Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
What will be My Sister’s Quality of Life After she Comes Off the Ventilator in ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED”, I am here with a live stream today, where I want to answer your questions if you have a loved one in intensive care. And this is one of the most commonly asked questions for families in intensive care and it’s a question that we get all time. And today’s live stream is about the 10 Things About ECMO You Didn’t Know in Intensive Care! (COVID and Non-COVID Related)! Live Stream!
10 Things About ECMO You Didn’t Know in Intensive Care! (COVID and Non-COVID Related)! Live Stream!
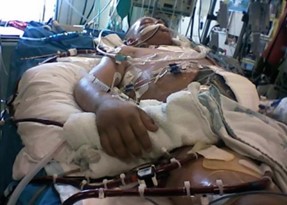
Welcome to another intensivecarehotline.com livestream. My name is Patrik Hutzel from intensivecarehotline.com. I’m a critical care nurse consultant, and also advocate, and consultant for families in intensive care. And I want to welcome you to this livestream today.
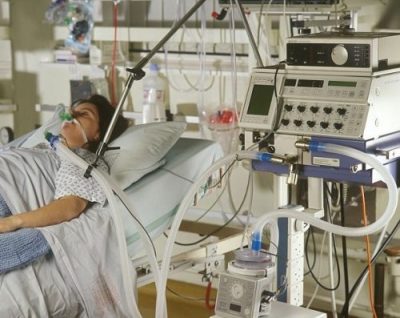
And today’s live stream is about, “10 things about ECMO (extracorporeal membrane oxygenation) in intensive care you didn’t know!” And you must know.
RECOMMENDED:
What makes me qualified to talk about this topic? As I mentioned, I am a critical care nurse by background. I have worked in intensive care and critical care for over 20 years in 3 different countries. Part of my career in intensive care/critical care involved being a nurse manager for over five years. And the topic today is about ECMO, and I’ve also looked after many ECMO patients in intensive care, and I’m therefore ECMO competent. I’ve worked in a big ECMO center for about 10 years. And that was part of my day-to-day work there. I have been professionally consulting and advocating for families all around the world for the last 8 years, for over 8 years now.
We’re also running an organization called Intensive Care At Home where we look after long-term intensive care patients at home. Some well worse in the area of intensive care and critical care. So, I know the acute side of things and I also know the follow-on or the less acute side of things, which is often Intensive Care At Home. So, I can combine both worlds and that is why I am qualified to talk about this topic today.
So, let’s dive right into the 10 things that you need to know about ECMO or that you didn’t know about ECMO, but you must know.
I would argue that before the COVID pandemic, very few people have known about ECMO. And I think it’s still a reasonably small number of the population that knows about ECMO. But obviously, with COVID being so prevalent, ECMO has become more center stage. And people that have been affected by COVID in intensive care, in particular, might have done some research about COVID. So, it’s certainly a very timely topic to talk about, and I want to talk about both options today, or both scenarios.
I want to talk about ECMO for non-COVID patients. I want to talk about ECMO for COVID patients.
The first thing that I want to talk about is there are two forms of ECMO. One is the VA ECMO , and one is VV ECMO. VA ECMO sense for venoarterial ECMO and it is basically used for heart failure. And VV ECMO is venovenous ECMO, and it is used for lung failure predominantly. Basically, ECMO can take over the function of the heart or the lung for a period of time, so that the heart and the lung can recover in case of lung failure. ECMO can also be used as a breach to a lung transplant. And VA ECMO can also be used after a heart transplant. VV ECMO can be used after a lung transplant as a bridge to recovery. So that’s in a nutshell, the two forms of ECMO during COVID.
If proning doesn’t work for COVID ARDS (acute respiratory distress syndrome), the next step might be ECMO. ECMO beds were in high demand pre-COVID and they’re now in even higher demand because people in ICU with proning just don’t seem to recover. And if they don’t recover, the next step should be ECMO.
The literature suggests that there is an age cutoff for ECMO patients. Some literature suggests 60 years of age, some literature suggests 65 years of age. I have seen patients as old as 67 or 69 going on ECMO. It all depends on the resources available. It depends on medical history, depends on negotiation skills. It depends on your bed and staff availability as well.
Prior to COVID, especially for lung failure, you would’ve started a patient on ECMO for lung failure. Again, probably for ARDS, pulmonary fibrosis, and bridge to a lung transplant. But at the moment, it looks like it’s predominantly for COVID ARDS.
