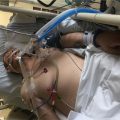
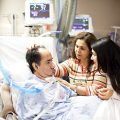
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
My Husband In ICU Is Getting Better From Covid-19 But Why Is He Not Waking Up?
You can check out last week’s question by clicking on the link here.
In this episode of “YOUR QUESTIONS ANSWERED” I want to answer a question from one of my clients Isabel as part of my 1:1 consulting and advocacy service! Isabel’s husband is critically ill in ICU and she is asking for help on how to get a second opinion about her husband’s real condition.
My Husband is Critically Ill In ICU And I Want To Have A Second Opinion About His Real Condition. Help!
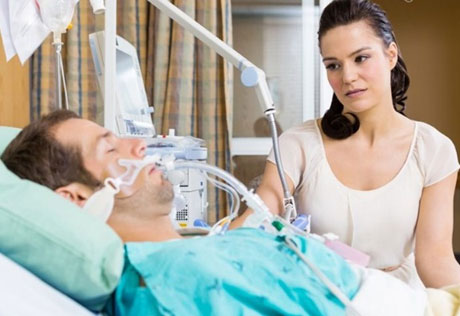
Isabel: Yeah. Was it Dr. Escueta?
Patrik: Exactly. He’s also ICU. There’s almost, I’m not saying there’s conflicting interests, but if you have a neurologist-
Isabel: There kind of is. –
Patrik: I believe there is. I believe you need a neurologist input that’s not attached to ICU. They might tell you the same and that’s fine, but you need almost like an independent neurologist’s opinion.
RECOMMENDED:
Patrik: I believe that the neurologist is not independent because he’s part of ICU.
Eli: But can they push back and say that he’s not healthy enough or it’s not allowed for him to be transferred to another location?
Patrik: Not really. If another location takes him, there’s no limitation. If someone can organize a bed for him in another location. No reason for him not to go.
Eli: Now, are we were putting him in risk to transport him?
Patrik: There always is more risk for transport, but the reality is people are getting transported all the time on ventilators, even on ECMO now. Yeah. You don’t want to risk it unnecessarily, but it’s a very unique situation.
Helga: She had said that, just tonight with the call, she had said something about him not being able to be transported because he’s on dialysis.
Patrik: I don’t buy that for a minute.
Helga: Okay.
Patrik: I don’t buy that because you stop dialysis for a few hours. He can live without dialysis for a few hours. I don’t buy that for a minute.
Eli: I’ll give you an example, here, where I’m close to, where I’m at. They have two hospitals. One specializes in neurology. When they took Dylan, they were going to take him to one hospital, and then the ambulance said, “No, we’re going to this one”, to Doctors versus the one that was close to him. It was because they have a neurology center or-
Helga: Yeah.
Eli: He had a hematoma to the brain and they had to do surgery on him.
Eli: I don’t know if this place can facilitate Noel, or maybe help him because it is with the brain. Maybe there’s some place closer to where he’s at. But, I think that question has to be brought up.
Isabel: Helga had asked something, I don’t know before you’re on Eli, Helga had asked, I think about a transfer. Patrik had said something about like, he didn’t know if that was the right thing to do right now. But, we do agree that he does need that we all agree he should get a 2nd opinion. Helga did ask about that. I think we need to specify, that if they have someone outside of ICU like Patrik brought up.
Helga: Yeah.
Patrik: You definitely want a 2nd opinion. You don’t want to take-
Helga: Because 2nd opinions going to be from the same-
Eli: Hospital.
Helga: Probably the same hospital.
Eli: So, how do we get the referral, or how do we get to request that? So that, they don’t control that.
Helga: I don’t think another doctor could come in from another place.
Patrik: All because of COVID. Because of COVID. Yeah, that could be a real issue. Because normally it’s not a big deal organizing a 2nd opinion. People want a 2nd opinion. No issue. But, that could at the moment, that could be a real issue with COVID.
Recommended articles:
Helga: Yeah.
Isabel: Now, for a 2nd opinion-
Helga: She had brought up-
Isabel: Go ahead Helga.
Helga: She had brought up beds not being beds available too because of the COVID.
Eli: Yeah.
Helga: Like hospitalizations being maxed out. The transports being maxed out. She had highlighted that too. Not that we shouldn’t try, but we might come across those bumps.
Eli: Okay.
Patrik: Yeah. So look, those are real issues at the at the moment with COVID, but that shouldn’t stop you from trying for a 2nd opinion. Shouldn’t stop you. They have to provide something.
Helga: So, should I ask for the 2nd opinion to be outside the hospital or within their hospital?
Patrik: I think you should ask for what you want, which is probably an outsider. Then they will tell you what they can and what they can’t do.
