Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
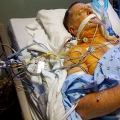
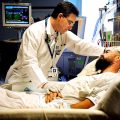
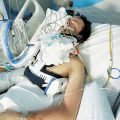
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tess, as part of my 1:1 consulting and advocacy. Tess’s daughter is with a tracheostomy in the ICU. Tess is asking how can her daughter prevent aspiration pneumonia in the ICU.
My Daughter is Ventilated and with a Tracheostomy in the ICU. How Can She Prevent Aspiration Pneumonia?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Tess/Romeo here.”
Tess: Hi, Patrik.
Patrik: Hi, Tess. How’s your daughter?
Tess: Been able to see her four weeks prior, because of the lockdown, okay?
Tess: Her hands have done contractions in that time, and using splints, and they have contracted, but that’s by the by. They changed her tracheostomy tube just prior to her movement on Saturday. We were told that she was going to be moved to the rehabilitation unit there. She was granted that at short notice because a bed became free, and that was very unexpected.
RECOMMENDED:
Tess: They changed her tracheostomy tube, they did a new catheter, and we were told yesterday out of the blue she was all right. She was on the ward there with three others. The tracheostomy, she aspirated, she must’ve aspirated because her saturation had gone down to 70. They did a bag and mask, to keep inflation going on the ward. Romeo went into in-depth conversation with a consultant, extremely experienced knowledge, and he was informing me and Romeo of the situation and was saying, that she was going to be taken to ICU because she was with difficulty. They suspected that she’d aspirated and it caused an exacerbation of the pneumonia.
Tess: She’s stable now. They made a mistake with that tracheostomy but of course, they don’t want to admit it. And they’re now wanting to change to a subglottic trach plan or if not Tuesday, which is a long way away. It’s closed off and she’s on the antibiotics, which they’ve previously given her when she was in ICU.
Tess: She’s on clonazepam, I took down all the notes this morning, because I actually rang through to the ICU just out of the blue, because she said, “Look, ring Patrik, get through to him.” That was her instinct. Yeah, because they basically said a lot, down to escalate, everything other than antibiotics.
Tess: She’s stable as a consequence of that then all is well, but they would’ve pushed for mask because she’s still got a DNR (Do Not Resuscitate). I’m going to pass it to you. Okay. Only this morning … yeah, excuse me. I will go through it eventually. I’ve spoke to the doctor on the ICU who’s there purposely, and he’s allowed me to ask all those questions that you’ve advised us to ask to assess the situation and I will run through it.
Tess: Okay, so, no sedatives, her eyes are reactive, they’re fine. She had a little bit of a … she was fine on her heart rate, she had a regular heart rate, and then she was woken up, and she’s a tad little bit agitated it had gone to 89, so basically all right. Just a little bit up.
Tess: To make she’s on the clinic she’s on clonazepam, she’s on 2 mg three times a day. And I asked-
Patrik: She’s on what?
Tess: Clonazepam.
Patrik: I got that, but the next one I didn’t get.
Tess: I can’t hear you very well, Patrik.
Patrik: I said, I got the clonazepam, but I didn’t get the other one.
Tess: That’s it. It’s 2 mg three times a day.
Patrik: Oh, 2 milligrams. 2 milligrams.
Tess: Yes.
Patrik: Okay.
Tess: Any anti-hypertension drugs? No. Does she present a temperature? No.
Tess: I asked about, they’ve given her a chest X-ray, and she’s got consolidation, a small consolidation on the left lobe of her lung, the left lung previously, which I don’t think it will be resolved, which is strange because it hasn’t. And the aspiration-
Patrik: Could be new from the aspiration. Could be.
Tess: Well, it’s appeared in the right lung.
Patrik: Okay, fair enough.
Tess: The lower right lung a little bit, from the X-rays. That’s what we’ve ascertained, but it’s not a lot. There’s no fluid. But she’s had … all the time that she was on the respiratory ward, she had really thick secretions, and then they gave her an injection, because she had a patch stuck up behind her ear, and they were giving her an injection to try and actually ease the production of the secretion in his tracheostomy.
Tess: And also as far as I’m aware, when I was last with her, she was attentive to what I was saying for over nearly an hour and a half, and the time passes, it goes really quickly, but I was at close quarters with her, and I knew that she was listening very attentively, because I know Sarah very well, I’ve been observing her all the way along, and she also tracked on the nurse as well, when he was doing some functioning on the other side, so I knew.
Suggested Links:
Tess: So I went around to her left side, because I was on her right side. Went round to her left side, because I noticed that she couldn’t … when I asked her to pay me attention on the left side of her body, there was a difficulty with looking round to the left. So I suspect that she could have a blind spot. That’s just my suspicion.
Tess: But Sarah is stable in her blood sugars. She’s on full percent oxygen, I mean you’ve got 100 on the calculation, because they got her from a 70 up to 100 which is great. Stable at the moment. The myoclonic seizures were pretty bad yesterday, but as the consultant said, it was no doubt due to the fact that she was in an agitated state.
Tess: Now the curious thing is that when I was at the other end, we were prevented from seeing her for four and a half weeks. So when I did get to see her, you know the little monitor that goes on the end of the finger?
Patrik: Yeah.
Tess: Yeah, for the saturation machinery, that thing in her hand keeps on displacing, and then affecting the machine. So obviously I’m hard onto that, getting the nurse, who was literally sitting outside the ward at a short distance, to come to her but they at the time had the door closed, because the nurse seen her that Sarah’s right and stable. Get it? So I would open the door and I would say, “Excuse me, the machine is not working.” Da da da …” so could there have been a danger of being desaturated as a consequence, I’m asking myself, of the fact that this little device was dislodged from her finger.
