Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How Much Longer Can my Critically Ill Mom Be on ECMO in the ICU?
You can check out last week’s question by clicking on the link here.
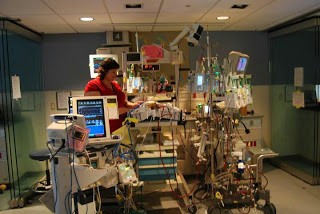
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Juan, as part of my 1:1 consulting and advocacy service! Juan’s mom is with a tracheostomy, balloon pump, and is now on VV- ECMO. Juan is asking what does recovery looks like for his mom on ECMO after leaving the ICU.
What Would Recovery Look Like for my Mom on ECMO After Leaving the ICU?

“You can also check out previous 1:1 consulting and advocacy sessions with me and Juan here.”
Patrik: That leads me to her liver function. Her liver function is slowly going down as well. I don’t know whether you’ve noticed that.
Juan: Mm-hmm.
Patrik: Are they saying something about that?
Juan: No, they didn’t really say, but we know that Ganciclovir can also affect liver function.
Patrik: Oh definitely.
Juan: And the Polymyxin as well was stopped a few days ago, but that could have some after-effects too.
Patrik: Yeah. You mentioned in your text earlier about there’s a little bit of bleeding from the lines. Her aPTT seems fine, her platelets seem fine, a little bit low, but not too low. So I’m wondering where the bleed is coming from. Are they saying anything?
Juan: Not really. They said they’ll keep an eye on it, I guess because of the heparin.
Kevin: This bleeding was a problem every time they did some kind of new procedure, whether they removed the catheter or they put in a new catheter, there was bleeding issues for her.
Patrik: I see. Okay, there’s nothing new there. The other thing is CRP levels…
Juan: It’s gone up.
Patrik: It’s gone up. And white cell count is normal.
Juan: It’s going down in size.
Patrik: Yeah. It doesn’t quite add up to me. Usually CRP and white cell counts often go hand in hand. If they’re going up, they’re going up, and if they’re going down, they’re going-
Juan: I think one of them also mentioned that CRP is kind of a non-specific indicator in some ways. So it could be multifactorial.
Patrik: Oh for sure. Look, it could definitely be multifactorial. The most important thing at the moment is that her blood gas is improving. That is the most important thing. There are definitely other issues with liver, kidneys. It almost looks like the moment like you can’t have an improvement with one organ without impacting on the other. That’s certainly a concern. With the Quetiapine and Olanzapine, yes definitely get a neurologist involved there. It’s damned if you do, damned if you don’t. The Midazolam-
RECOMMENDED:
Kevin: Yeah, that’s the question we had on basically the sedation and paralysis. And now that it’s been on for so long, it could be contributing to a lot of different problems including the ones we just spoke about. It could be a multifactor, and one of the factors definitely could be the sedation and the opiates.
Juan: I’d be surprised if it’s not..
Kevin: And the paralysis, that’s something that even the doctors want to try and take off or see how they can replace them.
Patrik: Yeah. You see, when you look at medication such as Quetiapine or Olanzapine, they are anti-psychotic medications. Your mom is not schizophrenic or anything.
Suggested links:
Juan: Yeah.
Patrik: I know it’s quite the common drugs in ICU when people come out of an induced coma, but they’re terrible drugs I believe. They’re anti-psychotic.
Juan: Yeah. We don’t want to use them also because honestly her mental state, from what we can gather, is quite strong. Yes she’s very active, and I guess that that’s a problem for her situation. But it’s almost a good thing in that like she’s that present, that her brain activity is high. So to suppress it, to me, sounds like something counter-productive almost. I understand that we have limitations and we only have so many options, but yeah that is a big concern on my mind as well.
Patrik: Yeah, absolutely. They’re terrible drug. Prolonged induced coma is always like a no-win situation. You need to sedate people to give them time to recover. And then when you get them out of the induced coma and try and wake them up, you got to go in with something else to manage that delirium.
