Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Juan, as part of my 1:1 consulting and advocacy service! Juan’s mom is with a tracheostomy, balloon pump, and is on ECMO. Juan is asking how the ICU team can wean his critically ill mom with COVID from ECMO in the ICU.
How Can the ICU Team Start Weaning my Critically Ill Mom with COVID from ECMO in the ICU?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Juan here.”
Juan: You know what? Feels a little bit like they are dancing around exactly saying how they’re going about it. I think they are figuring it out as well. I mean, we know that they’ve been trying to get the ECMO off. They’ve been trying the whole week. That’s pretty clear.
Patrik: If I was you, I would throw that scenario at them and say, “Okay, you’re taking VA-ECMO off. Let’s just say you’re succeeding with that. And then you’re going on to VV-ECMO. That’s all great. What’s next?” I would throw that scenario at them.
Juan: You mean in terms of the balloon pump?
Patrik: Yeah, not only at the balloon pump, but let’s just say best case scenario. Best case scenario is take ECMO off, take balloon pump off. That’s the best case scenario.
Juan: Right. Right.
Patrik: And then you’re left with VV-ECMO, and what’s next?
Juan: Right. I guess the ventilator would-
Patrik: Yeah. Yeah.
Kevin: And another concern as you said was probably the Atracurium.
Patrik: Oh, huge. Huge concern. Atra is fine for a couple of days, but not for two weeks.
Kevin: It’s been almost a month.
Patrik: Almost a month, has it?
RECOMMENDED:
Kevin: Yeah. Yeah. I mean, it’s been on and off-
Juan: It’s been on and off for about a month. Yeah.
Patrik: Right.
Juan: So what do you think? What do we say if they say that she needs it, what do you say?
Patrik: Well, have you seen them taking it off? Have you seen it for yourself?
Juan: Yeah.
Michelle: Yes. Yeah, I’ve seen it.
Juan: And what is-
Michelle: Her saturation starts to drop? She moves around and that’s risky with all these-
Patrik: Of course. Of course. Yeah, not disputing any of that.
Michelle: Having said that, even despite Atracurium and all of this, she still every now and then kind of moves around and she responds to us when we speak to her. She responds to my father, she responds to all of us. Like when we say, “Move your left hand.” She moved her left hand. This was some time ago and when-
Juan: Today when we spoke to her-
Michelle: Today when we spoke to her again, she moved her head.
Juan: She nodded her head in response to some questions.
Michelle: She nodded her head in response to some questions. And they even baffled at how she’s responding despite being on these sedatives and Atracurium as well.
Recommended:
Patrik: Right. That was my next question. Can she be talked through that? Because that’s what it often comes down to. When someone is waking up after an induced coma, the problem is people are often disoriented. They have no sense of time base or what happened. And imagine you’re waking up in an ICU after many weeks, it’s terrible.
Juan: So what do you say, Patrik, about the Atracurium? I mean, is that’s something that we’re going to bring up-
Patrik: Yeah.
Juan: … in front of the-
Patrik: Yes.
Juan: What’s the question-
Patrik: Yeah. I tell you what I would say, what I will say to that? I think it’s critical that they can take that off as quickly as possible. My concern is, or my question would be, can they increase the midazolam and the fentanyl to get rid of the Atracurium? Can they potentially add in some propofol to get rid of the Atracurium?
Patrik: I’ll text that to you as well. And can they… Potentially, you mentioned the Precedex earlier, the Dexmedetomidine. Can they potentially use that as well? I think they are all questions you should be asking. Another medication might be, and I’ll just text them here. I can never pronounce it, but Precedex is Dexmedetomidine. If you google Precedex, you’ll get the Dexmedetomidine. Another medication they can use, or they might be able to use again, it’s Clonidine.
Juan: Clonidine. Got it.
Patrik: I’m texting all of that while we’re talking.
Juan: Yeah. Getting those. Thank you.
