Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM here we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
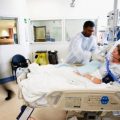
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Juan, as part of my 1:1 consulting and advocacy service! Juan’s mom is with a tracheostomy, balloon pump, and is now on VV- ECMO. Juan is asking if his critically ill mom will benefit from performing a bronchoscopy in the ICU.
Will my Critically ill Mom with Pneumonia Benefit from Performing a Bronchoscopy in the ICU?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Juan here.”
Juan: We will get through it.
Patrik: Oh yeah, of course. Of course. It’s like when I think about it, my grandparents and I don’t know about you, but my grandparents they’ve been through world war two, some of them through world war one, I just go like, “Okay, well, COVID, won’t kill us.”
Juan: Yeah. No, definitely. Definitely. Okay. I’ll give you an update this evening.
Patrik: Very nice to talk to you. Yeah, yeah.
Juan: Patrik, what time do you go to sleep?
Patrik: So, for me, at the moment, it’s 9:30 PM, but if you need to talk, I won’t be going to sleep before midnight.
Juan: Okay.
Patrik: And even if you need something after midnight, if it’s urgent, you just call me.
Juan: Okay. All right. Will do.
Patrik: Okay.
Juan: Okay. Thank you.
Patrik: Thank you so much. Thank you. Bye-bye. Bye.
Kevin: Bye.
Juan: Bye, Patrik.
Kevin: Bye.
RECOMMENDED:
Patrik: Hi Juan, how are you?
Juan: Hi Patrik. I’m fine thank you. How are you?
Patrik: I’m very well thank you. Now, how’s your mom?
Juan: She’s okay. They’re currently doing bronchoscopy and lung-toileting. That’s going on right now. They’ve upped her paralytics, the Midazolam is up to six and the Atracurium is up to eight, so she’s pretty much fully paralyzed and sedated. The Morphine’s also on, there’s no Fentanyl going on right now. They haven’t used Fentanyl since they started Morphine.
Patrik: Okay. Do the chest x-rays and the blood gases make sense to you?
Juan: I mean, there’s obviously been some kind of rapid deterioration this morning.
Patrik: Very much so.
Juan: The infection markers are not really up, so that’s why they’re a bit confused and trying to figure it out. The viral load was high for which they’ve given the Ganciclovir, and the other one, PCP came negative. They’re resending it today for another test, after they do the bronchoscopy they’ll take a culture and send that in, but preemptively they’ve given that other drug. I forgot what it’s called, hang on I just sent it to you earlier. They are giving Septran, I think that’s what it’s called.
Patrik: Did you send that earlier?
Juan: I did, I sent it in the morning 7 am update, the first message I sent you today. It says Septran and Ganciclovir.
Patrik: Hang on. Her breathing has become laborious.
Juan: It’s above that, it’s two messages above that.
Juan: It’s something for PCP (Pneumocystis Pneumonia), a PCP drug. I’ll double-check and give you the name.
Juan: Yeah, so I probably misheard and mistyped it. I will recheck for you, but they’ve started that preemptively because it’s unlikely that CMV (Cytomegalovirus) comes positive and PCP (Pneumocystis Pneumonia) comes negative, so they’re going to send the PCP for another test and see what it shows up, but preemptively they’ve started it. But I mean to be honest, we’re confused. We think that it’s mostly the inflammation and the fibrosis in the lungs potentially, I mean that’s why we’re asking.
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
Patrik: Well if you look at the x-ray from today and if you look at the blood gas from today, or I should say the second blood gas from today, clearly there’s something going on, clearly. And also they’ve increased the pressure control on the ventilator drastically, which is another sign there’s something going on. And you are saying they’re at the moment doing a bronchoscopy.
Juan: Yes.
Patrik: Okay, that’s good. How long did it take them to go from this blood gas to x-ray to bronchoscopy? How long did it take them?
Juan: Honestly, the bronchoscopy was already planned I think because they do it every three days, they’ve been doing the bronchoscopy and the lung toileting, so this will be the first one that they’re doing. So it was honestly routinely planned in any case. They were going to do it at 2, and it just got delayed to a little bit later.
Patrik: I see.
Juan: The plan to remove the IABP is still, I mean they haven’t said that it’s not happening, but it’s not done yet. So potentially I think they are very keen to get that out.
Patrik: Yeah, and just because what’s happening with the lungs, shouldn’t stop them from taking it out I would argue.
Juan: Also for the lungs, they want to take her to do a CT scan and getting the IABP off will allow them to do that, because they can’t fit all the machines in the elevator, so they need to get it off anyway.
Patrik: Yes, very much so. But there’s definitely something going on in the lungs that they probably weren’t expecting.
Juan: Yes.
Patrik: And they need to get on top of it.
Juan: Yeah, that’s exactly, I think all the doctors are consulting each other and they’re having conversations, so they’ve not given us a unified assessment yet because they’re probably trying to figure it out.
