Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM , where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from one of our dear readers and the question last week was,
“My mother wants to go home on a BIPAP machine from Intensive Care, can she survive?”,
you can check it out last week’s episode by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer another one of our most frequently asked questions from our readers and the question this week is
”HOW LONG DOES IT TAKE TO COME OFF A VENTILATOR/ RESPIRATOR IN INTENSIVE CARE?”
Now, if your loved one has just been admitted to Intensive Care for critical illness, chances are that you and your Family feel challenged, out of your comfort zone, fearful, frightened, vulnerable, stressed and you feel like you are overwhelmed. Furthermore, you feel like other people are running the show and you feel like you have no or very little power, control and influence over this challenging situation.
You are also looking for answers and some of your questions may have already been answered by the Intensive Care team, however you may also feel like not all of your questions are welcome, as the Intensive Care team often also speaks in medical terms and in their medical jargon that is difficult to understand.
Their answers are often not broken down into a language that speaks to you!
One of the biggest challenges for families in Intensive Care is that you don’t know, what you don’t know! Furthermore, the next biggest challenge is that you don’t know what questions you need to ask in the first place!
The quality of your questions and your ability to to manage doctors and nurses will clearly determine the outcomes you will be getting!
Therefore you will need to make sure you are asking the right questions in the first place and I can help you with that, after having worked in Intensive Care for nearly 20 years in three different countries where I literally looked after thousands of critically ill Patients and their families! I have also worked as a Nurse Unit manager in Intensive Care for over five years!
Here is what’s important!
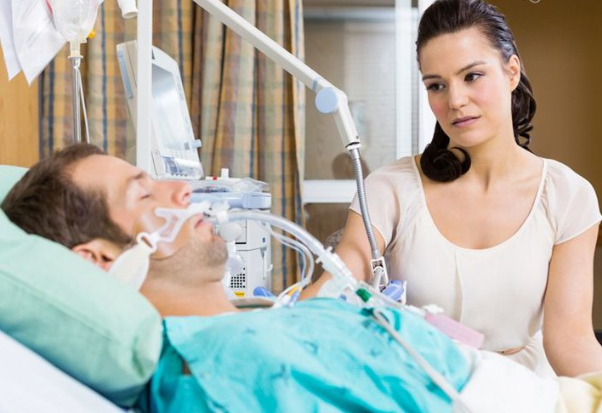
Your critically ill loved one is probably ventilated with a breathing tube(endotracheal tube) in their throat and in an induced coma.
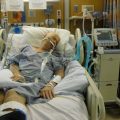
You are probably shocked by how your critically ill loved one looks with the ventilator / respirator and the breathing tube attached to them. You probably also feel intimidated by the Intensive Care team and by all the equipment and the technology in Intensive Care…
Nevertheless, you and your Family are wondering how long it will take for your critically ill loved one to recover and you are also wondering how long it will take for your critically ill loved one to come off the ventilator?
Ok, in order to give you an answer to this question, we have to break it down in some segments, because the length of a time for your loved one on a ventilator is dependent on a number of things that I will explain here:
I’ll give you some quick examples so that you understand
1. “Straight forward” and “soft” admissions to Intensive Care
If your critically ill loved one is a “straight forward” admission to Intensive Care after elective or planned surgery or is a “soft” admission to Intensive Care for a medical emergency on a ward etc… your critically ill loved one should come off the ventilator/ respirator and out of the induced coma relatively quickly within 12- 72 hours!
Ventilation and a breathing tube after surgery are sometimes stabilising and prophylactic measures and are also measures to make sure that your loved one isn’t bleeding before the Intensive Care team takes them off the ventilator/ respirator, which is especially important after surgery. The same applies to other “soft” admissions into Intensive Care after your loved one may have had some breathing issues and they may have required the ventilator/ respirator and breathing tube for a little while to improve your loved one’s lungs with some extra pressure and oxygen. In those situations, the induced coma, the breathing tube/endotracheal tube and the ventilator should be gone soon.
It all depends on whether your loved one’s chest X-ray is clear, whether they can breathe for themselves with minimal support from the ventilator/respirator(CPAP or pressure support ventilation mode), they will need to be able to cough and clear their secretions and airway, their arterial blood gases need to be satisfactory and they will also need to be able to follow instructions such as squeezing hands, poke out their tongue etc…
Related article/video:
2. Ventilation for 3- 7 days
If your critically ill loved one is a more complicated admission to Intensive Care and is more unstable, such as after a car accident or after major surgery where complications occurred or if your critically ill loved one sustained a head or brain injury or had a heart attack or cardiac arrest, then the breathing tube, the ventilator/ respirator and the induced coma might be required for more than 72 hours and if your loved one is stable and progressing, breathing up on the ventilator/ respirator with the support from the ventilator/ respirator being reduced then again, your critically ill loved one should be able to come off the ventilator/ respirator.
Again, coming off the ventilator/ respirator after more than 72 hours of ventilation and induced coma, might be a little bit more difficult, because as a rule of thumb, the longer ventilation is required, the higher the risk that complications and/or delays occur of course.
So, once again, if your critically ill loved one is stable and has shown strength to breathe by themselves there should be no reason that they can’t be taken off the ventilator after 3-7 days, generally speaking.
It all depends on whether your loved one’s chest X-ray is clear, whether they can breathe for themselves with minimal support from the ventilator/respirator(CPAP or pressure support ventilation mode), they will need to be able to cough and clear their secretions and airway, their arterial blood gases need to be satisfactory and they will also need to be able to follow instructions such as squeezing hands, poke out their tongue etc…
Related article/video:
HOW TO WEAN A CRITICALLY ILL PATIENT IN INTENSIVE CARE OFF THE VENTILATOR AND THE BREATHING TUBE!