So now the next question is how long can patients stay on ECMO? In the last 10 years pre-COVID, I’ve seen up to 3 weeks of patients staying on ECMO. We are talking to people all over the world, we have now seen patients being on ECMO for up to 6 or even 7 weeks. And that’s certainly pushing the boundaries. The risk of things going wrong, if someone is on ECMO for such a long time with blood clotting, with hemorrhage, is definitely there. Whilst it can save a life, the time that someone can stay on ECMO is certainly limited. And the longer someone stays on ECMO, even though it might be able to give patients time to recover, there are other things often going wrong. And the chances of survival often do go down the longer someone is on ECMO. But like with everything, there is always the exception to the rule. So that was number one is VA ECMO. Number two, VV ECMO.
Number three was timelines. I talked about the timelines, which is, I’ve seen up to three weeks. But at the moment, we’re just talking to a client in South Carolina. And they had their 35-year-old husband and brother on ECMO for almost 6 weeks for COVID ARDS and had a tracheostomy, and is now on their path to recovery, is now on their way out of ICU. And that is remarkable news. So, it can happen, but it certainly depends on a case-by-case basis.
Next, let’s look at some of the risks when someone is on ECMO.
One of the main risks is that patients on ECMO need heparin. Heparin is a blood thinner. And because blood is being extracted from the body, it goes through plastic tubes, goes through a filter, and that increases the risk of blood clots significantly. Therefore, heparin needs to be started. Heparin is a blood thinner, and it stops the blood from forming a thrombus or forming a clot. And if someone on ECMO ends up with a thrombus or a clot, they could end up with a stroke. They could end up with a pulmonary embolism and that could be lethal, really.
On the other end of the spectrum is that, if you are using too much heparin, the blood is too thin and then you could end up with significant bleeding in other major organs, including the brain. And that could cause a lethal situation as well. It could cause a stroke, a hemorrhagic stroke. It could cause bleeding in other organs, especially what I’ve seen GI (gastrointestinal) bleed, like bleed in the stomach or in the intestines. And that could cause significant complications as well. So, it’s a very fine line between managing the dose of the heparin so that it’s therapeutic and not causing any harm on either side of the spectrum.
Next, most patients when they do go on ECMO are on a ventilator, especially if they are in heart failure or if they are in lung failure. I have seen on the other occasion where patients don’t need to be on a ventilator, and they can be on ECMO awake. It’s probably only 1 in maybe 20 patients that I’ve seen that can be awake while they’re on ECMO and not on a ventilator. The aim basically is that, especially with lung failure, to give the lungs a rest. Minimal ventilation even though patients are still intubated or have a tracheostomy. Most of the time they’re intubated. I’ll come to that in a minute while they’re intubated and not necessarily have a trach or a tracheostomy.
So, it’s to give the lungs a rest, it’s to give the heart a rest. When patients go on ECMO for heart failure, it’s often after a cardiac arrest, after a heart attack. It can be for cardiomyopathy often, which is one of the other factors when people go on VA ECMO for heart failure. And often, it can be used, or sometimes it can be used as a bridge to a heart transplant as well or VA ECMO. But then it also often is a bridge VA ECMO for heart failure.
Next step is a VAD (ventricular assist device) machine, either for the left or for the right ventricle of the heart, sometimes both. And then it can be used as a bridge for a heart transplant. Often that’s supported by a dobutamine infusion or by a milrinone infusion and patients even can go home while they’re waiting for a heart transplant.
So, I’m jumping a bit all over the place here. But as you can see, it’s a very complex area, and many things need to come together here to make things work.
Next, if someone is on a ventilator with a breathing tube or an endotracheal tube, either for VA ECMO or for VV ECMO. One of the questions that we’re getting in those situations is, can patients have a tracheostomy? Should they have a tracheostomy if they are on ECMO for either heart or for lung failure?
So, the answer is that it depends. It depends on many circumstances and many details. So, let’s just break this down a bit more. So, if someone is on ECMO for heart failure, they have a breathing tube, they are in an induced coma, and they are on heparin, which is the blood thinner that I mentioned earlier. Can they have a tracheostomy? The risk is fairly high, just simply because of the heparin. Because if you do a surgical procedure, which is what a tracheostomy is, the risk of bleeding is significant. I.e., ECMO often prolongs the need to be in an induced coma because the tracheostomy sometimes can’t be done while they’re on ECMO.
If someone is on ECMO for lung failure, the same applies. That on heparin infusion, the risk of doing a tracheostomy is very high. The risk for bleeding is very high. Plus, if someone is on VV ECMO, often their ventilation supports are on a 100% of FiO2 (concentration of oxygen that the patient inhales). They’re often on high PEEP levels, which is then a contraindication for a tracheostomy as well. So, as you can see, it’s not straightforward, or very rarely is it straightforward in intensive care to make these things happen.