Patrik: Yep, okay.
Recommended:
Juan: We’ve heard a lot of very positive experiences with the ozone therapy and potentially also UV treatment. It’s been something that’s been suggested to us right from the beginning, from people outside, around the world actually. So that’s something that we’re exploring and we found a practitioner here who does it and who’s had great success with it, and it’s a minimally, there’s no real side effects to it, it’s a good treatment. So we’re going to explore that because as per the studies, it’s been used in post COVID or in severe COVID pneumonia patients to help with the inflammation at the site and the fibrosis, et cetera.
Patrik: Okay. I’ve never heard of it. I have, let’s put it that way, I have heard of ozone, but I’ve never heard it in context of ECMO and fibrosis, I’ve never heard of it in that context.
Juan: Yes, I know that it’s been used now in this last year, it is more alternative, it’s meant to be supplementary. They don’t do it in the hospital, it’s not something here in this hospital that they’ve done, but there are one or two hospitals where they have done it, where they do it. So it is a little bit more niche, but I guess they are doing everything that they know here, which is honestly, like they’ve added methylprednisolone again, they’re covering all bases that they know of.
Suggested links:
Patrik: Right. I mean most of it, what they’re doing, is what I’m familiar with. The only thing that I mentioned is obviously not introducing the inotropes earlier, and having the balloon pump. That’s the only thing I didn’t know, but other than that it’s pretty standard so far.
Juan: Yep.
Patrik: Is your mom still COVID positive?
Juan: No. Honestly, she came in with a positive test and a CT value of 27, 28. So it’s not that she had a high viral load when she came in, and I think about five days later they tested her again and she was negative. So I mean, she didn’t even come into the hospital with a fever or with a cough or anything.
Patrik: Right, okay. But it’s definitely, on the one hand it’s concerning, especially those chest x-rays and the gas. On the other hand, like I mentioned to you yesterday, two steps forward, one step back.
Juan: Yes I know. I think that’s sort of how everyone is looking at it here as well.
Patrik: I think it’s important, she’s made massive steps forward and now it’s sort of heading in the other direction again. What worries me is that the blood gas a while ago is pretty good, and within not quite three hours, drastic deterioration.
Juan: Yeah.
Patrik: And they didn’t see that coming did they?
Juan: No, it definitely took them by surprise. I mean, yesterday to be honest, her breathing had become a bit more laborious yesterday itself, and they started questioning things, which is why then they didn’t do the IABP and I think they just wanted to see her settle down a little bit. That’s why they introduced the Morphine and they kind of just changed things around yesterday. But then this big drop today, obviously they didn’t see, but we did have a slight indication yesterday I think.
Patrik: Right, and your mom prior to this did not have any lung disease?
Juan: No, not that we know of at least. I mean to be honest with you Patrik, she’s someone who just did not believe in doing regular checkups, she’s someone who just, she was sort of a walking miracle on her own just before this as well to be honest, like someone who had three stents in her heart, went 20 years without changing them, didn’t really care much to get tested. That’s just her, we pushed her a lot to do it but she never did, so she is a bit of a unique individual on her own anyway.
Recommended:
Patrik: Okay, so you are saying Septran. Just give me a second.
Juan: I think so, but after I hang up with you I’m going to call them and just double check again.
Patrik: Let me just type in Septran and see what I get. Oh yeah, okay, it is a treatment for a variety of bacterial infections. Trimethoprim, it’s Bactrim actually. That’s fine.
Juan: It looks like..
Patrik: Say that again?
Juan: It looks like it’s probably this.
Patrik: Yes, it’s a common antibiotic, it’s mainly used for UTIs, and do you know what a UTI is?
Juan: Yep.
Patrik: Right, it’s mainly used for that, but maybe that’s what they’re suspecting, I don’t know.
Kevin: Patrik, isn’t the PCP (Pneumocystis pneumonia) that they’re suspecting usually caused by fungus?
Patrik: Well yes. If she’s having a fungus in the lungs, they should be giving antifungals.
Kevin: Which they already were, yeah. So they’re suspecting the CMV (Cytomegalovirus) plus the PCP (Pneumocystis pneumonia), the CMV (Cytomegalovirus) came positive with a high viral load, I think 15,000 replications. And the PCP (Pneumocystis pneumonia), came negative, but they are assuming that it is there, because they usually see PCP and CMV together. So they’re giving the Ganciclovir to treat the CMV (Cytomegalovirus) and then I would assume for the PCP (Pneumocystis pneumonia), they would give an antifungal medication, right?
Patrik: You would hope so, that they’re giving it, you would hope so.
Kevin: So she was getting antifungals before as well, there was some other fungus that came positive about two weeks ago which they said is routine, that it usually comes up in the ICU. So I would assume that they would be giving antifungals for PCP (Pneumocystis pneumonia), but I think we just need to double check on that.
