Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How to Have Power and Control Over the ICU Team Whilst My Mom Is Critically ill in ICU?
You can check out last week’s question by clicking on the link here.
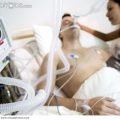
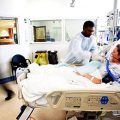
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Juan, as part of my 1:1 consulting and advocacy service! Juan’s mom is with a tracheostomy, IABP, and is on ECMO. Juan asks if ECMO with the intra-aortic balloon pump (IABP) would give a better outcome for his critically ill mom in the ICU.
Would ECMO plus an Intra-Aortic Balloon Pump (IABP) Give Better Outcome For My Critically Ill Mom in the ICU?

“You can also check out previous 1:1 consulting and advocacy sessions with me and Juan here.”
Juan: So we got her latest blood report at 8:00 this evening. The hemoglobin was at 7.5. Her platelets were at 144,000 and her WBC count was 10.
Patrik: Okay. That’s all right.
Juan: Her CRP in the morning today was at 2.3.
Patrik: Okay. And sodium?
Juan: Sodium in the blood was 155 this evening. Yeah, so they want to manage that as well.
Patrik: Right. What do they want to do with that? Do they want to give her some water?
Juan: No, I think that they’re a little wary of water since they’re trying to offload water.
Patrik: Exactly. Exactly.
Juan: I don’t know what they were planning to do. They said they were going to talk about.
RECOMMENDED:
Patrik: Right. Okay. I’m just looking through the medications again. So she’s on Methylprednisolone. She’s on Meropenem.
Patrik: She’s on-
Juan: She’s on Hydrocodone now.
Patrik: Okay. She’s on Hydrocodone.
Juan: I think Methylprednisolone was stopped.
Patrik: Okay. Have they talked about pulmonary hypertension?
Juan: Yes.
Patrik: And what’s their verdict there? Do you know?
Juan: They said I think that she had severe pulmonary hypertension I think. That was two days ago.
Patrik: I can’t see them managing that. Does she have a nebulizer?
Juan: Yeah. She’s getting a nebulization. Sorry. I have a note here that says severe pulmonary hypertension 71 mmHg. I don’t know what that means.
Patrik: 71 mmHg.
Patrik: If she has pulmonary fibrosis, she would have pulmonary hypertension. But besides the nebulization, she’s not on any other nebulizers?
Juan: Not that I know of.
Patrik: Okay. I’m just going down the list, whether there’s anything that I can see that would treat her pulmonary hypertension. It’s probably not so much of an issue at the moment because she’s on ECMO. The minute she comes off ECMO, the pulmonary hypertension will become an issue most likely. I’m just going down the list of medications there. Meropenem.
Suggested links:
Juan: I think Meropenem’s off now. I think the list that I sent you is categorized by types of medication. And then I think it’s chronological within those sections. So it’s not…
Juan: Everything isn’t what she’s currently on.
Patrik: I was just about to say, it can’t be everything she’s on at the moment.
Juan: No, no, no. Yeah. It’s not everything. I think the dates are next to each of the images.
Patrik: Yes. No, she would-
Juan: They were saying that after tomorrow, they were planning to remove most of the antibiotics.
Patrik: Right. Okay. And what was your concern with nutrition?
Juan: I think we just wanted to know what… because she didn’t get much nutritional feeds in the first couple of weeks because she was so sick, and they’ve only just started the feeds and kind of increased her intake. So we just wanted to know, is there anything else nutritionally you can add to help her healing and help in everything?
Patrik: Sorry. Before I answer your question, I mean, just because someone is sick, shouldn’t stop them from feeding her. That’s-
Juan: I don’t think that they weren’t feeding her at all. I think it’s just that her nutrition was less because her… It’s just that digestion takes up more energy and that the body needed to focus-
Juan: Yeah. She’s been getting feeds through the Ryles tube but in the last week it’s increased quite a bit, the amount of protein she’s getting.
