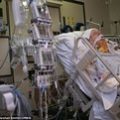
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Is it Safe for my Daughter to Undergo Tracheostomy Even with a Low Hemoglobin level in the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tess, as part of my 1:1 consulting and advocacy service! Tess’s daughter is a long-term ventilated patient in the ICU. Tess is asking why it is relevant for her daughter to be mobilized in the ICU.
Why is it Relevant for My Long-Term Ventilated Daughter to Be Mobilized in the ICU?
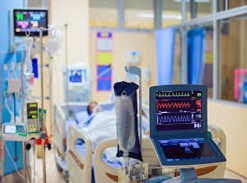
“You can also check out previous 1:1 consulting and advocacy sessions with me and Tess here.”
Tess: They’re actually basically got it in hand and they are doing the right thing. You suspect.
Patrik: That’s what I’m saying. That’s what I’m saying. Yeah. I do believe they’re doing the right things. The only concern is obviously the-
Tess: Hemoglobin
Patrik: … Hemoglobin, but also the DNR (Do Not Resuscitate) is a concern. But other than that, I do believe they are doing the right things. And with that in mind-
Tess: Okay.
Patrik: So with all of that said, so imagine, I believe she’s fairly close to having time off the ventilator. So if she’s having physical therapy well, that I believe will only help moving her towards weaning off the ventilator.
Tess: Exactly. They go hand in hand.
RECOMMENDED:
Patrik: Goes hand in hand, goes hand in hand.
Tess: Yeah. And will it help with the edema as well? Potentially.
Patrik: Where is her edema again?
Tess: Oh, it’s been popping up. It was popping up in her hands and in her feet.
Patrik: Yeah. Definitely. Yeah definitely. Part of having edema is not moving.
Tess: Yeah.
Rey: Yeah.
Tess: Okay. Makes sense.
Patrik: Right. So my biggest concern with everything that you’ve shared, my biggest concern is the cough or the lack of such. The low hemoglobin is of concern. But I think everything else is moving in the right direction. With her having the tracheostomy, I think everything else is moving in the right direction. I believe they’re doing whatever they can.
Tess: Okay.
Patrik: And that’s what I’m saying. Yes. Watch what they say. But more importantly, watch what they do.
Tess: And in terms of given that I can’t even see her at the moment, I can’t watch much Patrik though.
Patrik: Okay, sure. No, no, I get that. I get that. But look, I can’t tell you how many people are in a situation like that and the ICU is denying a tracheostomy and that’s often where we come in we then need to unravel the whole professional advocacy about tracheostomy.
Tess: Okay. So we are the lucky side. Yeah. Okay.
Patrik: Well, I wouldn’t say you’re on the lucky side. I would say they do it rightfully. That should be a given.
Tess: Exactly.
Patrik: That should be a given. I wouldn’t consider that lucky. I just think that is their duty.
Tess: Okay. Okay. I appreciate your sentiment. Totally I do understand exactly what you’re saying. Anything else? Do you have anything else that occurs to you, Patrik?
Patrik: Not that I can think of. What I will tell you is this, and I know that she asked me this yesterday, how long does it take for him to wake up? I do not have the answer to that. I really don’t. It could be days, it could be weeks, it could be months, it could be never. I don’t have a crystal ball.
Tess: Yeah.
Patrik: What a tracheostomy will give her though, a tracheostomy will give her the time to wake up. That’s what a tracheostomy does.
Tess: Exactly. Now with your knowledge of the palliative care, what does palliative care mean anyway?
Patrik: Well, palliative care is a euphemism. It’s a euphemism for end-of-life care.
Tess: Oh dear. So why would a palliative team be involved? They basically think she’s going to die?
Patrik: No, not necessarily, but they, again, this is where the doctors want to keep their options open.
Tess: Right.
Suggested Links:
- MY MOM’S IN ICU WITH GASTRIC PERFORATION&SHE’S NOT WAKING UP! WILL SHE NEED A TRACHEOSTOMY? (PART 1)
Patrik: If she’s not progressing as quickly as they would like, they will bring in palliative care. But I wouldn’t worry too much about it. It’s them keeping their options open.
Tess: Right. Okay. And also I’d really like to be able to hopefully get her into some form of neurorehabilitation after this process. And I know you say take each day as it comes, but is there any sense in trying to be anticipatory of that and sort of preemptive and proactive in terms of researching and how-
Patrik: I’ll tell you what it comes down to. If Sara can be off the ventilator and have the tracheostomy removed. I do believe that neuro-rehab is a possibility.
Tess: Okay.
Patrik: If she stays on the ventilator and she stays with the tracheostomy, it’ll be way more difficult to get her into neuro-rehab.
Tess: Right. Okay.
Patrik: Because managing a tracheostomy is a very specialized skill.
Tess: What, the tracheostomy and also the ventilator you’re saying is tougher?
Patrik: Very, very specialized skill that you rarely find outside of ICU.
Tess: Oh, okay. Understood, okay. So it’s all obviously up in the air until after that.
Patrik: That’s why I’m saying, and I know it’s not what people want to hear, but it’s really one day at a time.
Tess: Yeah.
Patrik: It’s one day at a time and you should also expect like a two step forward, one step back. There will be some setbacks. There will be two steps forward, one step back.
Tess: Okay. Now with the tracheostomy, is it the case that if there isn’t esophageal, shall I point this out that there could be an essentially an esophageal weakness potentially which led to particulates going into her lungs?
