What is a Tracheostomy?
A Tracheostomy consists of making an incision on the anterior(front) aspect of the neck and opening a direct airway through an incision in the trachea(wind pipe). The resulting stoma(surgical opening) can serve independently as an airway or as a site for a tracheostomy tube to be inserted; this tube allows a person to breathe without the use of his or her nose or mouth. Both surgical and percutaneous(needle puncture of the skin) techniques are widely used in current surgical practice. The Tracheostomy tube is an artificial airway. Whether a surgical or a percutaneous Tracheostomy is performed depends on the benefits and risks associated with either procedure. The ICU doctors in consultation with an ENT surgeon will discuss the case and make decision, however most Tracheostomies are performed in the ICU percutaneously by the ICU medical team.
The tracheal tube inserted into the Tracheostomy is a catheter that is inserted into the trachea(wind pipe) in order for the primary purpose of establishing and maintaining a patent airway and to ensure the adequate exchange of oxygen and carbon dioxide. Many different types of tracheal tubes are available, suited for different specific applications. A Breathing Tube or Endotracheal Tube is a specific type of tracheal tube that is nearly always inserted through the mouth (orotracheal) or nose (nasotracheal). A tracheostomy tube is another type of tracheal tube; this 2–3-inch-long (51–76 mm) curved metal or plastic tube may be inserted into a tracheostomy stoma to maintain a patent lumen.
The following description refers to adult Intensive Care Patients.

Typical Tracheostomy Tube for Adults
What is it used for?
Tracheostomy tube insertion is commonly used in Intensive Care
-
to maintain a safe airway and a more comfortable long-term alternative to a generally uncomfortable Breathing Tube or Endotracheal Tube
- to protect the airway, whilst the Patient has a reduced level of consciousness, an upper airway obstruction
- for easier management of suctioning, especially if the Patient has excessive secretions and an inadequate cough
- for comfort and ease to wean a Patient off the ventilator(Ventilators (Breathing Machines))
- to reduce sedation, as Patient’s comfort is enhanced
- to successfully wean a ventilated Patient off the ventilator
Generally speaking, if your loved one faces a prolonged time(> 7 days as a rule of thumb) on a mechanical ventilator with a Breathing Tube or Endotracheal Tube, it is considered to be a safer and more comfortable option to place a Tracheostomy tube for Patient comfort. Another reason for a Tracheostomy insertion is if a Patient has swallowing difficulties and if therefore the Patient is at risk to aspirate(secretions going into the lung)
Tracheal tubes can also be used to deliver high oxygen concentrations, a scenario that is quite common in Intensive Care, or to administer other gases such as nitric oxide or certain volatile anesthetic agents. Tracheal tubes may also be used as a route for administration of certain medications such as salbutamol, atropine, epinephrine/ Adrenalin, ipratropium, and lignocaine.
 Tracheostomy with Ventilation in ICU
Tracheostomy with Ventilation in ICU
How Does It Work?
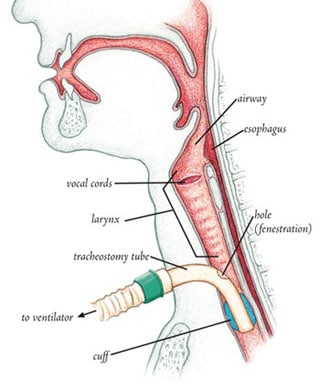
If your loved one has a Tracheostomy tube, air passes through the tube into your loved ones lungs. The Tracheostomy tube is secured and kept in place with a band around your loved ones neck. Furthermore a cuff around the tube is blocked with air, preventing any secretions and sputum to enter the lungs and also ensuring that whilst your loved one is mechanically ventilated that air and oxygen is not leaking out of the lungs, providing adequate and secure gas exchange. The Tracheostomy tube also provides an excellent and secure pathway to remove secretions(suctioning with Suction Catheters) from your loved ones lungs more easily.
In Intensive Care a Tracheostomy tube is viewed as a safe and temporary measure to provide safe mechanical ventilation until the Patient’s acute illness is over and/or until the Patient is fully independent from mechanical ventilation. As mentioned before, if your loved one is mechanically ventilated(Ventilators (Breathing Machines) for a prolonged period, a Tracheostomy tube usually makes it easier for them to breath, as well as having the ability to clean your loved ones mouth and also having the ability for your loved one to mouth words, if he or she is awake. Whilst having a Tracheostomy tube, your loved one is unable to speak. In some circumstances, after your loved one has managed without the ventilator for a while, but still requires the Tracheostomy tube, a speaking valve can be used which can allow your loved one to speak.
