Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Toni as part of my 1:1 consulting and advocacy service! Toni’s mom is critically ill in ICU and Toni is asking how she can fight for her mom’s life whilst ICU team is giving up on her mom.
My Mom is Critically Ill in ICU and the ICU Team is Giving Up on Her. What Should I do?
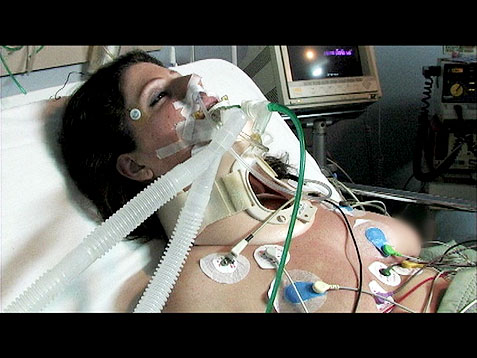
Hi Toni,
Nice to talk to you a moment ago.
As I mentioned, the biggest challenge for families in intensive care is that you don’t know what you don’t know.
Assessing if your Mom can come off the ventilator is dependent on multiple factors that need to be assessed.
It’s inappropriate for the ICU team to challenge your Mom’s advanced care directive.
After having worked in intensive care for 20 years I can help you fast making the right decisions and guide you with the decision making process, including but not limited to talking to the doctors directly or setting you up with the right questions to ask.
Regards,
Patrik
RECOMMENDED:
Hi Patrik,
I’m sorry it took so long for me to get back to you! I was finding ways to get my Mom’s medical records and we were able to access them online today. We feel a strong sense of urgency to get my Mom transferred because we do not feel they have been honest based upon her medical X-rays. We were told on February 22 by her doctor that my Mom suffered a punctured lung during her intubation but now they are saying she never had one.
However, notes on her X-rays seem to contradict that. So I wanted to see if I can sign up for the hour consult so you can go through her chest X-rays and help us clinically understand what they are saying. Just let me know your thoughts.
Again, this is a major sense of urgency so please let me know if you can help us out. I almost feel a bit panicked knowing they have not been honest. I know I mentioned to you that we felt they discharged her too early on January 10 which then led to her having to be re-admitted on February 2.
Our concern is she was intubated on February 21 and we were never given a solid reason as to why and then told on February 22 she had a punctured lung. Now they say she never had a punctured lung and actually want us to take her off the ventilation and let her go. They were going to discharge her on February 20 and then all this happened. Something just isn’t right!!
Regards,
Toni
Hi Toni,
We’re just reviewing the chest X-ray reports.
Do you know if your mom has a pleural drain or chest drain?
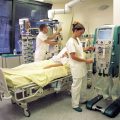
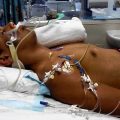
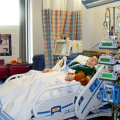
Also, would there be any chance you could send us a picture of the ventilator and the bedside monitor with the vital signs?
Kind regards,
Patrik
RECOMMENDED:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 2)
Hi Patrik,
She does not have a pleural drain or chest drain and they can take the picture first thing in the morning.
I will send over the pictures you requested tomorrow morning. I just wanted you to know a few things. We know how advanced our Mom is with her COPD so we aren’t expecting a crazy miracle.555 My Mom was scheduled for an appointment on January 7 for a consultation for newly approved non-invasive surgery to help with her quality of life. Then she fell and broke her arm and has just declined so much.
This hospital stay has been a horrific experience and from the first day when she was re-admitted. We were told she will never leave there and we need to let her go. We were attacked for making her suffer.
We had the best Christmas this past year and she was able to get around on her own but my sister was by her side through all of this. My family lives in a small town and this hospital is known as a “death trap”.
We had no choice where she would be taken when the ambulance picked her up. Then on February 20, we had our third “Ethics” meeting in the morning and I told them her directive would not be changed. I told them we were seeking legal counsel because of her pre-mature discharge in January and because they were asking her when she was all alone to change her DNR and it was scaring her.
Then that afternoon we received the call for her discharge and were preparing to get her home. Then suddenly she was intubated on the 21st. We then request a transfer and it’s denied and we are told we need to extubate and let her go. She deserves so much more than this.
My sister has given up everything the last two years to take care of her. I have been supporting them financially and my parents don’t have a lot of money but I would do anything to make sure my Mom is safe. All she ever wanted was to be at home when it was her time and we want to fight and do everything we can to get her home.
I appreciate all of your help. I can sleep tonight knowing we can have a third person looking at her info so we can truly understand what is happening.
Have a good night!
Toni
RECOMMENDED:
Hi Toni,
Thank you Toni for sharing more of your Mom’s situation.
She definitely had a Pneumothorax after intubation.
We will send you a summary of what we found in chest X-rays and arterial blood gases from February 22-25 before 8am EST tomorrow.