Patrik: I think you can. I think you can, whatever you think-
Tess: Would that discourage them from going ahead and doing it?
Patrik: No, I don’t think so. I don’t think so. I would hope that they would consider all of that.
Tess: Okay. Well, given that they alerted me to the fact it should be on the note, shouldn’t it?
Patrik: It should. It should.
Tess: Yeah. Okay. I’m not quite sure at this point, if there’s really anything else that I have to ask you.
Patrik: I don’t think there is at the moment as far as I can see. I think we’ve identified what’s happening, we’ve identified the risks, the benefits, I think it’s going to be a waiting game, I believe.
Tess: Yes. And also with these questions that you kindly sent, do I just print out a new lot and try to ascertain the same details and see if there’s any progression?
Patrik: I would.
Tess: … Whenever I can get a chance, yeah?
Patrik: Please, please.
Tess: Okay. Yeah, I’ll do that then between now and whenever she has the surgery and going forward, I’ll do that as best I can.
Patrik: Yeah.
Tess: And would it be a good idea do you think to keep liaising with the specialist, the neurologist?
Patrik: Absolutely.
Tess: Because she was the one who is giving this information, yeah?
Patrik: Absolutely. Absolutely.
Tess: Okay. And she was actually, even the day before, she actually was far more measured and more respectful and reasonable in her stance than she was previously. So I completely concur your line of questioning actually allows them to know that this person actually has some insight or somebody behind them has some insight.
Patrik: Absolutely. Absolutely. That’s the whole purpose behind it or one of the purposes. So they know, you know.
Recommended:
Tess: Do I need to establish anything more about this DNR thing or is it just-
Patrik: Yes, I will send you a link. I will send you a link for you to read and then once you’ve had to read, I think we should be talking again. Give me a second, I’ll just send you a link. Just bear with me. Yeah. Just have a look at that at some point, have a read and then on our next call, we’ll talk more about it.
Tess: Okay. Okay. Thank you very much indeed. I think that’s basically it and I will try the best ascertain whatever I can.
Patrik: Yeah.
Tess: Hopefully be able to see her tomorrow and just try and get as much information as I go along. And when would it be better to speak to you in the foreseeable future? What’s the best time of day for you generally?
Patrik: Look, you tell me what you need and I will try and make myself available. Obviously, I’ll tell you when I’m usually not available, is sort of between, so I’m 9 hours ahead of you.
Tess: Yes.
Patrik: The times that I’m difficult to reach is between 3:00 PM your time and 8:00 PM your time, because that’s night time for me.
Tess: Okay. That’s fine.
Patrik: But outside of those times, just like now I can make myself available. And if you need me in the middle of the night for an emergency, you reach out to me. Okay?
Tess: Okay. Thank you very much indeed, Patrik. And thank you from Romeo, who’s asleep currently and Rey who’s beside me. I’m sure he’d just like to say thank you quickly, Patrik, and wishing you a good day. I’m just going to pass you to Rey. Thank you very, very much, indeed.
Patrik: Thank you. Thank you.
Tess: And speak to you shortly.
Patrik: Yeah. Thank you.
Rey: Sorry. Oh, I’m not used to this. Hello Patrik.
Patrik: Hi, Rey. How are you?
Rey: Hi, I’m okay, thank you. I just happened to naturally, I found you I’m very much person who does their own research on these things. And so as soon as this happened, I was looking up studies and looking up all of the terms and I just happened to come across your YouTube channel.
Patrik: Right.
Rey: And I found it incredibly helpful to watch all of the videos that you’ve put out. And I appreciate all of the information that you’re sharing with your videos and I’m really happy and glad and thankful that you are here to help us with this.
Patrik: It’s a pleasure. It’s a pleasure. I mean, if I can do that, I love to.
Rey: And you mentioned in one of your videos that it was when you had the realization that you were quite desensitized to the things going on ICU and that’s why you left, yeah?
Patrik: Very much so. Very much so.
Rey: Yeah.
Patrik: I think-
Rey: Do you know what made you realize that?
Patrick: Yeah, I think I tell you what made me… a number of things. I do believe that euthanasia is happening in ICU every day, all over the world. And I was part of it and I didn’t realize it at that time. Euthanasia is illegal. And I think it’s happening every day in ICU, but nobody talks about it. So we’re basically killing people in ICU that could live. And that was sort of one of the turning points, but there were also other turning points where I have been asked to do things that I simply refused doing. And I said, I’m not part of this anymore. You know I have my own compass.
Rey: Yeah.
Patrik: And I have to make a decision whether I want to be part of it or not.
Rey: Yeah. Okay. Yeah. Just hello. I’m here, I’m always listening in on the conversations and-
Patrik: That’s great.
Suggested Links:
Rey: I’ve been Sara’s partner and I essentially gave up my whole life to move into her house and change my whole life around. So this really means a lot to me.
Patrik: Right, right. Yeah. No, that’s good. That’s good.
Rey: Yeah.
Patrik: Let me know what you need next, please.
Rey: Thank you very much, Patrik. We’ll be in touch soon.
Patrik: Yeah.
RECOMMENDED:
Rey: Yes. When we have more information. Thank you.
Patrik: Thank you so much, thank you. Bye bye.
Rey: Thanks, bye.
The 1:1 consulting session will continue in next week’s episode
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!