Patrik: Okay. Fair enough. Fair enough. When I look at it, I can see she’s getting thiamine, I can see she is getting vitamin C. You could always argue that more vitamins would be beneficial. The problem that I can see with giving her potentially more feeds is fluid overload.
Juan: Yeah. Yeah. That has been a concern.
Recommended:
Patrik: Right. Right. It’s all well and good to say, “Can we maximize nutrition?” Yes. You possibly could, but have you spoken to a dietician?
Juan: We have. I mean, we spoke to the dietician here and they’re quite… I mean, she said that they have the scientific formulas and they adjusted according to how the patient is performing. As her performance improves, they recalibrate what they’re giving her. I mean, that was sort of generally what she said. And she’s getting about 120 grams of protein per day.
Patrik: Right. Okay. Look, I’m not a dietician, obviously. I don’t see nutrition as a primary issue at the moment. What I do see as an issue is, in the last 20 years in ICU, there have been studies done to say, feed early, feed early. 30 years ago, people were dying in ICU because people weren’t fed and they ended up with gastric ulcers that were starting to bleed, and people were literally bleeding to death. I mean, that’s stopped. That stopped, because they started feeding people early. And that’s also why I was asking earlier, is she absorbing her feeds?
Juan: Yeah, she is.
Patrik: Right. That is very positive.
Juan: I think about a week ago maybe, about six days ago, I think I mentioned she got diarrhea and that they didn’t feed her for a little bit. I think the protein was at 1.6, and then they dropped it to about 1.1. And then as she got better, she’s been I think on 1.4 for about three or four days now.
Patrik: Okay. When you say she had diarrhea, is that because of an antibiotic? Is it because she had…
Juan: They said it was because of the protein most likely.
Patrik: Okay.
Juan: I mean, if you’re seeing antibiotics potentially..
Patrik: Look, whenever there’s Meropenem…
Juan: They did say that it could have been because of the antibiotics or-
Patrik: Yeah. Not surprised. Okay. Bigger picture. I am concerned about the intra-aortic balloon pump. This is something I haven’t seen before. Sort of when I first started out in ICU over 20 years ago, there was no ECMO. So you would start with a balloon pump, and then you had nowhere to go, right? Then ECMO came in, and the balloons more or less disappeared.
Juan: So I think literally what happened as far as we can see is that they wanted to take off the VA, but they knew that whenever they were trying to take off the VA, her BP would drop. So they put the balloon pump in thinking that that’s what they would need. But then she did this weird thing where her BP went up, and now they’re sort of in a little bit fix because they have to figure out how to do this. I think that’s what’s happening.
Patrik: Maybe they are figuring it out and hope they are. But it’s just a concept that I haven’t seen. The concern there for me is you’ve got ECMO, which is an infection risk in and of itself. You’ve got balloon pump, which is an infection risk in and of itself. You’ve got the PA catheter which is an infection risk. You’re adding in dialysis which is an infection risk. So-
Recommended links:
Juan: So the hemofilter is attached to the machine-
Patrik: Yeah, of course but…. Yeah, I get that. I get that. But it’s still…
Juan: But it’s an infection risk.
Patrik: It’s still. Wherever you have access, you have an infection risk.
Juan: Got it. Right. Yeah.
Patrik: But I mean, by the same token, it looks like your mom so far, she’s alive and whatever they’re doing keeps her alive. I mean, that’s the positive.
Juan: Yeah.
Patrik: Okay. The question is, how much longer? Let’s just say the balloon isn’t working, how much longer do they want to persist with ECMO?
Juan: I think as far as they said that maybe even tomorrow, they would again try weaning down the VA. I think they obviously don’t want to commit to us because things are fluid, but I think next week potentially they want to remove the VA.
Patrik: I mean, that would be fantastic if they could, so they can then tackle the next issue, which is the lungs. I mean, if the heart’s working, let’s look at the lungs.
Juan: So in your opinion, would it be the VA first going off or the balloon pump going off?
Patrik: That’s almost like a chicken or an egg question.
