Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
My Dad is in ICU with Pancreatitis. When Can They Wean My Dad Off the Ventilator?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Bong as part of my 1:1 consulting and advocacy service! Bong’s mom is critically ill in ICU and Bong is asking how he can stop the ICU team from being negative of her mom’s condition.
How Can I Stop the ICU Team from Being Negative of My Mom’s Condition? HELP!
Hi Patrik,
I have seen your website and it’s providing good information that is why I decided to send you an email.
For the past 7 days, my mom has been off any pain meds or sedatives. In that time the ICU only ran trials to determine if she would stop breathing.
She failed 2 times in the past week when she was tested while sleeping and they reduced O2 to room levels and air pressure support was 10.
She has had no failures to breathe while awake. There has been no weaning her down to 9 or 8. Yesterday I got a therapist to run her at 8 and with room air and she tolerated that for 2.5 hours before it brought on gagging.
RECOMMENDED:
Sunday morning when I was not there they tested her while asleep at 10 and room air and she stopped breathing 5 times. I suspect it was due to having run her at 8 yesterday with no additional help during the night to rest and recover.
I do not remember what she spent the night at likely 12 and room air. The 5 failures to breathe shoots down my efforts to get them to wean Mom at lower pressure settings.
I was observing all but a few of the ICU’s therapy sessions and in none of them did they reduce the air assist below 10 in order to wean my mother off the ventilator. This was for the past 7 days. When a therapist did so yesterday mother breathed for 2 1/2 hours with O2 the same as in the room.
I confronted them and they admitted they had never been below 10 before except to test Mom at 5. I told them going from 10 to 5 and expecting my mother to perform at 5 without any weaning at progressively lower pressures 6,7 & 8 ensure failure.
Their response was, before waking mom up, they performed spontaneous breathing trials which she failed 5 times. So there never was any reason to wean mom to 5. I have asked for mom’s vaporizer records for the past week of being off sedatives to see how often she stopped breathing on her own. I will have the records tomorrow.
Related articles:
Mom has had an existing stroke injury that the medical staff says is likely why she now stops breathing. I suppose we could wait longer to see if this goes away but I doubt it. That is a question for those that specializes in stroke damage.
Regards,
Bong
Hi Bong,
Thank you for being a client, I really appreciate it.
The biggest challenge for families in intensive care is they don’t know what they don’t know. They don’t know what questions they need to ask. And worst of all, they don’t know how to manage intensive care teams.
Most families in intensive care feel completely powerless. And they think that you know, they have to look up and even worse, suck up to the doctors and the nurses in intensive care and they are at their mercy, and nothing could be further from the truth, especially if you know how to manage them.
If you know what questions you need to ask and if you get professional consulting advocacy from us here at the intensive care hotline, because we understand intensive care inside out then we can help you very quickly to make informed decisions get peace of mind control, power and influence in those situations.
Can you please send a picture off the ventilator, an arterial blood gas result, a picture of the bedside monitor, recent chest x-ray results, kidney function such as Urea, Creatinine, BUN.
Also, please send a list of current medications your mother is on.
Kind regards,
Patrik
RECOMMENDED:
Hello Patrik,
I will have the medical records Monday morning. I do not know if it will give the name of the ventilator or will include the x rays.
Her lung x-rays are clear I was told just a small collection of fluid still in the lung at the time of the last x-ray. Mom is producing a few table spoons of discharge from the lungs in the last 24 hr. A small amount of possibly dry blood came up yesterday.
Mom had a collapsed lung which has since fully recovered. The chest tube is out 5 days. Mom is off all antibiotics for the past 5 days. No sedatives or pain meds for 7 days. Mom has a failing heart valve and strokes.
The doctors are trying to claim the stroke has damaged her brain and that is the reason she stopped breathing. But that does not jive with the 2 prior times she stopped breathing early in her recovery.
Yesterday’s incident came right after pushing her until she failed at 8 and not giving her any extra O2 to recover overnight. Mom has no history of kidney problems.
My brother with a private practice in infectious disease will be here tomorrow when we will meet again with the staff who are trying to disconnect Mom.
He headed off prior efforts by the hospital to deny Mom the ICU treatment even after the lung collapsed. There was a small air pocket in the lung that had to be drained they claimed it was a major procedure.
My brother corrected them that it was a quick bed side procedure. My brother foresaw the time for the lung to re-inflate and stopped the hospital from removing Mom before 14 days the minimum for recovery. The hospital doctors are in their late twenties.
Now they are selling this stroke as a reason for Mom to stop breathing. It that was the case it would be happening daily. The prior two breathing stops were early in Mom’s recover when she was under stress. They did not reappear until I pushed Mom’s rehabilitation.
Regards,
Bong
RECOMMENDED:
Hi Bong,
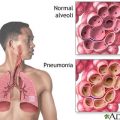
Extubation is the removal of the breathing tube or endotracheal tube after Intubation on the larynx or trachea (wind pipe). The purpose of extubation in Intensive Care is to take the Patient off mechanical ventilation so that he or she is able to breathe on their own.
“Normal” extubation parameters are:
- PEEP 5
- Pressure support <10
- FIO2 <30%
- Breathing spontaneously
- Good strong cough
- Can obey commands
- Minimal suction required
This is if someone has a good arterial blood gas result as well that confirms readiness for extubation on those parameters I mentioned above.
A stroke could potentially hinder swallowing properly, hence risk for aspiration post-extubation.
Please get more of the facts for a good assessment.
Kind regards,
Patrik
RECOMMENDED:
Hi Patrik,
Mom’s PEEP is consistently over 5. I have never seen it below.
The pressure support has run constantly at 10 for the last week with occasional 12 and 14 to assist in recovery from trials. At room air for last week. No effort was made except once to go below 10 once. This was without a doctor’s authorization.
Obeys commands, but spends long periods sleeping and difficult to get awake which ICU doctors encourage even when they are supposedly performing a trial. The therapists want Mom alert when performing trials.
If what appears to be gagging is actually an effort to cough then a strong cough. I have noticed less frequency of this coughing and less mucus from the lung tube. The doctors prefer to mislead with the claim Mom cannot protect her airway but they do not explain that this has to do with a strong cough. It is another ploy to justify ending her life.
There is now less and less need to put the suction tube down to her lungs to clear and extract mucus. Only when she has coughing fits. Those fits came about when I ran her at 8. Also when left at 10 for long periods.
RECOMMENDED:
When the therapist ran her at 8 for 2.5 hours the therapist was very pleased with performance. That was followed the next morning by 5 stop breathing events which the doctors have seized upon to renew calls to end her life.
The therapists rotate every 12 hrs. I do not see the same ones back for days. There is no one therapist that knows Mom’s case. They depend upon rotating doctors who issue commands and never oversee the treatment or results.
I am sending the hospital’s ICU weaning treatment. Nothing on gradually reducing air pressure.
Mom shows every sign of achieving 5, but they seize upon every excuse to call for end of life. One of the therapists cooperates with the doctors selling the 5 not breathing events Sunday morning as a reason, claiming it is evidence of brain damage.
Regards,
Bong
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!