Suggested Links:
Next, one of the major complications that I already mentioned is the stroke either because you’re not giving too much heparin. And then there’s the risk of a pulmonary embolus or a stroke. Or if you’re giving too much heparin, there is the risk of a hemorrhagic stroke or a major bleed. And that is definitely one of the major complications if someone is on ECMO.
Next, I want to quickly talk, without getting too technical here. But I do believe it’s important for you to understand that when someone is on ECMO. Again, doesn’t matter whether it’s VV ECMO or VA ECMO, they’re put on a flow in order to replace the gas exchange that the ECMO machine is doing. So, it should be 7 mls per kilo and that should be the flow in liters per minute. So, you know your loved one’s weight and then you can look up what the flow is.
I also want to encourage you to type in your questions into the chat pad if you have any. Your questions and comments are very welcome on the chat pad. And then I can get to them.
Also, I want to quickly talk about the principle of the ECMO machine. Basically, what it does is it is similar to when we breathe out in our lungs. We inhale oxygen and we exhale carbon dioxide. And the ECMO machine is doing that for a critically ill patient. Oxygen is put into the ECMO machine which is where the gas exchange is taking place and carbon dioxide is being removed. Sometimes when the ECMO cannulas are being inserted, the ICU team might start with smaller cannulas. And if then the flows can’t be achieved, the flows are too low and you can’t put them any higher through those small cannulas, sometimes a high flow cannula is being inserted as well in order to achieve higher flows.
I talked about blood clots already in terms of one of the main risks. But being on ECMO is that blood clots may form and therefore people might end up with a thrombosis, that could lead to a pulmonary embolus. Which could lead to a cardiac arrest, or it could lead to an ischemic stroke. Especially when someone is on VA ECMO for heart failure. They are often being weaned off through a weaning study. What often happens is, when someone is on VA ECMO for heart failure, they’re often being started on inotropes or vasopressors such as milrinone, dobutamine, but also norepinephrine, noradrenaline, epinephrine, sometimes vasopressin, depending on the severity. They need regular ultrasounds of the heart to determine ejection fraction.
Ejection fraction is the contractility of the heart. It’s often very low when people go on ECMO for heart failure and then over time as hopefully the heart recovers. Those inotropes and vasopressors can be weaned off. And hopefully then the heart can start to pump again, and contract again with a healthier disposition. And that can then be determined again, in ultrasound or in a transesophageal echocardiogram where the ejection fraction can be determined.
Now, just want to quickly go to Kimberly’s question, “So, the ECMO machine and the ventilator are two different things?” Absolutely. Absolutely two separate things. However, one can tie in with the other. As I mentioned, I don’t know whether you’ve heard what I said in the beginning that most patients on ECMO are also on a ventilator. There is an exception to the rule. Some patients on ECMO can be off the ventilator, but that’s the exception to the rule.
So, I talked about weaning studies, especially for VA ECMO patients for heart failure. That is one of the ways to wean someone off ECMO. Flows will be reduced, hopefully, inotropes and vasopressors will be reduced. And ejection fraction is going to improve. Contractility is going to improve and then you can wean someone or take someone off the ECMO completely.
For VV ECMO patients, you can still reduce the flow. Hopefully also reduce the ventilator settings and then check your arterial blood gases, similar to VA-ECMO as well. You need to check arterial blood gases. You need to do chest X-rays. You need to see whether flows can be reduced. And the patient can breathe more and more themselves, or whether the ventilator can take over the function of the ECMO with a chance of being weaned off the ventilator. So that is in a very nutshell how you wean someone off VV ECMO. Reducing the flow, increasing ventilation support, and then get back on the ventilator, and remove ECMO. But the goal still needs to be then to wean off the ventilator.
And, the next step then often is once ECMO is removed, and heparin is removed as well. The next step then often is, if weaning off the ventilator can’t be achieved quickly, to do a tracheostomy. That should be the next step.
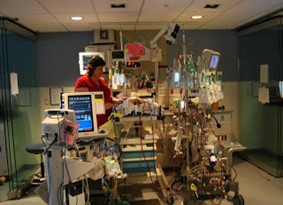
Brenan, you are asking, “What should be considered when reducing sedation paralytics and turning down ventilator?” So, Brenan, the first thing that needs to be removed is the paralytics. You can’t paralyze someone without sedation. Imagine someone is paralyzing you medically and you’re not sedated. You would be conscious while this is happening.
So, the first step is always sedation, and then it’s paralytics, and it’s the other way around. Remove paralytics and then reduce sedation. Only then can you reduce ventilation support. Because if someone is paralyzed medically, they can’t breathe at all. The muscles stop. Okay, that’s the cause of action there.
