Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
The ICU Team Express Negativity About My Ventilated Daughter’s Condition. How Can I Deal With It?
You can check out last week’s question by clicking on the link here.
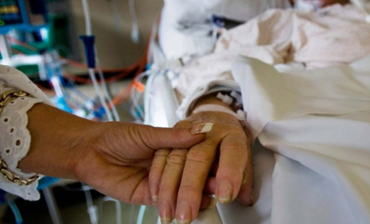
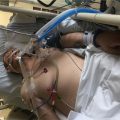
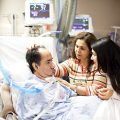
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tess, as part of my 1:1 consulting and advocacy. Tess’s daughter is with a tracheostomy in the ICU. Tess is asking how can they become the best advocate for their daughter.
Our Daughter is with a Tracheostomy in ICU. How Can We Become the Best Advocate for Her?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Tess/Romeo here.”
Tess: I’ve been gleaning as much as possible from those that I can, the nurses.
Patrik: Yeah, you need to get access to the medical records.
Tess: Well, I’m just juggling as it is the whole process of having to travel a distance to get to her.
Patrik: How far?
Tess: Well, south part of the town, which is about 45 minutes to an hour away.
Patrik: Right.
Tess: On the train and bus. Which is not that great a deal but at the same time, it is a concerted effort, so at least taking up about four to five hours thereabouts once getting there, then travelling back.
Patrik: Sure.
Tess: Well, three in all fairness maybe.
Patrik: Sure.
Tess: It depends on how long I’ve been in to see her. But they’re only giving me two video calls a week with two in person visits and being present at two assessments. So effectively, six out of seven days, and tomorrow’s the day that unfortunately, it’s been arranged that we can’t just visit. My point being is that it’s not good enough because they’re also not allowing her boyfriend to see her.
Patrik: Oh, my goodness.
RECOMMENDED:
Tess: They’re opening up restrictions to an extent. I have to go in and basically, relatively prevent us from seeing her. Romeo is giving up his time with her so that I can be with her more. Yeah, it’s just really quite stressful, the whole situation.
Patrik: There’s no question around that. Look, you need to establish guardianship because this could potentially become ugly. If you don’t want to be fighting with the hospital over guardianship, now is the time for you to put that in place. Because if you challenge the whole Do Not Resuscitate (DNR) and not going back to ICU, the hospital might do a grab for guardianship and you don’t need that. I know it’s stressful and I wish I had better news for you but in order to protect yourself and Sarah, that’s what you need to do as a next step.
Tess: And I assume that’s court protected.
Patrik: I am not the lawyer, Tess. My area of expertise is clinical, I couldn’t say how you go about it, I couldn’t point you in that direction. What I know 100% is you need to get guardianship with no uncertain terms, that’s what I do know.
Tess: Okay. Not power of attorney, guardianship?
Patrik: Again, you need to talk to the family lawyer about that. I am not a lawyer, I’m a clinician.
Tess: I know. And we’ve discussed this before.
Patrik: This is important, Tess. This is really, really important. If you end up in a fight over guardianship to the hospital, that could get real ugly, really, really ugly.
Tess: Right. Okay. Well, I’ll try and start working on it.
Patrik: In the meantime, my advice is that you will be continuing to advocate for her and say, “Look,” you want her back in ICU. It’s important that you document that, I would do that in an email. That’s how I would do it because if you’re not doing it in an email, they might say, “Oh, you’ve never talked to us.”
Patrik: And you have to challenge them. Well, if you don’t want to challenge them, you’ll definitely lose. It’s up to you, I just give you the best advice that I can do.
Tess: Yeah.
Patrik: Repetition is the mother of all skill, you need to, in the nicest possible way, challenge that every day. They need to know that you are serious about this because if you just mention it once or twice they just think, “Oh yeah, you’re not serious anyway.” So I would escalate this but before you escalate this, I would 100% making sure that you’ve got guardianship.