Tess: And then they went through this whole process of trying to get her up to the ICU to make sure that she was all right. I don’t know. I know she aspirated.
Patrik: But didn’t she aspirate when they changed the tracheostomy?
Tess: Romeo said something, excuse me, Patrik.
Tess: Okay. Yes, okay. Would you please help me in this way? Could we do a three-way call to the … is that possible-
Patrik: It is possible but I need-
Tess: Yeah?
Patrik: I need to ask a few questions first.
Tess: Yes.
Patrik: So when did we last speak? A couple of months ago?
Tess: Indeed yes, and four days remaining as I remember, three and a half days remaining of conversation of the meeting, yeah?
Patrik: Right, so just let me … hang on, just give me one second. So a couple of months.
Tess: Yeah, it’s been a long while because she’s been trying to get better all that while, and then there’s relatively no change. She was all right, waiting on rehabilitation.
Patrik: So when we last spoke I do remember she was sort of just on the verge of leaving ICU, is that correct?
Tess: She did leave ICU, Patrik.
Patrik: No, no, I get that. What I’m trying to find out is when we last spoke, was she on the verge of leaving ICU then?
Tess: Yes, I believe so, but I’d have to look back in the notes, yeah.
Patrik: And since when has she’s been off the ventilator?
Tess: She’s been off the ventilator for a long while.
Recommended:
Patrik: Okay, what does a long while mean?
Tess: She’s been breathing ambient air for a long while. Weeks.
Patrik: Okay, weeks, okay, great. What was her last Glasgow Coma scale through all this? Do you know?
Tess: I don’t actually. Hopefully you can ask that, because she can’t speak, no doubt because of the tracheostomy tube. I noticed that she’s tracking with her eyes. She’s still very, very still, and she’s not breathing heavily as I recall. She’s memory conscious, we’ve got the opportunity to wake her, and that’s what’s most important. They wouldn’t have taken her on, and they’ve thought that they can get her, with their expertise to actually be at some stage functional.
Tess: So they’ve got this DNR on her, Romeo’s asked for it to be taken off, I don’t want it on there. But they are saying that she could deteriorate from this pneumonia, they’re not going to bother any longer.
Patrik: Right, okay. This is new, is it?
Tess: Yes, it is. This is all new because of their failing to get the tracheostomy tube correctly done so it’s inaccurate.
Patrik: And when did they do the tracheostomy change? What day was that?
Tess: It was on … what day is it now? I would see Sarah on Thursday, because it all comes a bit of a haze because of stress. Thursday, I was with him on Thursday. She got moved Wednesday.
Patrik: Do you know if they stopped the feeds before they did the tracheostomy change?
Tess: Can you repeat that please, Patrik?
Patrik: Yeah, sorry. The first thing that comes to mind for an aspiration pneumonia with the tracheostomy is that they had not stopped the PEG (Percutaneous Endoscopic Gastrostomy) feeds, and because she had a full stomach, and if she had a full stomach when they did the change, that could have lead to the aspiration.
Tess: No, she’s still got a tube in her face.
Patrik: Yeah, so what needs to happen, before a tracheostomy change, people need to be fasting for a few hours. If you do a tracheostomy change, if the feeds are running, that’s a massive aspiration risk. So my question is-
Patrik: Sorry. My question is did they stop the PEG feeds hours before they did the-
Tess: That question hasn’t been asked because the persons are refusing to find out whether they did it right or wrong.
Patrik: Very important question.
Tess: But I didn’t know that.
Patrik: Very important question, because that’s the first thing that comes to mind.
Tess: Okay, did they stop at least two hours before they did the trachea change, and we’ve got also got to bear in mind that they need to know to be absolutely certain not to do the same mistake again when they do the tracheostomy tube change, because they’re going to get this subglottic suction poor, yeah?
Patrik: Right, that’s-
Tess: In a new change. Why did they change at that hospital just prior to going to it? People are more expert, I don’t know.
Patrik: That would be my next question, Tess, how often did they change it beforehand, or was that the first time they changed it?
Tess: First time in all of the whole experience?
Patrik: Was it?
Tess: Well, it hadn’t been changed as far as I … it gets adjusted and checked doesn’t it? She went from an 8 to a 7.5, so would that be doing a change?
Patrik: Right. The reason I’m asking … so a tracheostomy should be changed once a month, of this age it should be changed every three months. There are different schools of thought, but does she have an inner tube, inner cannula?
Tess: Inner cannula, I’m not sure.
Patrik: Right, okay. Is she getting mobilized? Or was she getting mobilized?
Tess: They just said, because we had an opportunity to take her tablet which has been giving all the feels of entertainment, and we had the opportunity to go and meet outside the ward, because there’s somebody with COVID apparently who’s tested positive in the ward up there, and we’ve been prevented from seeing her anyway for three weeks. So we had arranged to go up today, and now we can’t go. It’s not advisable because the expert, the consultant that I’ve just spoken to said that it’s too much stimulation and it’s inadvisable for her and not the right timing, and she needs rest.
Patrik: What’s your feeling around that?
Tess: Well, I don’t … try and caution it. I personally would like to go up there, actually get a chance to actually see her to give her a morale boost, and yeah I think that is important, but this person is taking a stance that no, that would be too much stimulation.
Suggested Links:
Patrik: Right, have you seen her-
Tess: Because her myoclonics were bad yesterday, and they’re not so bad now.
Patrik: Have you seen any-
Tess: But she doesn’t have them at all when she’s sleeping, Patrik.
RECOMMENDED:
Patrik: Have you seen her be mobilized at all?
Tess: She was mobilized into a chair, and they thought she could only bear for 15 minutes, but apparently, the timescale change, varies from person to person I spoke to, from the nurse to another nurse, but basically, about an hour she was able to sit upright, was recently, within the past week they did that.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!