Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
What Should We Expect if Our Critically Ill Mom in ICU Will Finally Come Off ECMO?
You can check out last week’s question by clicking on the link here.
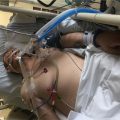
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Juan, as part of my 1:1 consulting and advocacy service! Juan’s mom is with a tracheostomy, balloon pump and is on ECMO. Juan asks if the ICU is being open and transparent on how they manage their critically ill mom in the ICU.
How Do We Know if the ICU Team is Open & Transparent on How They Manage Our Critically Ill Mom in the ICU?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Juan here.”
Patrik: Hi, Juan. How are you?
Juan: How are you?
Patrik: I’m very well. Thank you. What’s the current update for your mom now?
Juan: She tolerated the V-A removal well.
Patrik: Great.
Juan: She was mostly steady through the night and she’s quite steady right now.
Patrik: Right, but-
Juan: Yeah.
Patrik: That’s great. So, but you sent another picture from the ECMO. Is she now on V-V ECMO?
Juan: That’s right. So she was on-
Patrik: So this picture is V-V?
Juan: First she was on- Yes, yes. It’s V-V.
RECOMMENDED:
Patrik: I see. I see. Okay, well that’s good. And they’ve reduced the balloon pump to 1:2, which makes sense.
Juan: Yeah. And maybe they’ll try and reduce it to 1:3?
Patrik: Yes, that would be the next step. That would be the next step.
Juan: Yeah, and we just spoke with the doctor. And he said that he’s reduced the inotropes further.
Patrik: Wow.
Juan: After we sent you those pictures.
Patrik: Great.
Juan: And that they’re hoping to remove the IABP tomorrow.
Patrik: That’s fantastic. That’s fantastic.
Juan: Yes.
Patrik: And have they done an echo?
Juan: Yesterday they didn’t, but maybe today they will. We’ll check if they’re doing one.
Patrik: That’s fantastic. That is such great news. But your mom, looking at the pictures, it looks like your mom is back on the dexmedetomidine, the Precedex. How awake-
Juan: So, this is the first time she’s been, I think since the ECMO, she’s been given dex… Hold on.
Patrik: Dexmedetomidine?
Kevin: Hi, Patrik.
Patrik: Hi.
Kevin: What they did was they, because through the night she kept opening her eyes and she was fighting the ventilator.
Patrik: Right.
Kevin: So it was better, rather than adding midazolam or atracurium, they added dexmedetomidine infusion.
Patrik: Yep.
Kevin: And they increased the fentanyl slightly, so that she could go to sleep and not… because she keeps trying to talk right now, you know?
Suggested links:
Patrik: Yes.
Kevin: She’s obviously making conscious and wanting to talk, so.
Patrik: Okay. Well that’s really, that’s very positive overall. I have seen that they changed the ventilator settings slightly. Just give me one second. I just quickly need to compare the last ventilator picture with the one that you sent through. Yes, they have changed the ventilator settings quite considerably.
Patrik: So she was on 60% yesterday of oxygen and she’s still on 60%, but they changed her breathing rate from 12 to 18. And they have changed her from a volume control mode to a pressure control mode, which I actually think is a good thing. It puts her at less risk of a pneumothorax. Do you know what a pneumothorax is?
Juan: No.
Patrik: It’s basically a hole in the lung. Not that she’s got that, but with that ventilation mode, now she’s at risk of a pneumothorax. I like that. I like that. I don’t know why they changed them. It probably has everything to do with her having now V-V ECMO.
Juan: So actually, Patrik, something I wanted to tell you yesterday that we realized is that I think, you know when you said that maybe there’s something that they’re not telling you?
Patrik: Yeah.
Juan: And that’s kind of guiding the direction? I think they were hoping that maybe they could take off the AV ECMO altogether.
Patrik: Yes, yes.
Juan: Both the V-A and the V-V. I think that’s what they were hoping for. But then they realized that they couldn’t take off the V-V, but they didn’t want to raise our hopes.
Recommended:
Patrik: Yes.
Juan: So they didn’t really tell us that that’s what they were assuming they would be able to do.
Patrik: Yes. I tell you what you should be looking for as a next step. You should be looking for an arterial blood gas again. You should be looking for-
Juan: The blood gases?
Patrik: Yes, yes. Because that’ll indicate to you whether she can come off V-V ECMO or not.
Juan: Okay.
Patrik: That would be my recommendation to look for now. Yeah. That’ll tell you a lot. I am still worried. I’m still a little bit worried. So the last cardiac output you sent through from the PA catheter?
Juan: It was 3.1 I think, today. From yesterday.
