Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How to Have Control and Peace of Mind Whilst Our Daughter is Critically Ill in the ICU?
You can check out last week’s question by clicking on the link here.
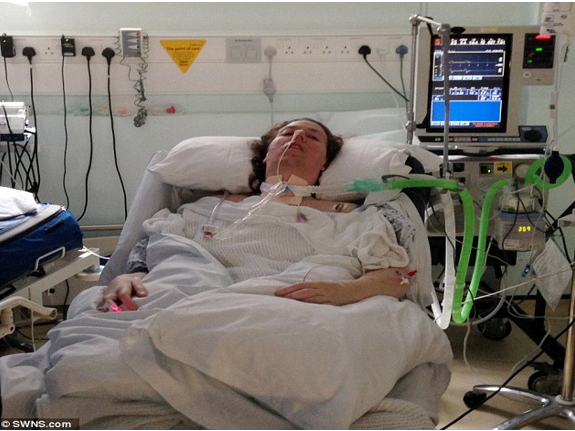
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tess, as part of my 1:1 consulting and advocacy. Tess’s daughter is ventilated and critically ill in the ICU. Tess is asking what are the risks of having a tracheostomy.
My Daughter is on a Ventilator and Critically ill in the ICU. What are the Risks of Having a Tracheostomy?
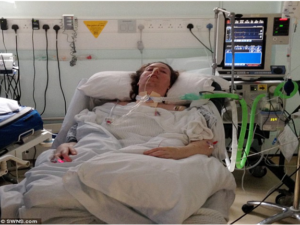
“You can also check out previous 1:1 consulting and advocacy sessions with me and Tess/Romeo here.”
Tess: So maybe as it is.
Patrik: Yes. No, I get that, I get that. When you mobilize someone in ICU, when you do this for the first time, it’s not that you sit them in a chair and you leave them there for hours. Mobilization in ICU might be they’re sitting even on a chair for 10 minutes and back to bed. And then maybe the next day, if she tolerates that, 15 minutes. So, it’s a stage process because of the risks that are there.
Tess: Yes.
Patrik: Mobilization might be a huge word. We’re not talking about big things in the beginning, we’re talking about little baby steps, but that’s how you start.
RECOMMENDED:
Tess: Yes. Well, they’re not going to do till she’s off the ICU ward. I’m assuming. What did you gather, if anything, about her breathing capability? Do you understand that there is still sticky phlegm?
Patrik: Yes, yes.
Tess: And the inability to cough all that up.
Patrik: Yeah. So part of the problem there is that she’s got no gag. That’s part of the problem. The physiotherapist is right when she says because she’s got no gag and she’s been ventilated for so long, that her secretions are sticky. And I think you did ask, “What are they going to do about it?” Actually can’t remember whether they said…
Tess: Nebulizer.
Patrik: Nebulizer, yes.
Tess: Nebulizer, and things they put in the nebulizer.
Patrik: That’s right.
Tess: But wasn’t specific with me.
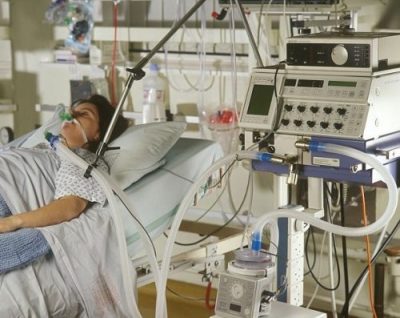
Patrik: Yeah. No, it would be a saline nebulizer. The other thing that you’ve got to check out, and that’s why I think a picture of the ventilator would still be valuable, whether she’s actually on a humidifier. I’m sure she is. I’m sure she is.
Tess: Humidifier. Well, I can just simply ask the question if I can’t get photographs, because I know that they’ve basically placed… if I were to… okay, right, sat facing Sarah on her right-hand side, they’ve got all of the ventilation equipment behind the stand sort of thing. It’s not that easy to actually… even if I were to be able to photograph it straight on, I wouldn’t really necessarily see all of the ins and outs anyway.
Patrik: Yeah, I hear you. Is it a small bed space? It is clumsy?
Tess: No. There is actually ample space going around the whole setup.
Patrik: Oh, okay. Okay.
Tess: Could you assist me, by telling me what simple questions could I put to the nurse to find out about these setups, the vent setup that’s being used?
