Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
Mom Had a Hypoxic Brain Injury After Cardiac Arrest. She’s Not Waking up in ICU! Live stream!
You can check out last week’s question by clicking on the link here.
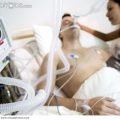
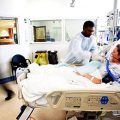
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tess, as part of my 1:1 consulting and advocacy service! Tess’s daughter is on a breathing machine and with a tracheostomy. Tess is asking why is it important for her daughter to be weaned off the ventilator as early as possible in the ICU.
Why is it Important for My Daughter to Be Weaned Off the Ventilator As Early As Possible in the ICU?
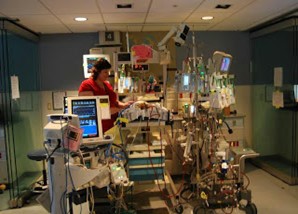
“You can also check out previous 1:1 consulting and advocacy sessions with me and Tess here.”
Rey: Basically we found a form here the…
Tess: Yeah. Bear with me. I’m just going to pass you to Rey.
Rey: Yeah. Okay. Hello.
Patrik: Hi Rey.
RECOMMENDED:
Rey: Hi. I’m right. Yeah. I found a GP (General Practitioner) referral form that they fill out when they’re trying to admit patients and consider the options for neuro-rehabilitation. Under listed the specific neuro-rehabilitation hospital that we would like her to go to as a first choice. It does say that they have specialized care for tracheostomy. It’s under the word tracheostomy. It’s listed as a specialized hospital dealing with that sort of thing.
Rey: There is another one nearby as well I think, but that stood out to me in particular, because I know what you say is that these places usually don’t have that specialized treatment. But the fact that they specifically listed that is ought to note.
Patrik: No. That is definitely to note. If there is something that’s better, that’s great. From experience, those hospitals are far and few in between.
Rey: Those hospitals are far and few in between, Tess. Yeah.
Patrik: No, it’s great. If there is something, that’s fantastic. Are they specifically talking about tracheostomy only or are they talking about tracheostomy and ventilation?
Rey: I believe it just said tracheostomy, but Tess’s going to get the actual paperwork now, so I can be very exact.
Tess: Ask if it’s necessary for her, because she hasn’t got a doctor at the moment. Would it be a good idea to be able to liaise with the doctor?
Rey: You mean the GP, right?
Tess: Yeah.
Rey: Would it be a good idea to liaise with the GP about where she would want to go?
Patrik: No, I don’t think so. I think the referral for rehabilitation needs to come from a neurologist.
Rey: It needs to come from a neurologist. Okay.
Patrik: That doesn’t mean don’t talk to your GP. I’m not saying that. But at the end of the day, this will probably be a neurology referral.
Rey: Yeah. I thought as much. It says here, “Specific areas of expertise, specialism,” section C. Where is it? It’s described as, “Complex physical tracheostomies, et cetera.” It also says, things about the other rehabilitation which is the one that we may want her to go to. So all it says is complex, physical tracheostomies.
Patrik: Right. Okay. Look, there might be a small chance of them being able to do ventilation as well, but I kind of doubt it. Hopefully they will do that.
Rey: Yeah. Okay. I’m going to pass you back to Tess now, okay?
Patrik: Sure.
Rey: Thank you.
Patrik: Sure. Thank you.
Tess: Okay. We’re in that place of neither here, nor there in the sense of we can’t do very much until she actually shows more signs of responsiveness, yes?
Patrik: Look, not necessarily. She may not show any signs of responsiveness and they still want her out of ICU. I think the next challenge for her will be, she needs to stay clear of an infection because that risk is there in ICU. But she needs to stay clear of an infection. It can be a long process. The longer the process goes on, they either want to send her to a ward as quickly as possible, which will be difficult if she stays ventilated. It’ll be easier if she can be weaned off the ventilator. At the moment, yes, you may want to think about rehab, but at the moment, her next steps are to leave ICU.
Patrik: Her next steps are to get off the ventilator if possible.
Tess: Okay. As with dealing with doctors, how do you suggest I proceed? Just like the circumspect and moderate about the way I handle them and not antagonize in any way, because obviously I’m conscious of the fact that they’re very much instrument. The doctor’s decision-making is either the make or break. Do you know what I mean? I don’t wish to alienate in any way.
Patrik: Yeah. Who is she? Is she ICU consultant or is she a neurologist?
Tess: No, she’s not a neurologist. We can’t even find actually what exactly she is, to be honest. We were looking at earlier. I couldn’t establish that as yet. I’ve got to find that out.
Patrik: Where do you get medical information from at the moment?
Tess: None whatsoever. For Sara, nor for myself. We don’t go to a doctor or anything. Is that what you mean?
Patrik: No, at the moment in ICU, how do you…
Tess: Oh, okay. I’m ascertaining what I can from the nurse, but it depends on the character. They tend to be somewhat reluctant to say anything. The person today, he actually referred me to the doctor and said, “If you wish for an update or any other details, you need to speak to the doctor.” The doctor was in the ward doing the round at that moment of a few beds up. So that’s on that front.
Suggested Links:
Tess: I usually ascertain things from either the neurologist, who’s consulted with us, or there’s a director of the whole area, who was a man. We spoke to him about six or seven days ago, I believe. Also, there’s this another doctor. I’ve never met her before, but she rang up randomly saying that she wanted to do the tracheostomy and that would potentially save her life given the situation.
Patrik: Yeah. I agree with that. The tracheostomy, I would argue she’s probably much more comfortable than last week with the breathing tube. Is that fair to say?
Tess: I would imagine, well. Yeah, very much so.
Patrik: Right. So you can see things are progressing, but it’s often baby steps. You may not see the improvement on a day-by-day basis, but you probably see the improvement compared to last week.