Suggested Links:
Tess: Okay. What, so one comes before the other, yeah?
Patrik: So I’ll tell you what could happen. Let’s just say you challenge them, and I believe you need to challenge them one way or another, if you keep challenging them, they might say, “Oh, I don’t want to deal with that, I’ll just try and get guardianship,” and some hospitals unfortunately succeed with that. If the hospital gets guardianship, you will have no say whatsoever, nothing.
Tess: Wow, so that’s no good.
Patrik: No, it’s no good. That’s why I said last time, you need to get guardianship. Because if you had guardianship already, you could go in with the hard guns. At the moment you almost need to tread carefully.
Tess: Oh yeah, another thing, yeah, that is quite important, the neurologist said on the phone with the director on the phone that from the computerized tomography (CT) scan, the radiologist had found that Sarah’s potential lung capacity… Because I asked her and she said, “It’s about 15, 20%,” which doesn’t make sense at all to me. She said, “Somebody could survive with 50% lung capacity or one lung,” but the point is that I’m being told there’s no infection.
Patrik: Right.
Tess: It’s not a matter of infection, it’s a matter of a sputum plug.
Patrik: Right.
Tess: And obviously she said that’s quite commonplace for that to happen with a tracheostomy.
Patrik: Well, I wouldn’t say it’s commonplace but I would say it can happen. A sputum plug can definitely happen but I also argue that if she was in a better environment than in rehab… And rehab is good but on the other hand, they’re not ICU nurses there and therefore, the chances of her ending up with a sputum plug are so much higher in that environment compared to ICU.
Tess: But the problem is she can’t be indefinitely in ICU.
Patrik: No, no, of course not.
Tess: And they may see that she’s actually stable on the whole, other than the fact that they actually change the tracheostomy tube. I’m assuming that they did, yeah?
Patrik: Assuming.
Tess: It’s extremely sketchy.
Patrik: Right.
Recommended:
Tess: And so, I get it, guardianship.
Patrik: Guardianship, guardianship.
Tess: Okay, I’ve got no choice, have I?
Patrik: You’ve got no choice. Yes, you’ve got no choice but also, it’s critical, it’s absolutely critical.
Tess: How long do you think it could take?
Patrik: I have no idea. Again, this is a question that you need to ask to a family lawyer, I have no idea. I think it should be fairly quick because you are the mom, there shouldn’t be an issue.
Tess: Okay.
Patrik: In the meantime, yes, you need to challenge it because yes, they’re doing what they want to do but you need to challenge it.
Tess: Yes, I am trying to do that as well but I was told that… Because basically, the day before her electrolytes were in balance basically, except for a little bit low on the potassium but well within range, that’s what I was told by the nurse on the ward itself with a few others. And yeah, obviously it’s almost like a potential hazard with all this. And also, two nurses turned up after I’d visited her yesterday and they did a suctioning action on her and they’d come from the ICU anyway, apparently.
Patrik: Right.
Tess: And she’d seen her on there and she didn’t think that she was bad, but that’s incongruent with what I’m being told by the neurologist.
Patrik: Right.
Suggested links:
Tess: Because they’re saying she’s apparently aspirated many times before and I can’t see that, that could be the case unless there’s been major negligence along the way. Because as far as I’m aware, they were trying to mobilize her a little bit at the last part of her stay at the hospital before she made her way over to the city. And also, they thought that she wasn’t going to be able to achieve it but she was able to sit in a chair for about an hour.
Patrik: Right.
Tess: But she hasn’t been properly being mobilized and yet a physiotherapist has been assigned to her, ostensibly, on the piece of paper, on the board behind her, and also a speech and language therapist who hasn’t spoken to her yet. I understand that she was at 40 kilograms and then has gained five kilos effectively in the past week, so she’s incredibly thin, yeah?
Patrik: Right.
Tess: And she’s tall, and she’s trying really, really hard to survive.