Patrik: This is where there are probably no simple questions. A picture of the ventilator, you will get 10 numbers and then I can really explain it to you.
Tess: Okay.
Patrik: You ask one question and one answer will trigger five other questions.
Tess: Right. Okay, so it’s a complex matter.
Patrik: It is a complex matter.
Tess: Okay, so I’ll try and get photographs, okay. I’ll try and do that today, okay? I can’t promise anything-
Patrik: No, I get that.
Tess: … because it’s well awkward in there.
Patrik: I get that.
Tess: And there’s only a matter of days when she could actually be… now, when she goes to the ward, what kind of setup should I be expecting in that scenario?
Patrik: Yeah, that’s a great question. So from what I gather, if she goes to the ward, they can look after a tracheostomy. That’s at least what they said.
Tess: Yes.
Patrik: To a degree, I question that. It’s a very specialized skill to look after a tracheostomy. I argue you need to have at least a couple of years of ICU experience to everybody really proficient with a tracheostomy. And very few ward staff have that experience. Now, what you might find is that you might find that there is what’s called an ICU outreach service. Have you heard of that?
Tess: No.
Patrik: There might be an ICU outreach or an ICU liaison service. What that means is when someone goes from ICU to a ward with a tracheostomy, everyone knows the skill level on the ward is not as good as in ICU, whether it’s on a nursing level or on a medical level. And therefore, a lot of hospitals now have an ICU outreach service, where there’s an ICU outreach nurse or even an ICU outreach team consisting of a doctor and nurse, and they are keeping an eye for the tracheostomy patients on the ward. They come by once a shift, once a day, twice a day, something like that.
Tess: Right.
Suggested Links:
Patrik: So I would think they would have an ICU outreach service.
Tess: Okay. So, should I be putting the question-
Patrik: Absolutely.
Tess: … is it possible to liaise with them?
Patrik: Absolutely. And then the other thing you’ve got to look for is depending on how many tracheostomy patients are on that ward, let’s just assume she’s the only one. Okay, let’s just assume that’s the case. She should be in a bed space close to the nurses’ desk.
Tess: She should be in a bed space, yeah, very close-
Patrik: To the nurses’ desk.
Tess: Be in a bed space. Yeah, okay, got that.
Patrik: Right, because if the tracheostomy blocks, if the tracheostomy comes out, her life is at risk, so she needs to be somewhere where they can react quickly.
Tess: Yeah. React quickly. Okay.
Patrik: And obviously, as I mentioned before, they might disagree with that if you put that to them, but I argue anybody with a tracheostomy should only be looked after by nursing staff that has ICU experience.
Tess: Yes.
Patrik: And chances are if she’s going to the ward, not all nurses have ICU experience, probably very few of them, which is where the ICU outreach or liaison comes in again.
Tess: Okay. That’s invaluable. Thank you very much for that, because I can work on that and do my best to put my point across for Sarah’s sake in the situation and do the best on that front. Okay-
Patrik: Here is another important question, and for whatever reason, I didn’t think of it yesterday, but now it comes to me. So, we know the DNR (Do Not Resuscitate) situation. However, there is another situation that’s closely related but is not a DNR as such. So let’s just say, God forbid, she goes on the ward, she’s still got the tracheostomy. God forbid, she ends up with a pneumonia and in order to deal with the pneumonia, she needs to be ventilated again, and she needs to go on antibiotics and she needs to go back into ICU. Now, they might argue that she is not a candidate for going back into ICU. I do believe you need to clarify that before she’s leaving ICU.
Tess: Okay. Find out the intention were Sarah to have another lung infection-
Patrik: Yeah, no, look, it could be anything really. I mean, I’m just giving you an example.
Tess: You’ve gathered from what Rhea said, she said basically, “Sara won’t be a candidate for replacement lung.” I’m not even thinking that, they wouldn’t bother. They’re not going to bother.
Patrik: I wouldn’t say that, no, no, I wouldn’t say that. There are certain things that they wouldn’t bother, but I do believe going back into ICU for a few days to treat a pneumonia is something that I believe they would bother with, or at least you need to ask the question.
Tess: Okay. Okay. Thank you. I will ask that question.
