Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM, where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question last week was
You can check out the answer to last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer another question that we get quite regularly from our readers and the question this week is
What’s the difference between an induced coma and sedation?
In today’s question I want to explain what seems to be very confusing for many families of critically ill Patients in Intensive Care!
Many families who come to seek out our expertise and advice seem to get confused about some of the terminology being used.
Today I want to look at some of the terminology and I want to make sure that you and your family understand the difference between an induced coma and sedation.
Let’s start with an induced coma.
An induced coma is a medically induced coma where critically ill Patients are put asleep by powerful sedatives(I.e. Propofol/Diprivan and/or Midazolam/Versed) and opioids(=strong killers I.e. Fentanyl, Morphine, Remifentanyl) in order to be able to tolerate mechanical ventilation and a breathing tube.
You may ask which issues are leading to what treatment and it’s obviously a chicken and egg question.
Is the induced coma leading to mechanical ventilation and the breathing tube or vice versa?
The answer is that it depends and in some instances a critical illness such as a severe Pneumonia, Asthma, rib fractures or COPD is leading to the inability to breathe, therefore it requires mechanical ventilation and a breathing tube as a first line and also as a life saving and life sustaining treatment.
Mechanical ventilation with a breathing tube can’t be tolerated without sedation and opioids(=strong pain killers) and therefore some critical illnesses warrant intubation(=insertion of a breathing tube in the throat) and the mechanical ventilator as a life saving measure first.
Before a doctor can intubate(=insertion of a breathing tube) a critically ill Patient, they need to be induced into coma, because again intubation, the breathing tube and mechanical ventilation can’t be tolerated without an induced coma as it’s too uncomfortable.
The reason mechanical ventilation and the breathing tube is so uncomfortable is simply that it requires high pressures to ventilate a critically ill Patient and having a breathing tube stuck in your throat is very uncomfortable too.
In other circumstances, an induced coma comes before the breathing tube and the mechanical ventilation.
For example, in road traffic accidents and/or Multitrauma where severe fractures have been sustained and severe pain or major blood loss can be expected, an induced coma is instigating mechanical ventilation and the breathing tube is another.
In those circumstances it’s not necessarily a breathing problem that’s leading to an induced coma and to mechanical ventilation and it’s more of an assessment of an overall critical or catastrophic clinical situation where complications are to be expected and therefore mechanical ventilation, a breathing tube and the induced coma are life saving measures to treat a critical illness.
Especially in such complex clinical situations like Polytrauma, Sepsis, Cardiac arrest etc… an induced coma, a breathing tube and mechanical ventilation are treatments of choice.
An induced coma is also a procedure being used during Anaesthesia for surgery.
Please check out this article/video about Induced coma in more detail
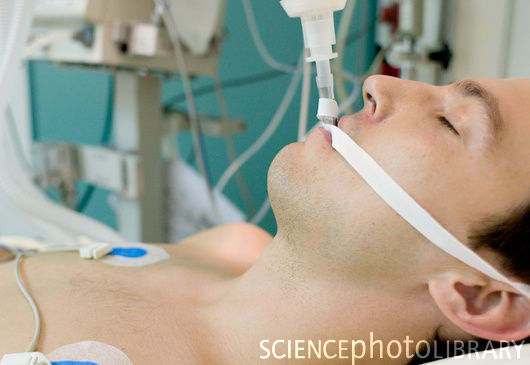
What exactly is sedation being used for?
Sedation on the other hand is just referring to the drugs that are being used for an induced coma.
Strictly speaking, sedation or sedatives are drugs being used to put a Patient asleep.
The most commonly used drugs to “put a Patient asleep” or in an induced coma are Propofol(Diprivan) and Midazolam(Versed or Dormicum).
Propofol(Diprivan) is a short acting sedative and it means that even after high doses of Propofol(Diprivan) a Patient should “wake up” within minutes or hours because it gets metabolized really quickly.
Propofol(Diprivan) is commonly being used for short term induced comas and it can also be used for longer term induced comas. Its main side effect is hypotension(=low blood pressure).
Midazolam(Versed or Dormicum) is a sedative that’s also being used to “put Patients asleep” and in an induced coma. It’s more longer acting and it’s often being used for longer term induced comas.
Midazolam(Versed or Dormicum) is a Benzodiazepine and can be addictive in nature. Therefore if critically ill Patients in a long-term induced coma are coming out of the induced coma it is recommended to reduce Midazolam(Versed or Dormicum) slowly because critically ill Patients might be addicted to it and they need to come off slowly due to the withdrawal.
The main side effect of Midazolam(Versed or Dormicum) therefore is addiction and potential withdrawal after use.
What’s also important to note is that sedation and sedatives can’t be looked at in isolation without mentioning and looking at Opioid drugs(=strong pain killers).
Related:
There is usually no use of sedation and sedative drugs without the use of opioid drugs such as Morphine or Fentanyl.
The induction of a coma always requires both, sedation and opioids(=strong pain killers).
The reason being is that sedation will put a Patient asleep but can still cause pain if not well managed.
Hence you can put a Patient asleep with sedatives like Propofol and Midazolam, get them on a ventilator and insert a breathing tube but that could still cause pain with the use of opioids such as Morphine or Fentanyl.
It’s also important to note that many critically ill Patients in Intensive Care who receive high doses of Midazolam(Versed or Dormicum) as well as receive high doses of opioids like Morphine or Fentanyl, especially after a prolonged induced coma are at risk of withdrawal from those powerful medications.
Both, Midazolam(Versed or Dormicum) as well as Morphine or Fentanyl are addictive drugs and therefore “coming off” those drugs often needs management and monitoring so that Patients don’t go through a withdrawal that’s not being managed.
Unmanaged withdrawal from Midazolam as well as opioids like Fentanyl or Morphine can cause critically ill Patients to become confused, agitated, delirious and/or aggressive. It could potentially also cause seizures.
I hope this clarifies he difference between induced coma and sedation.
Please also check out the following articles/videos for more information about induced comas
Your friend
Patrik Hutzel
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips& strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to your and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!



