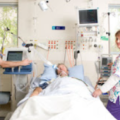
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Romeo, as part of my 1:1 consulting and advocacy. Romeo’s daughter is on a ventilator with a tracheostomy and Romeo is asking if it would be safe for his daughter to transfer to a nursing home.
Would it Be Safe for My Daughter with a Tracheostomy & on a Ventilator in ICU to Transfer to a Nursing Home?
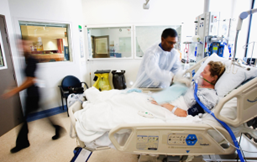
“You can also check out previous 1:1 consulting and advocacy sessions with me and Tess/Romeo here.”
Patrik: Hello Tess.
Tess: Hi Patrik. Let’s get on a call now.
Patrik: Yeah. I’m going to record this call, then we can send it to you.
Tess: Thank you very much, Patrik.
Patrik: It’s a pleasure. Look, I had listened, obviously. I’ll tell you my opinion on it. It sounded not too bad overall. It sounded like they want to help you, but again, like what I have been saying for the longest, you got to watch what they do, not what they say. My biggest concern that came out of the meeting that I can see is when they want to send her to this place where they’re having this score. That’s always a bit worrisome to me because they’re sort of going by numbers only without taking your opinion into account. And I was glad to hear that you and Romeo were saying, “Look, we know Sarah and we know what she’s like and we know she’ll get through this,” and all of that, whereas they will be only looking at numbers.
RECOMMENDED:
Tess: From the hospital, the implication was that they thought that their scoring system had continuity with the rehabilitation hospital, and from my understanding if I’m correct, that there would be a continuum, if she were to go there.
Patrik: No, as I said, that was a takeaway for me, but probably like yourself, you can’t trust just their words.
Tess: I know, but did you not catch what the doctor was saying, “Oh, well, you’ve just got to trust the numbers,” attitude.
Patrik: Exactly. And that’s why I was glad that you and Romeo said, “We know Sarah and it’s not only a numbers thing.” And I was glad that you said, “Assess her when I’m there.”
Tess: Yes. But I’ve got to really push for that in the sense of make sure that it’s put down on the notes, because otherwise, they may well go ahead without my opinion… And I’m only 25-minutes’ walk away. I’m prepared to be there at whatever time of day or night to assist, and I’m assuming that those such things would be happening on the wards that they’d proposed to send her to, after she leaves the ICU.
Patrik: Yeah, absolutely. What I couldn’t figure out, the person that was there besides that lady, who was that? Was that a physio…
Tess: Yeah. Dino, his name was, apparently.
Patrik: That man is counting numbers.
Tess: Counting numbers, did you say?
Patrik: Well, yeah, counting numbers. Counting dates. He wants to know how quick can we get rid of Sarah? That’s what he wants to know.
Tess: Oh, so would he be basically.
Recommended:
Patrik: He’s the bean counter.
Tess: Can you repeat that please, Patrik? I didn’t catch that.
Patrik: He’s the bean counter.
Tess: Okay.
Patrik: No, but that’s not what I meant. There was a man there, wasn’t there?
Tess: Yeah, he’s a physiotherapist, who’s had about 6 hours with Sarah thus far.
Patrik: That’s who I meant.
Tess: Yeah, but he kept completely quiet, basically. He’s there on the initial part of the call when he encounters Rey and gets Rey to come along. He’s the man, and he sat in the meeting, and he didn’t even really say anything.
Patrik: Did he take notes?
Tess: Nope.
Patrik: Okay. Did someone take notes?
Tess: I was the only person taking notes.
Patrik: Okay. Normally, someone takes notes from their end. And, he was gauging the mood, he wants to know how quickly can… and sorry to be so blunt, he wants to know how quick can we get rid of Sarah? That’s what he wants to know.
Tess: Yeah. And so, they’re basically stating this weekend, by the end of this weekend, aren’t they?
Patrik: Well, that’s what I understand, but isn’t there a stage process? First, she will leave ICU and then she will go to this other place. Isn’t that what they’re proposing?
Tess: Yes. And the timeframe could be a variable, anything between 2 weeks potentially or what was it? One to 3 months? 1 to 2 months. But I was horrified at the thought that a nursing home was being proposed, Patrik. I don’t want that to happen for Sarah.
Patrik: I was going to come to that. I was actually going to come to that. Number one, I was absolutely horrified because here in Australia, this discussion has been going on for many years, young people in nursing homes. This is just horrible. Even if she ends up with a tracheostomy in the long run, what I will do is I will set you up with one of our clients and his mom was in ICU for about 12 months. His mom is now at home on a ventilator with a tracheostomy, and she’s got 24-hour nursing care. And he fought long and hard for that, and I believe he can advise other families what to do.
Tess: That’s very kind. That would be very helpful.
Suggested links:
Patrik: Yeah. No, absolutely. I will also send you an interview that I’ve done with him a while ago. I think you can listen to that. It’s a different, but somewhat similar situation. I mean, his mom would be late 70s or early 80s now, and his mom did have a brain injury, so his mom could, and still can, indicate what she wants. But at the end of the day, the similarities are that if you have a tracheostomy, you might be stuck in the hospital system forever and a day because of the tracheostomy, and I can tell you, a nursing home won’t cut it with a tracheostomy.
Tess: No, I do realize that. I don’t know the ins and outs and the implications of the nursing home, but I’m imagining as much.
