Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Should I Trust the ICU Team with Their Next Steps Whilst My Mom Is Critically ill in the ICU?
You can check out last week’s question by clicking on the link here.
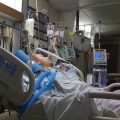
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Juan, as part of my 1:1 consulting and advocacy service! Juan’s mom is with a tracheostomy, balloon pump, and is on ECMO. Juan asks if how he will know if the ICU team is doing the right thing to get his mom off ECMO.
How Do I know if the ICU Team is Doing the Right Thing to Get My Mom Off ECMO?
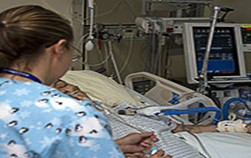
“You can also check out previous 1:1 consulting and advocacy sessions with me and Juan here.”
Patrik: Okay. The Impella is often being used for a bridge to a heart transplant. Now, that Impella can sometimes be in for months. And patients actually where I am, in one of the ICUs that I worked at, patients get the Impella. They are put on a transplant list, and they go home with the Impella plus either Dobutamine or Milrinone infusion. And that-
Juan: Okay.
Patrik: If you are on the Impella and a Milrinone or Dobutamine infusion, and you’re on a heart transplant list, you have no idea how long you are on the heart transplant list.
Patrik: It just doesn’t make sense from my experience.
Juan: Sure. Sure. No, that’s good to know. We can definitely discuss that then. I think we can push for it. Yeah.
Patrik: I’ll show you another thing. I will send you an ECMO weaning protocol. Just give me a second. I will send that to you now. It’s from one of the ICUs that I worked at. It’s coming now. You can have a look at that later.
RECOMMENDED:
Patrik: Yeah. You can see that Milrinone is on that list. You can also see that the balloon pump is on there. But I, in practice, I have not seen in practice what you are describing, ECMO plus balloon pump. I have never seen that.
Juan: Okay. Great. We can use this when we have the conversation, for sure.
Patrik: I think so.
Juan: Yeah. Yeah. We’ll do that.
Patrik: And you can see that Milrinone is documented on that document. And yeah. That’s all I can say.
Juan: Sure. Sure. We’ll discuss this. We’ll discuss this today and get back.
Patrik: What are they saying in terms of have they given you any timelines?
Juan: Not really.
Kevin: No. They’re going to see tomorrow how she is. Taking each-
Juan: Yeah. They’re taking each day at a time.
Recommended:
Patrik: Yeah. No. That’s good advice. Some people say the future doesn’t exist. What that means is you can’t predict the future. The future does exist. But at the end of the day, we’re all living in the present. It’s very difficult to predict the future. I mean, it looks like it’s already looking better than yesterday.
Patrik: Here is another thing with the Milrinone and the Dobutamine. I keep coming back to it. I apologize. But again, I think it’s important for you to understand. When you have balloon pump or ECMO, you need heparin. If you are weaned off the balloon pump and ECMO, you don’t need high doses of heparin. You might need a low dose of heparin. But the risk being on heparin for long periods of time is high. The side effects and the risk of bleed is just high. And I just think by introducing that Milrinone or Dobutamine and getting her off both, I just think it’s inevitable.
Juan: Sure. No, I mean, I appreciate you emphasizing it because it makes us that much more confident as well. I think we will push. We will push today.
Patrik: I don’t want to be … I’ll tell you what I have seen. Not very often, but I have seen it, someone being on ECMO, and let’s just say prolonged ECMO, which is probably two to three weeks is prolonged. And I have seen on the other case, again, not very often, but when it has happened, I clearly remember patients having a hemorrhagic stroke, having a brain bleed because of the heparin while they’re on ECMO.
Patrik: It’s terrible when it happens. It’s about risk management. And the sooner she can come off the heparin, the better.
Juan: Sure. No, I understand. We definitely want to minimize as much as we can.
Patrik: And they would know that. I mean, they would have probably seen it at some point.
Juan: They mentioned that as well, a few points that they want to be careful that there’s no bleeding in the brain and stuff.
Patrik: Absolutely. Absolutely.