And then you’re asking, “Most COVID patients have a hard time during this process, right? How do we make it easier?” It’s a very good point. COVID is, it’s terrible, what’s happening and it’s obviously a worldwide pandemic. And they have a hard time during this process. We are talking to so many people who have loved ones in ICU with COVID and basically, what we are seeing across the board is, they start off with COVID pneumonia, and they often go into COVID ARDS, then they start getting proned. And if proning doesn’t work, then they’ll be put on ECMO.
So, patients with COVID are in ICU for long, long periods of time. And the after effects will be massive from that. Either patients don’t survive or if they do survive, they will be in for a long recovery with all the side effects of a prolonged induced coma. I pretty much believe it’s not even known yet. If COVID patients survive ICU, what their quality of life will be, like in 6 months’ time, in 6 years’ time, there’ll be new territory charted there.
Okay, let’s move along. When someone is on ECMO, again whether on VV ECMO or VA ECMO, they often need inotropes and vasopressors. For the heart failure, ECMO patients, they almost always need vasopressors or inotropes. But also, the VV ECMO patients, the ones with lung failure also often need inotropes or vasopressors. Again, that’s considered life support. You got to picture this, when someone is on ECMO, 300, 350 mls of blood are always out of the body. That reduces blood pressure and one way to manage low blood pressure is with a vasopressor or inotropes. Again, those drugs are considered life support.
Another thing that’s happening when patients are on ECMO is because of the heparin. And because of blood being extracted through an extracorporeal machine, blood is being lost. Hemoglobin is going down. Red blood cells are going down. And patients often need a blood transfusion in the process as well.
As I mentioned to you, I have seen some patients that are awake on ECMO. Doesn’t happen very often, but it does. Which means they’re not on a ventilator because the ECMO machine can definitely take over the function of the ventilator or the heart for a period of time. I.e., they don’t necessarily need the ventilator, but it happens very rarely.
Here is one of the biggest risks when someone is awake on ECMO. So, question for everyone. What happens if someone is awake on ECMO? ECMO doesn’t work. There is no heart transplant available, there’s no lung transplant available. What happens next? You’re going to withdraw ECMO at some point on an awake patient and they’re going to die. So that raises huge ethical and moral questions in, how do you approach palliative care in a situation like that? But that’s not our discussion today, but I do want to throw it in that awake ECMO is an option.
But the question is, what does that look like on the other end, in case ECMO doesn’t work and no heart transplant or no lung transplant is available? I’ll give you an example. I have seen, I remember clearly a few years ago, I looked after a patient in ICU. Would’ve been a patient in his late 50s, who came in with, I believe it was pulmonary fibrosis at that time. He was put on ECMO pretty quickly. He was put on lung transplant at least the very same day. He wasn’t an awake ECMO patient. He didn’t need intubation and he had a lung transplant within 48 hours. That was an amazing story, but it doesn’t happen very often.
Recommended:
The question would’ve been, what if he had gone on awake ECMO and the lung would not have become available? What would’ve happened then? Massive, massive moral and ethical dilemmas here.
Then, I want to talk about the availability of ECMO. So, when we consult clients at the moment, all over the world about ECMO, we are finding the following, they have a loved one in intensive care with COVID ARDS, they are being proned. And when they’re being proned, if it doesn’t work, ICUs often come back to the families and say, “Hey, proning isn’t working. We have to stop treatment and we have to let the loved one die.” They’re not even mentioning to families that ECMO might be an option. So then if they contact us, we say, “Okay, has ECMO been considered?”. And they often say, “Well, what’s ECMO?”, they have no idea. ICUs are not transparent. They’re not telling them that ECMO might be an option. And what we also find is sometimes even they have ECMO available in the very ICU that people are in.
Now don’t get me wrong. Most ICUs don’t have ECMO available. So, the patients often have to go to an ECMO center. And those ECMO centers are often available in big metropolitan ICUs. Of course, in America, Canada, Australia, U.K., but beds and resources for ECMO are still limited. Not every intensive care nurse can look after ECMO. Not every intensive care doctor is specialized in ECMO. Intensive care is a specialized area and ECMO is a subspecialty.
So, I remember when I first started looking after ECMO, you need to do a two-day course. And then you need to work on the supervision, to begin with. It’s not a straightforward process. So, intensive care is highly specialized. ECMO in intensive care is again, super-specialized and it takes time. And therefore, the availability of ECMO beds and the availability of ECMO staff is definitely limited. And such as the availability of intensive care beds. So, you can see why ECMO is such a scarce resource, especially in this climate. ECMO beds were in short supply before the pandemic and now with COVID patients needing ECMO, you can imagine what that looks like in getting a patient on ECMO during this COVID pandemic.
