What is a stroke?
A stroke, or cerebrovascular accident (CVA), is the rapid loss of brain function due to disturbance in the blood supply to the brain. This can be due to ischemia (lack of blood flow) caused by blockage (thrombosis, arterial embolism), or a hemorrhage(bleeding into the brain, also associated with a higher risk of a Patient dying). As a result, the affected area of the brain cannot function, which might result in an inability to move one or more limbs on one side of the body, inability to understand or formulate speech, or an inability to see one side of the visual field.
A stroke is a medical emergency and can cause permanent neurological damage and death. Risk factors for stroke include old age, high blood pressure, previous stroke or transient ischemic attack (TIA), diabetes, high cholesterol, tobacco smoking and atrial fibrillation. High blood pressure is the most important modifiable risk factor of stroke. It is the second leading cause of death worldwide.
The onset and persistence of the resulting injury to the brain and nervous system (neurological system) depends on where the disruption of circulation or the Hemorrhage has occurred. It is important to understand that the disruption of blood supply to the brain can alter different areas of brain function, even though there is no direct damage.
An ischemic stroke is occasionally treated in a hospital with thrombolysis (also known as a “clot buster”), and some hemorrhagic strokes benefit from neurosurgery. Treatment to recover any lost function is termed stroke rehabilitation, ideally in a stroke unit and involving health professions such as speech and language therapy, physical therapy and occupational therapy. Prevention of recurrence may involve the administration of antiplatelet drugs such as aspirin and dipyridamole, control and reduction of high blood pressure, and the use of statins(Atorvastatin, Simvastatin). Selected Patients may benefit from carotid endarterectomy and the use of anticoagulants(I.e. Aspirin, Clopidogrel).
- The Brain
- What are the symptoms of a stroke?
- What tests are done?
- What happens in Intensive Care?
- How long will the Patient remain in Intensive Care?
- Internet Links
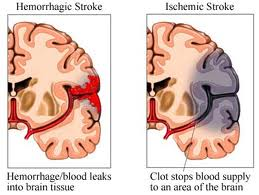
The image was found using a google search
The Brain
The brain is located between the skull and face bones and is attached to the spinal cord via the brain stem. The brain has many complex functions and is central to the functioning of body organs, nervous system and hormones. The brain has 4 main arteries that supply it, the right and left carotid arteries and right and left vertebral arteries. The brain is surrounded by layers or membranes that support the brain and moves blood and cerebrospinal fluid (the fluid produced in the spinal column to help with lubrication and suspending the brain to diminish any shocks from movement). All parts of the brain are at risk of being affected by a stroke. .
When someone has a ‘Stroke’ or CVA, it can mean there has been a blood clot in one of the arteries preventing blood supply to the brain(ischaemic stroke or CVA), or a bleed(hemorrhage) into the brain from a damaged artery or vein. The cause of a CVA will determine the treatment. The cause is also important when looking at the possible outcomes and prognosis of the Patient. The brain is a very complex organ and it is not always possible for medical and nursing staff to give a definite answer to your questions of what the outcome will be at the time of an injury.
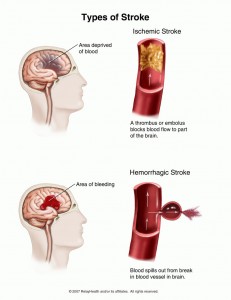
What are the symptoms of a Stroke?
Stroke symptoms typically start suddenly, over seconds to minutes, and in most cases do not progress further. The symptoms depend on the area of the brain affected. The more extensive the area of brain affected, the more functions that are likely to be lost. Some forms of stroke can cause additional symptoms. For example, in intracranial hemorrhage(bleed), the affected area may compress other structures. Most forms of stroke are not associated with headache, apart from subarachnoid hemorrhage and cerebral venous thrombosis and occasionally intracerebral hemorrhage.
symptoms may include:
- hemiplegia(one sided paralysis) and muscle weakness of the face
- numbness
- reduction in sensory or vibratory sensation
- initial lack of movement, replaced by spasticity (hypertonicity) and hyperreflexia
In most cases, the symptoms affect only one side of the body (unilateral). Depending on the part of the brain affected, the defect in the brain is usually on the opposite side of the body. However, since these pathways also travel in the spinal cord and any lesion there can also produce these symptoms, the presence of any one of these symptoms does not necessarily indicate a stroke.
In addition to the above CNS pathways, the brain stem gives rise to most of the twelve cranial nerves. A stroke affecting the brain stem and brain therefore can produce symptoms relating to deficits in these cranial nerves:
- altered smell, taste, hearing, or vision (total or partial)
- drooping of eyelid and weakness of eye muscles
- decreased reflexes: gag, swallow, pupil reactivity to light
- decreased sensation and muscle weakness of the face
- balance problems and nystagmus(involuntary eye movement)
- altered breathing and heart rate
- muscle weakness with inability to turn head to one side
- weakness in tongue (inability to protrude and/or move from side to side)
- Aphasia – not being able to talk because there are problems recognising what others are saying or problems expressing what they want to say
- Dysphasia – problems talking and pronouncing words
- Problems may appear in recognising people, reading words, common sounds, or a familiar touch. Ability to write, gesture, and express emotions can also be affected

What tests are done?
