loved one is critically ill in Intensive Care
- How to get what you want whilst your loved one is critically ill in Intensive Care
- 5 steps to become a better negotiator if your loved one is critically ill in Intensive Care
- How to make sure that your values and beliefs are known whilst your loved one is critically ill in Intensive Care
- How to make sure that “what you see is always what you get” whilst your loved one is critically ill in Intensive Care
- What the doctors and the nurses behaviour in Intensive Care is telling you about the culture in a unit
- How long does it take to wake up from a Traumatic brain injury or severe head injury
- How to take control if your loved one has a severe brain injury and is critically ill in Intensive Care
- Family Meetings in Intensive Care or the Elephant in the Room
- What you need to do if your loved one is dying in Intensive Care(part one)
- What you need to do if your loved one is dying in Intensive Care(part two)
- Intensive Care at its best?
- How INTENSIVECAREHOTLINE.COM Can Help You
- What you and your Family need to do if your critically ill loved one is very sick in Intensive Care and faces an uncertain future
- How long can somebody stay in Intensive Care?
- My Family can’t agree on what’s best for my sister in Intensive Care…Help!
- My husband is dying in Intensive Care, but we need more time…
- My mother sustained serious brain damage after a stroke and she now is in multi- organ failure