Recommended:
Kevin: And it’s usually Olanzapine or Quetiapine.
Patrik: Olanzapine, Quetiapine and sometimes Haloperidol, which is even worse, I argue. Haloperidol is even worse.
Juan: So there’s nowhere else we’re using that?
Patrik: Another option is Clonidine. I think I mentioned that previously; Clonidine. There’s also some Clonidine in Precedex, which has had a few days ago. The problem with Clonidine is Clonidine is probably the best medication to get people out of an induced coma. The biggest side effect with Clonidine is hypotension – low blood pressure, and bradycardia- low heart rate. Not a great combination-
Patrik: Not a great combination, but as long as it’s definitely being used to wean people off sedation. But patients have to be hemodynamically stable.
Kevin: Yeah.
Juan: Yeah.
Patrik: But, have you seen her today?
Juan: Yeah. We aren’t going too close because of the candida and the other bugs. So we’ve seen her only from a distance. But yeah she seems all right. Obviously the edema is there and she’s looking a little pale, but yeah she’s okay. She was moving a little bit when I was speaking to her. I could see her switching a bit, but she wasn’t doing before I started speaking. So yeah she always responds when we speak, in some way.
Patrik: Great, that’s good. That’s a good indicator for you, I would think.
Juan: Yeah. And the sedation, whenever they reduce it, you just instantly see responses. She opens her eyes, she starts trying to talk. Whenever the paralytics are off, she does this tongue-twitching thing a lot. Like she keeps moving her tongue whenever she’s awake. They aren’t really sure why, they just want to make sure it’s not a concern, but I think it’s just her trying very hard to talk. Because she can’t move any other part of her body, her mouth is the only thing she’s tries to move.
Patrik: Right. What are they saying are the next steps? You’ve outlined doing another troponin test, you’ve outlined…
Juan: I think the main thing right now is they’re going to change the tracheostomy. They’re going to stop the magnesium, get that under control. They’re going to get these cultures and take a call on reducing the downside further, and then the sedation paralysis question has to be addressed. And then obviously on the side, hoping for the… Yeah, addressing the gastro issue, it’s true. Not feeding her.
Kevin: ..the gastro tube.
Juan: What about the gastro tube?
Kevin: That goes straight into the intestine and not into the stomach.
Juan: Oh, they said one option for the gastro issue is to use a gastro tube which bypasses the…
Kevin: Stomach and the big intestine and goes straight into the small intestine.
Juan: And that’s how you can deliver-
Patrik: Oh. So she’s got the PEG tube or a PEJ tube?
Juan: I don’t know. But they were saying that could be an option to consider if…
Patrik: Yes, it’s true.
Kevin: It goes straight into the stomach.
Patrik: Through the tummy or through the nose?
Kevin: Through the nose.
Patrik: I see. They’re probably talking about… Okay. So going forward, if she remains in that situation, she probably will need a PEG tube or a PEJ tube. So basically, a PEG tube is a tube that goes through the abdominal wall into the stomach. Basically it goes in the same place, just through the abdominal wall, as opposed to the nose, or the other option is a PEJ tube. It goes into the jejunum and it bypasses the stomach. I would argue, yes that could be an option going forward. How have they given you any timelines around that or?
Juan: They just said that that’s something that they’re going to discuss and consider, and then get back to us.
Kevin: But the PEG or the PEJ tube that you just spoke about, does that involve another incision or a puncture?
Patrik: It does. The PEG tube is a small operation, and so is the PEJ tube, and sometimes they combine both. Sometimes they-
Juan: So is that something that we should be keen on or not keen on, or I guess we’ll have to wait and see?
Kevin: Because they’re always worried about doing any kind of procedure with the bleeding and the heparin.
Patrik: Oh, absolutely. They would have to stop the heparin. Look, on the one end I would be worried. In some countries, they often do the PEG at the same time when they do the tracheostomy. I guess cross that bridge when they bring it up again.