Stroke is diagnosed through several techniques: a neurological examination (such as the NIHSS), CT scans (most often without contrast enhancements) or MRI scans, Doppler ultrasound, and arteriography. The diagnosis of stroke itself is clinical, with assistance from the imaging techniques. Imaging techniques also assist in determining the subtypes and cause of stroke. There is yet no commonly used blood test for the stroke diagnosis itself, though blood tests may be of help in finding out the likely cause of stroke
- Computerised tomography scan (CT scan) – An x-ray which is taken in a machine which moves around the head /body to scan the tissues. The scan assists in identifying abnormal tissue changes
- Angiogram – A procedure where a catheter is inserted into an artery and guided into a blood vessel which supplies the brain and an x ray sensitive liquid is injected into the brain to review the blood vessels.
- Magnetic Resonance Imaging (MRI) – A MRI is a test which provides pictures of tissues by recognising different water density in body structures, and can identify specific changes in the brain from detailed images.
- Intracranial Pressure Monitoring(ICP monitoring) – A catheter which is inserted into the brain to measure the pressure in the brain
What are the treatment options for ischaemic stroke(CVA) and for hemorrhagic stroke for?
When there is a blood clot, there may be little or no blood supply to the brain beyond the blockage and this means the brain cells are starved of oxygen and nutrients and waste products build up in the brain cells. The initial reduction in blood supply causes the cells to stop functioning adequately and is called ischaemia of the brain. After a time of no blood supply, the cells die, and this is called infarction of the brain. The larger the area affected, the greater the number of brain areas involved. There are different medications which may be effective in treating a blood clot but this is individual to each Patient.
Definitive therapy in ischaemic stroke(CVA) is aimed at removing the blockage by breaking the clot down (thrombolysis), or by removing it mechanically (thrombectomy). The more rapidly blood flow is restored to the brain, the fewer brain cells die.
Thrombolysis (breakdown (lysis) of blood clots via drugs)
Thrombolysis with recombinant tissue plasminogen activator (rtPA) in acute ischemic stroke(CVA), when given before three hours of symptom onset increases the risk of death in the short term but in the long term improves the rate of independence and late mortality; the increase in long term mortality is not significant. When broken down by time to treatment it increases the chance of being alive and living independently by 9% in those treated within three hours, however the benefit for those treated between three and six hours is not significant. These benefits or lack of benefits occurred regardless of the age of the person treated.
Mechanical thrombectomy
Removal of the clot may be attempted in those where it occurs within a large blood vessel and may be an option for those who either are not eligible for or do not improve with intravenous thrombolytics. Significant complications occur in about 7%.
Hemicraniectomy
Large territory strokes can cause significant edema(swelling) of the brain with secondary brain injury in surrounding brain tissue. This phenomenon is mainly encountered in strokes of the middle cerebral artery territory, and is also called “malignant cerebral infarction” because it carries a dismal prognosis. Relief of the pressure may be attempted with medication, but some require hemicraniectomy, the temporary surgical removal of the skull on one side of the head. This decreases the risk of death, although some more people survive with disability who would otherwise have died.
When there is bleeding(Hemorrhagic stroke), the wall of the blood vessel is damaged and so blood leaks into the surrounding brain tissue where there is normally no blood. This blood forms a clot and begins to compress and destroy local brain tissue.
This places pressure on the surrounding cells and the blood supply to these areas are also affected because the blood supply is prevented from getting to the cells and they start to die. Sometimes surgery is indicated when a blood vessel is bleeding into the brain if it is likely to be stopped. Other times, the bleeding is too extensive to operate.
People with intracerebral hemorrhage require neurosurgical evaluation to detect and treat the cause of the bleeding, although many may not need surgery. Anticoagulants(blood thinners) and antithrombotics, key in treating ischemic stroke, can make bleeding worse. People are monitored for changes in the level of consciousness, and their blood pressure, blood sugar, and oxygenation are kept at optimum levels.
What happens in Intensive Care(ICU)?
- Your loved one is continuously monitored with a Bedside Monitors– Your loved ones vital signs such as Blood pressure is usually displayed continuously on the bedside monitor via an Arterial Catheter. Your loved ones Heart, Heart rhythm(ECG), temperature and breathing rate is continuously monitored and displayed on the monitor. Oxygen levels are continuously monitored by an oxygen saturation probe attached to the finger or to the ear. Furthermore oxygen levels are intermittently checked with ABG’s(Arterial Blood Gases), where blood is drawn out of the Arterial Catheter and tested immediately via a Blood Gas Analyser.