Patrik: When you see her, what is she doing? Is she making eye contact with you?
Tess: Yeah.
Patrik: Right. If you ask her to squeeze hands, is she squeezing hands?
Tess: Well, with the myoclonus, I don’t know whether it’s potentially normal movement in her forearm and her hands but she had hand splints on and I asked specifically to have it removed so I could hold her hand and it curled immediately into mine. But I don’t know whether that’s contraction related or genuine relief from being in a splint position, so it’s difficult to say. She’s got a very strong grip whilst holding my hand.
Patrik: Okay. Okay. So, let’s just say she’s not squeezing fingers because of the splint, can she do other things on command? It doesn’t have to be squeezing hands, it could be if you ask her to-
Tess: I think she is attempting or has attempted on my command to slightly close her eyes but it’s really, really difficult to determine because the actual myoclonus twitching around her eye muscles, as they were so active today, they would prevent me from really being able to read correctly. And there was a psychologist there, and then the psychologist took me to one side and said, “Do you know that we can give you a counsellor to help you with?” And I said, “I’m a strong person, my husband’s a strong person, we’ll close this in our own time.” And basically, “I don’t need your help.” Yeah.
Patrik: All right.
Tess: I think that was a setup in its own way because if I fall into a trap or try and confide in anybody else within that situation, it would be used against me.
Patrik: Right.
Suggested Links:
Tess: I suspect. I don’t feel inclined and I am a strong person, I don’t feel inclined to do that.
Patrik: No. But unfortunately, look, I’m all for making friends if you can but I also know how hospitals operate. And at the time, a few years ago, there is a very public case, did you follow that case in other institutions.
Tess: No.
Patrik: There was a very public case a few years ago. A very public case in one of the famous hospitals.
Tess: Yes.
Patrik: Right. Cutting a long story short, there was a very public case in the other hospital where in the end, they basically removed life support for a dying toddler even though the family had all the money and everything to fly him overseas and get treatment overseas. And it was a very nasty situation because the hospital got guardianship in the end, it was just ugly as hell. It was very public at the time, we were working with the family at the time, so I had insights into what was happening, you need to get guardianship, that’s all I’m telling you.
Patrik: Because hopefully it’s not getting to that point but I’m just telling you, from my experience, if you’re not having guardianship, you’d definitely be fighting an uphill battle.
Tess: Okay, okay. Well, I don’t have money to just throw at the process but I’m going to have to seek help, so I’ll do that.
Patrik: You will have to seek help there.
Tess: Yeah, okay.
Patrik: As far as the whole ICU readmission goes and the DNR, you do need to keep asking for that. You will also need to ask for access to the medical records. Again, this is right, not a privilege. You have every right, and I’m pretty sure I sent you the link way back when, that you have the right to access medical records, and you go from there.
RECOMMENDED:
Tess: Another thing that is also very important to consider is that they can drop her like a hot potato if they so wish and push going into a care home. Which obviously we don’t want and we stated that right from the get-go in the meeting, yeah? So really, genuinely, I feel very, very pushed because I don’t want to jeopardize Sarah’s chance of getting rehabilitation, it’s like she’s got one bite at the cherry as it were. And I think that she could potentially be close to emerging because deep action myoclonus, they are something that can manifest when somebody is in a minimally conscious state as they’re coming to emerge from that. It could be that she is becoming more aware of her surroundings and being distressed, internally distressed by it all.
Patrik: I could not agree more with you, Tess. I could not agree more with you.
Tess: And that’s what I’m genuinely concerned about, especially given she’s very attentive to me. She’s very attentive to my eyes.
Patrik: Yeah, I have the same concerns there, Tess. I have the very same concerns there. The only way at the moment forward is to keep challenging it. And I’ve just sent you in Skype more information, I shared this with you before but I’ll send it to you again now, just how to access medical records and how to deal with a DNR. Just because it’s difficult, you need to keep challenging it, there’s no other way.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!