Juan: Yeah. That’s definitely a whole bunch of good points that we can-
Kevin: Also the cardiac output is now 6.1-
Patrik: Yes. I’ve seen that. And that’s good. Its 6 point something with lower revs. So they reduced the output on the ECMO. Yesterday, it was sort of 3300, and today it’s 2995. They reduced that. And that’s a good sign, absolutely.
Suggested links:
Juan: Okay. Regarding the PA catheter, I think they said that they’ll keep it on right now, at least till they get the ECMO off, and they’re doing that first, I think. That’s what they said.
Patrik: Say that again please, regarding the what?
Juan: PA catheter. The PA catheter. They said that they were going to keep it on right now till they take off the VA ECMO and the balloon pump, I think.
Patrik: Yes. That makes sense. Again, it’s a great indicator for weaning. The PA catheter you can get all the numbers you need from the PA catheter. For anybody being weaned off VA ECMO, you can’t get more accurate numbers than from a PA catheter.
Patrik: However, again, similar to ECMO and balloon pump, high infection risk. But yeah, in terms of accuracy, it’s an amazing device for accuracy.
Kevin: Correct.
Juan: Sure. I guess that would be third in their list of priorities then. First is getting the ECMO off because those are larger and much more invasive lines or at least much more intensive lines, not invasive.
Patrik: Yeah. Look, PA catheter, the duration should be three days. It’s beyond that. It’s beyond that.
Juan: Yeah. I think that they also thought that they would get the ECMO off earlier and instead the PA catheter out, I think they’re first trying to get the ECMO off and then get the catheter out. I think they’re trying to handle the fish first, but yes. They did say … Yeah.
Patrik: But also there’s exceptions to the rule. And in this situation, you have to weigh up the risk. You have to weigh up the risk. In order to get the balloon out, and in order to wean the VA ECMO, you need those numbers.
Juan: Right. Yeah, I think that’s what they were thinking that they needed.
Patrik: Yeah, no. I can see why they’re doing it.
Recommended:
Juan: Okay. About the fibrosis medication, they said yeah, sure, no they’re not going to give it.
Patrik: And why is that?
Juan: Because I think it’s an experimental medication. It doesn’t have scientific literature on it. And it runs the risk of developing liver damage and also diarrhea. They just don’t think it’s necessary right now when she’s in such a precarious situation.
Patrik: Yup. Okay. Okay. And what are they saying if they can wean off the VA ECMO? What are they saying is next with her lungs, or is that too far ahead?
Juan: I think that’s a little far ahead, but I assume it would be VV going off next.
Patrik: Okay. You’ve seen her today, have you?
Juan: Yes.
Patrik: Is she waking up? Is she making eye contact with you?
Juan: They’ve closed her eyes. They’ve just put some eye drops and taped them down. But she is moving her head. She’s trying to talk. She keeps taking her tongue out. She’s shrugging and kind of squiggling around when she spoke to her granddaughter on the phone. I mean, by spoke to, I mean we put her on speaker and allowed her to speak. I mean, she was responsive to the family kind of speaking.
Patrik: Right. That’s good.
Juan: And she listens to the doctors now. They told us that now she responds to them and that when they tell her to stay calm she sort of listens and then she calms down.
Suggested links:
Patrik: Okay. That’s good. That’s good. That’s very good. That’s definitely improvement compared to yesterday.
Kevin: Yes.
Juan: Yeah. Yeah. I think so.
Kevin: They said she’s better than yesterday.
Juan: Yeah. They said that too. They said that today she’s doing better especially compared to yesterday and day before yesterday.
Patrik: That’s fantastic.
Recommended links:
Juan: Yeah. I think that those are the highlights. Her WBC count this morning was down to 10K. Her CRP was up 2.2. Her LDH was up 964. Sodium is down to 151. Potassium’s at 4.3.
Patrik: Sorry. Sodium is down to 151?
Juan: Yeah.
Patrik: Good. Good. Good. That’s good.
Juan: From 154 in the morning. In the evening, it was 151.
Patrik: And albumin and hemoglobin?
Juan: Albumin’s at 2.2. And hemoglobin, they sent the last test in at 6:00, so we should get it in a little bit. It’s 6:30 now, but in the morning, it was 7.1. But they said it usually is low in the morning after the night, and then by evening, it creeps up again.
Patrik: Okay.
Juan: We’ll get the next results and then message them to you as well.