Tess: Yes.
Patrik: Right. On the days where you think, “Oh my goodness, it’s not progressing.” You got to look at, “Okay, what did it look like a week ago?”
Tess: Now, I’m assuming that I didn’t even mention that time, the word agenda, can I have an agenda before we actually meet or anything like that? I was a bit preoccupied with Sara at that time. I wasn’t quite sure what was the most pressing thing to address in the moment. But the fact that they would want to have a more serious, formal meeting later on this week, I think that’s important that Rey is there as another witness. That would be possible come Friday or Saturday.
Tess: Can you imagine how long it might take potentially for Sara, if she’s at four hours on off, and then all through the night for her own comfort? How long could this weaning process potentially take if it was in a successful way?
Patrik: I can’t answer that question until I’ve seen a picture of the ventilator.
Tess: Okay. That has a bearing on your estimation.
Patrik: Very much so.
Tess: Okay. I will try and do that tomorrow. I’m going to be seeing her at 4:00.
Patrik: Or what we could do, if you’re there, I could call you and I could talk to the nurse. I could ask some questions.
Tess: Yes, that would be a good idea, actually.
Patrik: Yeah, sure.
Tess: I would be there at 5:00 in the afternoon.
Patrik: Yes.
Tess: And then we can try and work it out from that point on, going forward for this coming day, an opportunity maybe to speak to the nurse.
Patrik: Another maybe simpler option might be we just call them anytime.
Recommended:
Tess: Okay.
Patrik: Yeah. We just call them and talk to them.
Tess: Talk to the actual ward, because I have a direct number for the ward. But the actual line is really poor quality.
Patrik: Right. Okay. Fair enough. We have to try.
Tess: Yes. Okay. Also, it might be because there’ll be a one-on-one nurse to Sara, it may have to be arranged that they actually can take time out from Sara and then be replaced in the moments. So it’s all…
Patrik: No. Does she have a phone in the room?
Tess: There is a phone literally in front of Sara’s bed, a bit of a distance.
Patrik: Then it shouldn’t be a problem for the nurse to talk. If he can stay in the room, there shouldn’t be a problem.
Tess: Okay. That’s good. Shall I give you a ring later on and see where we are at in the whole scheme of things and see if it’s possible? Because I know that their changeovers occur for us at about 7:30, roughly in the evening. They like to know everything’s going to happen for the day. So it’s an 7:00 in the morning, and 7:30 in the evening changeover.
Patrik: Right. Are they doing 12-hour shifts there?
Tess: Yes.
Patrik: Right. Okay.
Tess: Yeah. Would it be better to get to speak to somebody that had obviously spent the past 12 hours with her than to get involved with somebody who’s just literally coming on board?
Patrik: It doesn’t matter. A good nurse knows what they’re talking about. They have information.
Tess: Okay. We do that as a three-way conversation, yeah?
Patrik: Yeah, absolutely.
Tess: Okay. That sounds encouraging to me. Because I think you may well potentially get better result from the nurse than from the doctor. I don’t know, she’s quite pompous.
Patrik: Right. She’s an intensive care specialist or…
Tess: This is the thing. I’m not entirely sure what her position is. I know she does tracheostomies at the bedsides.
Patrik: She did the tracheostomy at the bedside?
Tess: Yes, she did.
Patrik: That’s probably ICU specialist. Is she someone you’re dealing with regularly?
Tess: No. It’s the first time I’ve met her. I did speak to her as I said, when she alerted me to the fact that it was going to go ahead on Saturday morning.
Patrik: Right. Have you spoken to any other ICU specialists in there?
Tess: Other than Dr. Kamila briefly on two occasions, no. Not really.
Patrik: That’s terrible. How do you get updates?
Tess: I’ve had most updating through the neurologist, the consultant. But in terms of the doctors, they gave it a bad prognosis as we’ve already stated, Patrik.
Patrik: Yeah. No, for sure. Be prepared that they will give you a bad prognosis for some time to come.
Tess: Okay. Yeah. I’m prepared for that. Obviously, I wish for something different and much better, but I’m prepared for that.
Patrik: Yeah. You will need to be prepared for that negativity.
Tess: Okay. I think that they do four-day shifts, these doctors. There’s potentiality for this doctor to have been gone by the end of that shift, which would come up maybe midweek anyway. So I don’t know. I’m not entirely sure. I’d have to find out more about her somehow. But ascertaining from the nurse probably would be better. How should we take that? Just I introduce you as the professional advocate of Sara and myself.
Patrik: You can do that or you can introduce me as a family friend with a critical care nursing background, that’s helping you to make sense out of what’s happening either or I…
Tess: Which you think would work better?
Patrik: I am not sure to be honest with you. It really depends on the dynamics. What’s your feel? Which one would work better in this situation?
Tess: I think being straightforward and saying that you are Sara and our professional advocate.
Patrik: Yeah. Okay. I’ll take that because sometimes ICUs can feel intimidated. They get that backs up.
Tess: Okay. Right. Yeah. I’ll have to think about that. I’ll ask Romeo.
Patrik: Yes, ask Romeo.
Suggested Links:
Tess: He’s asleep at the moment. I’ll get that and ask him that for you in the morning. I’ll give you a ring later on today.
Patrik: Yeah, absolutely. But I think since we last spoke, there are definitely positives. She’s moving forward. Ask for the Glasgow Coma Scale.
Tess: Okay. I might be able to get that until 5:00 tomorrow afternoon.
RECOMMENDED:
Patrik: I doubt it. Let me ask you this. If you rang the nurse now and you ask them, “What’s her Glasgow Coma Scale?” Do you think you’ll get the nurse on the phone?
Tess: Not necessarily, because they are the nurses milling around.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!