Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from one of our clients and the question in the last episode was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED“, I want to answer another question that we get asked frequently from our readers, but where we also believe our readers don’t know enough about the topic because we are finding that not all ICU’s are transparent about the options for some irreversible forms of heart failure and lung failure.
Can ECMO be a bridge to a heart transplant or a lung transplant?
Now first off, if you are reading the topic of this blog post and you are wondering what ECMO stands for, don’t worry we’ll get to all of that in a moment!
Given that you are here on this blog I must assume that you have a loved one in Intensive Care with some form of major and irreversible lung failure or heart failure and you are looking for a solution to this life threatening situation!
And give yourself a pad on your back for doing that! 99% of families in Intensive Care don’t know what to do, they don’t do their own research, they don’t question and they continue to be intimidated by the Intensive Care team!
Therefore, they don’t make any informed decisions, they don’t have peace of mind, control, power and influence!
I can’t tell you how many families in Intensive Care come to us when its too late, they come when we can’t help them anymore because their loved one has already passed away or is at a point of no return…
It’s very sad and it’s a sign that most families in Intensive Care underestimate the gravity of having a loved one critically ill in Intensive Care!
If your loved one is in Intensive Care, you and your family are in a “once in a lifetime” situation that you can’t afford to get wrong!
One of the reasons I decided to answer this question “Can ECMO be a bridge to a heart or lung transplant?” is that many families in Intensive Care come to us and they tell us that they have a loved one in Intensive Care with some form of irreversible heart or lung failure and therefore the Intensive Care team has told them that it’s “in the best interest” for their critically ill loved one to die…
And if you are like 99% of the families of critically ill Patients in Intensive Care, you again would have just nodded the death sentence of your loved one off without questioning and without doing your own research!
Recommended:
The quality of your questions will determine the outcomes and it will also determine the level of informed decisions you can make, it will determine the level of peace of mind, control, power and influence you will have also!
You must always, always question, because otherwise the Intensive Care team will drive their agenda and their agenda is often driven by their bed and staff availability, by their financial budgets, politics or by their medical research interests!
Recommended:
So let’s assume your critically ill loved one is in Intensive Care/ICU with one of the following respiratory and/or heart conditions.
ARDS, COPD (chronic obstructive pulmonary disease), Cystic fibrosis (CF), Idiopathic pulmonary fibrosis, Interstitial lung diseases, Primary pulmonary hypertension and also previous lung transplant.
Cardiomyopathy, heart failure, cardiogenic shock, heart attack, ejection fraction <30%, previous heart transplant, recurring ventricular arrhythmias, LVAD.
Therefore, if your loved one has been admitted to Intensive Care and is in one of the situations I mentioned before and the Intensive Care team is suggesting that the only option for your loved one is to die, you should consider your options and you need to start asking questions!
Again, the biggest challenge for families in Intensive Care is that you don’t know what you don’t know!
Another challenge is that most ICU’s don’t have ECMO available as a therapy option!
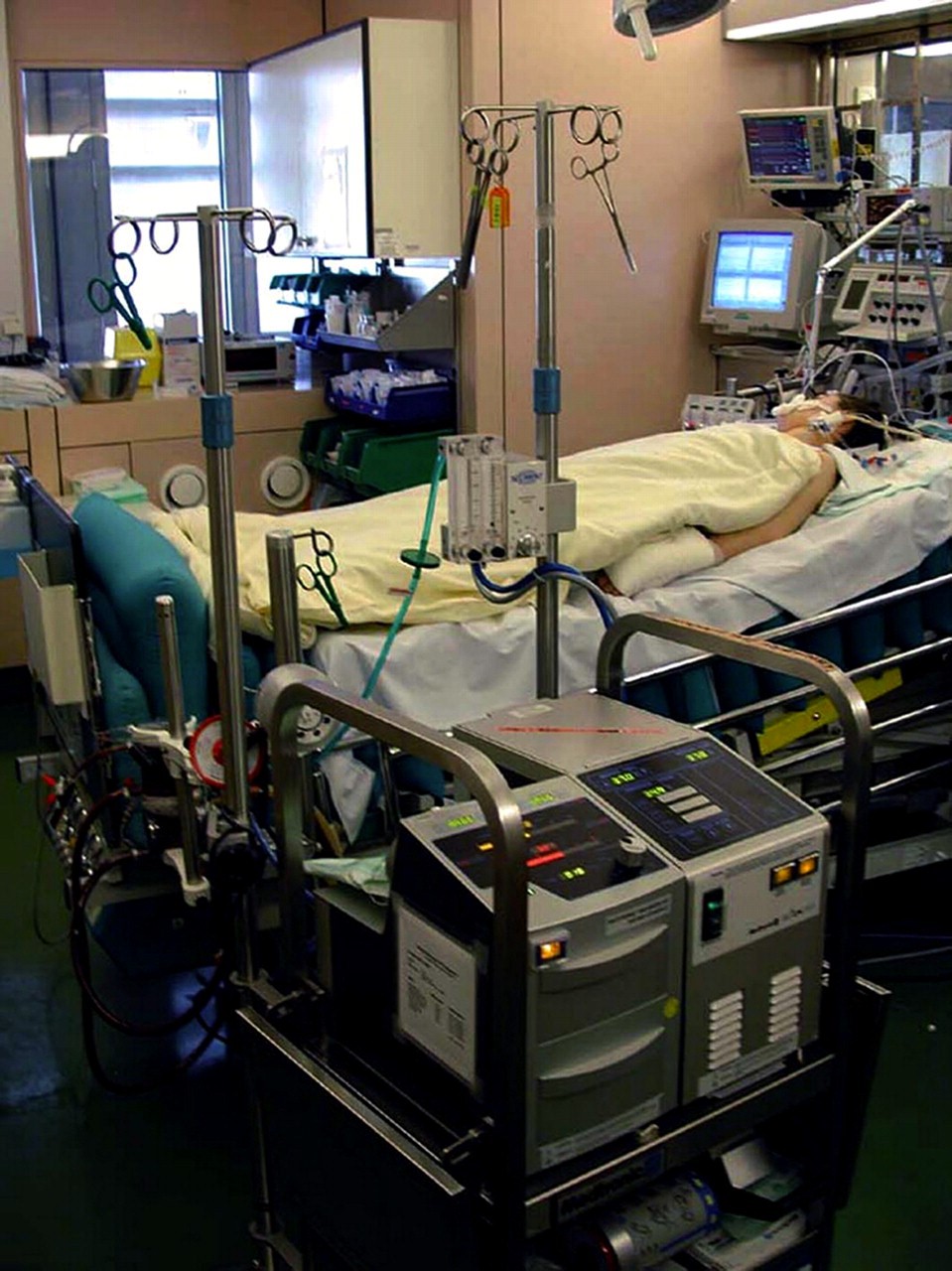
So what is ECMO? ECMO stands for Extracorporeal membrane oxygenation and you can find out more detailed information about ECMO here
http://intensivecarehotline.com/ecmoextracorporeal-membrane-oxygenation/
There are two major forms of ECMO VV-ECMO for all forms of lung failure and VA-ECMO for all forms of heart failure.
In essence VV-ECMO can take over the function of the lungs for a period of time and VA-ECMO can take over the function of the heart for a period of time.