Patrik: I’ll send you a link, if you Google PCP (Pneumocystis pneumonia), it’s actually funny, it’s saying treatment and outcomes, it’s actually saying exactly that one of the treatments is actually the Septran. It’s actually interesting to see that. I’ll send you the link in a minute, I’m surprised to see that, that’s new to me.
Suggested links:
Patrik: Part of the issue probably is your mom would have been on steroids.
Kevin: Yep for quite some time.
Patrik: That’s right, and if people are on steroids the risk of them getting a fungus is quite high.
Kevin: Yeah, we are quite aware of that. So again, they’ve given her a bolus of, I think they’ve given her more steroids to treat this essentially.
Patrik: Say that again, they’ve given her a bolus of what?
Kevin: Of methylprednisolone.
Patrik: Okay, no surprises there.
Kevin: So if it’s caused by steroids, do you treat it with steroids?
Patrik: I can tell you that anyone, generally speaking, with cystic fibrosis will have steroids going most of the time. Have they ever mentioned that a lung transplant might be an option? Has that ever been on the cards?
Kevin: They did mention it but as a last resort and a last line of therapy, like at the end, they said first they didn’t even say lung transplant, I think they were more worried about the heart initially. So when they said first IABP, if IABP doesn’t work, then Impella, and if Impella doesn’t work then we’d think about a transplant at that time.
Patrik: Right.
Juan: And then they generally just mentioned that heart and lung transplants have their own issues. But at that point we were focused on the heart as the complication.
Patrik: Of course, look no doubt about that heart transplant and lung transplants have their own issues, there’s no question about that. The question is, what are the alternatives if everything they’re doing is not working?
Juan: Yeah. I think obviously that’s why we are also keen to at least attempt with the ozone and with the UV if possible, because I don’t know if you saw the papers that we sent you guys that were kind of patients with similar issues that have had success with these treatments, and if it doesn’t work in a couple of days, no harm done really compared to the fact that we’re giving her everything under the sun in any case.
Patrik: No, there’s definitely no harm done by trying. Hopefully, the bronchoscopy often does improve things.
Recommended links:
Juan: It really did help her the last two times, both the last two times they did it they’ve been doing it at three day intervals, the chest x-rays after that have come a lot clearer, her breathing has improved, I mean they’ve been extremely surprised by how effective the bronchoscopy and the lung toileting has been with her, so I mean I’m sure that will contribute definitely to helping.
Patrik: That’s good to hear that last time that worked.
Juan: It did work.
Patrik: When was the last one done?
Juan: About three to four days ago, we’ll double check. They were intending to do it every three days, I know that we did the first one and then we did the second one after three days.
Patrik: That’s really good.
Patrik: The bronchoscopy worked last time and I hope that will be the case this time as well.
Juan: I hope so. Because the secretions this morning was blood tinged, the last couple of days they’ve been clearer, they’ve been clear. Not just clearer, they’ve been clear pretty much for the last four days, and then today they were a little bit blood tinged.
Patrik: Right. So I’ll tell you what you might want to look for. Those blood gases need to improve quickly, those blood gases need to improve fairly quickly, and the x-rays hopefully will improve as well. That’s probably your best sort of indicator whether what they’re doing is working or not.
Juan: Okay.
RECOMMENDED:
Patrik: And the treating team there knows her well, they’re not changing all the time are they?
Juan: No, everyone knows her well. It’s the same team on rotation, I think they all know her well now and understand her. The head doctors are all the same and we’re in very regular contact with them.
Patrik: No that’s good and important. And you think they’re pretty committed?
Juan: They’re very committed, they’re very committed.
Patrik: Okay good, that’s good.
Juan: They’ve been very receptive, they’ve been quite open minded, they’ve been very honest, they’ve been doing everything. I don’t have any actual complaints in that sense.
Patrik: Okay good. There hasn’t been any talk about stopping treatment, any of that?
Juan: No.
Patrik: Good.
Juan: It’s honestly, it’s my girlfriend’s hospital, it’s her family’s hospital. My girlfriend is the one who you just spoke to.
Patrik: Yep, I see.
Juan: So it is their hospital, so that’s why the VIP status and that’s why she is getting the best care in that sense.
Patrik: That’s good. I mean, normally ICUs are very quick in wanting to stop treatment, they’re usually very quick, and if they have been positive that’s good.
Juan: Yeah. And I think that honestly, in the last week, 10 days, since we’ve been talking to you, there have been such good indications. It’s really motivated them as well to do that, so I think we’re going to go meet the doctors right now actually, they’re just calling us. So we’ll speak with them and then give you an update.
Patrik: Sure, okay, no worries.
Juan: Okay all right, thank you Patrik.
Patrik: Thank you so much, thank you, bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!