Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Loved ones in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
I Want To Request For My Dad’s Medical Records In ICU But Do I Have A Right As His Daughter?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions that we get quite frequentlyas part of my 1:1 consulting and advocacy service!
What Is an Arterial Blood Gas Test (ABG)?
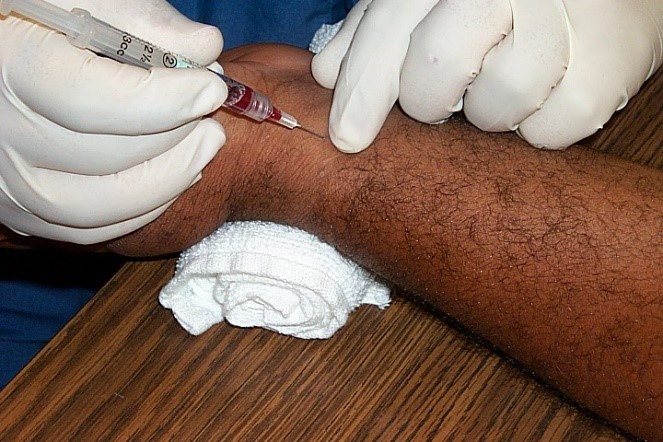
An arterial blood gas (ABG) test measures oxygen and carbon dioxide levels in your blood. It also measures your body’s acid-base (pH) level, which is usually in balance when you’re healthy.
This test gives the doctor clues about how well your loved ones lungs, heart, and kidneys are working.
Every cell in your body needs oxygen to live. When you breathe in (inhale) and breathe out (exhale), your lungs move oxygen into your blood and push carbon dioxide out. That process, called gas exchange, provides the oxygen we (and all of our cells) need to survive.
Your red blood cells transport oxygen and carbon dioxide throughout your body. These are known as blood gases.
As blood passes through your lungs, oxygen flows into the blood while carbon dioxide flows out of the blood into the lungs. The blood gas test can determine how well lungs are able to move oxygen into the blood and remove carbon dioxide from the blood.
Imbalances in the oxygen, carbon dioxide, and pH levels of your blood can indicate the presence of certain medical conditions. These may include:
- uncontrolled diabetes
- hemorrhage
- chemical poisoning
- a drug overdose
Arterial blood gas values may be indicated before and after the start or discontinuation of oxygen administration to the patient, after ventilator changes, and when a change in patient status has been noted.
Why Is an Arterial Blood Gas Test Done?
Arterial blood gas test is done to:
- Check for severe breathing and lung problems such as asthma, cystic fibrosis, or chronic obstructive pulmonary disease (COPD)
- Check how treatments for your loved ones lung problems are working
- Check whether your loved one needs extra oxygen or other help with breathing
- Check your loved ones acid-base balance. They can have too much acid in your body from kidney failure, a severe infection, specific toxic ingestions, complications of diabetes (DKA=Diabetic ketoacidosis), or under-treated sleep apnea.
Arterial blood gas analysis is a common investigation in emergency departments and intensive care units for monitoring patients with acute respiratory failure. It also has some application in general practice, such as assessing the need for domiciliary oxygen therapy in patients with chronic obstructive pulmonary disease.
An arterial blood gas result can help in the assessment of a patient’s gas exchange, ventilatory control and acid–base balance. However, the investigation does not give a diagnosis and should not be used as a screening test. It is imperative that the results are considered in the context of the patient’s symptoms. (8)
While non-invasive monitoring of pulmonary function, such as pulse oximetry, is simple, effective and increasingly widely used, pulse oximetry is no substitute for arterial blood gas analysis. Pulse oximetry is solely a measure of oxygen saturation and gives no indication about blood pH, carbon dioxide or bicarbonate concentrations.
How to Draw an ABG?
An arterial blood sample is collected from an artery, primarily to determine arterial blood gases. Arterial blood sampling should only be performed by health workers for whom the procedure is in the legal scope of practice for their position in their country and who have demonstrated proficiency after formal training.
The sample can be obtained either through a catheter placed in an artery, or by using a needle and syringe to puncture an artery. These syringes are pre-heparinized and handled to minimize air exposure that will alter the blood gas values.
An arterial blood gas requires the nurse to collect a small sample of blood – generally, a full 1 ml is preferred. Blood can be drawn via an arterial stick from the wrist, groin, or above the elbow. (6)
The radial artery on the wrist is most commonly used to obtain the sample. However, the femoral artery and brachial artery can be used if necessary. If your loved one already has a pre-existing arterial line , this can be used to obtain the sample.