VV-ECMO for end-stage lung diseases can be used as a bridge to a lung transplant and VA-ECMO for all forms of end-stage heart diseases can be used for a bridge to either a heart transplant or to a VAD.(=Ventricular assist device)
VA-ECMO for heart failure and end-stage heart disease can lead to a heart transplant but it can also be used for a VAD (Ventricular assist device) and that can be used as a bridge to a heart transplant. With a VAD Patients often can go home and await a heart transplant at home.
Recommended:
Why do most ICU’s don’t have ECMO available and why don’t they tell you about the option if they don’t have ECMO available?
First off, ECMO is a specialised therapy form that takes special training for doctors, nurses and perfusionists and it also takes expensive equipment such as the ECMO machine!
Even big ECMO centres only have a few machines and a few staff members available who are specialised to look after Patients on ECMO.
Especially in cases of VA-ECMO bridging to VAD or heart transplant, ICU staff also need to be trained to look after VAD!
Again, you need to ask and again the quality of your questions will determine the quality of outcomes you will get!
To give you some examples and case studies what could go wrong if you don’t start asking the right questions have a look at this case study from one of our clients here.
This case study in particular illustrates what can go wrong when Patients in Intensive Care get the wrong treatment and are not being referred to ECMO centres with a view of heart transplant!
On the other hand we also have some case studies from some of our other clients that will illustrate what ECMO can do for lung failure Patients even without a bridge to a lung transplant.
In clinical practice however, I have looked after quite a few Patients on VV-ECMO for lung failure and ECMO was the vehicle that was used to buy those Patients time to receive a lung transplant.
I have also looked after many Patients in ICU on VA-ECMO pre or post heart transplant and I also looked after many Patients on VAD.
Here are some case studies from some of our clients and you can see how they managed to get their loved ones through this ordeal with guidance, consulting and advocacy!
The bottom line is this, whenever you are in a situation where your loved one is in Intensive Care with some form or end-stage heart or lung failure and you are being told that there are no other options, chances are the Intensive Care may have gotten it wrong or they are simply not transparent with you and your family!
Again, the quality of questions will determine the outcomes and results you will be getting!
As you may be aware by now, not asking the right questions when you have a loved one in ICU or Intensive Care could be the difference between life and death!
It’s never what you’ve been told by Intensive Care teams that determines the outcome, it’s how you respond that determines the outcome!
How do I know?
After having worked in Intensive Care for nearly 20 years in three different countries where I literally looked after and worked with thousands of critically ill Patients and their families, I have seen my fair share ICU Patients, the outcomes, the politics, the dynamics, the psychology etc… in Intensive Care and I know the ICU teams communication strategies inside out!
I have also worked as a Nurse Unit Manager in Intensive Care for over five years!
Recommended:
Now, since 2013 I have consulted and advocated for hundreds of families in Intensive Care all over the world and I know how to get results for families in Intensive Care through advocacy, through asking the right questions, understanding the politics and the dynamics in Intensive Care inside out!
Furthermore, coming back to heart and lung transplant again, please also note that ECMO can sometimes be used after heart transplant or lung-transplant, especially when Patients are very unstable after heart or lung transplant.
Related article/video:
In the next episode of “your questions answered” we’ll continue with the series of consulting and advocacy questions with our client Sharon, it’ll come out in a few days, keep an eye on it!
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!