Recommended:
Juan: Yeah, I think so. If the gastro issue is sort of resolved and that settles…
Kevin: The kidney.
Juan: … and the kidney issues as well, as they reduce the morphine and the Ganciclovir, then maybe we won’t have to deal with that. But let’s see.
Patrik: I think so.
Juan: Yeah. They’ve not come to any conclusions. These are all preliminary discussions that happened today. So it’s all still just playing out options I guess, and thinking ahead.
Patrik: Yeah, I think so.
Juan: Okay.
Patrik: So yeah it looks like one is improving, the other one is not. That’s what it looks like at the moment.
Juan: Yeah, it looks like a lot of the issues that are caused are now because she’s not healing fast enough to take off the supports and the medication, which is dealing with a lot of other issues that are coming up because of the ICU situation, the tubes, the fungal, the infections, the medications, the side effects of those medications, et cetera.
Patrik: Absolutely.
Juan: Yeah. Okay well her blood gases are improving. Let’s hope they continue to improve, and then if that gets better, then everything else maybe can also get looked after, bearing in mind if the infections, the fungal level and viral infections also come under control. So maybe that’s what we can just focus on, hoping for, when working towards.
Patrik: Absolutely. That’s what I’m thinking. And again it’s one day at a time, unfortunately. It’s good that you are telling everyone that she seems to respond to you, which is great. That is really positive, that’s important for you to recognize that that means she’s got life in her.
Juan: Yeah. Without a doubt, she definitely does.
Patrik: Right. And how are they in general? Are they staying positive? What’s your impression about that?
Juan: Well, I think it depends also from doctor to doctor. Some of the ICU doctors rather than the head doctors. I think it comes down to people’s perception of life, and how often staying positive they are in general. So I wouldn’t even say that anyone who’s negative is negative only for my mom. And I think it’s the kind of negative in general as people, or they’re more pessimistic in nature. And naturally they focus more on worst case scenarios and sort of seeing it as, “Oh, things are quite bad.”
Juan: But then there’s a whole lot of people who are really optimistic and who focus on, “Okay, these are great signs. Let’s focus on those, and yes we can manage these other things.” So, of course it’s a mixed bag, but I understand that in critical care, you have to have all guards up, and constantly be managing anything that may arise, any problems. So we’re taking it with a pinch of salt, and trying to focus on the positives.
Suggested links:
Patrik: Absolutely. And also at the moment, with COVID, all ICUs are breaking new ground.
Juan: Yeah, they are.
Patrik: All ICUs are breaking new ground. There are situations now that nobody would have ever predicted even two years ago. So, a lot of the things that are happening at the moment, I believe, are experimental.
Juan: They are, definitely. There’re experimental drugs like Remdesivir as they’re being given. And then they’re also open to alternative therapies that say, we might be that keen on exploring, like the ozone and stuff like that, Ivermectin or high-dose vitamin C. So I guess, yeah it’s a strange place to be.
Patrik: Yeah. It’s a strange place to be. I have not seen people being on ECMO for more than three weeks. That, in and of itself, I believe, is experimental. And what will also be experimental is if people survive this, what does their recovery look like, what does it look like once they’re leaving ICU.
Juan: Yeah. It’s pretty clear that this is a wonderful kind of scenario, I think. Yeah, I think we literally have absolutely no option but to stay one day at a time. Right now there’s no other way to think about it. It’s very strange.
Patrik: Yeah.
Juan: The doctors, I guess that’s what they’re trained to do and it comes through, they’re staying calm and confident, and not letting things show on their face necessarily, which I guess is a skill, and just keeping centered and thinking about, okay, next steps.
Patrik: Very much so. It’s a waiting game.
Juan: Yeah.
Patrik: And it’s also a good sign, in other jurisdictions, when she had this event yesterday, that they started CPR. In many other jurisdictions, they may have had the discussion with you even beforehand, saying, “We would recommend not to resuscitate.”
Juan: Oh really?
Patrik: Yeah.