Juan: Yeah. Yeah.
Patrik: As I said, what I’ve seen is, you start with the balloon, and if the balloon doesn’t work, then you come in with ECMO, but you never go back on the balloon. That’s why I’m saying I haven’t seen that.
Juan: Yeah. I don’t think they have either and I think that my mom’s behavior was strange really, and that they sort of were like, “We have to do…” Everything I think was sort of a last-ditch effort. I think that they’ve been really pushing the envelope with her because all traditional modes of doing this weren’t really working. Yeah.
Suggested links:
Patrik: I keep looking at the list of medications you sent me. She had an injection of Cordarone. Cordarone is 300 milligrams. Cordarone is also known as Amiodarone. And she must have had some atrial fibrillation during that period.
Juan: Sorry, can you explain that a little bit more?
Patrik: So I explained to you about sinus rhythm, irregular heart rhythm. And given that she had 300 milligrams of Cordarone. Again, Cordarone is also known as Amiodarone. She must have had an irregular heart rhythm, at least temporarily.
Juan: She did have.
Michelle: She did have it once, which is why they gave it. Yeah, you’re right.
Patrik: Right. If that fixed the problem, that’s great. But it’s just when someone is on VA-ECMO, has had a heart attack, the risk of going into atrial fibrillation is high, which brings me back to the potassium. Potassium level monitoring and managing the potassium level is critical, because if it drops below 3.5, going back into atrial fibrillation is high.
Suggested links
Michelle: Right. So we have to ensure that they’re monitoring the potassium.
Patrik: Absolutely. And it looks like they are.
Michelle: Sure.
Patrik: But my first guess would be why did she need Cordarone? Why did she need that? My first guess would be, okay, she probably went into atrial fibrillation. Then my next question is, why did she go into atrial fibrillation? Well, the answer to that question is, they didn’t manage potassium and also magnesium levels properly, or…
Michelle: Exactly.
Patrik: Right. Or she might’ve been fluid overloaded, or it might’ve been a result of the heart attack.
Juan: I think the combination of both because after that they started focusing on the potassium and magnesium.
Patrik: Yeah. Most likely combination of all of it. Yeah. But like you said, I agree that just by looking at everything, the balloon pump obviously concerns me. I probably agree with you without having spoken to the doctors, that they are pushing the envelope. Yeah. How often do you speak to the doctors? Every day?
Juan: Yeah. Quite often.
Patrik: Right. Prior to this event, or to those events, the lungs were not an issue. Mom is not a smoker.
Michelle: No.
Juan: I mean, she was, about 20 years ago, then she gave it up.
Juan: And then again, she started smoking. Yeah, she was the smoker…
Patrik: But not recently.
Juan: Not recently, not in the last I think one year.
Patrik: Okay. Okay. What picture are they painting in terms of… They’re probably taking day by-
RECOMMENDED:
Juan: You know what? Feels a little bit like they are dancing around exactly saying how they’re going about it. I think they are figuring it out as well. I mean, we know that they’ve been trying to get the ECMO off. They’ve been trying the whole week. That’s pretty clear.
Patrik: If I was you, I would throw that scenario at them and say, “Okay, you’re taking VA-ECMO off. Let’s just say you’re succeeding with that. And then you’re going on to VV-ECMO. That’s all great. What’s next?” I would throw that scenario at them.
Juan: You mean in terms of the balloon pump?
Patrik: Yeah, not only at the balloon pump, but let’s just say best case scenario. Best case scenario is take ECMO off, take balloon pump off. That’s the best case scenario.
Juan: Right. Right.
Patrik: And then you’re left with VV-ECMO, and what’s next?
Juan: Right. I guess the ventilator would-
Patrik: Yeah. Yeah.
Kevin: And another concern as you said was probably the Atracurium.
Patrik: Oh, huge. Huge concern. Atra is fine for a couple of days, but not for two weeks.
Kevin: It’s been a month.
Patrik: A month, has it?
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!