Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
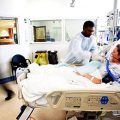
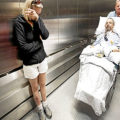
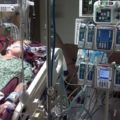
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Juan, as part of my 1:1 consulting and advocacy service! Juan’s mom is with a tracheostomy, balloon pump, and is now 25 days on ECMO support. Juan is asking why his mom has a blood clot in her lungs now.
My Mom is on ECMO Support for 25 days in ICU & Now She Has a Blood Clot in Her Lungs! Help!
“You can also check out previous 1:1 consulting and advocacy sessions with me and Juan here.”
Patrik: Oh yeah. It would have been. So yeah just ask them if the plan is to wean it off, because you don’t want to be on steroids for longer than necessary.
Juan: Yeah.
Patrik: So yeah look, there’s a few challenges she has to work through. But keep asking the right questions. And it sounds to me like they’re trying all the right things, which is very important. You’ve got the ozone, and go from there.
Juan: Yeah. We’ve added a few of our home remedies from here, so that’s started as well. Yeah, I think we’ll see tomorrow. I do have the feeling maybe, I don’t know. I’m her son, so I will have such feelings, but I feel like in another day, we might see a little bit of an improvement. So I’m keeping my hopes on that.
Patrik: No, absolutely. No, you should definitely be positive. There’s no need to be pessimistic. There’s no point in that.
Juan: That’s the doctor’s job, right, and the family doctor?
Patrik: Absolutely, that is definitely the doctor’s job. Your job is to stay optimistic.
Juan: Yeah. I gave mom a big pep talk last night. She was looking a little bit down after the day. I think those work for her, because I do think she can listen. I do think the sound with the messages get through. So, yeah.
Patrik: All right. We can talk later tonight, if you want to, after you’ve visited her again and maybe get a little bit more information.
Juan: Yeah. We’ll try and have this conversation about the points that we just discussed, and then hopefully we’ll have some updates as well that we can share with you and talk about.
Patrik: Yeah, we can talk later again.
Juan: Okay. All right.
Patrik: Okay. Thank you so much.
Juan: Thank you Patrik. We’ll make the payments today as well.
Patrik: That’s okay, all good.
Juan: Okay, all right.
Patrik: Thank you so much.
Juan: Thank you.
Patrik: Thank you. Bye.
Juan: Have a nice Sunday. Bye.
Patrik: Thank you. Bye.
RECOMMENDED:
Patrik: Hi, Juan, how are you?
Patrik: I’m very well, thank you. Yes?
Juan: Okay, they were planning to give her a suppository, because she hadn’t passed a stool in four days but then they didn’t need to. She passed a stool last night and then this morning. They said she passed a big stool last night and this morning.
Juan: Then this morning at around 6:45, they turned her over to clean her up and they put her back down. After which or around that time, she had a sudden crash in blood pressure and her heart rate had stopped for about a minute. Then they had to administer CPR. She stabilized again after that. They were on 0.4 of norepinephrine and then they tapered it down to 0.2 now. They’ll probably taper it down further.
Juan: The incident happened and then after that, after they administered the CPR and stuff and just stabilized. There were no other changes in say all her other reports and results. Pretty much everything was the same.
Juan: Her ejection fraction, they did a preliminary echo in which they think it looked like about 25 to 30, which they say is common after an incident, but they’re going to do a full 2D echo now to get a more detailed picture.
Juan: They are changing the arterial line and the central lines because as we mentioned yesterday, they wanted to do that in any case because of the yeast infection. They’re saying that this could be caused by either a new heart attack or an event, a cardiac event, or it could be due to severe hypotension.
Juan: What is the severe hypotension caused by is the question. We were looking at, I mean, what’s new that’s been introduced because she was stable till last night, and this seems to have been a sudden thing which has then stabilized kind of on its own. It’s settling down.
Patrik: I don’t think she was stable. She was only stable because they didn’t move her. I kept saying that blood gas leaves a lot of room for error, which is exactly what’s happened. As soon as they moved her, she crashed. There’s no surprises there in my mind, which is why I asked yesterday, “Have they moved her?”