Patrik: Yup. No, that’s much more positive than yesterday. Her ventilation settings compared to yesterday haven’t changed.
Juan: Yes.
Patrik: That’s good. The only thing that I have noticed, and that could just be a snapshot, when you look at her oxygen saturation from yesterday, it’s 100%. When you look at her oxygen saturation … But that could just be an artefact. It could just be as simple as by at the time when you were taking the photo that-
Kevin: Basically, it’s fluctuating between the high 80s and mid-90s. Some parts are at 100. The reason they also said this is because they reduced the flow today. The upper limbs are getting a little less because they reduced the flow on the ECMO.
Juan: And I think they said that the limbs that are farthest away from the ECMO are showing a little bit less saturation than the others.
Patrik: Yup. That would make sense. That would make sense.
Kevin: And also that since she’s off the Atracurium and the Midazolam she’s more awake now. She’s-
Juan: She’s just doing more on her own, I think.
Recommended:
Kevin: And that usually drops the saturation.
Patrik: Yeah. No. That all makes sense.
Juan: Okay. I think our two big points to bring up with them is one is definitely the Milrinone and Dobutamine, and the other one is about the pulmonary hypertension and why they think that’s not a concern.
Patrik: I would. I mean, it’s probably not an immediate concern because the heart is more important at the moment. But-
Juan: Yeah. I think just focusing quite heavily on the VA by getting the VA out, I think that’s the big thing in everyone’s mind, and I think that’s what they’re holding up for. By the end of the week, they said they were looking at doing it. And I imagine that if today they’re seeing it’s much better than yesterday and day before yesterday, then I can’t see why they wouldn’t be on track to do this tomorrow?
Juan: But I’m being cautiously optimistic obviously.
Patrik: Yeah. That’s good. That’s good. I’m just trying to think. Yeah, no. I think you’re watching all … Yes, who is in charge of weaning the ECMO? Is it ICU or is it the ECMO specialist? Is it the cardiologist? Who’s driving that?
Juan: It’s the ECMO specialist.
Kevin: It’s the ECMO specialist who’s also a cardiologist. She’s done heart transplants and bypasses and all of that. She’s a cardiologist and ECMO specialist.
Patrik: Right. Okay.
Juan: And there’s a couple of them actually. Two more consultants who are also ECMO consultants who are assisting and-
Kevin: There’s one doctor who’s done over something like a thousand ECMOs or something like that. How many do you think she’s done?
Juan: I think like 160 or something.
Kevin: Right. She’s done like … She’s quite experienced, yes.
Patrik: Yeah. That’s great. That’s great. That’s good. That’s good. Okay. Well, all you can do is take one day at a time and keep asking questions, I guess. Keep monitoring what you’re monitoring there. And hopefully tomorrow-
Juan: Patrik, I just wanted to ask you about that venous insufficiency. Can you tell us more about that? I mean, it worried me a little bit, and I just want to know more a bit more about that.
Recommended links:
Patrik: Basically, the ECMO machine is functioning as the heart and as the lung at the moment. Okay? Because the heart is not pumping at its full capacity at the moment, some organs are not getting as much perfusion as if the heart was pumping at normal capacity. Where is the access? Where is the access, and where is return? Where is it in terms of position, do you know?
Kevin: V-V is return, and access in the artery-
Patrik: Yeah. No. No. I know that of course. But where does it sit? Does it sit in the groin? Does it sit in both?
Kevin: I think it’s in the … Right?
Juan: Yeah. Yeah.
Kevin: The venous cannula, one is in the neck, and the other one is in the left leg. And the arterial cannula is in the groin.
Patrik: Yup. You can-
Juan: No. Sorry. Isn’t it the other way around? The arterial cannula is in the left leg, and the other V is in the left leg, in the groin area.
Kevin: In the right leg.
Juan: Sorry. Yeah. Right leg.
Patrik: It also depends on the size of the cannula. Sometimes they’re using a high flow cannula as opposed to a low flow cannula. I don’t know what they’re using obviously. But let’s just say for argument’s sake they’re using a low flow cannula. You can already see that the leg, for example, might not get the best perfusion at times.
Patrik: Am I making sense?
Juan: Yeah. That makes sense.
