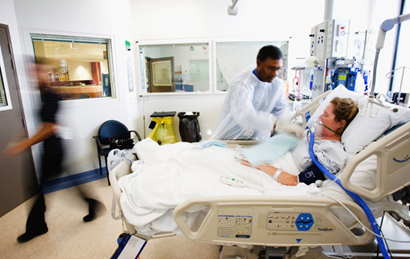
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tess, as part of my 1:1 consulting and advocacy. Tess’s daughter is with a tracheostomy in the ICU. Tess is asking how can they prevent their daughter to be on a DNR (Do Not Resuscitate) status in the ICU.
How Can We Prevent Our Daughter to be on a DNR (Do Not Resuscitate) Status in the ICU?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Tess/Romeo here.”
Patrik: Have you seen her be mobilized at all?
Tess: She was mobilized into a chair, and they thought she could only bear for 15 minutes, but apparently, the timescale change, varies from person to person I spoke to, from the nurse to another nurse, but basically, about an hour she was able to sit upright, was recently, within the past week they did that.
Patrik: Okay. Can I ask, so there are no visitation limitations because of COVID, are there?
Tess: I don’t know about the ICU specifically, but the person who is really, really like full on clinically a well-educated individual, she said quite clearly that she didn’t think it was a good idea necessarily to go up there, and she wasn’t suggesting I see her, even though I want to see her. And she wouldn’t be in charge of that necessarily anyway. All they’re in charge of at this point is they use the ward, the physiotherapy ward, and so she’s sort of liaising with the ICU to check on her intermittently.
RECOMMENDED:
Tess: But she did backtrack after Romeo pushed. She did backtrack. She was going to just basically leave her on the ward, and if it didn’t work out, she could potentially die. But she backtracked, and now she’s in a room to himself, not on a bay, which is more scary. She’s in a room on himself being on one to one with a nurse.
Tess: Her blood sugars are all right, and coming back to what I found out. Arterial blood gases were fine, I asked about the PH, PCO2 (partial pressure of carbon dioxide) and the PO2 (partial pressure of oxygen). There’s a little bit of differentiation there. But they said basically is all right. There’s no fluid on his lungs at that point. She’s on the same antibiotic that she was given when she was originally in the ICU for pneumonia. She’s on the same feeds. She hasn’t had a bowel movement as at the point of my speaking. I don’t know what that’s going … she’s on Tresiba-
Patrik: She’s on what?
Tess: Tresiba. Insulin.
Patrik: Okay.
Tess: IV insulin, and they’re checking it every hour.
Patrik: When you say she’s on IV insulin, that must be new. That must be just ICU specific.
Tess: Yes, it is, to ensure that she’s stable.
Patrik: What are they doing with the pneumonia? Is she getting IV antibiotics?
Tess: Yes, she must be, because she’s got an IV, hasn’t she. That’s what I basically told them, she’s on antibiotics for that, and it’s Actrapid, rather.
Patrik: Actrapid is insulin.
Tess: Okay, serves me I’ve got it written down. Tazocin.
Patrik: Tazocin, that sounds like an IV (intravenous) product. That makes sense.
Patrik: All right, and so what’s your biggest challenge at the moment? You would like to take the DNR (do not resuscitate) off of course.
Tess: Of course, because we want Sarah to survive this. She’s a miracle in her own way to survive not only a heart attack, all that she’s endured already. They kept her stable up until this point, and things have gone a bit haywire, but obviously I understand … she anticipated that they’re giving antibiotics and all that because people losing, they can destabilize. Well, I appreciate that that’s a good possibility that that can happen as well, and it would have been agitating moving, but I did try to calm Sarah with what I had to say to her the night before.
Suggested links:
Tess: She’s on a ventilator, but then all the tubing is attached to the tracheostomy. And the sugars are controlled.
Patrik: Of course.
Tess: And she’s relatively okay, those were her words at the time that I spoke this morning.
Patrik: She’s not on any sedation?
Tess: No, she’s not.
Patrik: Okay. Let’s just quickly look at his Glasgow Coma scale. Just give me one second please, because I think that’s really important, just bear with me. Is she opening eyes spontaneously?
