Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
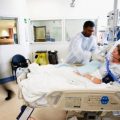
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tess, as part of my 1:1 consulting and advocacy service! Tess’s daughter is ventilated and with a tracheostomy. Tess is asking how she would stop the ICU team from pushing her daughter out of ICU.
How to Stop the ICU Team from Pushing My Ventilated Daughter Out of ICU? Help!

“You can also check out previous 1:1 consulting and advocacy sessions with me and Tess here.”
Tess: Okay, so as I’m leaving the hospital, I went back to the reception
and picked up 3 copies of a letter confirming Sarah being an
inpatient.
Patrik: Hang on, sorry.
Tess: … signed by her doctor.
Patrik: Hang on. Can you say that last part again, please? You picked up what?
Tess: Yeah. On my leaving, I went back to the reception and picked up three copies, of a letter confirming Sarah being an inpatient-
Patrik: Oh, okay.
RECOMMENDED:
Tess: … signed by the doctor. So all the while that I’ve been there… will be revelatory, because all the while I’ve been there, she had an opportunity to speak to me, probably.
Patrik: Yeah.
Tess: But she chose not to at that time, I believe. Not really, other than…
Patrik: Yes.
Tess: Yeah. I had agreed with the nurse, a Zoom chat with Sarah for Romeo and Rey last night. The doctor unexpectedly rang at 7:00 PM asking if she could update me tomorrow at 2:00 PM as Sarah will be leaving soon.
Patrik: Leaving to where?
Tess: I don’t know.
Patrik: What?
Tess: Exactly.
Patrik: Leaving?
Tess: Yeah, leaving the ICU.
Patrik: Okay. So where is she going?
Tess: Exactly. I have no idea. I couldn’t even discuss in the moment, she took me unaware.
Patrik: So you have no idea where she’s going to?
Tess: No, I don’t.
Patrik: She basically told you, “Oh, by the way, she’s going tomorrow.”
Tess: No. She’s just saying she’ll be leaving soon. Just basically, as perfunctory as that, even though I said to her in front of Sarah on the ward, the first time I encountered her, I wish for Sarah to go to the neuro-rehabilitation. And she said, “Well, she can’t move. That’s highly unlikely.”
Patrik: That doesn’t make a lot of sense to me, especially if… she’s still on the ventilator at times, isn’t she?
Tess: Yes. And she went on to say they’re going to try her on unassisted breathing tonight.
Patrik: Right.
Tess: Which I would have thought, may be inadvisable given she’s still got sticky secretions. Anyway… and said that would not be convenient. I said that would not be convenient for 2:00 PM because she’s just doing a rush job on me. She suggested at 4:00 PM, when I intended to see Sarah. I said, “Well, I wish to see Sarah at that time.” She said, “How about before or after?” My appointment to see Sarah. I said it would be more convenient Sunday because then we can prepare. Rey could potentially be there at the same time, and I would have obviously a witness in Rey as well, with me.
Patrik: Yeah, absolutely.
Tess: And, “I would have to consider the matter,” I said to her, “And get back to her in half an hour.” She said she was contactable on the ward because I said, “Where do I ring back?” Although the number was withheld, I decided not to ring back last night, and because of the very bad interconnection outages, decided to not ring the ward, and go ahead with Zoom meeting with Sarah, so we aborted the Zoom meeting because we genuinely had really bad outages in this area, and it would have interrupted the process of the Zoom call.
Tess: But at the same time, she unexpectedly rang up and she was trying to obviously take the power from me, and then dictate to me when it was going to happen. And even then, I don’t know whether I’m going to be faced with a palliative care team… all this I don’t know, I didn’t know.
Patrik: When you talk to them, can you record on your phone?
Tess: No.
Patrik: Right. It would be good. It would be good, but anyway.
Tess: I can, but I only can when I have access to the phone that Amy has got.
Patrik: Right.
Suggested Links:
Tess: And I can’t be assured of how easy or otherwise that would be. My point is this, she wanted the meeting at 2:00 PM. She was a little bit funny about the fact that I was reluctant to do it before or after, me seeing her today at 4:00 PM. It’s already inconvenient for me because I’ve aborted… well, with the outages as well, but it put me off the idea of having a Zoom call because why would I be going ahead and having a Zoom call between 8:00 and 9:00 with the nurse assisting the process, when she’s just rung from the ward at 7:00? Do you know what I mean?