Patrik: That’s very low. That’s very low.
Juan: Hmm.
Kevin: But they don’t seem that concerned because they’ve reduced the flows on the ECMO as well.
Patrik: Yes. Understood. However, have they, they were talking about the PiCCO (Pulse index Continuous Cardiac Output) yesterday. Has that happened?
Kevin: No. So they decided against the flow-
Juan: FloTrac.
Patrik: FloTrac, okay.
Kevin: It would interfere-
Juan: No, they said that with the IABP and everything on their readings, wouldn’t be that accurate?
Patrik: Yes, correct.
Juan: So maybe they’ll look at using it after they removed that.
Patrik: Right. Okay. My concern with the cardiac output is, it’s 3.1. Okay? And my concern there is, your mom is 90 kilo isn’t she?
Juan: I mean she’s-
Kevin: She’s probably lost weight by now. She’s about 80, 85.
Patrik: Okay. Let’s just say for simplicity, she’s 80.
Kevin: I would say 75.
Patrik: Okay. Okay. Let’s just say 75 for simplicity. Cardiac output should be around 7 mls per kilo, which means you’re looking at a cardiac output of 5.2. Right? So it’s too low from that perspective. However, I tell you-
Kevin: What they said was also that the PA catheter isn’t too accurate.
Patrik:Right. Okay. That might be the case. That might be the case.
Kevin: Because they said that it’s based on the last echo. It was better. They wouldn’t go by the reading on the PA catheter.
Recommended:
Patrik: Right, okay.
Kevin: They said that’s quite inaccurate.
Patrik: Right. Okay, fair enough. Hmm. Okay, alright. I tell you what you should then ask for, then. If they think it’s inaccurate, ask them if they can get you a cardiac index. I’ll text that to you. Ask them if they can get you a cardiac index.
Kevin: Okay.
Patrik: Ask them for an arterial blood gas.
Kevin: Arterial blood gas, okay. ABG?
Patrik: ABG.
Kevin: Okay.
Patrik: And I think that would be the most important things to look for. And ask them. Okay. I’ll tell you another thing. If they’re not worried about this low cardiac output, ask them if she’s making urine.
Kevin: Ask them if she’s?
Patrik: Making enough urine, urine.
Juan: Urine, okay.
Kevin: Yes, yes.
Patrik: And I’ll tell you why. So if her cardiac output is low, her kidneys won’t be perfused enough. And if her kidneys are not perfused, she won’t be making any urine.
Kevin: Okay. She’s passing good urine as of now.
Patrik: Oh, that’s good. That’s good. That’s good to hear.
Juan: A few days before that, it was at least 1500.
Kevin: That’s why they took off the filter because she was passing a lot of urine on his own.
Patrik: Okay, good, good, good. No, that’s good. And when you look at this picture that you sent me off the monitor where you can see the PA catheter, her blood pressure is 100/42. You can see that?
Kevin: Yes.
Patrik: You can see that on the left-hand side, there is 66, the smaller number. Can you see that?
Kevin: Yes.
Patrik: So the 66 is the mean blood pressure. That blood pressure should be above 65 for kidney perfusion.
Kevin: Right, right.
Patrik: But it’s just-
Kevin: When she was assessed, this was when she was asleep. So when she woke up after that, the MAP went up to like 75, 80.
Patrik: Okay. That’s good. That’s good to know. Okay. That is an indicator for me that her cardiac output might be sufficient.
Kevin: Okay, yeah. Because this was when she was asleep, and then she woke up maybe 10 minutes after we sent you the photos.
Kevin: And then her blood pressure goes to like 130/60, 130/50. And his MAP was around 75, 80.
Patrik: Yeah. Okay, great. Great. That’s good. The other thing on that note is, so when you look at the blood pressure, 100/42. So the 42 indicates to me that she’s probably a little bit dehydrated. The lower the diastolic blood pressure, I don’t know, have you heard of systolic and diastolic blood pressure?
Kevin: Yes. Yes, yes.
Patrik: Right, right. So the 42 is the diastolic blood pressure. The lower that number, generally speaking, the more dehydrated someone is. I don’t see that as a negative at all, because you know, now that the focus shifts, the focus may be shifting more and more towards the lungs now.
Juan: Okay.
Patrik: Given that the focus is shifting more and more towards the lungs, you do want to be dry. You do want to be dehydrated because the last thing someone needs with a pneumonia/ARDS is fluid overload on the lungs.
Recommended articles:
Kevin: Got it, got it.
Patrik: Okay. So I see that as a positive, as long as she’s making enough urine.
Kevin: Okay, good.
