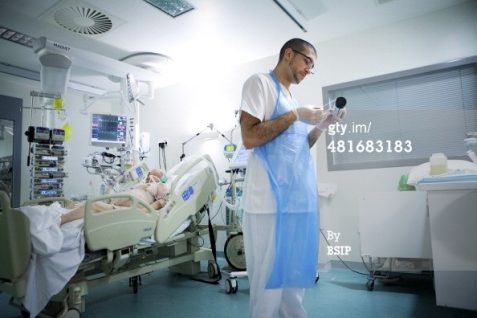
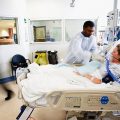
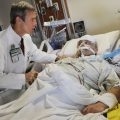
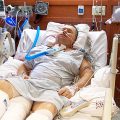
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
How Long Can We Get Our Sister Off the Ventilator in the ICU?
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Joyce as part of my 1:1 consulting and advocacy service! Joyce’s sister is still in the ICU on a ventilator. Joyce is asking, now that her sister is off sedation, can they bring her home while on a ventilator?
Can We Bring My Sister Home from the ICU Even If She’s On A Ventilator?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Joyce here.”
Joyce: So you could just tell me where I’m at. I’m going to wait for her to wake up. I’m going to tell them to go sit up. I’m going to actually call her, tell her to pull her up, let’s see how she takes that critique. When my sister wakes up, what advice would you give me from the emotional standpoint? Tell her, “You’re going to be okay. We’re with you.” Just that encouragement … I’m just freaking out.
Patrik: Yeah. You don’t necessarily have to tell her she’s okay. I mean, positivity I believe helps. But at the same time you don’t want to sort of mislead her either. Probably depends on how cognizant she is. It depends on a number of things. You know your sister best.
Joyce: Right.
Patrik: I do believe, it’s so important for her to hear you. I do believe that is so important..
Joyce: Do you think she still hears me now? I mean.
RECOMMENDED:
Patrik: Yes, she does, because what people also report after being in an induced coma, they do report that … I don’t remember much, but I do remember about my family talking to me. I do remember the nurse talking to me. Not that they can give you the specifics most of the time, but they do remember people talking to them, for sure.
Joyce: Okay. We’re going to do that. Nobody over there in the ICU is doing what me and my sister are doing, about having the tripod. Like we’re literally watching her like a security camera. It’s unprecedented. When people come in, we ask them questions, what are you doing? We have the closest hand on deck as possible.
Patrik: Absolutely.
Joyce: I mean, that’s all we can do..
Patrik: That’s all you can do for now. I can tell you what I’ve seen in the ICU over the years. I have seen people in ICU for months on end, on a ventilator, on a tracheostomy. Eventually they did come off in all age spectrums, the younger, the higher, the chances. But that’s not to say it can’t happen for your sister. But I’ve also seen the other end, where people come off the ventilator, then they bounce back, they deteriorate. There is no hard and fast rules.
Joyce: But I’m hoping maybe it’s COVID, and the lungs are going to work. Maybe I’m just being naïve.
Patrik: It’s not about being naïve. It’s unpredictable. It’s unpredictable for me, or for anyone. I’ve seen too much to say, “This is what it’s going to look like in four weeks’ time.” I wouldn’t put any money on that.
Joyce: So if we can get her off the vent. The number one goal is get her off this vent. We can get her off this vent. Then the first thing is she’s going to wake up, and then let her really aggressively breathe, and maybe we can get the numbers where we could be out. I guess that’s our next hurdle.
RECOMMENDED:
Patrik: Absolutely. Do you have access to your sister’s medical records?
Joyce: No.
Patrik: I think, as long as you can get information from the doctors, or the nurses, that’s fine. Some clients, they have access to the medical records online.
Joyce: I think I can request it, but it’s a whole thing. I think it would be easier for me to ask these direct questions.
Patrik: Right.
Joyce: And get back.