Patrik: And this is where it’s so important that you have access to the medical records. So, did you remember she said something in that meeting where she said something along the lines of, “Oh, a few years ago, we didn’t even have to tell families when patients have a DNR.” Do you remember she’s saying that? I do.
Tess: Yes.
Patrik: Right.
Tess: Yes.
Patrik: Right. And I would argue, Tess, that when she leaves the ward, if you’re not pulling them up on it, they will document in the notes, she’s not for ICU readmission, and they wouldn’t even tell you.
Recommended:
Tess: When she goes to the ward, they wouldn’t even tell me if she had a DNR, is that what she said?
Patrik: No. The DNR we are clear of, and they had to tell you. What I am saying is, similar to the DNR though, once she’s going to a ward, they might document that she’s not for ICU admission.
Tess: Okay, I’ve got to find that out.
Patrik: No. You got to approach it in a different way, Tess. You don’t ask them, “What have you documented?” You state what you want.
Tess: Yes.
Patrik: You don’t ask them, “What did you document?” No, no. That puts them in control. You can’t put them in control.
Tess: Okay. So I’ve got to speak to Sharon today. I’ve got to put the request form in, the SAR, subject access request, and actually push this whole matter really hard.
Patrik: Yeah, you will. You will need to.
Tess: Okay.
Patrik: You will get them, but they will make it difficult for you.
Tess: What’s the likelihood, and I know that we don’t have a crystal ball, but what’s the likelihood, given that she’s got sticky secretions, that she goes to quickly contract another pneumonia in the ward?
Patrik: Look. Anyone that’s on a ventilator, anyone that has a tracheostomy is at a much higher risk of a pneumonia than anybody else, okay. A lot of it comes-
Tess: You’re saying there’s more chance, yeah.
Patrik: A lot of it comes down to nursing care, and that’s why I’m sort of saying what I said to you earlier, a tracheostomy should only be looked after by ICU nursing staff to avoid things like that.
Tess: Okay. Well, I appreciate that. That is a very important point. And I will ascertain, through the ICU outreach team, these matters. With regards to the medical records, I will push on that, and I’ll also do the best to get some shots within the situation today, if it’s appropriate. Okay, if I can get away with it. I tried before. I got a bit of footage of Sarah from the floor going up, where the ventilator is, equipment, yeah.
Patrik: Yeah.
Tess: Very small snippets, the video, and then a passing over of Sarah to showing the other side, a little bit of video, and that’s the extent of it. Whatever photographs I did take were absolutely ridiculously poor, so at that time, because I was really quite nervous as I was trying to do it, and the flash was on. And I was already up on the ventilator so it was really obvious what I was doing, so that put me off completely. I need to try and use Rey’s phone and do that today, if I can do it. Okay. I don’t know what else there is to say, Patrik, at the moment, other than…
Patrik: No, I think really, I guess, watch what they do, not what they say.
Tess: Yeah.
Patrik: Watch what they do, and make sure they do assess her when you’re there.
Tess: Yes. Okay, that means that they’ve got to be very vigilant giving me a good spot, say, two hours warning, or an hour warning before they go ahead and do the thing.
Patrik: Yeah. No, absolutely.
Tess: So I can be present.
Patrik: Absolutely.
Tess: Okay. Yeah, okay. Should I be telling the reception that? Should I be telling the doctor that?
Patrik: I think the more, the better because-
Tess: Okay.
Patrik: Yeah.
Tess: Okay. The doctors. Okay, thank you very much indeed, Patrik. Not just the fact that you’ve had a probably, very tiring day, a lot of effort on your part. You need to get some good rest, and I wish you well and maybe speak to you later on, what do you reckon?
Patrik: Yeah, look. I think you signed up for the four days, I can’t remember, I have to look-
Tess: It’s seven.
Patrik: Oh, okay. I’ll have to have a look. Yeah, no, sure, all good. All good. Yeah.
Tess: Yeah?
Patrik: Then we’ll talk next time.
Tess: Yes, okay. In the meantime Patrik, wishing you a good rest from all of us. Thank you very much indeed.
Suggested Links:
Patrik: It’s a pleasure. Thank you so much.
Tess: Okay.
Patrik: Thank you.
RECOMMENDED:
Tess: Thank you, Patrik.
Patrik: Bye.
Tess: Good night. Thank you, bye-bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!