Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
My Mom is In ICU After Cardiac Arrest. Does She Have Brain Damage, And Can She Survive?
You can check out last week’s question by clicking on the link here.
This is another episode of “YOUR QUESTIONS ANSWERED”. And in today’s episode, I want to answer a question from one of our readers, Rhea.
Rhea’s mother is recovering in the intensive care unit. She is asking, is moving to a long term acute care facility beneficial for her mom?
Is Moving to a Long-Term Acute Care Facility Beneficial for my Mom?
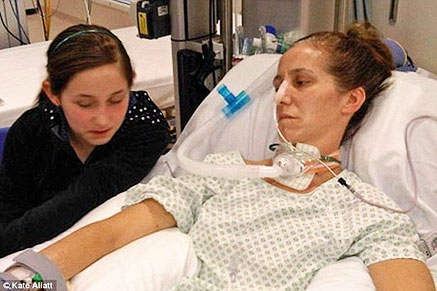
Hi Rhea. It’s Patrik here from intensive care at home and intensive care hotline. I’m just recording this message to talk you through what to look for and what questions to ask when your mom is going to an LTAC.
RECOMMENDED:
So first of all, when somebody is going from ICU to Long-Term Acute Care Facility or LTAC, you got to keep in mind that a patient is critically ill in intensive care and goes from a breathing tube to a tracheostomy and is in intensive care obviously, it requires the specialized skills of intensive care nurses, intensive care doctors, respiratory therapists, physical therapists, they’re all intensive care trained because anything that’s obviously life support related and tracheostomy ventilation, that’s all considered life support needs that specialized skill, specialized training that you’re aware of by now.
So when people go from ICU to LTAC basically most of the time it’s simply a money-saving exercise, especially where you are in the United States. Here in Australia for example there are very few LTACs. Most people get weaned off in intensive care with the tracheostomy and the ventilator successfully. And if they’re not successful, well here we are providing the intensive care at home service.
RECOMMENDED:
So basically the care in intensive care here, for example, continues with ICU doctors, ICU nurses, physical therapists, we don’t have respiratory therapists here in Australia, but that doesn’t really matter. The point is this, when somebody is on life support, ventilation, tracheostomy, and even if they come off the ventilator while they’re having a tracheostomy, a tracheostomy is still an artificial airway and an artificial airway needs to be managed and maintained. And the unfortunate issue in LTAC is the skills that are available in intensive care are simply not available in LTAC.
Also, you would have seen in ICU, now there’s one on one or one to two nurse to patient ratio at the most, whereas an LTAC, it’s often one to five and sometimes even one to ten overnight and again, they’re not ICU nurses. So you know, I mean you would have seen some of the reviews online for those LTAC facilities already and you would know by now it’s pretty dismal those reviews and from experience, we often have families come to us that have loved ones in LTAC and they’re literally begging us to help them get them home or get them back to ICU.
So, you know, the unfortunate reality is that LTACs are designed to, number one, empty ICU beds, number two, save money for the health funding agencies or you know Medicare, Medicaid or if your mom has private health insurance, I don’t know, but you, you get where I’m going with this.
RECOMMENDED:
So the other issue in LTAC is that, depending on the LTAC, there’s only one visiting doctor often again, and that is often a pulmonologist/respiratory physician. But again, the ICU skills are usually not readily available there. So here is another issue.
Another issue is simply that when patients deteriorate in LTAC, they then, need to go back to ICU. And now there are some LTACs that have an ICU attached. But again, it’s usually not at the quality or at the level than a big metropolitan ICU. It’s sort of a washed down ICU, if you will. But most LTACs don’t have an ICU attached in the first place, which means, patients do deteriorate and they often get shifted around, which is terrible.
You know, that a critically ill patient doesn’t need the added stress of going from a hospital to LTAC then potentially bouncing back to ICU. And often it’s not the same ICU because the LTACs are often far away from the referring hospital. There’s a number of issues attached when patients go from ICU to LTAC you know, I have seen so many situations now where the LTACs where families get referred to is two hours away, sometimes even further. It’s ridiculous. So from my perspective, there is very little rhyme or reason to send patients to LTACs.
RECOMMENDED:
But questions to ask the LTACs are the following, number one, what is their skill level? Are they working with ICU nurses, ICU doctors because of the artificial airway management? And at the end of the day, the artificial airway is life support. And you can’t just pick any RN to look after people with life support that come out of intensive care and that’s where the LTACs are falling short. The LTACs will most likely when you ask that question, the LTACs would most likely tell you that they have ventilator and tracheostomy competent nurses but they’re not ICU nurses, I can assure you of that. And then, they often have nursing aides working with them and it’s just a terrible arrangement.
Then, you should be asking for what their doctor cover is. Do they have a doctor on site 24 hours a day? Because again, we are also finding this often no doctor cover 24 hours a day in LTACs. So definitely ask them for that.
Next question need to ask is, what are their success rates? Ask them if they can talk, if you can talk to a family that had success in there with weaning, ask them that. If they haven’t got any case studies or if they can’t get you to talk to a family that has had success in their facility, you probably already know the answer whether you should send your mom there or not.
RECOMMENDED:
The other issue is, you remember when earlier today we spoke to the doctor, you know, let’s just say your mom goes into LTAC and God forbid becomes end of life. You would also want appropriate palliative care services or hospice services to facilitate that if it came to that point. And again, LTACs often don’t have that. And you can see the dynamics there already that when the patient leaves ICU, they go to LTAC, they bounce back to ICU and often it’s a different ICU.
So your mom could end up in three hospitals/facility within a few weeks. And again, a critically ill patient needs consistency of care and not bounce around between places. So from that perspective, keeping your mom in the hospital at where she’s at the moment, with a tracheostomy, and then try and go home, I believe would be the preferred option.
RECOMMENDED:
So those are the things that I think are important. As I said, the other thing is you should be asking for what are their plans at an LTAC to escalate care and treatment if need be without getting your mom back into ICU. Because again, I’ve seen that sometimes patients obviously do deteriorate and they then go to ICU straightaway. Some LTACs have the capabilities to escalate treatment to avoid ICU, but again, it’s not the same as ICU.
The bottom line is this Rhea, when somebody is on life support, tracheostomy, ventilation, but even tracheostomy without ventilation needs the specialized skills of an intensive care nurse, intensive care doctors. Anything less than that is just simply dangerous and the LTACs will probably promise you the world, but we know from experience it’s not happening.
RECOMMENDED:
So I hope that helps. I will also send you an email shortly with an extension for your consulting for another three days. Look out for the email. As you know, my number again is 415-915-090. Looking forward to talking to you again. Take care.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!