Eli: Okay. Now, what obstacles with that are, and I hate to ask this, but is it going to cost more or is the insurance not going to cover it? Is that like a cosmetic versus something that you have to get versus something that you’re just wanting? You know what I mean? Does that make sense?
Patrik: It does. I couldn’t answer you that question because it probably depends on the health insurance plan.
Eli: Yeah.
Patrik: Couldn’t answer the question.
Eli: But you know what I’m saying, Helga? I don’t want them to say, “Oh, well then you need to come out of pocket for that” or “The insurance is not going to cover that” or “That’s just something that you want to request and that’s not something that the hospital is saying needs to be done.” So, we have to foresee those things coming up.
Helga: She gets to ask yeah.
Eli: Yeah.
Eli: And then is there.
Helga: Okay. Because, I know for sure that when I ask for the 2nd opinion, I know it’s going to be within the hospital. That I could almost guarantee it.
Patrik: Outside of COVID times, it’s not within the hospital. But during, with the situation at the moment, that can be a real obstacle.
Helga: Right.
Patrik: But outside of COVID times, you’ll get a 2nd opinion from an outsider. No problem.
RECOMMENDATION:
Eli: Okay. And then I had a last question and that is, is there any type of technology that we’re not using? Like, let’s say there was a something they could attach to the brain and do tests or reactivate or something. I might be thinking kind of out of the box here, but?
Helga: No, that’s a good question. Dani asked the doctor for shock therapy. But, the shock therapy only works for depressed state patients or. She had mentioned something else, like the shock therapy wouldn’t work for him because, it was only like for people that are depressed.
Helga: Can you elaborate on that, Patrik? What shock therapy is good for?
Patrik: I cannot remember. I’ll tell you what I cannot elaborate on. I don’t know enough about the shock therapy, to be honest with you.
Patrik: I’ll tell you what I can elaborate on. So, you take the major organs, heart, lung, kidneys, liver, and brain. Okay? Heart, lung, kidneys, liver, and brain. The worst case scenario, you could always do a transplant of an organ. Okay? You can do that, if a compatible organ from another donor is available. With the brain, you can’t donate a brain yet. Right? So, if the brain is without oxygen for more than three minutes, it causes irreversible brain damage.
Patrik: As far as I’m aware, there is no cure for a brain that has had more than three minutes without oxygen. Basically, has been starved of oxygen. Now, that’s not to say that people haven’t improved, but it usually happens over time and it’s not a quick or gradual process. It takes time. Takes rehabilitation.
Patrik: As far as I’m aware, there’s little technology that can work on the brain that has been starved from oxygen.
Eli: Okay.
Patrik: So, that is within my knowledge. You could ask and I think the neurologists are really the people that have more insight there in terms of, “Okay, what’s the best approach for rehabilitation, for what someone that has had a massive hypoxic brain injury like Noel had in this situation.” So, the neurologists are really the ones that should have the insights on that.
Helga: So, is it not called anoxic anymore. It’s now hypoxic because of the damage? I have to look up those terms. I don’t know what that means.
Patrik: No, the terms are interchangeable as far as I’m aware.
Helga: Okay. Got it.
Eli: So, that’s our next step then. We have to try to get a 2nd opinion from a neurologist.
Helga: And the reports.
Patrik: That and, I do believe once you’ve had a look at the report, I do believe depending on them to what conclusion you as a family have come, you then should think about, do you want to push for a tracheostomy or not?
Patrik: But those are the next steps after you’ve had access to the report and the 2nd opinion.
Eli: Now let’s say, then all of this happens and he comes home and he starts his rehabilitation or how you say it.
Helga: Yeah.
Eli: And now does he want to live like that? Does he want to live in a state where he’s, I foresee him being maybe in a wheelchair or just doesn’t talk or where you have to take care of him 24/7. I’m not saying that’s a bad thing. Maybe that is what we want to do. And that’s what he wants. But now we have to think, does he want to be like that for the rest of his life? I don’t know if that’s how it’s going to be.
Eli: And I’m sorry for asking those questions but I’m talking because I know that in my case here with Ryla, her son is nonverbal, he’s autistic and she takes care of him and he needs to be taken care of 24/7 and she wouldn’t have it any other way. And I know Helga, you wouldn’t have it any other way either. You want him there, you want him to be there and his kids want him there. We all want him to be there now, but are we being selfish and thinking, Oh, well we want him here because we love him or we want him alive. And you’ve already had the conversation with him and how does he want to live?
Helga: I know my husband would not want to be in a wheelchair. If he couldn’t dance, if he couldn’t sing anymore, he wouldn’t want to be here. He wouldn’t, We’ve had those conversations. He would not want to be dependent on a machine or even an oxygen tank. He just wouldn’t, that’s not your brother. I mean, that’s not a lot of people, but yeah.