Kevin: They moved her twice the day yesterday.
Patrik: Right.
Juan: She was fine after those moves.
Patrik: Right but they didn’t have to clean her up like that it needs to after a bowel movement. It probably took them a lot longer to clean her up after a bowel movement. With that blood gas, yes, they turned her probably briefly yesterday. But with that blood gas, the longer it takes for someone to be turned, the higher the risk for something like that to happen, which is exactly why I asked yesterday, “What are they doing about the blood gas?”
Patrik: I’m not surprised at all but they do need to find out, is it A) the lungs or is it B) is it something related to the heart? That’s probably the biggest question at the moment.
Juan: Well they said that it could be maybe pulmonary embolism. They’re going to see. They said maybe it’s very unlikely that that small clot that they found in her leg could have travelled up but they said that’s quite unlikely but not impossible. I guess, the possible options on the table and once they just do a few more tests and the various doctors go and see her, they’ll have a bit more insight.
Patrik: If it is a PE (pulmonary embolism), is she still on heparin? Her last APTT that I’ve seen, I think was fairly low, which means if they haven’t increased her heparin, yes, a PE might be an option. But by the same token, I’m not surprised. You know, these things happen when people are in such high support.
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Patrik: With the heart attack, they should be taking a troponin result. Have you heard of troponin?
Juan: Sorry? No.
Patrik: If they check the troponin, they will have a very quick answer, whether she had a heart attack or not. I’ll send you that. They should be checking troponin. They should be checking her APTT. They should be checking her white cell count because that’ll give them an indication, whether the infection has gotten worse, right. I mean, they’ve done the check off the echo with the ejection fraction.
Juan: Yeah.
Patrik: Do you know whether they start the high-flow cannula?
Juan: Yesterday? No, we forgot to ask. Let me just ask right now.
Patrik: Because if she’s got a low flow cannula, a high-flow cannula might help. It might.
Juan: Let’s find out.
Patrik: With the CPR, did they do manual CPR or just with medications?
Juan: I think with medications. What did they do? What kind of CPR did she specify? We’ll ask but I know that they use medications as well. We can ask that.
Patrik: Potentially, a combination of both, potentially.
Juan: I think so also. I think they said they did some chest-
Patrik: Chest compression?
Juan: Yes, maybe.
Patrik: I would also look at her hemoglobin again.
Kevin: Seven.
Juan: It’s seven. It’s seven.
Kevin: They’re transfusing.
Patrik: Okay. They are?
Juan: They are doing transfusion.
Kevin: Yeah.
Patrik: That’s good. That’s good. Are they doing a CT scan of the chest?
Juan: Not again. It’s too much to do and did one day before yesterday.
Kevin: No, actually yesterday, Patrik, they removed the PA catheter and they removed the sheath as well. I think that led to a little bit of bleeding last night, yesterday. I think probably another additional factor that I could think of.
Patrik: Yeah, if she had the PA catheter, it would be easier to find out if she had a PE. How many days has her ECMO been running, the VV ECMO?
Kevin: Day 25.
Juan: 25.
Kevin: The ECMO has been in for about 25 days, and the VV ECMO around 15, 14, 13 or 14.
Patrik: That in and off itself increases the risk for the PE.
Juan: I mean, from what we’ve read also that the medicine that they started last night can cause a drop in blood pressure. It can cause hypotension.
Patrik: The ozone?
Juan: No, no, the Anidulafungin.
Patrik: Oh, it may but that would probably be the last thing on my radar. The first thing on my radar is poor blood gases on maximum support that leaves a lot of room for something like that to happen.
Juan: Okay, so what do you suggest? We asked them if they’re doing a troponin test.
Patrik: Yes. Take APTT.
Juan: Yeah.
Patrik: Take white cell count. Check for any infection markers. Right. In terms of ejection fraction, if it is 25% to 30%, I would argue they need to start the Milrinone again and potentially support with a little bit of noradrenaline.
Juan: Yeah. They were talking about potentially switching back to the VA ECMO but we’re really not too keen on that.
Patrik: Right? Why? Again, the first step there from my experience should be to look at Dobutamine or Milrinone.
Juan: Yeah. Yeah.