Tess: Yes, she’s opened eyes to touch.
Patrik: Okay, if you ask her to squeeze your hands, would she do that?
Tess: I haven’t been able to determine readily because of my chronic twitching is significant enough to not be able to fairly discern whether she’s actually trying to indicate … but yes, the contractions have become quite strong in her hands. So, I can’t give you an honest answer on that one, I don’t know.
Patrik: Well look, if you grabbed her finger, and you would ask her, “Can you squeeze my fingers or my hands?” you would notice if she was doing that on purpose or not.
Tess: Yes, but at the time when I was with her I was very intent just to basically try to give her a pep talk and to try and bolster her morale, and my intent was not to do a Glasgow Coma assessment. I was rubbing her forearm gently, and stroking forearm, and occasionally, occasionally touching her forehead, and stroking her head in conversation with her. So my assessment was how very focused she was on me as she was tracking, I didn’t take into consideration the whole matter of her squeezing it.
Patrik: Right, okay. Maybe when you go back there, maybe you can almost integrate that in your routine. I think it’s a really good indicator of whether she can hear you or not. Well, she can probably hear you … no, no, she can probably hear you, but whether she can more or less connect the dots sort of thing.
Tess: This woman, which the doctor, the consultant, she used the word vegetative in conversation with me. Like I don’t know whether she was doing that to be punitive, but they haven’t even given her opportunity to be assessed. She was a lot lighter mannered to me today, talking to me as I was, being straightforward with her and asking certain questions and being civil with her.
Tess: Now I had made it very clear that Sarah is in a memory conscious state and she is aware and she is tracking. Not only that, the doctor in the morning confirmed that to me. And she said, “That’s good that I can … it’s good that I know that I can speak to her, because I wasn’t quite sure.” Get it?
Patrik: Yeah. But if they are using the words vegetative, that’s why I think the Glasgow Coma scale is very important for you to make your own assessment rather than her using words that may or may not be appropriate. The Glasgow Coma scale is a really good tool to get away from any words and rather do an objective measure. Can I just ask, are you under the impression that … I know she can’t talk because she’s got the tracheostomy. But do you think she’s trying to talk?
Suggested Links:
Tess: No, but what I have noticed in my presence, not necessarily, but her eyes are more inclined to sporadically open wider and then close. We’re not talking about what you would see in a coma state individual. We’re talking like expressive. Her eyes are really from going from a sort of in like a half position and looking somewhat sluggish, her eyes were very intent, like a normal person would look at you, a little bit of twitching going around the eyes muscles, which is understandable because of the myoclonic, but she actually would open her eyes considerably. I would see that as tend to indicate that she’s trying to communicate, because it was sporadic.
Tess: But then it’s really difficult to know. All I know is that for somebody in her condition, to hold her gaze on me for that long, and be able to openly look at other areas of the room and be aware of her environment as I believe she is, I believe that’s remarkable to me. Yeah?
Patrik: Sure.
Tess: Well I think she’s really thin still. I don’t think she’s gained any weight but the feed is pretty high. I think it was 75 mL the last time I found out.
Patrik: Right, she needs that.
Tess: That has to be taken into account. That’s what she said. The Myoclonic, because they take up a lot of energy in the body, they need to make sure that she’s relaxed and that she’s not really having issues and twitching, and she did say to me, “We are expert. We are expert here in how to handle these methods.”
Tess: And I was asking about the sodium bitrate, and I stated clearly that my suspicion was that after that was introduced, that she became a little bit more dejected, a little bit sadder in my opinion, slightly less alert, and that concerned me, and then I looked into the actual side effects of sodium bitrate and one of them obviously, in the capsule, in the combination they haven’t increased it, he’s on 1.5 grams twice a day on the sodium bitrate, and I said what about hers liver toxicity? She didn’t seem concerned about that. She said that we’re going into around it, and then she explained, and slightly reluctantly explained to me about suicidal ideation, because I mentioned that as a side effect, and depression, and she then went on to explain to me how that mechanism works with the brain.
Tess: So she was kind enough to clarify that point, and in her opinion it’s unlikely that that would happen because she’s not depressed, and because she wasn’t depressed before all of this matter happened.