Patrik: Yeah. So, it’s not there yet. She’s got to leave ICU next. Maybe there is a chance that she can have the tracheostomy removed. The problem is, as long as she’s not gagging, she needs the tracheostomy.
Tess: Yes. I would like to pass you to Romeo so he can have a quick word.
Patrik: Sure.
Tess: Thank you, Patrik.
Patrik: It’s a pleasure.
Recommended:
Romeo: Hello, Patrik.
Patrik: Hey Romeo, how are you?
Romeo: Oh Patrik, you know, I saw Sarah in a dream last night.
Patrik: I see.
Romeo: … and even talked to her.
Patrik: Good. Oh, that’s good. Let her talk to you, I think that’s a good dream to have.
Romeo: Yeah. I often think about my daughter, I want to be there inside, you know…
Patrik: Yeah.
Romeo: So yeah, just trying to deal with that. I’ve been with them and just see what they’ve got in, what their plans are for once, you know. And taking to heart, fill up in my mind the things about this process and all things, but if you don’t try… you don’t know until you try…
Patrik: Absolutely.
Romeo: And the other fella, the doctor, said that she knew about… but she does in a sarcastic way, that she knows about Sarah’s got to get back to being.. you know, and she needs the right… I’ll check BP recordings. Do you know what I mean?
Patrik: Yeah.
Romeo: And you never know what they’re conniving, and they might say things like that are classed as, you know, and people like that for other people. But he’ll have a word. I’ll say to Sarah, we’ve got to do the right thing when we’ve got a chance to do the right thing. I’ll reward her and all that, if I can, in the future. But then when I mention I’ll reward her in the afterlife, now when I say I’m going to reward her, see, I’m looking at the expression even though I’m not blinking or nothing like that. So, I ask, she will know what I’m saying, and I’ll watch her, because I want to encourage her. And they’re pleased with that.
Romeo: But then when I say the opposite, they’re like, “Ooh.” They’ve gone off. But that’s fine. You don’t know. You’ve got one chance to get it right. That’s, for us to know in our self, the reasons why we try, the reason why we try to do the best that we can. It’s not always easy to bring the best out in other people when there’s a lot of emotions involved but you can always try, Patrik.
Patrik: You know, the thing that I always say in those situations is ICUs are always trying to push for end of life and I say well, once someone is dead, they’re dead. There’s no coming back from that as far as we know.
Romeo: Yes. But what other chance… Someone will tell her a thing and then suddenly, she’s had a heart attack or she’s not breathing in a couple of seconds. If they’ve got a respirator, if they got things like that, they’re not helping, sort of thing, in my opinion, then just leave it, or cause the situation. I like to mention also about her organs, and they get attitude, but when they do change her, get a bit like things when I say, Tess’s got 2 degrees or a BA and a MA and Rey’s got a degree and everybody around here sort of thing, everybody’s got a degree, and that’s when I say, purposefully, I’m the only ignorant one. And I’m seeing those things.
Patrik: Yeah.
Romeo: Do you know what I mean?
Patrik: Yeah.
Romeo: Anyway, I’m not talking about that. I’m talking about Sarah and things like that.
Recommended:
Patrik: Right. I think what’s also important for both of you, and I know they have almost been dismissive of that, but one question that I always have for any client really, is what’s your gut feeling? We know the science, and they will always be referring back to the science, but what’s your gut feeling? That’s number one. What are your personal beliefs, are you religious, any of that? Not that I’m asking you that now, but this is something for everyone to answer in this situation. The problem is the hospitals are not asking those questions. They just have their own agenda, and they don’t care about that sort of stuff.
Romeo: They want the bed space…
Patrik: They want the bed space.
Romeo: … out of there, but safely, safely.
Patrik: That’s right.
Romeo: But they’ve got to give her a chance.
Patrik: Give her a chance. That’s what it is. Give her a chance, that’s what it is.
Romeo: Give her the same care and compassion that they’d like, that makes her agreeable. Like you say, baby steps, one day at a time.
Patrik: Yeah. Look, they were agreeable because they didn’t want to cause any friction and you will see whether their words match their actions in the next few weeks.
Romeo: Yeah, I understand Patrik. Thank you very much for your assistance, and for your professionalism and your experience, and the dedication that you’ve given during your life for other people, and your reasons for not continuing where you were, and obviously to make a better situation, a better scenario for other families that need your help. And I appreciate that very much.
Patrik: Oh, it’s a pleasure. I hope things will improve.
Romeo: You’re the kind of person who work not for wages, Patrik, you know what I mean.
Patrik: Yeah.
RECOMMENDED:
Romeo: Helping not for wages, because wages is third world, third stream, you know what I mean. We did our best. And the doctor admitted, there was a surgeon, and a midwife and a pediatrician and the pharmacist as well, and everything, you know?
Patrik: Absolutely.
Romeo: Anyway. Look, I like looking at evidence and things like that, I like seeking out who this person could have been dumped here on the motorway. You have to face your companion in public law. There’s an old friend who, she tried to assassinate me, and she felt comfortable with me being there, so I was assisting through 24-hour shifts in any way I can, even in a companion her secretary is there.
Romeo: Truly though, be the bodyguard sort of thing, in my years for sitting, when there weren’t enough statements for people, because it’s not as bad as they say in that location. They’re trained in civil and criminal law, so if you come to the government and you bring a lawyer with you to explain the situation, you’re going to have to pay the lawyer, but the lawyer’s not going to pay the government. You just come and explain yourself and they’re trained in civil and criminal law, and can guide people through the situation, 24 hours, 24/7, like 365 days a year.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!