Patrik: What would be their reasoning to restart VA ECMO?
Juan: It’s not come to a conclusion but they just said, that’s something that the doctors will see and it’s an option.
Kevin: I mean, they’re potentially re-cannulating it so I think that’s a bit of a risk in itself.
Juan: I’m not keen on going back to that. It’s so that her heart remains that level of support if this was just a … yeah, we have to get to the bottom first. I think we need more insight before making any decisions.
Patrik: Absolutely and you’d hope that they’ll give you an answer of why this happened.
Suggested links:
Juan: Yeah.
Patrik: You need an answer for that.
Juan: You’re saying that the more likely reasons could be moving her around with unstable blood gas. It’s not unstable, but poor blood gases?
Patrik: Very much so.
Juan: Poor blood gases.
Patrik: You’ve got fluid shifting when you turn someone especially on ECMO. One way to manage that going forward is if she’s getting a unit of blood that might help in and of itself.
Juan: Right.
Patrik: Right but if they are talking about VA ECMO straight away, I would argue they need to start the Milrinone or the Dobutamine.
Juan: Yeah. Yeah.
Patrik: That might help. That might help with the instability as well when she’s being turned.
Juan: I mean, the blood pressure is normalizing though. It’s like, it’s settling down. It’s getting back to its … they’ve reduced the Norepinephrine from 0.4 to 0.2 and she said, they’re continuing to reduce it further. Her FiO2 requirement was, it was at 100 on the ventilator and then they tapered it down to about 70 now. It’s holding at her SPO2 of about 94%-96%. They’re continuing to taper those down slowly.
Patrik: The oxygen on the ventilator is almost irrelevant at the moment because she’s on 100% through the ECMO. You can’t, if more than 100%, whether it’s through ECMO or through the ventilator. You can’t give 150%.
Kevin: That’s it?
Juan: What does that mean?
Patrik: Well, what it means is the VV ECMO is taking over the function of the lung.
Juan: Yeah, no. I mean, if we’re saying that we can’t give more than 100%, so the ventilator oxygen requirement is irrelevant.
Patrik: Irrelevant. What that means is whether the oxygen ventilator setting is at 100% or at 21%, it doesn’t really make any difference because VV ECMO is doing what it needs to do.
Juan: Right. Right. Okay.
Kevin: They just forward it this morning.
Juan: They’re saying the ECMO cannula is always high flow.
Patrik: Is it? Okay.
Juan: Or probably always high flow.
Patrik: All right. If they always do high flow, fair enough. That’s good.
Juan: Yeah.
Patrik: That also means that there is no wiggle room for the ECMO, which means they’re already on maximum, you know?
Juan: Okay. I guess our next steps would be, let’s wait for some more reports and for the 2D echo and we’ll ask if they’re doing a troponin, if they’re getting a troponin result.
Patrik: Yeah. Ask them, are there any clots in the ECMO?
Juan: Okay.
Patrik: Are there any clots in the ECMO? You see, once I do understand that going for a CT scan, won’t be an easy undertaking, but in order to find out if she had a PE that’s one way to find out very quickly.
Kevin: Isn’t that treatment for PE just more heparin?
Recommended:
Patrik: Yes. That could be. That could be one way, but there could also be other things such as they could do a thrombectomy if she had a PE. But, given that the blood pressure has recovered, probably not-
Kevin: It’s unlikely.
Patrik: Unlikely but we want to know.
Juan: Okay. Okay.
Patrik: There’s nothing that I haven’t seen before in terms of, it’s nothing there that hasn’t happened with VV ECMO on those patients with borderline gases. It’s just a case of, okay, what can they do about it going forward? Because she will need turning again.
Juan: Okay. Yeah.
Patrik: When did that happen?
Juan: Okay. 6:45 AM this morning. It’s 8:45 now. Two hours ago.
Patrik: Oh, so 6:45. The reason I’m asking, the risk for someone to drop their bundle in the middle of the night is higher than someone to drop their bundle during the day. You know?
Juan: Yeah. Yeah. Usually, I mean, any dips she’s had have usually been at night. This one was a strange one. Yeah.