3. Ventilated for more than 7 days
If your critically ill loved one has been in Intensive Care for more than one week now and has been ventilated for more than one week by now and is still in the induced coma, you’re probably wondering and you are more importantly worried when your loved one will finally come off the ventilator.
Now, if after one week of ventilation and an induced coma the Intensive Care team still doesn’t feel confident to take out the breathing tube, they may suggest to insert a Tracheostomy. Before they actually suggest a Tracheostomy they should try and get your loved one out of the induced coma first and if your loved one is “waking up” and is cooperative and can breathe, the Intensive Care team should remove the breathing tube and give your critically ill loved one “a fair go” first to find out whether your loved one can breathe without a breathing tube and without the ventilator/ respirator.
Related articles/videos:
If that fails, then the Intensive Care team might have a fair point to suggest a Tracheostomy, but once again that shouldn’t be brought up before or after at least 7-10 days of ventilation with a breathing tube. And again it shouldn’t be done until the Intensive Care team is certain that there is no other alternative.
Furthermore, especially when it comes to tracheostomy in the USA, the risk is that once a tracheostomy is performed that the ICU wants to send your loved one to Long-term acute care(=LTAC). This strikes a disaster, as LTAC’s are designed to save money but not to provide quality care for critically ill Patients.
If LTAC is mentioned as an option for your loved one after or before they have a tracheostomy, your alarm bells need to go off and you will need to avoid LTAC at any cost.
I can’t tell you how many desperate families we have calling every week who want us to help them to get their loved ones out of LTAC. We can help them achieve that with our 1:1 consulting and advocacy service, however more importantly we can help you advocate and make a clinical argument to keep your critically ill loved one in the right environment in the first place, which is Intensive Care!
The only place where a Patient can be safely looked after on a ventilator with tracheostomy or with a breathing tube/endotracheal tube is Intensive Care! If you are not clear on this, it could literally cost the life of your loved one!
The only alternative for Patients on ventilation with tracheostomy is INTENSIVE CARE AT HOME where highly skilled ICU nurses provide care in your home for your loved one as a genuine alternative to a stay in Intensive Care.
Why?
I’m glad you’ve asked!
Because anybody on a ventilator needs the skills and expertise of a critical care nurse, critical care doctor etc… Anything less than that is literally killing Patients!
Let me say this again, one more time, because if you’re not clear on what is clinically required for your loved one on a ventilator with tracheostomy could literally kill your critically ill loved one, because LTAC’s simply don’t have the skills, expertise and professionalism to look after a critically ill Patient on a ventilator with tracheostomy!
Most of the time LTAC’s work with doctors and nurses who have no ICU skills and expertise, hence they have no skills and expertise to look after ventilated Patients.
The only place where a Patient can be safely looked after on a ventilator with tracheostomy or with a breathing tube/endotracheal tube is Intensive Care! Let me repeat this because if you are not clear on this, it could literally cost the life of your loved one! The only alternative for Patients on ventilation with tracheostomy is INTENSIVE CARE AT HOME where highly skilled ICU nurses provide care in your home for your loved one as a genuine alternative to a stay in Intensive Care
Once your loved one has a Tracheostomy we should be looking at the next example number 4.
4. Having a Tracheostomy
Your critically ill loved one is having a Tracheostomy because they went through one or multiple failed extubations (removal of the breathing tube in the mouth) and they were unable to breathe without the ventilator/ respirator support. Furthermore, your critically ill loved one may also be required to stay in Intensive Care for a prolonged period of time with ventilator support due to their critical illness.
The advantage your critically ill loved one is having now is that they should be able to be taken out of the induced coma and they should be able to “wake up” and hopefully communicate, at least non-verbally, because a Tracheostomy doesn’t give your loved one the ability to talk.
Keep in mind that with ventilation through the breathing tube in the mouth, an induced coma would have been necessary, whereas a Tracheostomy can usually be tolerated without the induced coma.
Recommended resources:
A Tracheostomy generally speaking also brings the advantage of getting your critically ill loved one off the ventilator quicker by trying to breathe without the ventilator/ respirator just via an oxygen mask with humidified oxygen via the Tracheostomy.
The goal here is to increase the frequency your loved one can stay off the ventilator/ respirator. Initially this might be two hours on the ventilator and two hours off the ventilator. As soon as your loved one can stay off the ventilator for >24 hours, they should, in most instances, be able to leave Intensive Care, even with a Tracheostomy still in place. However many Patients also can have their Tracheostomy removed in Intensive Care before going to the ward.
How long does it take to wean ventilation and the Tracheostomy? It depends. It can range from a few days to a few weeks and sometimes few months.
If you are finding that your critically ill loved one is stuck on a ventilator with Tracheostomy and is not moving forward you have a few alternatives and options to consider:
A)Read this article here
“Tracheostomy and weaning off the ventilator in Intensive Care, how long can it take?” (Click on the link)
B) look for alternatives such as Intensive Home Care services that provide a genuine alternative to a long-term stay in Intensive Care for long-term ventilated Adults& Children with Tracheostomy. Find more information here www.INTENSIVECAREATHOME.COM (Click on the link)
C) Put pressure on the Intensive Care team and demand more AND DON’T TAKE “NO” FOR AN ANSWER! How do you do that?
I’m glad you’ve asked!
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!