Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Will my Critically ill Mom with Pneumonia Benefit from Performing a Bronchoscopy in the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Juan, as part of my 1:1 consulting and advocacy service! Juan’s mom is with a tracheostomy, balloon pump, and is now on VV- ECMO. Juan asks how he will know if the ICU team gives his mom enough sedation for her recovery.
My Mom Is Critically Ill in the ICU & How Do I Know If the ICU Team Gives My Mom Enough Sedation For Her Recovery?
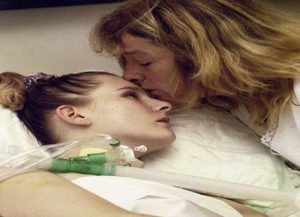
“You can also check out previous 1:1 consulting and advocacy sessions with me and Juan here.”
Patrik: And the treating team there knows her well, they’re not changing all the time are they?
Juan: No, everyone knows her well. It’s the same team on rotation, I think they all know her well now and understand her. The head doctors are all the same and we’re in very regular contact with them.
Patrik: No that’s good and important. And you think they’re pretty committed?
Juan: They’re very committed, they’re very committed.
Patrik: Okay good, that’s good.
Juan: They’ve been very receptive, they’ve been quite open minded, they’ve been very honest, they’ve been doing everything. I don’t have any actual complaints in that sense.
Patrik: Okay good. There hasn’t been any talk about stopping treatment, any of that?
Juan: No.
Patrik: Good.
Juan: It’s honestly, it’s my girlfriend’s hospital, it’s her family’s hospital. My girlfriend is the one who you just spoke to.
Patrik: Yep, I see.
Juan: So it is their hospital, so that’s why the VIP status and that’s why she is getting the best care in that sense.
Patrik: That’s good. I mean, normally ICUs are very quick in wanting to stop treatment, they’re usually very quick, and if they have been positive that’s good.
Juan: Yeah. And I think that honestly, in the last week, 10 days, since we’ve been talking to you, there have been such good indications. It’s really motivated them as well to do that, so I think we’re going to go meet the doctors right now actually, they’re just calling us. So we’ll speak with them and then give you an update.
Patrik: Sure, okay, no worries.
Juan: Okay all right, thank you Patrik.
Patrik: Thank you so much, thank you, bye.
RECOMMENDED:
Patrik: Hi Juan, how are you?
Juan: Hi Patrik. I’m fine. How are you?
Patrik: I’m very well, thank you.
Juan: Great. So sorry. Yeah, yesterday was a little bit hectic, but…
Patrik: That’s all right.
Juan: … essentially mom stayed stable through the night, as in she was more or less the same as last night. No major changes there. Her morning blood work seemed to be all right. The chest x-ray was similar to yesterday. As you saw, the CT scan has given us some insight at least, into what’s going on. And yeah, they’re taking us to PA catheter today.
Patrik: Good. I still don’t like the blood gases, they are borderline, even the level of support she’s on. So I’ve explained to you why I’m worried about the gases. So she’s on 100% of oxygen on VV ECMO.
Juan: Yeah.
Patrik: So that means she can’t get more support than that. She can’t get more than 100%, and her pO2 in the gas is sort of hovering around the 60 mark. The only way you could potentially improve that, as far as I can see at the moment… It sounds to me like you’ve got some alternative therapy there with ozone. But from a purely clinical and medical point of view, the only way to improve the gas at the moment, as far as I can see, is potentially increasing the flow on the ECMO.
Recommended:
Juan: Increasing flow on ECMO.
Patrik: Yeah.
Juan: Okay.
Patrik: So, if you look at the last ECMO picture that you sent to me, which in the revs… Hang on, where is it?
Patrik: Yes. The revs are set at 2,715. If you put that up to, let’s just say 3,000, you get a higher flow, and that might increase your oxygenation. But the goal of the ECMO should be to reduce the flow. Do you know if she’s got a high-flow cannula or a low flow cannula? Do you know?
Juan: No, but I can find out.
Patrik: Yeah, find out. So sometimes when gases are poor, despite being on maximum support, they might change from, I wouldn’t say low flow cannula, I would say normal flow cannula, to a high-flow cannula. And she might have that already. I don’t know, but it’s definitely something for you to ask. And I would also ask what’s their plan to improve the gases.
Juan: Yeah. I think one of the things that they’re assuming is that CMV (Cytomegalovirus) virus might be causing some of the issues. So they gave Ganciclovir shots to work maybe that will help. Yeah, we will ask them again, although it sounds like there’s not that many options to that…
Patrik: I agree.
Juan: … but I think as you mentioned, increasing the flow on the ECMO is probably something that they have to look at, maybe. We’ll ask this well about it.