- Your loved ones breathing will be supported by additional oxygen via an oxygen mask, or Non- Invasive Ventilation(NIV) or BIPAP ventilation, however your loved one may be on a Ventilator (Breathing Machine) and have a Breathing Tube (Endotracheal tube) inserted into their airway. Some Patients need to be ventilated for more than a week and they require a Tracheostomy insertion. The ventilated Patient will require suctioning to remove secretions from the lungs and airways
- Some stroke Patients may require Intracranial Pressure Monitoring, which basically monitors the pressure in your loved ones head
- Your loved one will be receiving intravenous fluids via several intravenous cannula’s or Central Venous Lines(central line or CVC). A Urinary Catheter is used to monitor urine output and a Nasogastric Tubes will be used to rest the intestine if this has been injured or if your loved one requires ventilation.
- You can expect your loved one to have frequent Chest X-rays and blood tests(Blood& Pathology tests in Intensive Care) especially arterial blood gases (ABGs)
- Medication and intravenous fluids may be given via an intravenous cannula or a CVC(Central Venous Lines)
- Sequential compression devices may be put on the legs to prevent deep vein thrombosis
- An air mattress may be used to prevent pressure areas developing
How long will your loved one remain in Intensive Care?
Your loved one will remain in Intensive Care while they have investigations and treatment. If your loved one continues to require mechanical ventilation(Ventilator (Breathing Machine)) and have a Breathing Tube (Endotracheal tube) or a Tracheostomy, your loved one continues to be managed in Intensive Care. If your loved one is long-term ventilator dependent with Tracheostomy, click on this link for treatment options www.intensivecareathome.com.au
Each Patient’s condition is very unique and it is important to speak with the medical team caring for your loved one to discuss the potential outcome and prognosis.
Internet Links
- Stroke Foundation Australian stroke foundation
- http://www.strokeassociation.org/STROKEORG/ American stroke association
- http://www.stroke.org.uk/ UK stroke association
Any Questions?
Of course, if you have any questions or concerns, please discuss them with the ICU nurses and doctors.
All Intensive Care interventions and procedures carry a degree of potential risk even when performed by skilled and experienced staff. Please discuss these issues with the medical and nursing staff who are caring for your loved one.
The information contained on this page is general in nature and therefore cannot reflect individual patient variation. It is meant as a back up to specific information which will be discussed with you by the Doctors and Nurses caring for your loved one. INTENSIVE CARE HOTLINE attests to the accuracy of the information contained here BUT takes no responsibility for how it may apply to an individual Patient. Please refer to the full disclaimer.
Related articles:
- How to take control if your loved one has a severe brain injury and is critically ill in Intensive Care
- How long does it take to wake up from a Traumatic brain injury or severe head injury?
- What you need to do if your loved one in Intensive Care is brain dead or is considered for organ donation
- How long can a breathing tube or an endotracheal tube can stay in?
- How long should a Patient be on a ventilator before having a Tracheostomy?
- How long is a Patient kept on a BIPAP machine in Intensive Care?
- What is an induced coma and why is my critically ill loved one in an induced coma?
- The 3 most dangerous mistakes that you are making but you are unaware of, if your loved one is a critically ill Patient in Intensive Care
- How to always achieve your goals whilst your loved one is critically ill in Intensive Care
- Why you must make up your own mind about your critically ill loved one’s situation in Intensive Care even if you’re not a doctor or a nurse!
- Follow this proven 5 step process on how to be in control and influential if your loved one is a long-term Patient in Intensive Care
- How to quickly take control and have real power and influence if your loved one is critically ill in Intensive Care
- Why does my loved one need a Tracheostomy in Intensive Care?
- Tracheostomy and weaning off the ventilator in Intensive Care, how long can it take?
- Be more selfish if your loved one is critically ill in Intensive Care
- How to stay positive if your loved one is critically ill in Intensive Care
- 4 ways on how to be more persuasive if your loved one is critically ill in Intensive Care
- My sister has been in ICU for 21 weeks with Tracheostomy and still ventilated. What do we need to do?
- Severe lung failure and my aunty is not expected to survive…
- 3 quick steps on how to position and prepare yourself well mentally, whilst your loved one is critically ill in Intensive Care
- How to get what you want whilst your loved one is critically ill in Intensive Care
- 5 steps to become a better negotiator if your loved one is critically ill in Intensive Care
- How to make sure that your values and beliefs are known whilst your loved one is critically ill in Intensive Care
- How to make sure that “what you see is always what you get” whilst your loved one is critically ill in Intensive Care
- What the doctors and the nurses behaviour in Intensive Care is telling you about the culture in a unit
- How long does it take to wake up from a Traumatic brain injury or severe head injury
- How to take control if your loved one has a severe brain injury and is critically ill in Intensive Care
- Family Meetings in Intensive Care or the Elephant in the Room
- What you need to do if your loved one is dying in Intensive Care(part one)
- What you need to do if your loved one is dying in Intensive Care(part two)
- Intensive Care at its best?
- How INTENSIVECAREHOTLINE.COM Can Help You
- What you and your Family need to do if your critically ill loved one is very sick in Intensive Care and faces an uncertain future
- How long can somebody stay in Intensive Care?
- My Family can’t agree on what’s best for my sister in Intensive Care…Help!
- My husband is dying in Intensive Care, but we need more time…
- My mother sustained serious brain damage after a stroke and she now is in multi- organ failure


