Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
Your Questions Answered Live: How to treat COVID-19 ARDS/Lung failure in ICU!
You can check out last week’s question by clicking on the link here.
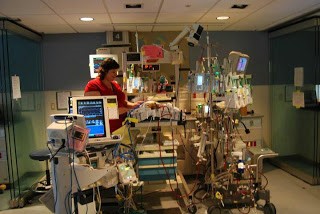
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Juan, as part of my 1:1 consulting and advocacy service! Juan’s mom is with a tracheostomy, IABP, and is on ECMO. Juan asks how his critically ill mom be able to successfully wean off from ECMO after a heart attack.
How Can My Critically Ill Mom Wean Off From ECMO in the ICU?

Patrik: Hey, Juan. Can you hear me?
Juan: Hello?
Patrik: Hey, Juan. It’s Patrik here. How are you?
Juan: Hi, Patrik. I’m fine, thank you. How are you?
Patrik: I’m very well, thank you. This is a good time?
Juan: Yes, this is a good time. I have Michelle and Kevin here with me.
Patrik: Sure.
Michelle: Hi, Patrik.
Kevin: Hi Patrik.
Patrik: Hi, Michelle. Hi, Kevin. How are you?
Kevin: Doing well. Thank you.
Patrik: That’s brilliant. That’s brilliant. So…
Patrik: Go on. What burning questions do you have to begin with?
Juan: So I guess, yeah. We’ve shared sort of the overall status.
Patrik: Yeah.
Juan: We’re kind of at a, I don’t know, potentially a turning point, but I mean, we’re cautiously optimistic in that sense because things have rapidly changed multiple times. As of now, she’s still on three to four machines. She’s on maximum support. I think we’re wondering how to go about weaning off the machines and balancing that with obviously being careful, but also understanding that she’s on extreme support for a while now.
RECOMMENDED:
Patrik: Yes, of course. How many days ECMO?
Juan: It’s been 14 days since the VA-ECMO. It’s been probably seven days with it being VAV-ECMO, and it’s been one day with VVA.
Patrik: Okay. What I don’t quite understand is why did she go on VA-ECMO? Has she had a heart attack? Has she had a cardiac-
Juan: Yes. Yes.
Patrik: Right.
Juan: She did. So we came to hospital because we suspected that she had a heart attack.
Patrik: Right.
Juan: That was exactly about a month ago on mid-July. So when we arrived and they took her in, and they did an angiogram, they found that she had a heart attack probably the night before or that morning. And actually about 20 years ago, she’d had an angioplasty and she already had three stents in her heart, from almost 20 years ago.
Patrik: Right. And now they stented it again.
Juan: They stented the LED.
Patrik: Yeah. Yeah. Stented the LED.
Juan: … which is a new stent.
Patrik: Right. Okay.
Juan: They found three other blockages in three of the arteries. The old stents essentially were blocked, but they said they would have liked to do a bypass, but obviously that wasn’t a question given her weak state.
Patrik: Okay.
Juan: Because of the COVID and issues and her lungs were quite damaged. So she had to be put on a ventilator immediately after the procedure.
Suggested links:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Patrik: Right. How old is your mom?
Juan: She’s in her 60s.
Patrik: Right. And any other pre-medical history?
Juan: Not really. I think the heart is the main issue.
Patrik: Right.
Kevin: Just the heart and hypertension and…
Juan: She’s not fit.
Kevin: She’s not particularly healthy and fit. She leads a very stressful lifestyle. She’s a workaholic.
Juan: Right.
Kevin: Works late out of the night, midnight, 1:30 AM.
Juan: No frequent exercise.
Kevin: Doesn’t exercise frequently. She had habits that are too bad and the lifestyle such as the high stress environment and generally that.
Patrik: Right. Okay. But no diabetes.
Kevin: Not before, but I guess now they’ve been… I mean, now during the procedure they’ve been mentioning it, but they haven’t really made a big deal out of it.
Juan: So, we’ve known her to be diabetic before this experience.
Patrik: Okay. Lot of patients in ICU go on insulin even though they’re not diabetic.
Juan: She’s not on any insulin right now.
Patrik: Okay. Fair enough. Okay. Sticking with the heart for the moment. So you are saying her ejection fraction was down to 20% at some point.
Kevin: When she came in.
Juan: Yes, when she came in.
Patrik: Right. And now it’s back up to 35, did you say?
Juan: That’s right.
Kevin: Between 30 and 35. They also attribute the increase to the supports because she’s on VA-ECMO.
Patrik: Of course.
Kevin: and IABP or Intra- Aortic Balloon Pump. She was on some inotropes before.
Patrik: That was my next question. So she’s on ECMO and IABP.
Juan: That’s right. So they had tried to wean off the VA-ECMO. They were trying that the whole week actually, the VAV, but she would desaturate and her BP was falling. So they needed to preemptively insert the IABP, which they had actually put in right when she came in. She had it in for four days, when she first was admitted, and then they took it out. So I think day before yesterday, they inserted the IABP again.
Recommended:
Kevin: They added the IABP before they were going to try weaning her off the VAV. So they added the IABP the day before yesterday. And suddenly, the blood pressure increased quite a bit, and they could come off the inotropes completely. In fact, now she’s on the IABP and the ECMO, the VA, which they’ve switched to a VVA. Her blood pressure is being maintained around 120, along with the sodium nitroprusside.
