Most of the patients in intensive care unit (ICU) are unable to swallow or otherwise unable to receive nutrition by mouth either because they are sedated, intubated or with difficulty swallowing, intestinal failure, head or neck cancer, or they are patients with gastrointestinal disease. In such cases, intravenous nutrition is necessary or inserting a feeding tube may be desirable.
There are several types of feeding tube insertions, differing depending on location and method of insertion.
- Nasogastric tube – tube is inserted through the nose and into the stomach.
- Percutaneous jejunostomy – tube inserted into part of the small intestine.
- Percutaneous Endoscopic Gastrostomy – a tube into the stomach which can be done with a very small incision.
WHAT IS PERCUTANEOUS ENDOSCOPIC GASTROSTOMY?
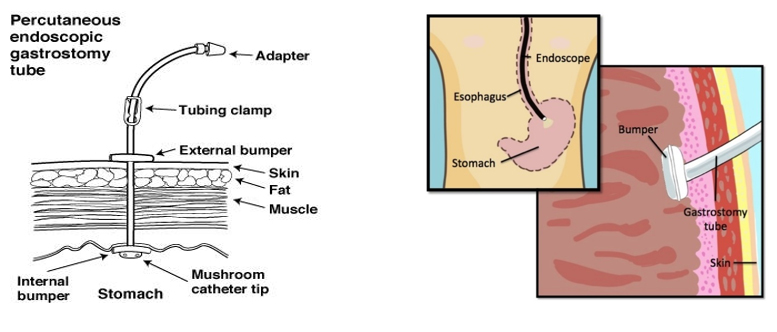
The term percutaneous endoscopic gastrostomy clarifies the details of the method of insertion of this particular type of feeding tube.
- Percutaneous is a synonym for transdermal, meaning “through the skin.”
- An endoscope is a long, slender optical instrument containing a light source and a camera and used to examine areas deep within the human body.
- Gastrostomy refers to an opening into the stomach through the abdominal wall.
Percutaneous endoscopic gastrostomy (PEG) is a surgical procedure for placing a tube for feeding without having to perform an open operation on the abdomen (laparotomy). It is used in patients who will be unable to take in food by mouth for a prolonged period of time. A gastrostomy, or surgical opening into the stomach, is made through the skin using a flexible, lighted instrument (endoscope) passed orally into the stomach to assist with the placement of the tube and secure it in place.
Percutaneous endoscopic gastrostomy (PEG) is performed to deliver enteral nutrition directly to the gastrointestinal tract, bypassing the oral cavity. It plays an important role in maintaining nutrition in patients unable to eat orally. Such patients include those with PEG is first line treatment for patients with a functional gastrointestinal tract but inadequate oral nutrient intake who require long term nutritional support (>30 days).
A percutaneous endoscopic gastrostomy (PEG) is a safe and effective way to provide food, liquids and medications (when appropriate) directly into the stomach.
WHAT ARE THE INDICATIONS OF PEG?
FOR ADULTS:
Indications include difficulties with oral intake often where obstruction to the upper airway or gastrointestinal tract makes passing a nasogastric tube difficult:
- Neurologically unsafe swallowing:
- Acute ischaemic or haemorrhagic stroke: in patients with acute stroke, gastrostomy feeding should be considered at 14 days post-stroke.
- Chronic progressive neuromuscular disease.
- Failure of feeding:
- Dementia; however, there is insufficient evidence to suggest that enteral tube feeding is beneficial in patients with advanced dementia. There is presently no evidence to suggest long-term survival rates improve in patients with advanced dementia who undergo PEG placement for difficulty of swallowing.
- Cystic fibrosis: PEG feeding is safe, efficacious and acceptable in children and adults with nutritional failure due to cystic fibrosis but should be carried out only in the context of close co-operation between cystic fibrosis chest physicians and an enteral feeding team.