Patrik: And that might help to get rid of the Atracurium. At the moment we’re talking about survival, but long-term, what’s the goal? Long-term the goal is a recovery. And the longer your mom stays in an induced coma, the higher the chances are, she will go through a very, very lengthy recovery with a very uncertain outcome.
Juan: Yeah.
Patrik: And I’m not only talking about heart and lungs, I’m talking about just in general, physical recovery.
Juan: Of course. Yeah. Yeah.
Patrik: And it would be very difficult for them to predict the future as well. I mean, we always say, and I say that to my clients as well, as much as we all want to live and look into the future, it’s a take one day at a time.
Suggested links:
Juan: Yeah.
Patrik: What does your mom want in this situation? If she could make the decision herself, what would she want?
Juan: I think she wants to get off everything and just get up.
Patrik: Sure.
Juan: She wants everything off her. I mean, we know her.
Kevin: We know she’s fighting it.
Juan: It’s like she wants to start talking. She just wants to get up.
Patrik: Good. Good, good, good. Well, that’s good. That’s good. That’s a sign of life.
Juan: Yeah, very much. I mean, it really feels like she’s-
Michelle: She’s a fighter.
Juan: She’s a big fighter. Yeah.
Suggested links:
Patrik: Okay.
Juan: She doesn’t like resting. She likes being on the move.
Patrik: Good, good, good.
Juan: That’s her general personality as well.
Patrik: Good, good, good. No, that’s good. That’s good to know. I can see why they will be guarded, because it’s very critical. But is it fair to say that… Just from me trying to piece the puzzle together. So when she came to hospital, she came in with a heart attack, but she was COVID positive, but she was COVID asymptomatic.
Michelle: No.
Juan: I wouldn’t say COVID asymptomatic, and that she-
Michelle: She had breathlessness.
Recommended:
Juan: She had breathlessness and she’d been struggling through the week. So she got admitted in on a Wednesday. And for the 12 days before that, is probably when the COVID kind of started. Obviously first we thought it was just a regular fever. She was on paracetamol for about a week. So she would come and go. And then about six days before the heart attack is when her breathlessness began, and then the fever stopped, but she started getting progressively weaker and her breathlessness and her breathing issues just got worse and worse.
Juan: As her breathlessness got worse and she got weaker, that’s when she probably forgot about her heart medication, because she wasn’t fully herself anymore. She wasn’t thinking the way she normally did and she started just getting weak. So I think by the time she went into hospital, yes, she was struggling a lot with the breathing and she was very weak. In terms of fever, she didn’t have a fever when she entered. And she didn’t really have a cold. She did have a slight congestion or maybe a cough, I think, but it wasn’t very dramatic. I think it was more than the heart attack, which really precipitated it, but it’s a little bit of guesswork as well.
Patrik: Yeah. Yeah. No, I can see that. I can see that.
Juan: So they didn’t really change too much, to be honest. And then after, that’s when we started the MATH + protocol. I don’t know if you’ve heard of it. I can send you a link. So we kind of went on the MATH + protocol, which was Ivermectin, Methylprednisolone, the vitamin C, D, Zinc, thiamine etcetera. And that seemed to help quite a bit, but then that desaturation happened with the TRALI (transfusion-related acute lung injury) and that’s when the ECMO happened. And then you know the story from there.
Patrik: Yeah, sure. I have not heard of the MATH + protocol, however, I have heard of the combination of those medications, but I haven’t actually heard of the term.
Juan: Sure. I will send it to you just so that you have it.
Patrik: Yes please. I guess the next few days will be critical.
Juan: Yeah.
Patrik: They need to really get rid of the VA-ECMO and the balloon.
Juan: In your opinion, Patrik, is it possible to get rid of both, one after the other, in a short span of time?
Patrik: I would say yes. If her heart is coping, I would say yes, but it all depends on her heart. I mean, she’s had a rest now for the last two weeks. I mean, that’s the goal of the ECMO, to let the heart recover and recuperate, that’s the goal.