Eli: So are we setting ourselves up for that? Do you think? Is it Randy? I’m sorry. No, that’s okay.
Patrik: No, that’s okay. And that’s what I’m saying. That’s exactly the questions I believe you need to ask yourself as a family. What does it look like going forward? You could probably prolong his life for a long time. The question is about quality of life and what is acceptable for you, for him? They have Eli. These are the questions that need to be asked. You can prolong his life probably for a very long time to come artificially, but that’s on a ventilator. Whether it’s with the tracheostomy, it’s all doable. It comes down to perceived quality of life. What is acceptable for you and for him?
Related articles:
Eli: Okay.
Helga: Yeah. That’s a good point because we could preserve his quality of life. It would be on a vent, on a breathing tube and him never responding to us. Is that what we want?
Eli: I’m going to tell you right now and it’s probably sad, but I would want him to be with us regardless if he was on a breathing tube and he needed to be taken care of 24/7. I would be there for him, but that’s selfish for me to say that because that’s for me, I love him. I don’t want him to pass. That’s a hard decision. I can’t make that decision. I can’t say that’s not fair to him, if he can’t speak up for himself.
Patrik: May I ask you a question? Are you a religious family?
Eli: Yes.
Helga: Yes. We are. We’re very religious and not religious. I want to say more like we have a close relationship with God. We’ve always had our whole lives.
Patrik: So do you then believe in God gives life, God takes life? Is that your sort of view?
Helga: Yes, for me, it is.
Eli: For me as well. God has control. God is in control. And I believe that if his will is for Noel to live and be back then that will happen.
Patrik: And Noel would feel the same?
Eli: I’m sorry.
Patrik: Noel would feel the same if he was part of this discussion.
Eli: That God is in control? Yes.
Helga: Yeah. Actually a week after COVID shutdown, March 17th. He actually went on Facebook Live, Patrik and he prayed for everybody. He prayed for his family to be protected against COVID. He, being diabetic was made sure to stay home and didn’t want to chance or risk. And I remember in that prayer, him saying we’re praying for this, but you know, God’s in control. And I keep thinking about what he said, because he said that it’s not over until the fat lady sings. And I keep thinking about that right now with what is going on. Little things improving and just wondering maybe we all feel, we don’t understand why this is happening. We don’t feel that we can question God, even though we want to say “God why?” We know that there’s things that we just don’t understand that are part of just being in this world. And so we don’t want him to suffer. We want him to be with us. We want him to be healed, but we also know that that may not happen.
Patrik: Okay. Can I ask another question? So, and again, that’s probably sharing some insights that I believe are important for you as a family. You might’ve heard the doctor saying at 1:30, when we spoke to her, sort of again, her hinting towards end of life. That was even before she talked about DNR, Do Not Resuscitate, they were talking about making him comfortable and let him die. That’s what pretty much she was alluding to as an option. So here is where I, as a professional, have a problem with that. And I always had a problem with that, right? That is always an option in ICU. You can make quote unquote people comfortable and let them die. In my mind, that is through euthanasia. And that is one of the reasons why I opted out of ICU eventually, because euthanasia is happening in ICU all the time. And I don’t feel comfortable with it. Right. But it happens all the time.
Helga: What is that?
Patrik: Euthanasia is hastening of death. Medically. They give patients morphine and midazolam and they basically sedate them and they put them asleep.
Isabel: Versus letting them die on their own?
Patrik: Yeah, exactly. It’s hastening death.
Helga: It’s like when someone’s so ill, you’re basically killing them before they like their body hasn’t closed, shut down on its own.
Patrik: Correct.
Isabel: No, go ahead, Patrik. I appreciate where you’re going with this. Please go.
Patrik: It hastens death and at the end of the day it kills them. Yes. And some people in some countries there’s voluntary euthanasia for end stage cancer patients. And I have no problem with that. If that’s what people want, where I do have a problem with is hospitals, ICU in particular, rushing people to death and making it seem like that’s the only option. That’s what I have a problem with. But again, other families might have a different point of view and that’s fine too. That’s just my point of view. And I had a big problem with that in ICU. I don’t agree with it.
RECOMMENDATION:
Isabel: And I can see where that, with faith would be kind of, we’re playing God by saying, go ahead and take his life. Versus if he were to pass, like if his body stopped on its own and that happened then, okay, that happened. That’s different. But if we’re to say yes, go ahead and let him go. Don’t support him. His body isn’t shutting down. It’s just them removing the support. We are euthanizing him. Like they do to animals, putting them to sleep.
RECOMMENDED:
Patrik: But the problem is nobody’s using the word euthanasia in ICU. If anything, if you were to say to them, you’re euthanizing a patient, they would go up in arms because in most countries, euthanasia is illegal, including in the U.S.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!