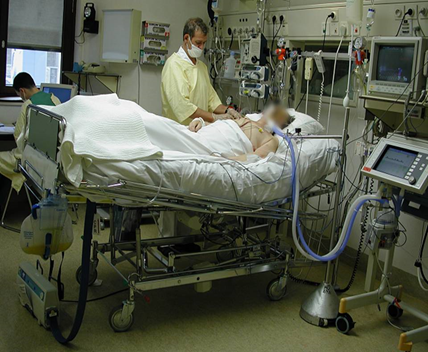
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
Does the ICU Team Have an Agenda that We Don’t Know Whilst Our Mom is Critically Ill in the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Juan, as part of my 1:1 consulting and advocacy service! Juan’s mom is with a tracheostomy, balloon pump, and is on ECMO. Juan is asking if he should give his 100% trust to the ICU team who’s managing his critically ill mom in the ICU.
Should I Give My 100% Trust to the ICU Team Who’s Managing my Critically ill Mom in the ICU?
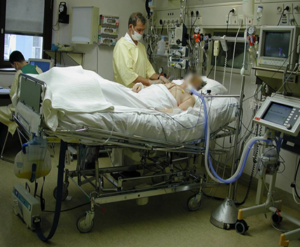
“You can also check out previous 1:1 consulting and advocacy sessions with me and Juan here.”
Juan: No sir I guess it’s worth… Yeah, I mean we have brought it up. We brought it up with two different doctors and I don’t know, they were… It’s not that they said no to the Dobutamine and Milrinone but it just wasn’t with as much urgency and even the balloon pump they were like, “No that’ll stay.” I don’t know. But yeah, we completely understand where you’re coming-
Patrik: Have you asked about the infection risk?
Kevin: Yes.
Patrik: And what are they saying about it?
Juan: Yeah they were going to take out the PA catheter today-
Patrik: Okay.
Juan: And then this happened, and then this took priority.
Patrik: Right and what are they saying with the infection risk specifically?
Kevin: They’re saying that there’s no less risk than there is from any of the other lines.
Patrik: Okay, all right. I dispute that. Yeah, again look, maybe there is something that I’m missing here, just-
Juan: Or maybe there’s something that they aren’t telling us, I don’t know.
Patrik: That’s what I’m fearing, there is something they’re not telling you and I don’t know what it is at the moment. Just trying to think… Are the blood results today? Have you got them?
Kevin: The morning ones? Yes.
RECOMMENDED:
Patrik: Hemoglobin?
Juan: Hemoglobin is at 6.4, the platelets have dropped I think to what 90-
Patrik: Yeah, yeah I’ve seen that.
Patrik: Yeah-
Juan: And her WBC count has gone down but her CRP has gone up, which they said could be a very early indication of infection.
Patrik: Yes, for sure. Do you have an Arterial Blood Gas?
Juan: We can try and get that.
Patrik: Keep an eye on her lactate.
Recommended:
Juan: Yeah.
Patrik: Lactate could also be an indicator for, if lactate is going up, could be an indicator for an infection, could be an indicator for hypoperfusion. Yeah, it just… After two weeks of ECMO, they should be moving towards decannulation more aggressively and I do believe that by using the Milrinone or Dobutamine and maybe a little bit of noradrenaline, it can be achieved. It just doesn’t make sense from my perspective, maybe I’m learning something, yeah I don’t know.
Kevin: One more thing Patrik, what they said was that the saturation, even when they’re trying to increase the FiO2 on the ventilator, the saturation is still a bit low which is why they feel that, that she still requires the VV on for a bit-
Patrik: Sure.
Kevin: That hasn’t made any…
Patrik: Impact?
Kevin: Impact or effect.
Patrik: Yeah, I can’t see it at the moment. Just give me another second, I’m just looking at all the pictures again that you sent, just looking through all of them again. Ventilation hasn’t changed… Balloon pump And that’s why I would want possibly from a ventilation point of view, it would be very valuable to have a blood gas.
Kevin: The Arterial Blood Gas? Yeah
Patrik: Yes, would be valuable. Her cardiac output is around the same, her PA pressures are up a little bit, and she’s on Fentanyl?
Juan: Yeah.
Kevin: They reintroduced the Atracurium because she started hyperventilating and her respiratory rate was going up quite a bit.
Patrik: Right.
Juan: In your opinion Patrik, is reintroducing Atracurium necessary or could they achieve the same results by just increasing the Fentanyl and the Midazolam?
Patrik: If she’s fighting the ventilator, there’s two options from my experience. A) you increase the midazolam to a point where she doesn’t need the Atracurium, but then you have the side effect, I don’t know how much you know about Midazolam. Midazolam is a benzodiazepine and is addictive.
Juan: Yeah, yeah.
Patrik: Same with Fentanyl. They’re both different and she might go through withdrawal after she’s coming out of the coma. Having said that, the Atracurium is also very bad because it causes muscle weakness, so does sedation but it’s causing a massive muscle weakness and they’re all not great drugs. Yeah, they’re doing the job but they’re all not great drugs to be used. You want to minimize any of that drug use as much as possible.
Suggested links:
Juan: Yeah. But in this situation you’re saying that they could lessen two evils than not introducing, reintroducing the Atracurium and just increasing the Midazolam?
Patrik: I would think so, I would think so. At least try…
Juan: Okay.
Patrik: At least try… They could also add in a little bit of Propofol instead of the Atracurium however, the challenge with Propofol is… Propofol causes hypotension and if she’s hypotensive already-
Juan: Yes, that’s something they mentioned actually when we-
Patrik: Right, yeah, no surprises there. Yeah, it does not make sense to have that balloon pump there and not inotropes. Just does not make any sense to me.