Patrik: Yes. I saw that. It’s always been hypertensive, if anything. When she was on inotropes, do you know what she was on?
Kevin: Yeah. So she was on noradrenaline 0.2, and a very small dose of vasopressin, about 0.02.
Patrik: Okay.
Kevin: But prior to that, it was a bit higher. It was 0.4 of Noradrenaline, and about 0.3 of vasopressin.
Patrik: Right. No Dobutamine, no Dopamine or Milrinone as far as you’re aware.
Kevin: No. No, none of that.
Patrik: Okay.
Kevin: None of that.
Patrik: Okay. Fair enough. Okay. And have any weaning studies being done?
Kevin: Well, about a week ago, they’d started to try and wean her off the VA, and they just wanted to leave as a VV. But every time, as we said, that they would try removing the VA, her blood pressure would drop. So then they slowed that down, and then they decided to make the switch. They added the inotropes, and then they decided once she’s on the inotropes, they switched it to VVA, and then they added the IABP.
Patrik: Right.
Kevin: I mean, now the blood pressure has gone the other direction. When they don’t have the sodium nitroprusside, the blood pressure goes up to about 150, with a mean of about 100, 110.
Patrik: Right.
Juan: Regarding the weaning studies, we’ll have to ask them again, exactly when they did one. As of today, they didn’t really say they had done one today, or yesterday.
Recommended:
Patrik: Okay. It’s a bit unusual. I haven’t really seen someone on VA-ECMO with sodium nitroprusside. That’s unusual in my experience, but I don’t see that as a negative at the moment. I mean, if anything, patients are usually hypotensive, not hypertensive. So that’s not necessarily a bad thing. Is she on any Heparin?
Juan: Yes. 500. Yeah.
Patrik: 500 units an hour. Probably while she’s on ECMO.
Juan: I think so. Yeah. I’ve noticed it going up over the last day and a half. I think it was 250, 300, 400. Just now when we went down to the ICU, it was about-
Patrik: Right. Right. That also leads-
Michelle: That’s also because she’s on so many machines.
Michelle: So they don’t want any clotting in the machine.
Patrik: Oh, absolutely. Absolutely. But I mean, the heparin is necessary. Just remind me again, how long has the balloon been in?
Michelle: One to two days.
Juan: They added it in just yesterday… I think one, one and a half days. Sorry. Time is just merged into one. I think yesterday or day before. We’ll just double check. So about one, one and a half days, I think.
Patrik: Okay. What’s your mom’s weight roughly?
Juan: About 92 kilos.
Patrik: About 92 kilos. Okay. I’m just quickly looking up. I’m just bringing up the picture of the balloon. So she’s on one and one. Do you know a little bit about the balloon?
Juan: Yes. They’ve explained it to us a little bit.
Patrik: The reason I’m asking is, she’s on one and one. So it means every time the heart beats, she’s also getting the balloon. One way to wean off the balloon is to put it to one to two and then to one to three. Yeah. What-
Juan: I think they mentioned that the balloon would be one of the last things to come off, if I’m not mistaken. I think they said that the VV-
Michelle: The VA-
Juan: The VA would come off first, then the VV. No?
Patrik: Yeah. Look, it is but very rarely have I seen… What I’ve seen from my experience is, balloon first. If the balloon doesn’t work, go on ECMO, but I haven’t seen as part of the weaning, that people go on a balloon, back on the balloon when-
Juan: I think the balloon situation surprised them, so they put it in prophylactically because they thought that her BP would drop once they wean, hence they tried to remove the arterial cannula. But then when her BP went up, they actually mentioned to us that she’s kind of performing better without the balloon, but they just put it in, so it’s not like they could take it out immediately either.
Patrik: I see.
Juan: I think it’s a bit of a strange situation. They’ve mentioned a few times that she’s doing some unexpected things and taking them by surprise.
Patrik: Right. Right. Okay. Yeah. I haven’t really seen that. I have seen balloon after heart attack. And then if the balloon is not sufficient, then you go onto ECMO. I have not seen the sequence where you’re putting the balloon back in to wean off VA-ECMO. I haven’t seen that in my experience.
Juan: So initially when she came in and then they put the balloon in for four days, and then they took it out, she was improving.
Patrik: Right.
Juan: And actually two weeks ago, suddenly, we suspected that and it was triggered by the blood transfusion. And then she rapidly desaturated. That was the night she was on her way to recover actually getting on ventilator potentially very rapidly. That’s the night they had just quickly put her on the ECMO.
Patrik: Right.
RECOMMENDED:
Juan: The VA-ECMO because that just took everyone by surprise. And then I guess weaning her…
Kevin: It’s also because she picked up some bugs in there. Some fungal infections, some…
Kevin: A bunch of things. ICU induced bugs or whatever.
Patrik: Right. That was my next question. Does she have an infection besides the COVID?
Kevin: So now everything seems to have settled, but when she desaturated right before they put her on the ECMO, she had about two or three bugs, fungal bugs. If you had heavy congestion and things of that sort.
Patrik: Right. Okay. Coming to the COVID or coming to the lung infection as such, does she have tracheostomy?
Kevin: Yes, she has a tracheostomy.
Patrik: How long ago has she had the tracheostomy?
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!