Once the blood is obtained, it is either sent to the hospital’s central lab for analysis or tested by the respiratory therapist on the unit’s blood gas analyzer. Most ICUs have one on the unit for a quick turnaround.
While arterial samples are the best for diagnostic reasons, they do provide some challenges for nurses and providers. The main issue is if your loved one does not have a functioning arterial line, a frontline clinician has to draw the arterial sample. Some hospitals allow specially trained nurses or phlebotomists to perform this skill but only after an intense training program. If a provider is not available to perform the arterial stick, treatment could be delayed.
What are the risks and contraindications of a blood gas test?
The ABG test is a standard blood test and a very safe procedure. If performed correctly, there’s very low risk involved, aside from the normal risks associated with any blood draw. Because the test is normally performed on an artery, which is typically located deeper within the body than veins, there may be some slight pain.
If you’re loved one is taking supplemental oxygen therapy, your oxygen levels must stay consistent (without assistance) for at least 20 minutes before giving blood for an ABG test. Precautions are observed if your loved one is currently taking any blood thinners such as heparin, warfarin or aspirin, or even supplements such as fish oil.
Possible side effects associated with the blood gas test include:
- bleeding or bruising at the puncture site
- feeling faint
- blood accumulating under the skin
- infection at the puncture site
What are the complications related to arterial blood sampling?
There are several potential complications related to arterial blood sampling. The points below list some of the complications related to the procedure, and how they can be prevented (7)
- Arteriospasm or involuntary contraction of the artery may be prevented simply by helping your loved one to relax; this can be achieved, for example, by explaining the procedure and positioning them comfortably.
- Haematoma or excessive bleeding can be prevented by inserting the needle without puncturing the far side of the vessel and by applying pressure immediately after blood is drawn. Due to the higher pressure present in arteries, pressure should be applied for a longer time than when sampling from a vein, and should be supervised more closely, to check for cessation of bleeding.
- Nerve damage can be prevented by choosing an appropriate sampling site and avoiding redirection of the needle.
- Fainting or a vasovagal response can be prevented by ensuring that your loved one is supine (lying down on their back) with feet elevated before beginning the blood draw. Those requiring arterial blood sampling are usually inpatients or in the emergency ward, so will generally already be lying in a hospital bed. Children may feel a loss of control and fight more if placed in a supine position; in such cases, it may be preferable to have the child sitting on the parent’s lap, so that the parent can gently restrain the child.
- Other problems can include a drop in blood pressure, complaints of feeling faint, sweating or pallor that may precede a loss of consciousness.
How to interpret results of a blood gas test?
The results of a blood gas test can help your doctor diagnose various diseases or determine how well treatments are working for certain conditions, including lung diseases. It also shows whether or not your loved ones body is compensating for the imbalance.
Due to the potential for compensation in some values that will cause the correction of other values, it’s essential that the person interpreting the result be a trained healthcare provider with experience in blood gas interpretation.
The test measures:
- Arterial blood pH, which indicates the amount of hydrogen ions in blood. A pH of less than 7.0 is called acidic, and a pH greater than 7.0 is called basic, or alkaline. A lower blood pH may indicate that your blood is more acidic and has higher carbon dioxide levels. A higher blood pH may indicate that your blood is more basic and has a higher bicarbonate level.
- Bicarbonate, which is a chemical that helps prevent the pH of blood from becoming too acidic or too basic.
- Partial pressure of oxygen, which is a measure of the pressure of oxygen dissolved in the blood. It determines how well oxygen is able to flow from the lungs into the blood.
- Partial pressure of carbon dioxide, which is a measure of the pressure of carbon dioxide dissolved in the blood. It determines how well carbon dioxide is able to flow out of the body.
- Oxygen saturation, which is a measure of the amount of oxygen being carried by the hemoglobin in the red blood cells.
In general, normal values include:
- arterial blood pH: 7.35 to 7.45
- bicarbonate (HCO3): 22 to 26 milliequivalents per liter
- partial pressure of oxygen (PaO2): 75 to 100 mm Hg
- partial pressure of carbon dioxide (PCO2): 35 to 45 mm Hg
- oxygen saturation (O2 sat): 94 to 100 percent
Abnormal values may be signs of certain medical conditions. An abnormal result basically means that your body is out of acid-base balance. As a result, your body fluids may become too acidic or too alkaline and less able to effectively support normal functioning.
