Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
My Dad Needs Dialysis in Intensive Care After Sepsis! What are His Chances of Survival? Live Stream!
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tess, as part of my 1:1 consulting and advocacy. Tess’s daughter is ventilator-dependent and the ICU team is limiting their treatment. Tess is asking how can she stand against their decision.
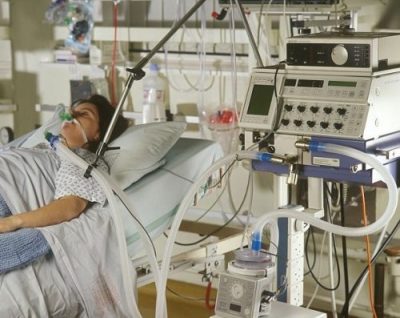
The ICU Team is Limiting Their Treatment to My Ventilated Daughter. How Can I Stand Against Their Decision?

“You can also check out previous 1:1 consulting and advocacy sessions with me and Tess/Romeo here.”
Patrik: Hi, Tess.
Tess: Hi, Patrik.
Patrik: How’s your daughter?
Tess: They say that Sarah’s been pretty unwell. They say that they wanted to put her in the palliative care route and we refused that.
Patrik: Sorry. Say that again, please. They’re going to…
Tess: They said that they want to put her in the palliative care and I’ve refused that.
RECOMMENDED:
Patrik: Yes, good.
Tess: The doctor and the director of the hyper-acute rehabilitation unit, they’re of the opinion that Sarah should be placed on that pathway, and I’m working with Romeo and Rey. We’re in complete opposition to that. And all in all, we’ve just explained in short, being with Sarah for the past three days with very little sleep, about half an hour myself. And Sarah is really not very well at the moment, but she’s trying really hard. Her saturation has been good at oxygen of 28% on five liters. 100 saturation. She’s been maintaining at times, 98, 99, 100. Currently, she’s at 100. And 138 heart rate. And she used to be clearing 152, one occasion 160.
Tess: They have given her diazepamThey actually refused to give the clonazepam because they don’t believe that she’s going to… she might aspirate that, anything going into her stomach. She had a PEG (Percutaneous Endoscopic Gastrostomy) tube on her stomach and they check the gastric contents. And potentially, there was blood there she’d aspirated, 500 ml thereabouts of feed that virtually sat on the stomach and they took that off. They’re saying that her lung tissues isn’t that great, but they’re holding out hope. And they’ve stopped feeding her. They’re refusing to give her anything since 10 o’clock, the day before yesterday.
Patrik: Why would they refuse feeding her? Have they given you any…
Tess: Excuse me?
Patrik: Why are they refusing feeding her?
Tess: Because they say she just might aspirate the feed.
Patrik: Okay. Have they offered TPN (Total Parenteral Nutrition) instead? Do you know what TPN is?
Tess: No.
Patrik: TPN is intravenous feeds, because basically what you are telling me, correct me if I’m wrong here, you are basically telling me they are potentially starving her to death.
Tess: Well, that’s what we suspect, and I’m very concerned. They’ve got her on a glucose saline drip.
Patrik: Right. That’s not enough.
Tess: They’ve been giving her insulin. Yes.
Patrik: That’s not enough.
Tess: Excuse me?
Patrik: That’s not enough, that’s not enough.
Tess: No, of course it’s not. And she’s underweight despite giving it anyway.
Patrik: And how long has that been going on?
Tess: About a couple of days.
Patrik: Couple of days, okay.
Tess: And they’re going to be reviewing it this morning, the doctors. They came to the bedside yesterday with very good doctor, who has been the next consultant, neurological various other places, and is basically a sort of floating member of staff, and actually not on the staff here having a resistance to our side of the situation. There’s no way I can get, currently, a power of attorney. There’s no way I can get, at short notice, a welfare protection order because the process is complicated and it will take time.
Tess: These people I’ve stood up to and said that in order of five others who’d just come to the bedside yesterday, and that doctor was just completely indiscreet, saying that Sarah may potentially die. I’m sat in holding her hand. And she’s very much conscious and aware of my presence. She’s tracking, she’s discriminating, she’s localizing. She’s watching intently and listening.
Patrik: Right, okay.
Tess: And they’re not going to send her back into palliative care which was completely discreet as well.
Patrik: Hang on, hang on. Just let me clarify this. You are saying they are going to send her back to intensive care, or they aren’t?
Tess: No, they’re not going to take her to ICU. They’ve refused to do that.
Patrik: They refused to do that, okay. Okay.
Suggested Links:
- Quick tip for families in ICU: What’s the difference between palliative care and hospice?
- Aspiration Pneumonia in intensive care! Live stream!
Tess: That’s their decision.
Patrik: Okay, I see.
Tess: With the radiologist-
Patrik: Okay, I see.
Tess: They checked out the CT (Computed Tomography) scans of Sarah’s lung. And they wanted to give her morphine and they want to literally make it look like she’s asleep and basically euthanize her-
Patrik: Yeah, euthanize.
Tess: And I don’t want that to happen.
Patrik: Of course not, of course not. Okay. Where is she at the moment? Still in the same place?
Tess: She’s literally in the room with us on her own. She’s being attended to day and night by the nurses.
Patrik: Yeah, I get that, but what I’m asking is… Tess, what I’m asking is, is she still in the same location to when we last spoke?
Tess: Yes.
Patrik: Okay.