Patrik: I don’t think you need it at the moment, but there can be situations where-
Joyce: Actually I will ask. If the palliative guy ever calls me back, he’s the only middleman that I have at the moment. If he ever calls me back I’ll ask him if I can get the medical record. I don’t trust him. I’m telling you. He wants to get into my head. Every time I speak to him, I feel like pulling the plug. Literally, I mean, that’s how bad he makes my sister seem, and really it sucks.
RECOMMENDED:
Patrik: Right.
Patrik: What do you think he wants, the palliative care guy?
Joyce: He was babysitting me for every day for two and a half weeks. He was babysitting me, because when I got to the fork in the road of doing the trach or not, he really thought in hearts and hearts that we weren’t going to move forward with it, because I was really buying the story he’ s giving me. But the minute I told it to my mom, she’s such a believer, and she wants no medical information, she doesn’t even want to see my sister. She’s a believer, and we know she’s going to get out of it, and she made that trach decisions within two seconds. She made us go back to being a believer.
Joyce: We basically told the palliative care guy like, “We’re not going.” The minute that we moved forward with the trach, he ghosted us. He didn’t pick up the phone every day, he didn’t show up to the meetings. I actually said, “I feel a little ghosted.” He goes, “Yeah, you don’t need daily updates anymore. I’ll basically talk to you when I can.”
Joyce: He was so attentive, and now that we basically continued with this, listen, he wanted me to end it. He wanted me to end it, because he needs the bed, and I didn’t do it. Now it was like, what’s the point? I think palliative care is for the end of life.
Patrik: Exactly.
Joyce: And now that it’s not the end of life, he doesn’t really care.
Suggested links:
Patrik: Yeah. Quick other question, just remind me Joyce, this ICU is a small ICU?
Joyce: Correct.
Patrik: This is where I’m also wondering, how much experience do they have in the small ICU to wean somebody off the ventilator? I’ve mainly worked in big ICUs. Take a 40, 45 bed ICU, there is always 10 patients in there that need weaning long term. The exposure of the staff is there, and they have experience. You take, what is it seven beds, or 10 beds?
Joyce: I think it’s 10, but Melissa who’s been a 35 year old nurse, was the one that was able to take her off sedation when for three weeks everybody said, “She can’t tolerate it. She can’t tolerate it. She can’t tolerate it.” She came in and she goes, “I got it.” And she took her off completely. How do you explain that?
Patrik: Well, because she’s probably been around.
Joyce: Yeah, she’s like, “I got it.”
Patrik: That’s a red flag in and of itself.
Joyce: She said to me … Then I said to them, “How can it be that all these weeks you’re telling me she can’t tolerate even going down a little bit. And now all of a sudden overnight she’s a zero. That is so fishy.”
Patrik: Small ICU.
Joyce: I get the air pocket, but it was like, “Oh, we can’t do.” And now she just takes her to zero. That was so suspicious to me, so suspicious.
Patrik: Yeah. And you haven’t come across this lady before, this nurse?
Joyce: I think she was in the beginning, but they shift.
Patrik: Of course.
Joyce: She just came back into the picture where my sister was trached, and she was ready to go. She got her at a good time. But I felt like, she goes, “I spoke to the doctor. I have a plan today. I got it.” She got her off. I was like, “Oh my God.” Listen, she’s off now. I guess we’ll monitor, and wait for her to get off.
Joyce: I will advocate for everything you told me. I will advocate to get all the settings. I will text it to you. I guess this thing is just going to be where it goes, and I have to respect the process, because I will drive myself crazy.
Patrik: You can’t drive yourself crazy.
Joyce: I mean, I’m already crazy.
Recommended:
Patrik: Yeah. I know you can’t drive yourself crazy, because these could go on for a while with some ups and downs. But I do believe, now that we talk about this Joyce, the whole home care, I believe it’s now or never in terms of environment, right?
Joyce: Yeah, but how do I get them to do it?
Patrik: Let’s just say LTAC is not going to take your sister, because of the COVID.
Patrik: Let’s just say that’s the case. What are the options? The options are home care.
Joyce: Well, no. The option is she stays in the hospital.