Patrik: Yes. Bear in mind, so let’s just say they will increase the flow on the ECMO. There could be other flow on effects from that, which your hemoglobin will probably drop lower. Again, they might need more of the noradrenaline specifically or maybe also by suppressing, because the blood pressure will most likely go down, because you will be extracting more blood from the body. So the risk, when you put in a high-flow cannula, is definitely higher, but that’s then often the only way to manage that.
Recommended:
Juan: I think my sense is that they’re probably waiting to see how she does today. And if she doesn’t improve by tomorrow, then I think that probably might be the direction that they’ll look at. But yeah, that’s what I assume, because anyways it’s weekend today and there’s not that many doctors and it’s more of a quiet day. But yeah, I think… Yeah.
Patrik: I can tell you from experience, no you wouldn’t want to do that on a weekend. But if they have to, they will do it on a weekend.
Juan: Yeah. I think just because yesterday they moved her around as well for the CT scan, I think they just want to give her a little bit, to see how she does.
Patrik: Right. Yeah, absolutely. And that would have been a massive undertaking, just taking her for a CT, just on ECMO. You need almost 10 people for taking someone for a CT scan with ECMO.
Juan: Yeah. And with the ventilator and everything in general, it was a whole expedition. So I think that did look like it dialed mom down.
Patrik: Look, no question about that. The other question is, which will give you an indicator as well in terms of how is she doing, so every so often, they will turn your mom on the side, just to give her back a wash, to change linen. Do you know whether she can tolerate that well? So what I mean by that is when you turn her, she might drop her bundle-
Juan: So actually not this morning, because they’re administering the ozone rectally. And she said that she’s been tolerating that well, and that’s when her oxygen dropped from 91 to 88, and that now just climbed up again soon after.
Patrik: Oh, good. Okay, because that will also give you an indication. When you turn someone on ECMO, they can drop their bundle. If the gases are borderline already, again, it’s quite an undertaking just to turn someone and give their back a wash, clean them up if they are so unstable. And if you’re telling me she dropped a little bit, fair enough. What we sometimes did as well is, coming back to the revs, what’s at the moment 2715, before you turn someone, you might crank up those revs to sort of increase-
Juan: To keep her comfortable.
Patrik: Yeah, absolutely.
Juan: Yeah, I think they were considering doing that if she didn’t tolerate it. But now she has tolerated it, now they’re okay. They also were applying some oil and stuff to her, what could be emerging bedsores and just standing by where there’s some damage sores. We are looking after that already, preemptively, and yeah we’re doing whatever we can.
Patrik: Yeah, of course. And I’ve noticed the Atracurium is back on.
Juan: Yes, she’s been having… It’s Cisatra now. It’s not Atracurium, it’s Cisatra.
Patrik: Yeah, okay. It’s pretty much the same.
Juan: Yeah. They had introduced it after her deterioration on Friday because she was fighting the ventilator quite a bit, and she was gasping. So when she’s a bit more paralyzed, she doesn’t fight it as much; they don’t want any lung injury because of that resistance. So they were reluctant as well, and I think they did it because they felt like they just need her to stabilize a little bit. And if we see a slight improvement, then they can look at reducing that.
Patrik: Yeah. No, that’s great. And I can see that Milrinone has been offered a little while, which is a very positive indicator by the way.
Juan: Yeah. Isn’t it normally kept at 0.04… Is it at 0.2 now? Okay, yeah 0.02, because they just feel like that’s a tiny dose just to keep her comfortable at where she’s at.
Patrik: Yeah. Bear in mind, if they need to increase the flow, there’s a very good chance she will need more noradrenaline. But that’s probably the least of my concern.
Juan: That’s trade off.
Patrik: Probably not so much my concern. My concern is the blood gas.
Recommended:
Juan: I think everyone’s concern is just the blood gas now. I think that’s what they’re keeping the closest eye on and just trying to keep everything as stable and not rock any other boats, while we see and hope for that to improve.
Patrik: Yeah. The other thing that I’ve noticed is they change the ventilator settings again. And I think I might explain that to you. So the last picture you sent, she’s in a volume control mode. And all the previous pictures you sent from the ventilator is a pressure control mode. I am unsure why they made the changes, but I would ask. So most of the time in ICU, in this day and age, you do a pressure control mode. It’s limiting the risk of a pneumothorax. Have you heard of a pneumothorax?
Juan: No, I haven’t.
Patrik: Well, basically what it is, a pneumothorax is basically-
Juan: So is it this… Okay. No, never mind. Go ahead.
Patrik: A pneumothorax is basically a hole in the lungs. If you are ventilating someone with a pressure control mode, you’re minimizing the risk for that to happen. Now-
Juan: Go ahead Patrik, sorry.
Patrik: No, that’s okay.
