Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
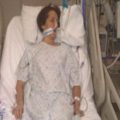
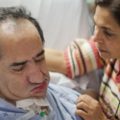
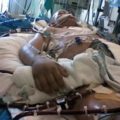
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tess, as part of my 1:1 consulting and advocacy. Tess’s daughter is critically ill in the ICU and she is asking if they are limiting treatment for her daughter to end her life.
My Daughter is Critically Ill in the ICU and Are they Limiting Treatment for Her to End Her Life? Help!
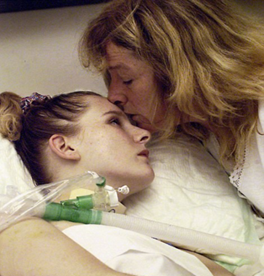
“You can also check out previous 1:1 consulting and advocacy sessions with me and Tess/Romeo here.”
Rey: Hello Patrik. The point about… Can you hear me all right?
Patrik: Yes. Who is this speaking? Who is this speaking?
Rey: Rey is speaking.
Patrik: Okay. And you are… And what’s your relation?
Rey: I’m the partner.
Patrik: Okay, okay. Okay, sorry. Yeah, okay.
Rey: Hi. Yeah. I just wanted to say just one thing was that we have thought about the food being discontinued because of the risk of having an aspiration, which is the part they’re taking care of. And this goes for other treatments as well, and other medications that they could be giving, their opinion is that, any treatment that they give, that they know, quote, unquote, know wouldn’t be effective, would be not only futile, but it would be potentially assault. But you know, I disagree on that. And I need to try to stop them from doing that.
Patrik: Look, I get all of that. My advice in this situation is, if you don’t try, you know what’s going to happen if you don’t try, right?
Rey: Exactly. You know what’s going to happen if you don’t try. I know, I know. I completely disagree with the idea that they know what’s going to work and what’s not.
Patrik: But on the other hand, if they feel so confident that this is what they’re going to do next, in essence, euthanize her, right, if you think you can’t stop that with your current resources, I do believe that you need to seek legal advice as a matter of urgency. Right?
RECOMMENDED:
Rey: Yes.
Patrik: Because you can argue with all the hospital policies and you can argue what we just talked about, but if they’re going to proceed with that, you will need to seek legal advice.
Rey: Exactly. I mean, Tess and Romeo will tell you more about this, but they’re already been seeking legal advice and the way it works in this country is that even if it’s a matter of great urgency, if it’s going to counsel to the high court, it has to be put on a waiting list and you obviously have to write a witness statement. Well, anyway, so there’s a lot of obstacles-
Patrik: Barriers.
Rey: … in this. Yes. And that’s just a point I wanted to raise because the thing is Patrik, is that, and I’m sure you probably guessed, it’s the director of the whole rehabilitation unit. He’s extremely well-versed with the law, and extremely well-versed because I actually watched a lecture with him speaking about the national guidelines for rehabilitation patients. The majority of the PowerPoint, the hour-long lecture was just talking about palliative care, and talking about the realities and all of that. So, he clearly knows what he’s talking about in that area of law.
Patrik: How can you be so sure he knows what he’s talking about? Because he’s a doctor? He might just be talking good game, I don’t know. You might as well be right. But I don’t know. As I said-
Rey: Well, maybe he’s neglecting to include loopholes, or maybe he’s neglecting to include certain information from the power point that could be of benefit to a patient and their family, yeah. That’s a good point.
Patrik: Right. All I believe at the moment you can do is you need to seek legal advice as a matter of urgency because in this situation, you know I’ve sent you information, I’ve sent Tess information about the policies and if they are breaching those policies, which I believe they are, I believe you need to seek advice from a lawyer as a matter of urgency. I can advise you clinically. I don’t know whether you’ve heard that earlier. I believe another option, if they’re wanting to starve her, another option that they could do is they could give her TPN (Total Parenteral Nutrition). Have you heard of that?
Rey: What is that, sorry? TPN.
Patrik: TPN is basically intravenous nutrition.
Rey: Oh. Oh, right. And that would be something that they would perhaps do in the intensive care unit, is that correct?
Patrik: Well, I mean, it’s an alternative to nasogastric tube feeds or PEG (Percutaneous Endoscopic Gastrostomy) feeds. It’s definitely an alternative. And obviously the only thing they’re telling you is that they want to kill her, then they’re not giving you any options, so I can advise you clinically, but if they want to proceed anyway, by basically, killing her, I do believe you should be writing an email to hospital administration as a matter of urgency and you should be, as I said, you should be seeking legal advice as a matter of urgency.
Rey: Yes. Okay. I’ll pass you back to Tess, okay.
Patrik: Thank you.
Rey: All right. Thank you, Patrik.
Patrik: Thank you.
Tess: And also the whole thing of this TPN, obviously is working well and that may be a way to get around it, because if they’re going to make that as an excuse, and they’ve not given all the possible options including the nasogastric tube, yes. Is that right, Patrik?
Tess: Okay. I get your point about TPN.
Patrik: Yes.
Suggested Links:
Tess: So the doctors is going to come round. Now if they put her back into ICU, then they can basically, effectively knock her off in that environment, and so, “Well, we told you so,” kind of attitude. I’ve seen the scans extensively. I don’t know, anybody can type in a name, but I’ve seen scans of parts of her brain that were taken on. So I’ve seen that there’s damage extensively starting deep on Sarah’s brain, but I know enough brain damage to know that it can’t be as quick acting as it appears on the X-ray films because it can take days because there’s the shrinkage of the brain in itself, and then there is a kind of walnut aspect with dark areas where the seizure happened and then that… you know.