Patrik: Sure. I get that, but then even the hospital wants her out. LTAC doesn’t want her, let’s just say that’s the case. LTAC doesn’t want her because of-
Joyce: They’ll take her. They’ll find it, like you said … From what I understand, they will find, because I spoke to many people, they say, they will find a location. I spoke to Joey, the palliative guy, he said, “You won’t be able to take her home, because the ventilator settings, there is nobody that really does it here. That’s very rare.”
Patrik: That is the challenge. But then again I do know Intensive Care at Home is doing it here, and there. We’ve certainly referred people to it, and then I get an email six months later saying, “Oh, thank you so much. We’re now at home with intensive care at home.”
Recommended:
Joyce: Basically if she’s at home, the advantage of home care is that she’s at home. I have physical therapist coming, I have this coming, that coming, that coming. The thing is, do I need the machine? The extensive physical therapy? Am I dumbing it down at home as well?
Patrik: No, you’re not dumbing it down. Yes, you need equipment, you need a ventilator, you need backup equipment, tracheostomy, you need all of that, but there is two hurdles for home care; the biggest hurdles, finance, and then staff. Let’s just say I was in your area. Okay, we get the finance, we can pull it off. We’d have no concerns there, but then you’ve got issues like, we’ve tried to put together a team, but then some of the team members are not right for your sister, not right for your family. So, there are lots of hurdles, can be overcome, but it’s certainly not a smooth and an easy process.
Joyce: Because you’re doing it on your own. That’s hard.
Patrik: Yeah. You’re doing it on your own. I mean, at the end of the day we’re setting up a mini ICU at home. That’s pretty much what we do. But you got to keep in mind, as positive as it sounds, you still got to keep in mind, all of a sudden you have strangers in your home 24 hours a day.
Joyce: Yeah. What a headache? Well, I guess, let’s see what happens. The best scenario is she’ll get off the ventilator before she leaves, and she’ll need a little thing. Let’s just hope. Listen, she never was up. So, she would never participate in getting better. All these signs showing that now her body is not in distress has to show an indicator that maybe the problem can be fixed. So, that’s the only thing we can go on. The fact that everything is still working, and she never participates. So, let her wake up, let her participate, let her actively get through this, and maybe she can get off the vent.
Patrik: Yep. You got to stay positive. No matter what happens, staying positive helps, no matter the outcome.
Recommended:
Joyce: Yeah.
Patrik: I know you’re realistic. The worst case scenario is … It’s always good in hindsight. Worst-case scenario, your sister is not going to make it, you have more time with her for now. You have bought her time to see what happens.
Joyce: Yeah. I mean, listen, I said toJoey, I said, “What if I want to do hospice?” He goes, “Right now, you can’t take her.” Look, if I get to the 60 day mark at the ventilator, and it really looks like it’s going to be a lifetime thing, then we’ll bring her home, and-
Patrik: Yes.
Joyce: But I’m still going to put the fight. I’m 25 days into it. That means I have a little bit more time to see which way it goes.
Patrik: 25 days. In a situation like this, I know 25 days is like an eternity for you and your family, it’s not much.
Joyce: But you do agree that the 60 day mark is telling?
Patrik: I would argue it’s the 60 day mark, that’s two months. It would almost go a little bit longer, maybe 80 days. I have seen people on a ventilator for 80, 90 days even, and they come off.
Joyce: But it’s rare?
Patrik: But it’s the longer the riskier.
Joyce: Right. I guess my sister is going to determine where she’s going to go with it.
Patrik: Yes.
Joyce: Her body is going to determine where it goes, and we’re going to follow, or we’re going to fight tooth and nails.
Patrik: You have put her in that position where hopefully she has the chance to take further steps, hopefully.
Joyce: Right. Okay. All right Patrik. I’m going to get you the information. Let’s take it from there.
Patrik: Yeah. Please.
RECOMMENDED:
Joyce: Till we talk again.
Patrik: Okay. Thank you Joyce.
Joyce: Bye Patrik.
Patrik: Take care. All the best.
Joyce: Bye-bye.
Patrik: Thank you. Bye-bye.
Joyce: See you.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!