Juan: Yeah. I think actually this is one of our big questions, where we’re like, “Okay, now we’ve waited for so long. Is it that you can take off these machines consecutively one day after another?” Is there a time period you have to wait between them? How quickly can you go without being too dangerous?” So sort of where we are confused as well.
Recommended:
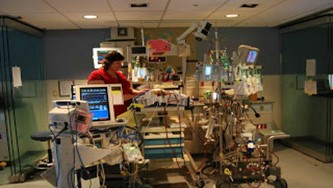
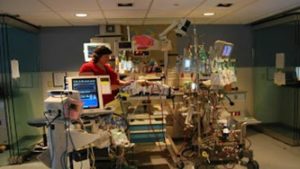
Patrik: Yeah. Yeah. Look, so what you can do. It’s quite simple actually, when I say simple. Okay, let’s just quickly go back to the picture that you sent of the ECMO. Okay, because I think that’s… I’ll show you that. Let’s just quickly look at that. So when you look at the ECMO, you can see 33-40 and 5.1. Can you see that?
Juan: Yeah.
Patrik: So 5.1 is the cardiac output, approximately which… When you look at the cardiac output on the monitor with the PA catheter, it’s 4.6. So it fluctuates a little bit. So 0.5 plus, minus. So it’s about the same. So you can see the revs on the left side. The revs is basically the rate per minute. How quick is the ECMO pumping? That’s at 33-40. So what you do during a weaning study, is you basically reduce the revs.
Juan: All right.
Patrik: And then you see what your cardiac output is doing.
Juan: Okay. Yeah.
Patrik: Right? That’s one thing to assess. The other thing to assess, a lot of ICUs during the weaning study, they also do an ultrasound of the heart, to see what is the heart doing while we are reducing the ECMO.
Juan: Yeah.
Patrik: That’s-
Juan: I think they have been doing that. We can ask them for the results of that actually.
Patrik: Right.
Juan: We just got told that the cardiac output is 4.6L per minute.
Patrik: Yeah. And that is too low for a 90 kilo per person.
Juan: Right.
Patrik: It keeps coming back to the Dobutamine and the Milrinone.
Juan: Okay.
Patrik: Because that is increasing the contractility of the heart.
Juan: Right.
Patrik: Okay. For a person without ECMO and without a balloon pump, if you have a low cardiac output for a person without ECMO and without a balloon pump, you start using those inotropes to begin with.
Juan: Right.
Patrik: And I guess, given that they want to remove both ECMO and balloon pump, that would be my suggestion or I can only talk from my experience, that this would be a natural next step.
Juan: Got it. Okay. Yeah, so we’ve got a bunch of questions here.
Patrik: Yeah.
Juan: I’m just going to run through quickly what I have written down as our main talking points-
Patrik: Please.
Juan: You can tell me if I’ve missed anything.
Patrik: Yeah.
Juan: One is what you just mentioned, improving the cardiac output using Dopamine and the other two drugs that you mentioned. What is their plan with the ECMO and the balloon pump removal, because both need to be removed at the earliest time?
Patrik: Definitely.
RECOMMENDED:
Juan: The PA catheter, when do they plan to remove it? Because the risk of infections. Question them about the weaning studies and get the results of that. You’ve mentioned a regular sinus rhythm. I don’t have any point to discuss. There was potassium being low. I think that’s what we have to discuss too.
Patrik: Yeah.
Juan: Third spacing could be because of the low albumin and the fluid overload. Are they managing sodium?
Patrik: Yeah. And how are they managing it? Because one way to manage a high sodium is to give water.
Juan: But that’s not something that they want to do-
Patrik: No, no.
Patrik: Definitely not.
Juan: Right. And then the pulmonary hypertension. Are they doing any kind of nebulization?
Patrik: So when I talk about pulmonary hypertension, there’s a few treatment options for pulmonary hypertension. And again, I will text that to you. For pulmonary hypertension, you can use a medication called sildenafil, which is also known as Viagra. So I’ll just quickly text you that. Viagra/sildenafil.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!