Patrik: Yeah.
Tess: And in the moment, it took me off guard. So my question to you Patrik is, I really want to be able to have you talk to this woman-
Patrik: Sure.
Tess: … if it were humanly possible.
Patrik: Yeah, sure. For sure. For sure, we can do that.
Tess: With me on the line as well?
Patrik: Yeah, for sure.
Tess: Will it be over a three-way call?
Patrik: Yeah, for sure.
Tess: I think that, that would be ideal at this point, because at the moment, I’m assuming because I haven’t heard from the ward, that Sarah’s okay, that the night was okay for her, I don’t know. I haven’t rung the ward, and I wished to speak to you and put this by you beforehand, so that you’ve got an idea. She had ample opportunity in my personal opinion, to just acknowledge me, quickly come over to me. I think what they did was by cancelling my appointment, they probably agreed amongst themselves… and this is just suspicion on my part, they have agreed amongst themselves, “Oh well, let’s cancel her appointment, she’ll be free for an hour and then you, the receptionist, suggest to her that an update can be given by the doctors.”
Tess: But I didn’t take him up on that opportunity. I didn’t feel comfortable at that moment, and so I left with Romeo, the reception area, and went and sat downstairs. But the point being, is that I can’t be avoiding talking to them at the same time all I would like is for them to just be transparent with yourself, with myself, over a matter that is really like… I know that there’s a ward. Okay, another factor… I know there’s a ward for rehabilitation, a neuro-rehabilitation ward in the same hospital, but it’s like a catchment area thing, and because I’m in another place, Sarah wouldn’t literally be taken maybe to that ward within the hospital, because she doesn’t fall under that catchment area.
Tess: So the only other option would be the other rehabilitation.
Patrik: Why? Do you know why?
Tess: I don’t know whether her shift ends today and that’s why she was eager not to let me have Sunday as a possibility of my suggestion, so it’s all a bit up in the air at the moment, Patrik.
Patrik: Why is she avoiding the subject about this one rehabilitation facility? Why do you think?
Tess: Because Sarah’s not moving at the moment, and they probably think that she’s not even worthy of getting their attention, but she certainly is. She needs help desperately.
Patrik: Yeah, yeah. No, there’s no question about that.
Tess: She needs care and time to heal.
Patrik: Yeah. No, for sure. For sure, absolutely. If she needs anything, she will need time. Absolutely, I couldn’t agree more with you.
Recommended:
Tess: Certainly. And the fact that they really got her off, they’re really weaning her really quickly in spite of the fact that she’s got potentially, this… whatever it is, residual… I mean, for all I know, she could have had an allergic reaction and she’s just trying to get through that, or it’s a post-infection resulting in her lung tissue, but the whole process is, obviously the suction aspect, is very uncomfortable for her. You can see it on her face when it happens, whether she’s under the influence of paracetamol or not.
Tess: But she’s there, she’s there, and her eyes are open, and I know that Sarah’s present, so it’s very distressing for her not, ostensibly, to be moving. Except for this twitching aspect that is being suppressed, I’m assuming, by whatever they’ve placed her on. Keppra, 1.5 gram twice a day apparently, and the sodium valproate, 500 mg two times a day, I established yesterday.
Patrik: Yeah. When do you want me to talk to this woman?
Tess: Well, I think that it’s now 10:20, I think that I’ve got to try to establish whether it’s possible to have a call, and also indeed, whether it’s possible for us to have a three-way call.
Patrik: Tess, you don’t ask for permission. You just get me on the call. You need to change your thinking.
Tess: Okay.
Patrik: You do not ask for permission. You never ask for permission when it comes to your daughter.
Tess: Yes.
Patrik: Stop being intimidated by them. You do not ask for permission. You do not ask for permission taking pictures, you do not ask for permission getting someone on a call. Stop that.
Tess: Okay.
Patrik: This is your daughter, don’t be intimidated by their tactics.
Tess: Okay.
Patrik: Because I’ll tell you what they will do. They will turn around and they will say, “Oh no, we can’t give information to somebody else.” You just get me on the call and you say, “Oh, I’ve got Patrik here.” That’s how you do this. Keep things simple.
Tess: Okay. So how do we do it? What would you prefer? Because that was the first suggestion of 2:00 PM.