- Peritoneal dialysis: PEG insertion can improve nutritional status but increases the risk of fungal peritonitis and failure of dialysis. PEG insertion can be undertaken in patients on peritoneal dialysis. Dialysis should be stopped for three days and prophylactic antifungal therapy given.
- Oro-pharyngeal and oesophageal malignancy: enteral tube placement into the stomach may hinder surgical techniques in oesophageal cancer and should be avoided if curative resection is planned.
- PEG tubes may also be indicated in other clinical situations such as malignant bowel obstruction, head injury, Crohn’s disease, fistulae, other causes of short bowel syndrome, AIDS and HIV encephalopathy, and severe burns.
- Usually PEG and Tracheostomy with Chronic Illness coincide. PEG feeding (infusion of nutritional feeds through an artificial opening into the stomach, as the patient has lost the ability to swallow due to some neurological change), and Tracheostomy management (an artificial airway into the trachea that reduces the effort in breathing and clearing of the secretions (most commonly related to similar neurological conditions that affect the swallowing mechanism).
FOR CHILDREN:
In the past, it was considered that the lower limit of body weight to insert PEG tubes should be 10 kg but PEG has been reported to be inserted safely in infants with a weight as low as 2.3 kg. The use of PEG may be indicated for children with:
- Neurological disorders with inability to swallow or dysphagia.
- Craniofacial abnormalities.
- Oncology problems with malnutrition.
- Other clinical conditions that lead to wasting and malnutrition – eg, chronic kidney disease, cystic fibrosis, metabolic problems, chronic infection such as HIV, cardiac disorders, short bowel syndrome and Crohn’s disease.
- Children with severe neurological impairment requiring tracheostomy and long term ventilation may have significant oral motor dysfunction and are at increased risk of nutritional deficiencies, poor growth, and aspiration pneumonia. PEG tube feeding is increasingly being used for nutritional support in these children.
WHAT ARE THE BENEFITS OF PEG TUBE FEEDING?
PEG feeding provides valuable access for nutrition in patients with a functional gastrointestinal system. Its high effectiveness, safety and reduced cost underlie increasing worldwide popularity. Benefits include:
- It is well tolerated (better than nasogastric tubes).
- Nutritional status is improved.
- Ease of usage over other methods (nasogastric or oral feeding) reported by carers.
- Satisfactory use by home carers.
- Low incidence of complications.
- Reduction in aspiration pneumonia associated with swallowing disorders.
- Cost-effective relative to alternative methods, particularly when reasonably long survival is expected.
WHAT ARE THE DISADVANTAGES OF PEG TUBE FEEDING?
Nasogastric tube (NGT) feeding is a classic, time-proven technique, although its prolonged use can lead to complications such as lesions to the nasal wing, chronic sinusitis, gastro-oesophageal reflux, and aspiration pneumonia. Another method of infusion, percutaneous endoscopy gastrostomy (PEG), is generally used when there is a need for enteral nutrition for a longer time period. There is a high demand for PEG in patients with swallowing disorders, although there is no consistent evidence about its effectiveness and safety as compared to NGT. (9)
Still, PEG tube feeding have several disadvantages:
- These medical devices are generally uncomfortable. This is particularly reported if the tube is not inserted properly. The body also needs some time to adapt to liquid food.
- In case of leakage at the site of insertion there is a chance of infections.
- Definitely the most serious problem and disadvantage of PEG feeding tubes is possibility of clogging.
WHAT HAPPENS DURING THE PERCUTANEOUS ENDOSCOPIC GASTROTOMY PROCEDURE (PEG)?
The treating doctor has a duty to obtain informed consent from competent patients and to undertake adequate consultation with those closest to patients not competent to make the decision. PEG tube placement should be carried out under full aseptic technique. Antibiotic prophylaxis is indicated to prevent skin site infection.
There are basic steps to a percutaneous endoscopic gastrostomy:
- First, the throat is anesthetized and an endoscope is passed into the stomach.