Kind regards,
Patrik
Hello Toni,
As per your email with regards to the clinical information (chest x-rays and blood gases results) of your mom from February 21-25. Here are some points to note:
1. Chest x-ray on March 22 at 11:42 am, confirmed that your mom has pneumothorax.
IMPRESSION:
Small left lateral loculated appearing pneumothorax. This finding was called to the intensive care unit at 11:49 AM on 2/22/2020 and I was told that they were already aware of and acting on this finding. Progressive left basilar opacity has developed since the recent prior film with shift of the mediastinum toward the left suggesting this density represents atelectasis. Persistent right basilar opacity suggestive of pneumonia.
A pneumothorax is a collapsed lung. A pneumothorax occurs when air leaks into the space between your lung and chest wall. This air pushes on the outside of your lung and makes it collapse.
Pneumothorax can be a complete lung collapse or a collapse of only a portion of the lung.
A pneumothorax can be caused by a blunt or penetrating chest injury, certain medical procedures (like for the intubation when the doctor told you that they have punctured your mom’s lungs), or damage from underlying lung disease.
Now the question is, after knowing the result of her chest x-ray, what actions have they done for your mom? Has your mom received any immediate medical treatment for this? If so, what are those treatments? Have they inserted any chest tubes or drains?
A chest tube can help drain air, blood, or fluid from the space surrounding your mom’s lungs, called the pleural space. Chest tube insertion is also referred to as chest tube thoracotomy. It’s typically an emergency procedure. During chest tube insertion, a hollow plastic tube is inserted between your ribs into the pleural space. The tube may be connected to a machine to help with the drainage. The tube will stay in place until the fluid, blood, or air is drained from your chest.
It is also important to know that the standard practice is to place a chest tube for any pneumothorax occurring during mechanical ventilation, due to the risk of positive pressure expanding the pneumothorax into a tension pneumothorax. It is alarming as well knowing that the result of the chest x-ray on that date says that there is a “SHIFT OF THE MEDIASTINUM TOWARD THE LEFT” which can be a tension pneumothorax because any type of pneumothorax can lead to a TENSION PNEUMOTHORAX.
An emergent condition classically presenting with mediastinal shift is tension pneumothorax. This is caused by a leak in the pleural space that resembles a one-way valve. As a person inhales, the air leaks into the pleural space and becomes trapped. It cannot be released during an exhale. This process leads to increased air pressure in the pleural space that is life-threatening and needs immediate treatment. it is often noted because of a sudden deterioration in condition.
If there’s a high clinical suspicion for tension pneumothorax, needle decompression (should be performed with minimal delay). Place a chest tube as soon as feasible after needle decompression of tension pneumothorax.
2. With the most recent results of the arterial blood gases of your mom after intubation on February 21, it shows that your mom’s having persistent high PCO2 which they cannot control. Arterial blood gas (ABG) studies measure the degrees of acidemia, hypercarbia (increased CO2 in the blood), and hypoxemia (decreased O2 levels in the blood), the occurrence of which depends on the extent of cardiopulmonary compromise at the time of collection.
A person with COPD may have an increased pH and partial pressure of carbon dioxide (PCO2) because not enough carbon dioxide is being exchanged in the lungs. People with COPD may also display low levels of dissolved oxygen and oxygen saturation.
Oxygen saturation (sO2) is a measurement of how much oxygen is bound to hemoglobin and is expressed as a percentage. Oxygen saturation less than 94 percent indicates a decrease in respiratory function. Your mom’s having acceptable oxygen saturation with most of the blood gases and the ventilator setting specifically for the FiO2 should have been decreased but it was all set at 80%. What could be their reason for this? The doctors should be explaining to you their reasons and their next course of plan.
Your mom as a known case of COPD, treatment for her should be focused on any underlying conditions and improve her airway function. Some strategies include:
- Antibiotics (to treat infection) – Have they started any antibiotics for your mom for her pneumonia because it can aggravate her COPD primarily?
- Diuretics (to reduce excess fluid affecting the heart and lungs)
- Bronchodilators (to expand the airways)
- Corticosteroids (to reduce inflammation)
- Mechanical ventilation – your mom is currently ventilated and the ventilator setting should correspond accordingly to her current cardio respiratory status, chest x rays and result of recent blood gases.
I hope this helps. If you have any further questions, we’re always here to help.
Kind regards,
Patrik
RECOMMENDED:
Hi Patrik,
Thank you so much!!
I am composing an email to the hospital to request a meeting tomorrow to go over this information. I will be reaching out to you again for your availability.
We feel a sense of urgency with this and can’t express enough how much this means.
Thank you,
Toni
RECOMMENDED:
Hello Toni,
You’re welcome Toni! We’re always grateful to be of help.
Just update us on the time the meeting will commence tomorrow.
Take care.
Kind regards,
Patrik
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!