But you got to ask the question. If you type into Google, ECMO centers. You’ll find a link to a website pretty much on top of Google somewhere, where you get all ECMO centers around the world. And don’t be shy of contacting them. If you feel like you need ECMO for your loved one and you want to make some inquiries.
But the bottom line is this, ECMO beds are in short supply. Simply because it takes a lot of time to train doctors, nurses, and everybody else involved in the process. And ECMO machines are obviously very important. They need to be maintained. I also know of some situations, it hasn’t happened in my lifetime very often, but I have seen. Normally, it’s a 1:1 nurse-to-patient ratio for an ICU patient, including ECMO. But I have seen some patients needing two nurses during a shift because there are just so many things going on at the same time that one nurse simply can’t cope with the workload.
And last but not least, I think I’ve gone way over 10 points now, but doesn’t matter. Often ECMO patients also need dialysis because the kidneys are failing. Many ECMO patients go into septic shock, and when they’re going to septic shock, they often end up with kidney failure. And then they need to go on dialysis, which again is another complicating factor for an already complex patient. And again, just increases the risk of bleeding or clots. Increases the need for heparin, which then increases the need for bleeds on the other end. It also increases the need often for blood transfusions. It increases the need for inotropes or vasopressors.
So, it’s a very complex situation when someone is on ECMO. A lot of tests need to be done every day. Blood tests, six-hourly. Chest X-rays need to be done. As I mentioned, ultrasounds need to be done. Sometimes CT scans need to be done and I can tell you from experience, it’s a massive undertaking. Taking someone on an ECMO machine to a CT scanner, it can be done. If an intensive care unit is telling you can’t take someone to a CT scan on ECMO, that’s not true. Done it plenty of times, but it takes a lot of work. It’s a lot of effort, you need almost like seven or eight people to get people ready and also then for the transport.
So, those are my 10 things. I think I’ve listed actually at least 12 or 13 that you need to know about ECMO. If you do have any questions, please type them into the chat pad so I can answer them.
Suggested Links:
- Quick tip for families in ICU: When should ECMO be initiated for COVID/ARDS & proning isn’t working?

In the meantime, if you feel like there’s value in this video, I would appreciate if you can give it a like. If you can give it a thumbs-up, and if you can subscribe to my YouTube channel. For families in intensive care, you are more than welcome to leave a comment below of what your insights are, what your comments are, what other videos you want to see, and click the notification bell.
If you do have a loved one in intensive care, I encourage you to watch some of my other videos. I encourage you to go to my website, intensivecarehotline.com. Call us on one of the numbers on the top of the website. Or simply send us an email to [email protected].
The biggest challenge for families in intensive care is simply that they don’t know what they don’t know. They don’t know what to look for. They don’t know what questions to ask. They don’t know their rights and they don’t know how to manage doctors and nurses in intensive care. And that’s one of the biggest challenges.
Brenan, can I do a video on COVID patients in ICU? I’ve done plenty of videos about COVID patients in ICU. I would’ve done one in the last three weeks. If you look through my livestreams, you will find at least two videos about COVID patients in ICU, about treatment options.
Brenan, do you have a family member in intensive care on COVID? Is that your situation? Or are you a health professional and you’re studying the subject? What’s your situation, Brenan? So, you have a loved one in intensive care with COVID? Yeah. There are plenty of resources on my YouTube channel and also on the website. We publish what’s on the YouTube channel, and also on our website.
I can also only encourage you to contact me directly either again, through my email [email protected] or just call me on one of the numbers on the top of our website at intensivecarehotline.com. If I don’t answer straight away, leave a message, and I will get back to you in due course.
Recommended:
I hope that helps. I really want to thank you for coming on to the livestream. I want to thank you for your support, and for your questions. I will wrap this up in a minute unless you have another question, I’m happy to stay on for a few more minutes. If you have another question.
Again, I can only encourage you. If you have a loved one in intensive care, go to our website intensivecarehotline.com and either call us on one of the numbers on the top of our website, or send an email to [email protected]. You can also leave a comment below this video, and I will get back to you on the chat pad.
I will do another livestream next Saturday night. I will see you all then.
RECOMMENDED:
Look out in the next few days, I will announce the topic for next Saturday and I’ll talk to you then. Thank you so much for your support and for coming onto this livestream. I hope you and your families are well.
Take care for now.
This is Patrik Hutzel from intensivecarehotline.com and I will talk to you in a few days.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!