Juan: So I guess that’s probably then just exactly what we’re going to lead with now.
Patrik: I would lead with that if I were you. How long have they been telling you about decannulation? How many days have they been sort of talking about that? That’s what they’re aiming.
Juan: It’s been about a week now.
Patrik: And why has it taken them a week so far and it hasn’t happened yet?
Recommended:
Juan: So, the early part of last week she would desaturate, she wasn’t tolerating when… And her BP would drop whenever they tried to wean off.
Patrik: Yeah, Yeah.
Juan: I’m pretty sure that they… I mean even on Friday they said, “Tuesday is probably when we’re going to take off the VA.” Even yesterday, they said they would take it off today. And then I think when this leg started swelling up, because there were some blisters on coming on the leg as well which I think they got quite concerned about because that right leg is looking quite big.
Patrik: Right.
Juan: And I think they were just quite concerned about it, it seemed like they were in a big hurry to just switch that.
Patrik: Yeah, sure.
Patrik: She’s still on heparin?
Juan: Yes.
Patrik: How much?
Juan: I think 450.
Patrik: 450.
Juan: I think I sent you an image of the heparin.
Patrik: Yes, 450, okay. Do you know her aPTT?
Kevin: Oh we’ll find that out.
Juan: We’ll find out, I’ll get the-
Patrik: Yeah do that. Yeah. I think that they seem to be over-complicating, given the information that you share with me again, maybe there is something that they haven’t shared. Maybe there is something they’re hiding. From the information that you are sharing with me, they’re over over-complicating I believe.
Juan: Yeah, I mean I felt, I mean obviously with my very limited knowledge and being emotionally involved in this situation, I just feel like she’s ready to get off the VA ECMO I think-
Patrik: Yeah, I agree.
Recommended:
Juan: It doesn’t make sense to me that a few days ago as well they said, “She’s performing better without the IABP than actually the IABP, but now we put it in.” So I mean I’m not understanding, if the heart is performing well and the BP has been holding all this time. So why aren’t we just getting the whole thing off?
Patrik: Yeah.
Juan: I don’t really get it.
Patrik: Yeah, the other thing that I’ve seen, I have seen people coming off VA-ECMO, possibly with an ejection fraction of 25 to 30%. And with Dobutamine or Milrinone, you know what I’m saying? It just…
Juan: She’s in a position to do it.
Patrik: Correct.
Patrik: That’s what I’m saying, that’s exactly what I’m saying. From my experience, I have seen patients being on ECMO, 25-30% ejection fraction, you add in some Dobutamine and some Milrinone, one or the other, and you wean them off and the ejection fraction is reasonably low and they still manage. And, it just doesn’t make sense.
Juan: I mean one of the things, I don’t know if this is their reason of course but yes, they’re being super over cautious with her-
Patrik: Sure.
Juan: She is very weak, I totally understand-
Patrik: Oh absolutely.
Juan: … Very unpredictable things that have taken them by surprise, so I think they also kind of felt like she’s not a usual patient and we’re a bit scared that she might do something strange. Like we said, that might be the VIP syndrome issue. And I think COVID has complicated things where sometimes, there’s just too many other question marks which then kind of make them a bit overcautious and over complicating.
Recommended:
Patrik: Yeah, but that’s where I believe that judgment should come in.
Juan: Yeah.
Patrik: And also, I keep coming back to the infection risk. Yes, you’ve got to be cautious, but one of the biggest risks in ICU whether you are on ECMO or whether you’re not on ECMO is infection risk. That’s one of the biggest risks.
Juan: And they keep mentioning it, but then I don’t understand it. They sort of made it sound like this is the only option with her, she’s in such a precarious situation, these are the only options, this is what she needs and..
Patrik: Yeah.
Juan: I don’t think it’s with ill intention, I just think that’s-
Patrik: Yeah, I’m not saying there’s ill intent-
Juan: Yeah of course, yeah.
Patrik: It just doesn’t make sense to me, that’s all.
Juan: Okay. We’re going to go in and just have this conversation be really pushy about why, why not, why give them these ways to do it and say why can’t those ways be done and just kind of really push and say that have we not been getting the indications over the last few days with all the last couple of times that she is ready to get off this ECMO and the balloon pump?
Patrik: Absolutely.
Juan: Potentially if her BP drops, then we can manage that with noradrenaline?
Patrik: Noradrenaline and also another blood transfusion, and if they’re worried about fluid overload, because that is a delicate situation too. Yes, she needs a blood transfusion, but then she might get fluid overloaded, which might be too much for the heart. But if it’s too much for the heart, then I’d argue, okay, let’s use some Lasix, let’s use the dialysis or again, let’s use the inotropes.
Juan: Yeah.
Kevin: Okay.
RECOMMENDED:
Patrik: The other thing is the balloon pump, especially in ICUs where ECMO is available has more or less come out of vogue. It feels a little bit like going back in time, I’m not saying… The balloon pump has its time and its place, especially in units where you don’t have ECMO.
Kevin: Great, okay. I think Patrik we’re going to go in with these questions-
Patrik: I think so.
Kevin: Then let’s take it from there.
Patrik: Yeah.
Juan: Yeah, I think we’ll do that.
Patrik: And sent through a blood gas if you can-
Juan: The arterial blood gas-
Patrik: Yes please.
Juan: Yeah and aPTT.
Patrik: And aPTT, and the rate of heparin, yeah.
Juan: Okay, and the lactate-
Patrik: The lactate will be part of the blood gas.
Juan: Oh, yes. Okay thank you Patrik, we’ll get back to you.
Patrik: Pleasure, all the best. Thank you, bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!