Patrik: Right? That’s on that note.
Patrik: With the PA catheter. Yes, it might be inaccurate because the waveform of the PA catheter, the yellow waveform would look differently if it was in the right place. The PA catheter has to be in the right place. And that would be, you would see a different waveform if it was in the right place. And therefore, I probably agree that the cardiac output may not be accurate.
Juan: So if it’s inaccurate, the reading, then what other purpose is the PA catheter serving?
Patrik: I tell you what the purpose of that might be. You might be able to get a mixed venous blood gas. What does that mean?
Kevin: Okay.
Patrik: So you get an arterial blood gas, you know, about that already. You can get a venous blood gas very easily from, just from the central line or even from a peripheral line, you can get venous blood gas with a PA catheter, the location where the PA catheter sits.
Patrik: It’s a mixture between venous and arterial blood. It’s where the exchange is happening.
Kevin: Okay, okay.
Patrik: And that makes venous gas will be a very good number to determine cardiac output. You get a lot of information from a mixed venous gas.
Kevin: Got it.
Patrik: But-
Kevin: Also, yeah sorry.
Patrik: But I think, again, the risk of having it in there for infection is still high. But they may want the mixed venous gas. They may. And then take it out.
Kevin: Right, right, right. One more thing, Patrik, that we want to tell you was, yesterday after they took out the arterial cannula.
Patrik: Yep.
Kevin: They found two clots.
Patrik: Yep.
Kevin: In between the arterial cannula and the sheaths.
Patrik: No surprises there.
Kevin: Yeah. They took them out. They removed them. They showed us photos of it.
Patrik: Right.
Kevin: It was around three or four centimeters.
Patrik: Right.
Kevin: But they said that he had expected it, and these are common in these cases.
Patrik: Very common.
Kevin: That’s why they look for them and check them out.
Patrik: Very common, no, no surprises there.
Juan: And one other thing, Patrik. This morning, the doctor told us that potentially, as in often, patients can be on V-V ECMO and have no sedation. They can be completely awake. And so we can try and work towards getting mom to calm down a bit and not fight the ventilator so that potentially we cannot use any sedation on her at all.
Patrik: Well, it’s not only on V-V ECMO. It’s also on V-A ECMO that patients can be awake. Both.
Juan: Oh, really. Okay. But maybe he meant that it’s more common on V-V than V-A.
Patrik: It’s probably more common because V-V ECMO is also more common compared to V-A ECMO.
Juan: Right.
Patrik: Okay. Having said that, let’s just say out of 10 ECMO patients, whether V-V or V-A, I would say you might have three out of 10 being awake.
Juan: Okay. Okay.
Patrik: But, if-
Juan: They said that if she’s-
Patrik: If they can move towards waking her up, fantastic. Fantastic.
Juan: Yeah.
Kevin: I mean, she is awake, because even though she’s on fentanyl, and the Dexmedetomidine, she was awake. She’s been awake, even while he was on V-A-
Juan: I mean, she responds to simple commands from the nurses and the doctors. She opens her mouth when they tell her, she starts fighting them when they try to do the suction.
Patrik: Right.
Juan: She blinks yes, I think quite a lot of the time if you ask her a question and say blink. If the answer is yes, she does do that. She’s been trying to move her head, and kind of shrugged her shoulders a bit, I guess.
Patrik: Great.
Juan: Yeah. So she’s doing all of that. And I think, yeah.
Kevin: She’s trying to talk quite a lot.
Patrik: She’s trying to what?
Kevin: Talk.
Patrik: Great. That’s a good sign. That means her brain is intact, which is also important to know in a situation like that.
Juan: Patrik, how long will it take her to learn how to speak again? Once we remove the trach tube.
RECOMMENDED:
Patrik: Okay. Great question. So as soon as she’s off the ventilator or let’s put it that way, as soon as she can have time off the ventilator and she’s strong enough, they might try a speaking valve.
Kevin: What’s that again?
Patrik: Yeah. So when someone has a tracheostomy and has time off the ventilator, so just because someone has a tracheostomy doesn’t mean they need a ventilator all the time.
Kevin: Right.
Patrik: Okay. So let’s just say she’s coming to a point where she needs the ventilator only intermittently. Okay?
Patrik: And if she’s strong enough, they can trial a speaking valve.
Kevin: What is that?
Patrik: Yeah. So basically when you take off the ventilator of a trachy, you could attach the speaking valve and then you have to deflate the tracheostomy cuff, and then you can do speaking exercises.
Kevin: Ah, okay okay.
Patrik: But I think he’s a long time away from that at the moment.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!