Patrik: And now she’s in a volume control mode, and I’m not sure why they changed her to a volume control mode. The risk for a pneumothorax in the volume control mode is higher than in a pressure control mode. I won’t go into too much detail, but what you need to understand for now is volume control mode is in that now, and the risk for pneumothorax to happen in that mode is higher.
Juan: So we can ask them why have they switched, and for how long do they plan to stay in that mode.
Patrik: Yeah, and just ask them why.
Suggested links:
Juan: Okay.
Patrik: Yeah, ask them why. The volumes are higher now. However, the volumes are higher with the risk of a pneumothorax. And if they want to take that risk, fair enough. But what is the reason for them taking that risk.
Juan: Yeah, okay.
Patrik: So, I think the focus for now will be on the gas, and you are saying they’re taking the PA catheter out.
Juan: Yeah, they’re taking that out today.
Patrik: And what are they saying with the Cisatracurium? Is that going to be temporary?
Juan: This whole Friday, they had kind of taken off the Atracurium. They had taken it off completely, and that was going on for a bit. I think they reintroduced it with what happened this weekend. They were quite concerned about it. And my assumption is that as soon as it starts to settle, they will look at removing it. I did ask last night as well, if the sedation is still the same. Actually I asked this morning as well. And yeah I think that’s what they said. They said yeah she just needs it right now because we don’t want her fighting the ventilator, agitating her lungs again. So as soon as we see it done, then I think they will just start to reduce that, taper it off.
Patrik: Fair enough.
Juan: Kevin is that right?
Patrik: Say again?
Juan: I was just asking Kevin, who’s on the call if that’s correct.
Kevin: Yeah. I think they’ve not given a specific timeline, essentially for when the Cisatracurium will abort, or how they will taper. Ask them that.
Juan: Yeah. I think, Kevin, it sounds like they’re taking everything day by day right now, and they’re not looking at a timeline because I think they all are just concerned about the lungs, about the fact that the x-ray hasn’t changed in two days, that these data points are kind of steady with the gas exchange. So I think tomorrow we’ll have a better picture. Let’s see how today goes. But yeah, these are the points that we can raise, maybe back tonight.
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
Patrik: Yeah. Are they still testing her for COVID?
Juan: No.
Patrik: No, okay. The reason I’m asking is simply given that it looks like the virus has come back. If it’s a CMV (Cytomegalovirus) virus, that’s great. I would imagine there would be other COVID patients in that ICU, wouldn’t there?
Kevin: No, the COVID ICU is separate actually.
Patrik: Ah, okay. Fair enough.
Juan: Yeah.
Patrik: If, God forbids, all attempts fail, I guess lung transplant.
Juan: Yeah, I think that’s in the back, like right at the bottom. But there in the back of everyone’s mind, I think we are aware of that. So let’s see. We’re hoping that she won’t need it.
Patrik: Yeah, absolutely. Look, absolutely one day at a time.
Juan: Yeah. But that was mentioned when we were talking about the heart and the apparent stuff. So, that is there. I know that it’s at the back of their minds as well.
Patrik: Yeah, okay. Are you going to see your mom today?
Juan: Yes. We saw her in the morning, and I will go see her now in a bit as well.
Patrik: Yeah, that’s good.
RECOMMENDED:
Juan: She was quite responsive to me last night actually. I gave her a little talk. She woke up and she was looking at me, and I feel like she was responding. She was moving her mouth quite a bit.
Patrik: That’s good. That would have been before they started her back on Atracurium?
Juan: No, it was after she’s been on Atracurium for a while though. Yeah.
Patrik: That should completely paralyze her.
Juan: Nothing has really completely paralyzed her. She seems quite interactive throughout, which has confused the doctors as well.
Kevin: I think the resistance to these medications has built up. So I think it’s not having as big of an impact on her as it used to.
Juan: She moves her head, she does like…
Kevin: Everyone is surprised on how she reacts. Even though she’s on paralytic, and quite a lot, she’s able to move.
Patrik: Right. It’s a bit of a worry that she’s on the Atracurium, and she’s still responding. I’ll tell you what on the one hand, what worries me on the other hand. So when someone is on Cisatracurium or the Atracurium, they should be heavily sedated, and she’s not. And I’ll tell you why she should be heavily sedated. Imagine you’re paralyzed and you can’t move, but your brain is working potentially. It’s a terrible feeling.
Juan: Yeah. I think that is what was causing her a lot of the anxiety. But that’s why they’ve kept up with the paralytics as well because they don’t want her to feel that. But they don’t really know what to do because obviously she’s not completely there, and it’s not that she’s fully interacting the whole day. But she definitely does respond to them and to us, in a sense like you know she’s listening. And she is and she’s listening.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!