Juan: Yes, the DNR, is what you’re saying?
Recommended:
Patrik: Yeah.
Juan: I know in the UK, it became a big issue as well.
Patrik: UK, America, everywhere. It’s a big issue. And it’s good to see that they have not mentioned anything to you about that. It’s a sign that they’re going full steam ahead.
Juan: Yeah, they absolutely are. I think that’s definitely the mindset, and I appreciate that of course.
Patrik: Yeah, absolutely.
Juan: Okay. Well maybe then let’s see by tonight. We’re doing another dose of the ozone therapy that happens tonight at 9:00. And yeah it went well last night. She’s been tolerating it well, and we’ve been able to do it with minimal movement. So, that’s good.
Patrik: Yeah, that is good. And any more issues around turning her?
Juan: Well, they’ve just not turned her, to be honest, since yesterday. I know they were a little bit nervous even about the ozone. So we managed to do it with minimal movement, and she responded well to that. There were no issues.
Patrik: So you are saying they haven’t turned her since the last event?
Juan: I don’t think they have. No?
Kevin: No.
Juan: No, they haven’t. No. Although her BP is now holding and they’re tapering off the Noradrenaline. I don’t know what it’s at right now, but this morning it was 0.1, and they were saying that they were just going to slowly taper it off because her BP is doing well.
Patrik: Right. I am concerned if they’re not turning her. Definitely concerned. But you got to see and you’ve got to keep an eye on it. But I am-
Juan: I know that after yesterday, they’re quite nervous that that moment when they lifted her to clean her, that that’s what may have contributed to the cardiac event. So I think maybe they’ll give it a day more, and see if her hemodynamics are stable, then maybe they could look at that.
Patrik: Yeah. But you can see what I’m saying, that if they don’t turn her, and she ends up with a pressure sore, that she-
Juan: We’ve been bringing up pressure sores like twice a day though. So it’s on their mind. We keep bringing it up, and they keep saying, “Yes, we’re keeping an eye on it. They haven’t turned her yet.” I brought it up every day.
Recommended:
Patrik: Okay. I can tell you that if they’re not turning her, they can’t keep an eye on pressure sores.
Juan: Yeah.
Patrik: They can’t. Because if you’re not turning, you can’t look at the skin. This is a massive risk.
Juan: So how do we get around the fact that obviously they’re scared to move her?
RECOMMENDED:
Patrik: Yeah. I’ll tell you how they might go around it, if they can’t turn her. They would need to use like a ceiling hoist, a hoist machine, and lift her in the ceiling, so they can take off the pressure off her back wash her back. Someone can look at her back while they are hosting her. That is the only way. And I’ve looked after many patients on ECMO that you can’t turn, because they are too unstable. And the way to manage them is, most bed spaces where I worked at and we had patients on ECMO, there was a ceiling hoist in the bed space, and we were using the hoist to lift patients up. Because you’re not changing much of their position, you’re just lifting them up, that’s how they stay hemodynamically stable, and that’s how you manage the pressure sore. Now, I don’t know whether there is a ceiling hoist where your mom is or not.
Juan: I don’t know either. We have to ask.
Kevin: We’ll ask them.
Juan: We’ll ask them.
Patrik: Yeah. You definitely have to ask them.
Juan: Okay.
Patrik: Because if she keeps improving, you don’t want the pressure sore to…
Juan: … throw that off.
Patrik: … throw that off.
Juan: Yeah, I understand. So I think we can just ask them about the hoisting, and if they have that there and how are they thinking about lifting her up.
Patrik: Yeah.
Juan: Okay, sounds good.
Patrik: Okay. All right. Let me know if you want to talk later.
Kevin: Thank you.
Patrik: Thank you.
Juan: Yeah. As soon as we have another update or something, we’ll just forward you the images as well.
Patrik: Yes please, yeah. Okay great.
Juan: Okay. Thank you Patrik.
Patrik: Thank you so much. Thank you. Bye.
Juan: Bye.
Patrik: Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!