Patrik: Because it’s not the same than the heart pumping because the gas exchange and the pumping is more like … It’s extracorporeal. It’s outside of the body.
Juan: I understand. Yeah.
Patrik: That’s why. That’s the simple reason why there is low flow.
Juan: Is that something that then resolves itself, that can be resolved, if they’re seeing that there’s a small clot?
Patrik: Yeah. Yeah. It can be resolved, but again, that’s why it’s so important to get everything removed. The other issue is there would also be interference from the balloon. The balloon can cause obstruction as well.
Juan: Okay.
Patrik: Right?
Juan: Okay.
Patrik: Those are all the issues there. The sooner that can come out, everything can come out, the better.
Juan: Okay. You mean the balloon or-
Patrik: Or both. Balloon and the ECMO both.
Juan: If we just suggest or if we ask why can’t the VA and the balloon come off first or before the VV, what do you think that they might say in retaliation, and how do we kind of take that conversation forward?
Patrik: Say that again please.
Juan: If we say why aren’t we taking out the … If we use Milrinone and Dobutamine and this balloon pump could be causing this obstruction which is leading also to the venous insufficiency, then what might they say about why they can’t do that, and how do we kind of push that conversation forward?
Patrik: Yup. Great question. I would want to hear that answer too because it doesn’t make sense at the moment. I think you should ask that question, and I would be very interested in that answer too because it doesn’t make a lot of sense at the moment to me.
Juan: What if they say … I’m just assuming. I’m putting myself in their shoes here. What if they say one of two things? One is that she’s just not strong enough or maybe she’s not ready or we don’t want to remove all … What if she still needs support? That could be one thing that they say. Or the other thing is that we can’t remove two things at once. It’s just too much for her. That there might be too many complications with removing one and one.
Patrik: Could be. Could be.
Kevin: Yeah. Because I think they would essentially say that we need to monitor … If the VA is come off, then the first monitoring is within 24 hours and then 48 hours, and then if anything happens, we’ll put the cannula back in.
Patrik: Yeah. Yeah.
Kevin: And just being safe, I think, essentially is-
Juan: Yeah. Yeah. That’s what I’m thinking.
Patrik: Maybe that is what it is. Maybe it’s just extreme caution. Maybe it is.
Recommended:
Kevin: Do you think this caution could be a result of VIP syndrome?
Patrik: Well, is she a VIP?
Juan: Yes.
Kevin: Yes.
Patrik: She is? Okay. Yeah. Yeah. Then that’s the case. Yeah. Sure. Probably.
Juan: I mean, they’ve mentioned it to us once or twice as well when they said, “Look, we don’t want to treat her as a VIP.” And we’ve heard them say that, that we want to just treat her like a regular patient. And sometimes we can be over cautious.
Juan: They are conscious of it too.
Patrik: Right. Okay. Well, if that’s the case, yeah, that could play a part of it. As I said, from my perspective, if her ejection fraction is 30 to 35%, and they would add on the Dobutamine or the Milrinone, I would argue chances of her coming off are there. But then again, different hospitals have different protocols.
Juan: Yeah. Actually, the ECMO specialist, the main doctor who handles the ECMO said to us today, she was just giving us an example, she was saying last night they had a patient who was rapidly deteriorating, and they thought they had to insert a VA ECMO. But then they decided to wait for one or two hours, and then she rapidly improved, and today she didn’t need it at all. And she was just like, “Sometimes you just have to give it time. We wouldn’t have known if that would have been the right decision or the wrong decision, but in hindsight, obviously it was the right decision.”
Juan: I mean, she was just giving us examples I think of how it’s complicated.
Patrik: Yeah. Sure.
Juan: Yeah.
Kevin: Okay.
RECOMMENDED:
Juan: Okay. Sure. I think the balloon pump, Milrinone, Dobutamine point is the main one to bring up right now immediately, especially before tomorrow. And let’s see how they respond to that. And then I think we’ll bring up the pulmonary hypertension issue after that.
Patrik: Yup. Great. Great.
Juan: Okay. Thank you so much, Patrik.
Patrik: Pleasure. Pleasure. You’re welcome.
Juan: All right. Keep me in touch.
Patrik: Stay in touch. Thank you so much. Bye bye.
Juan: Thank you. Bye.
Patrik: Thank you. Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!