Patrik: Okay, all right. 2:00 PM. Yeah, we can do 2:00 PM.
Tess: Shall we try-
Patrik: Yeah.
Tess: … if you don’t mind, please?
Patrik: Yeah, not at all.
Tess: And I’ll get you to ring, what? Ring the ward or how can I… I’ll try and establish if there’s a direct number for the doctors-
Patrik: Well, try and set it up with her and ask her who you need to call. You don’t need to talk about me. You can if you want to. It’s up to you whether you want… but I tell you, they are already putting up the barriers, so you don’t want to put up another barrier. You introduce me when we are on the call.
Tess: Okay.
Patrik: Unless you feel like you want to talk to her about me when you set it up, but I feel like knowing how hospitals operate, I just think they need to deal with the facts, not with maybes or maybe-nots or you know, that’s how I view it.
Tess: Well, my deepest concern in all of this is that Sarah, obviously her life has been saved, a tremendous amount of money has been spent thus far to achieve that. I’m extremely grateful to them for all of the efforts-
Patrik: Of course.
Tess: … they’ve conducted thus far. Don’t get me wrong in any way. I’m very appreciative, but at the same time, I get a distinct impression that the next placement in Sarah’s life, where she’s placed and the amount of consistency in the care applied, is incredibly important for her overall well-being going forward. And also, her potentiality to survive what she’s already gone through. And that is my paramount concern, and I believe that the quality of care that could potentially be given to her via different neuro-rehabilitation would be the wisest move to make in this situation for Sarah’s sake.
Tess: Not being placed in some kind of end-of-life, nowhere land where she could potentially die and die of… well, of malpractice or of failure on their part, whoever’s in her care, whoever’s conducting her care. At this particular point, I wish to stress obviously that, because that’s where I’m at-
Patrik: Yeah, I know.
Tess: … as her advocate. And I know that Sarah would genuinely wish to have an opportunity to get the best that she could possibly get given the circumstance she’s in.
Suggested Links:
Patrik: I agree, I agree. This doctor, is this the first time you’re dealing with her?
Tess: Well, the first time I dealt with her was she unexpectedly ringing me about the fact that the tracheostomy was going ahead, and she said, “She needs the tracheostomy, it will save her life.” She said that they’d discussed it amongst themselves and there were those that were against it and they want it to be conducted in the theatre. But she claimed to be the one that said it could be done at the bedside.
Patrik: Right.
Tess: I said to her, “How many, amongst yourselves, were for the theatre idea?” And she wouldn’t tell me.
Patrik: That’s ridiculous.
Tess: But it was the right thing to do.
Patrik: Yeah, no.
Tess: She made the right decision in the given situation.
Patrik: Yeah.
Tess: And as you’ve already gathered from me, Patrik, there are many people that don’t even get to that point of getting a tracheostomy.
Patrik: Oh, of course. Yeah, we know that. We know that. Yeah.
Tess: Yeah. And she’s being weaned off really successfully, as far as I can see.
Patrik: Yeah, no, no, she’s on her way. She’s on her way out of ICU, there’s no question about that.
Recommended:
Tess: What would you imagine the next move, having worked in this country, what do you think that they would want to do?
Patrik: If you weren’t advocating for her, or if you hadn’t advocated for her from day one, they would have moved her to palliative care by now, that’s for sure. But obviously, that’s not the case, but you got to be prepared that if, for whatever reason, things are deteriorating, they will try again. What do I think is going to happen next? She needs to be off the ventilator so that she doesn’t go back on the ventilator. Once she’s off the ventilator, they will probably move her to a hospital ward next, and then they will probably look for rehab next. But she won’t go from ICU to rehab. I would be very surprised.
Tess: Yes. Okay. If we get in the call together, should I mention the matter of the neuro-rehabilitation ward? Would it be possible for her to go there in the interim period?
RECOMMENDED:
Patrik: Again, Tess, you’re overthinking things. Any questions that you have, you ask her. You’re overthinking. If you have questions, ask her.
Tess: Okay. Right. So, my task now is to… I’m assuming that it would be you calling the number that I relay to you, yes? And then I’m on the phone at the same time?
Patrik: Yes. And how do you think you want to introduce me to this woman? Do you want to go about it like we did with the nurse, or do you want to go about it…
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!