- Second, a small incision is made in the abdomen over the stomach and a needle is inserted into the stomach.
- Third, the feeding tube is slid through the needle into the stomach.
- Finally, the feeding tube is secured in place.
MANAGEMENT AFTER INSERTION OF PEG TUBE
- Education of carers and patients is essential to reduce tube problems and complications.
- A number of studies indicate the support and education of patients should be multidisciplinary, involving:
- Nurses (wound care and ostomy expertise)
- Dieticians (nutritional advice and support)
- Ongoing care involves:
- Inspection and maintenance of the access device
- Wound care advice
- Nutritional support and advice
WHAT ARE THE COMPLICATIONS OF PEG TUBE INSERTION?
IMMEDIATE (within 72 hours)
- Endoscopy-related:
- Haemorrhage or perforation
- Aspiration.
- Oversedation.
- Procedure-related:
- Ileus.
- Wound infection.
- Wound bleeding.
- Injury to the liver, bowel, or spleen.
DELAYED
- Gastric outlet obstruction
- Migration of the internal bumper of the PEG tube into the gastric or abdominal wall
- Dislodged PEG tube
- Peritonitis
- Peristomal leakage or infection
- Skin or gastric ulceration
- Blocked PEG tube
- Tube degradation
- Gastric fistula after removal of the PEG tube
- Granulation around site of insertion of the PEG tube.
Enteral feeding (or ‘tube feeding’) is a very common inpatient intervention to maintain nutritional status where the oral route is inadequate, unsafe or inaccessible. A proportion of patients will need to continue tube feeding in the community after their admission and will require a gastrostomy tube. Although gastrostomy insertion is relatively straightforward, it is not without complications in an often frail and vulnerable group of patients and a multidisciplinary approach is necessary to ensure that the procedure is appropriate. Some patients are better managed with careful assisted hand feeding or nasogastric tubes. Decisions regarding the provision of enteral nutrition at the end of life or where patients are not competent to make an informed judgement are particularly challenging and need to be made on a case-by-case basis.
Choosing the best method of nutritional support for an individual patient is often challenging. A thorough understanding of the patient’s needs, home circumstances and support alongside knowledge of the risks and benefits of each route of administration of enteral nutrition is paramount in making a good decision. This is usually best achieved by a multidisciplinary team including doctors, nurses, dietitians and, where possible, the patient and their carers. For patients at the end of their lives, the over-riding principle should be to preserve good quality of life for the patient.
REFERENCES:
- Percutaneous Endoscopic Gastrostomy (PEG)
https://my.clevelandclinic.org/health/treatments/4911-percutaneous-endoscopic-gastrostomy-peg
- Percutaneous endoscopic gastrostomy (PEG): a practical approach for long term management
https://www.bmj.com/content/364/bmj.k5311
- What is a Percutaneous Endoscopic Gastrostomy?
https://www.wisegeek.com/what-is-a-percutaneous-endoscopic-gastrostomy.htm
- PEG Feeding Tubes – Indications and Management
https://patient.info/doctor/peg-feeding-tubes-indications-and-management#nav-0
- Image from: Percutaneous Endoscopic Gastrostomy (PEG) Tube Placement
https://my.clevelandclinic.org/health/treatments/4911-percutaneous-endoscopic-gastrostomy-peg
- Image from: PEG Tube
https://www.pinterest.ph/pin/553098397956558264
- Percutaneous Endoscopic Gastrostomy (PEG)
https://www.medicinenet.com/percutaneous_endoscopic_gastrostomy/article.htm
- PEG Feeding Tubes – Indications and Management
https://patient.info/doctor/peg-feeding-tubes-indications-and-management
- Percutaneous endoscopic gastrostomy vs nasogastric tube feeding for adults
https://www.ncbi.nlm.nih.gov/pubmed/22419328
- Gastrostomy tube feeding in adults: the risks, benefits and alternatives
- Feeding Tubes Pros And Cons