Once the reason/s for having the trache tube have resolved your loved one will go through a weaning process and the tube will be removed. This weaning process is supervised by the intensive care team. A small number of Patients are discharged from ICU with a trache tube still in. When this happens there is a special team of doctors, nurses, physiotherapists and speech pathologists who help the Patient – this may take from days to months.
Once the trache tube is removed the hole will close over and the person will be able to breathe normally.
In some instances a prolonged stay in Intensive Care is necessary for mechanical ventilation with Tracheostomy. With a prolonged stay and a prolonged ventilator dependency, we consider everything above 30- 60 days a long -term ICU stay. Usually a slow weaning process from mechanical ventilation is the underlying issue for the prolonged stay in Intensive Care. If the weaning process is a difficult and lengthy one, your loved one might feel depressed and weak, as it takes its toll to be long-term ventilated with Tracheostomy in Intensive Care.
Weaning Patients with Tracheostomy
For Patients who are long term mechanically ventilated with Tracheostomy there is also the option for them to go home and being weaned off the ventilator at home. There is more information for family members about weaning options off Tracheostomy ventilation in the home as a genuine alternative to a long-term stay in Intensive Care. Please find more information at www.intensivecareathome.com
Also, if you or your loved one want to go home with a tracheostomy it is possible, take a look for home-tracheostomy services here
Are There Any Complications?
Common complications may include
- Blockage and displacement of the tube
- Bleeding from Tracheostomy tube
- Pressure sores around the stoma
- Infection
Any Further Concerns?
Of course, if you have any questions or concerns, please discuss them with the ICU nurses and doctors.
All Intensive Care interventions and procedures carry a degree of potential risk even when performed by skilled and experienced staff. Please discuss these issues with the medical and nursing staff who are caring for your loved one.
The information contained on this page is general in nature and therefore cannot reflect individual Patient variation. It is meant as a back up to specific information which will be discussed with you by the Doctors and Nurses caring for your loved one. INTENSIVE CARE HOTLINE attests to the accuracy of the information contained here BUT takes no responsibility for how it may apply to an individual Patient. Please refer to the full disclaimer.
Related articles:
- How long does a cardiac arrest patient stay in Intensive Care?
- Six weeks in Intensive Care after Cardiac Surgery and my mother isn’t getting any better
- How long can a breathing tube or an endotracheal tube can stay in?
- How long should a Patient be on a ventilator before having a Tracheostomy?
- How long is a Patient kept on a BIPAP machine in Intensive Care?
- What is an induced coma and why is my critically ill loved one in an induced coma?
- The 3 most dangerous mistakes that you are making but you are unaware of, if your loved one is a critically ill Patient in Intensive Care
- How to always achieve your goals whilst your loved one is critically ill in Intensive Care
- Why you must make up your own mind about your critically ill loved one’s situation in Intensive Care even if you’re not a doctor or a nurse!
- Follow this proven 5 step process on how to be in control and influential if your loved one is a long-term Patient in Intensive Care
- How to quickly take control and have real power and influence if your loved one is critically ill in Intensive Care
- Why does my loved one need a Tracheostomy in Intensive Care?
- Tracheostomy and weaning off the ventilator in Intensive Care, how long can it take?
- My sister has been in ICU for 21 weeks with Tracheostomy and still ventilated. What do we need to do?
- Severe lung failure and my aunty is not expected to survive…
- 3 quick steps on how to position and prepare yourself well mentally, whilst your loved one is critically ill in Intensive Care
- How to get what you want whilst your loved one is critically ill in Intensive Care
- 5 steps to become a better negotiator if your loved one is critically ill in Intensive Care
- How to make sure that your values and beliefs are known whilst your loved one is critically ill in Intensive Care
- How to make sure that “what you see is always what you get” whilst your loved one is critically ill in Intensive Care
- What the doctors and the nurses behaviour in Intensive Care is telling you about the culture in a unit
- How long does it take to wake up from a Traumatic brain injury or severe head injury
- How to take control if your loved one has a severe brain injury and is critically ill in Intensive Care
- Family Meetings in Intensive Care or the Elephant in the Room
- What you need to do if your loved one is dying in Intensive Care(part one)
- What you need to do if your loved one is dying in Intensive Care(part two)
- Intensive Care at its best?
- How INTENSIVECAREHOTLINE.COM Can Help You
- What you and your Family need to do if your critically ill loved one is very sick in Intensive Care and faces an uncertain future
- How long can somebody stay in Intensive Care?
- My Family can’t agree on what’s best for my sister in Intensive Care…Help!
- My husband is dying in Intensive Care, but we need more time…
- My mother sustained serious brain damage after a stroke and she now is in multi- organ failure