Patrik: Yeah. The question is how are they going to manage it going forward and are the antifungals and antiviral and everything that they’re doing to treat the lungs, is that working?
Juan: I mean, even if it’s not working, they’ll say this is everything that we can do. There aren’t that many options left and that’s why we’ve introduced the Ozone because when they run out of options, if this is something that can definitely help with that, and that is believed to help with that and is shown to help with it, then why not?
Patrik: Yeah, of course.
Juan: Why not as a supplementary treatment? If it’s meant to help with fungal infections, bacterial, viral replication, et cetera, if the medication they’re giving needs a little supplement and a push, then this may well be that.
Patrik: Absolutely. It’s probably a critical phase she’s going through now. But I do believe a bit of Milrinone especially if ejection fraction has dropped, they need to do, because that might help. That might help to stabilize her before she’s even being turned, you know?
Juan: Okay. Okay.
Patrik: The other risk-
Juan: Okay, we’ll wait for the next ones.
Patrik: The other risk is definitely the length of time of ECMO. If the ECMO filter has been on for 24 days, the risk of clots to build and to shoot off is definitely there.
Juan: Well, they can’t take off the ECMO clearly.
Patrik: Well they can change the filter, but it’s a little bit risky as well. If they plan to continue keeping her on ECMO, I think that’s something they might consider.
Juan: Yeah. This morning because of the yeast infection, they also messaged saying that they would probably need to change the …
Kevin: Arterial and the central lines.
Juan: The arterial and central lines but also the vascular catheters, including ECMO..
Patrik: Right. Okay. Yeah. Well, I think that’s necessary. It’s a little bit risky, but if they plan to keep her on ECMO, I think it’s almost inevitable.
Juan: When you say, if the plan to keep her on ECMO, isn’t it that if she’s on 100% of ECMO support, then they can’t really take it off? Do they have a choice?
Patrik: No, they don’t really have a choice at the moment, but-
Juan: They have to keep her on ..
Patrik: They have to keep her on but then the question arises, how long is a piece of string? I haven’t seen people on ECMO for much longer than three weeks, which then inevitably brings up the question, “Does she need to go on a lung transplant list?”
Suggested links:
Juan: Okay. Let’s wait to hear from the doctors this morning. Let them analyze and do that test. I’m sure a lot of these points that you brought up will be ones that they consider. We just spoke to the ICU doctor and I think it’s yeah, preliminary. They’re just being honest with us and all the questions running in their mind, but I think, yeah, they’ll need to do some more reviews and then maybe we’ll have a better picture as well.
Patrik: Yes, yes.
Juan: Yeah. I don’t think we can make … yeah, we can’t really come to any-
Patrik: No.
Juan: We can’t make any decisions either until we know more from them, I guess.
Patrik: They need to find out what happened.
Juan: Yeah, yeah. Yeah and I think that’s exactly what they’re going to do right now. Try to find out what happens.
Patrik: The other thing that might have happened, do you know whether she was on Cisatracurium this morning?
Juan: Yeah. Yeah, she probably was. There’s no reason why she wouldn’t be.
Patrik: Right. Okay, because sometimes when people aren’t paralyzed … okay, when people are not paralyzed and they’re getting turned on ECMO and they are already sitting on the fence, like your mom does, paralyzing them helps to keep them stable. But if that’s what happens, if she’s paralyzed already.
Recommended:
Kevin: She is.
Juan: She is. Yeah.
Patrik: Right. Right. Right. Sure. Then it’s almost not the point of discussion.
Juan: Okay. Okay and is there anything else?
Kevin: No, I think let’s wait for them to do some analysis.
Patrik: Yeah.
RECOMMENDED:
Juan: Yeah.
Kevin: They are changing the arterial and the radial line I think about an hour ago.
Patrik: Right. Right.
Kevin: They will do the 2D echo and they’re going to do whatever other tests that you suggested as well. We’ll maybe ask them for those then we’ll get back to you and see.
Patrik: Yeah. Absolutely. All right.
Juan: Okay. Thank you, Patrik.
Patrik: Let me know what you need next. Thank you so much.
Kevin: Thank you.
Patrik: Thank you.
Juan: All right.
Patrik: Bye.
Juan: Bye.
Patrik: Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!