Tess: ..and that was back then, but I can’t see how that could just be the cause of immediate effect. And also, the CT scan, I see it being shown something, but I’m shown something on the screen that was going up in incremental levels through, supposedly, Sarah brain. It might be, it might not, I don’t know. I’m just being shown. And I’m not a radiologist. I can’t necessarily read these things and know with absolute certainty that what I’m looking at is actually, is true.
Patrik: Yeah, totally understandable. And that’s why I think one of your next steps is if you’re writing or contacting the hospital administration.
Tess: Repeat that, please Patrik.
Patrik: Yeah. If you are contacting, I think you need to contact hospital administration as a matter of urgency and I do believe part of your communication with hospital administration is you still haven’t got access to medical records, right. That is a right, not a privilege. That is your right.
Tess: Yes.
Patrik: And you want her to be back on full treatment until you have access to the full medical records. What do they have to hide? That needs to be part of your communication with hospital admin and with the hospital there.
Tess: With the clonazepam, is it something that can actually be introduced intravenously or not?
Patrik: Say that again.
Tess: With the clonazepam-
Patrik: Yep.
Tess: … they’re making it out like they’ve stopped because it might be aspirated.
Patrik: Right.
Tess: So is that something that, from your knowledge, do you know whether that can actually be intravenously introduced or not because it’s making Sarah really drowsy.
Patrik: Oh, it does. It does have a sedative effect, big time.
Tess: And would that actually slow her breathing rate and make it more difficult for her to actually get through this whole procedure, calculated risk?
Patrik: Look. The clonazepam will make her more sleepy and more drowsy, which puts her at higher aspiration risk. I do believe if they’re trying to kill her, they would give her clonazepam or a similar medication to make her to go to sleep, so to speak.
Tess: Well, I don’t want this, okay.
Patrik: Of course, of course.
Tess: … happening.
Patrik: I get that. And that’s why I believe you need to speak to hospital administration. You need to escalate this as quickly as possible.
Tess: Do you think it might be a good idea to actually go straight to the director? He’s the person who’s supposedly a neurological grievances expert.
Patrik: Say that again, say that again please, Tess.
Tess: The director of this unit. He’s the one that everybody answers to. Do we do a three-way call with him? I’ve got his mobile number.
Patrik: I’m happy to get on a three-way call with him. However, if you feel like he is the driver behind all of this, what’s the point, because you need to escalate this to another level.
Tess: Okay. Okay.
Patrik: That would be my advice because you’re just beating a dead horse by talking to him.
Tess: Beating a dead horse by talking to him. He’s obviously behind all of this and he’ll be instrumental in trying to do what’s going on now and being an expert in palliative care, he’s got his ducks, his I’s dotted and T’s crossed, yeah.
Patrik: He’s an expert in euthanasia.
Tess: He’s an expert in euthanasia.
Recommended:
Patrik: You don’t need that.
Tess: No, we don’t need that.
Patrik: I believe that given the gravity of the situation, you need to escalate this as quickly as possible to hospital administration. I do also believe that you need to-
Tess: I think I should call. Shouldn’t I call?
Patrik: Yes, you should. However, I also believe you need to put it in writing because otherwise they might say, “Ah, we’ve never spoken to this person.” If you put this in writing… You probably need to do both.
Tess: Okay.
Patrik: You probably need to do both. I would also advise you to speak to a solicitor, to a lawyer that is versed in this area. Again, I’m a clinician, I’m not a lawyer, but I do believe in order to potentially take this further, if the hospital is not responsive, you unfortunately, I believe your next step is you need to take them to court. You need to seek an injunction in the court.
Tess: We need to seek an injunction in court, apparently. Look, and it seems that we have got enough time for that. Do you have a means now Patrik, to find out what the admin number as the head of the admin at the hospital, I’ll spell it to you, on the computer, please? Because we don’t have access to one.
Patrik: You don’t have access to what?
Tess: We can do it on the phone, I suppose, yeah. Okay, we can do it. I was going to ask if you could do it on the phone. Because then we could do a three-way call with Robert here and now. Get that call digested and then get the email down as a second attempt.
Patrik: Absolutely. And as I said to you-
Tess: And you can record it your end. I think that’s more important. Let’s do it that way.
Patrik: Right. I would strongly recommend you to put something in writing as well. I’m happy to-
Tess: Oh yes, indeed. I appreciate you, but I want you to be strong with me Patrik, on this one. Because if you’re not, Sarah could lose her life.
Patrik: Yeah, no, I agree. I agree.
Patrik: You need to take action as quickly as possible, there’s no question about that. What would you want to do as a next step?
Tess: Do next is speak to the admin person at the head of this hospital.
Patrik: You need to speak to the hospital CEO, that’s what you need to do. My recommendation is to go to the office now, given that you are in the hospital. My recommendation is to go there in person.
Tess: Right, okay. Okay, yeah. I’m going to go there with Rey. You’re staying here, Romeo. Rey and I are going to the admin office now and we’re going to have a word with them now. Then we’re going to, without their knowledge here, in this place, yeah, any conversations that are going ahead, you, me, you don’t have any further discussions with them until our return, okay. And we’re going to be away for about, I don’t know, I suspect probably half an hour, thereabouts. Yeah? Is that good, Patrik?
Patrik: Yeah.
RECOMMENDED:
Tess: And I can call you to indicate progress, all right?
Patrik: Yep.
Tess: Okay, Patrik. So, you’re saying to the senior officer of the admin, yeah?
Patrik: No, you need to speak to either the hospital CEO or the hospital general manager, either/or.
Tess: Hospital general manager. Okay. Hospital manager or the CEO. All right. Okay.
Patrik: Thank you.
Tess: We’re going literally, now. All right, Patrik?
Patrik: Thank you.
Tess: Okay. Thank you, Patrik.
Patrik: Thank you. Bye. Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!