Patrik: Okay, I just sent you the Glasgow Coma scale in Skype. I do believe it’s-
Tess: I have it before, yes. Thank you.
Patrik: I’m very happy to talk to the doctors if you wanted me to do that. And we can argue on the DNR (do not resuscitate). So just remind me, on her last stint in ICU, they wanted a DNR as well, didn’t they, and just remind me, what happened then?
Tess: Okay, so then she has to take the DNR, and the last thing before she was moved from the ICU to ward 4 basically was the DNR was intact. We insisted that the DNR be taken off, and you know there was a whiteboard in front of her, within the room that she was separated off from everybody else, she was in a room on her own in close proximity to the nurses, there was no DNR written on there. Just the bowel movement, the rate of saturation that they wanted to keep stable at 94, and then the nurse and the doctor, doctor’s name, but no mention of DNR.
Patrik: I thought we had discussions then, but I might be wrong. I might be wrong. Yeah, no that’s good. That’s good that she didn’t have it last time, and she shouldn’t have it now.
Tess: No, she shouldn’t. But making quality decision at this woman’s taking I’m assuming with the belief of what they think is best for her best interests, but I don’t agree with that at all.
Patrik: Or it’s in the best interests of the hospital, but this is a different ICU than last time, isn’t it?
Recommended articles:
Tess: Yes, completely different. It’s like only two floors above her where she’s at. They could get her there really quickly, let’s put it that way. And the fact that they put her in a room on his own, I think was a wise move, don’t you?
Patrik: Put him in a room by her?
Tess: Yes. And not in-
Patrik: In ICU?
Tess: Yes, in ICU he’s being monitored by a nurse.
Patrik: I don’t think that’s a bad thing at all, I’ll tell you why. It’s generally speaking less infection risk.
Tess: Less infection risk, I immediately assumed that, and also it’s going to be a lot less stressful, because I checked with the doctor this morning, she’s far more conscious than she was, and it’s a good possibility that with all the sounds and everything, it could become over stimulating for her, and be deleterious to her recovery.
Patrik: Absolutely. I don’t see her being in a single room as a bad thing, not at all.
Tess: But if it wasn’t for Romeo question in her way, and talking about different methods but to get to the end point of her actually giving in to an extent that she’s now in the situation she is. I think they’re being a bit lackadaisical just in the moment. They shouldn’t let somebody die when they’ve got to the point of rehabilitation-
Patrik: Oh no, definitely not.
Tess: And there’s a chance of the person under their own assessment to actually have good, relative good chance in a three to four months period of actually making it with help.
Tess: He’s got a three-week assessment period that they will commence after she has come out of the ICU. I asked the doctor, how long do you think it might take for her to return to the ward, the physiotherapy ward, and she said about a day and a half. And then it’s going to be a tracheostomy tube change and there’s going to be a delay in the trach change, they may actually keep her in that room, mightn’t they?
Patrik: They might. They might.
Tess: But I don’t see why they shouldn’t do it today, because I said, “Is there any risk for Sarah with it not being changed right now?” She said no.
Patrik: Again my question goes back to, if they do want to do it today, they would have to put her nil by mouth, well, stop the feeds, if that makes sense, just as I mentioned before.
Tess: Okay, well that’s a part maybe you can actually broach in a moment and we can get across to them, because basically it’s an important point.
RECOMMENDED:
Patrik: Look, they probably feel offended if I ask that question, because it should be a basic skill for them, however, given that she aspirated, that’s the first thing that comes to mind.
Tess: There’s no risk if when they take the tube out that feed can come out of it, or they’d flush it wouldn’t they?
Patrik: Say that again.
Tess: Is there any risk that when they take the nasogastric tube feed out, that it could cause any further problems?
Patrik: Look, you want to keep the feeds going of course, generally speaking, but you can’t keep the feeds going when you’re doing a tracheostomy change. You need to stop it temporarily.
Tess: I wonder if they did it. I don’t know, Patrik, maybe you can ask.
Patrik: Look, they probably feel offended when I’m asking, because you know this is a bit I like, did you fasten your seatbelt when you drove the car sort of thing, but it’s still-
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!