Tess: When we went to the court and then she was released in the ICU and down into the ward, and she spent four days there, and then they’ve basically moved in on the situation with their determinations, which I don’t agree because Keppra and sodium valproate, I argued with the doctor, that they could potentially be causing her to stir up in agitation. Can you hear me?
Patrik: I can hear you. I can hear you.
Tess: So it was that because what they did was they actually refused the clonazepam, which goes hand-in-hand apparently, with the Keppra and the sodium valproate. They refused that by mouth, the drip and so effectively, that’s sort of making Sarah awake for the past nights very, very stressful for her. She was very high. She didn’t sleep. She’s been that condition and then they postponed the Keppra and the sodium valproate by about a matter of two or three hours, yesterday, early hours in the morning. So they’ve done it as like a deliberate mistake or a mistake unintentionally by accident, but the point is that they are making things off and they’re causing very much undue stress for her. And she’s frightened for her life as we speak.
Patrik: I can imagine. I can imagine. So Tess, what’s the issue with power of attorney?
Tess: I tried to open up about that. She had virtually shown some signs of concern.
Patrik: Right.
Tess: And we have got potentially somebody who could come to visit but it’s extremely difficult to determine with the myoclonic twitching, exactly whether Sarah actually is in a position to… they postponed the joint assessment on Thursday because Sarah was not in any fit shape. And that would have maybe actually given Sarah an opportunity to prove her responses to them. But because she’s so tired and because they’ve basically, I believe, deliberately turned these around so that it makes it somewhat difficult for Sarah to write, they’ve really been poor, in my opinion.
Patrik: Yeah, I hear you. I hear you.
Tess: In a room of literally, with Sarah trying to give them as much support as possible.
Patrik: Yeah. So when I got your message this morning my time, didn’t you mention something about tachycardia as well?
Tess: Yeah. It’s tachycardia. It starts between about 130 and 150 at times. I’m holding her hand and it’s 99 saturation with around 121 heart rate.
Patrik: Right.
Tess: 130.
Patrik: Does she have an infection?
Tess: No, she doesn’t. I’ve been told they haven’t been able to identify infection.
Patrik: Right, okay.
Tess: She hasn’t got any infection. They say there’s chronic lung damage and because there’s ulceration and they’re basically covering themselves for whatever the potential neglect that could have occurred over these past four months, making out that Sarah’s at fault, and it isn’t her fault.
Patrik: Right.
Tess: You get a tracheostomy so you save your life and for all intents and purposes, I was under the assumption that was an inflated port, that there shouldn’t be instances of potential aspiration or anything what might have caused Sarah harm. And at the end, they’re basically saying there’s been no new indications. I would argue rightly so, instances whereas he’s saying, the doctor is saying in front of others that there’s been no new instances, and I wholeheartedly agree, especially on the desaturation because he’s not even getting that right. He’s saying it’s saturated on a regular basis and has actually been able to contradict in front of others, and he also said what was actually effect of… “Well, we might as well just reduce the Keppra.” Stop the valproate and Keppra. We know full well that would be extremely detrimental for her. And then when I brought that up in front of the other doctors, he sort of looked at them and said, “No, that’s not true.” But obviously, I’m recording.
Recommended:
Patrik: Right. Okay.
Tess: And Romeo says we can prove it. He’s alienated and I appealed for him to be as good, in a friendly manner as they manage possible, but really the way he was basically talking about Sarah was completely inappropriate, and he doesn’t care about everything he said, the first steps. So what was the point in trying to get her into rehabilitation in the first instance if he wasn’t going to give his full and wholehearted support of the process?
Patrik: Right. Okay. So have you mentioned that to them, that from your perspective, they’re trying to euthanize her? Have you mentioned that to them?
Tess: Say that again.
Patrik: Have you mentioned to them that if they will be giving her morphine and other sedatives, that they would, from your perspective, would euthanize her? Have you mentioned that to them?
Tess: What’s that last word, use of what?
Patrik: Euthanasia.
Tess: Yes. Yeah, exactly.
Patrik: Okay.
Tess: I’ve said that repeatedly.
Patrik: Yeah, have you mentioned that to them?
Tess: They said that’s illegal and that wouldn’t be the case, no. But they’re doing it anyway.
Patrik: Yeah, sure. Sure, okay. So I would do the following if I was you at the moment. I would send an email to the hospital administration as a matter of urgency.
Tess: Send an email as a matter of urgency to the hospital administration, yeah.
Patrik: Yep, absolutely. To hospital administration. And share your concerns, obviously, that they’re starving her and that they want to give her morphine, midazolam and that they want to kill her, and that you think this is illegal and that you would pursue a murder charge.
Tess: Yes.
Patrik: And by the same token, I would, if I was you, I would seek legal advice as a matter of urgency.
Tess: Right. We need to seek legal advice as a matter of urgency because we need to write to the administration of the hospital saying that effectively, they’re trying to murder Sarah.
Patrik: You need to call them out on euthanasia or murder, or both. You need to start using stronger language. But if they are going to-
Tess: Then wait for the feedback on there, wouldn’t it?
Patrik: But if you are-
Tess: Let me pass you to Rey.
Suggested Links:
Rey: Hello Patrik. The point about… Can you hear me all right?
Patrik: Yes. Who is this speaking? Who is this speaking?
Rey: Rey is speaking.
Patrik: Okay. And you are… And what’s your relation?
RECOMMENDED:
Rey: I’m the partner.
Patrik: Okay, okay. Okay, sorry. Yeah, okay.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!