Abnormal results can be signs of certain medical conditions, including the ones in the following table:
| Blood pH | Bicarbonate | Partial pressure of carbon dioxide | Condition | Common causes |
| Less than 7.4 | Low | Low | Metabolic acidosis | Kidney failure, shock, diabetic ketoacidosis |
| Greater than 7.4 | High | High | Metabolic alkalosis | Chronic vomiting, low blood potassium |
| Less than 7.4 | High | High | Respiratory acidosis | Lung diseases, including pneumonia or COPD |
| Greater than 7.4 | Low | Low | Respiratory alkalosis | Breathing too fast, pain or anxiety |
Measuring arterial blood gases can be a useful adjunct to the assessment of patients with either acute or chronic diseases. The results show if the patient is acidaemic or alkalaemic and whether the cause is likely to have a respiratory or metabolic component. The PaCO2 reflects alveolar ventilation and the PaO2 reflects the oxygenation of arterial blood. When combined with your loved ones clinical features, blood gas analysis can facilitate diagnosis and management.
Why is arterial blood gas necessary before and after extubation?
Guidelines have been developed by the major health care professional groups involved in the management of mechanically ventilated patients and provided a framework for weaning from mechanical ventilation and extubation.
Recommendations include the control and elimination of factors that may contribute to ventilator dependence, early assessment after clinical stability for discontinuation of mechanical ventilation, as well as assessment for the potential discontinuation of mechanical ventilation during spontaneous breathing (as opposed to during supported breathing).
The ABG values represent an aggregate of many events, involving cellular metabolism, muscle activity, oxygen consumption and carbon dioxide production, cardiac function, tissue perfusion, ventilation, and perfusion. As an aggregate measure, ABG values represent the patient’s response to the SBT (Spontaneous Breathing Trial) and provide insight to the response to extubation.
Most frequently the clinician uses a spontaneous breathing trial (SBT) to determine your loved ones readiness for liberation from the ventilator. Then the patient is assessed for ability to breathe without an artificial airway (extubation). ICUs measure ABGs during SBTs and use ABG values in conjunction with clinical data to determine if your loved one is fit for extubation or not.
The importance of avoiding an inappropriate extubation based on ABG values should not be underestimated. Failed extubation means reintubation and increased risk of pneumonia, longer ICU stays, hospitalization, and increased mortality.
Your loved one once extubated, needs to still undergo series of blood gas or as necessary to determine if they are able to tolerate removal of the breathing tube and thus breathing on their own.
Arterial Blood Gas and Other Parameters
While arterial blood gas monitoring is particularly required for assessment of pulmonary functions, arterial blood gas in ICU is also a good way to quickly check your loved ones blood level of:
- ELECTROLYTES – Especially potassium, calcium, magnesium and sodium values. This is particularly important in the immediate management of cardiac arrhythmias as it gives an immediate result.
- LACTATE – produced as a by-product of anaerobic respiration. A raised lactate can be caused by any process which causes tissue to use anaerobic respiration. It is a good indicator of poor tissue perfusion and it can be an early sign of an infection or sepsis.
- Haemoglobin (Hb) – acts as a guide but maybe inaccurate in an ABG. Lab samples should be used to verify results.
- Glucose – This should always be checked during ABG or as otherwise ordered by the doctor. Glucose is especially pertinent in the management of the patient who has decreased consciousness or seizures. It is also important in patients with known or suspected diabetes. Glucose may also be raised in patients with severe sepsis or other metabolic stress. Glucose levels are often raised for critically ill patients in ICU even though they are not diabetic. This is often a stress response to the critical illness in ICU.
REFERENCES:
1. Arterial Blood Gas Test (ABG)
https://www.webmd.com/lung/arterial-blood-gas-test
2. Blood Gas Test
https://www.healthline.com/health/blood-gases
3. Arterial Blood Gases
https://www.uofmhealth.org/health-library/hw2343#hw2397
4. What Are Arterial Blood Gases?
https://www.verywellhealth.com/arterial-blood-gases-914885#citation-1
5. Arterial Line Sampling
6. Know Your ABGs – Arterial Blood Gases Explained
https://nurse.org/articles/arterial-blood-gas-test/
7. Arterial blood sampling
https://www.ncbi.nlm.nih.gov/books/NBK138661/
8. The interpretation of arterial blood gases
https://www.nps.org.au/australian-prescriber/articles/the-interpretation-of-arterial-blood-gases
9. Blood gases, weaning and extubation
http://rc.rcjournal.com/content/respcare/48/11/1019.full.pdf
10. ARTERIAL BLOOD GAS (ABG) INTERPRETATION FOR MEDICAL STUDENTS, OSCES AND MRC.
http://www.oxfordmedicaleducation.com/abgs/abg-interpretation/
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!