Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
What Questions to Ask if You’re Locked Out of ICU Due to COVID and Your Loved One is Critically Ill!
You can check out last week’s question by clicking on the link here.
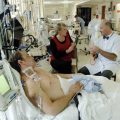
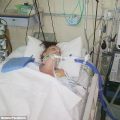
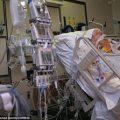
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tess, as part of my 1:1 consulting and advocacy. Tess’s daughter is with a tracheostomy in the ICU. Tess is asking how they can stand against a DNR status for their daughter in ICU.
How Can We Stand Against a DNR (Do Not Resuscitate) Status for our Daughter in ICU? Help!

“You can also check out previous 1:1 consulting and advocacy sessions with me and Tess/Romeo here.”
Patrik: Look, you want to keep the feeds going of course, generally speaking, but you can’t keep the feeds going when you’re doing a tracheostomy change. You need to stop it temporarily.
Tess: I wonder if they did it. I don’t know, Patrik, maybe you can ask.
Patrik: Look, they probably feel offended when I’m asking, because you know this is a bit I like, did you fasten your seatbelt when you drove the car sort of thing, but it’s still-
Tess: But Patrik, in all fairness, they will probably say we can’t attest to that because we don’t know because we aren’t the ones that did the tracheostomy tube change. Should I try and find out from them? Are they going to necessarily answer that question?
Patrik: Well, they have to. It’s a case of … let’s say they don’t want to answer the question, it’s a case of you then asking for access to the medical records. Simple as that.
Tess: But I’ve already been refused those by the medical records office.
Patrik: Well, that’s illegal.
Tess: That was done ages ago because I don’t have any power of attorney, I’m not an appointee.
RECOMMENDED:
Patrik: That part I can’t help you with, but for the power of attorney, you could have access to the medical records, that much I can tell you.
Tess: There’s obviously copious amounts of information going on, but I have the suspicion given that they’re doing this as a precautionary measure, that’s the words she used, to ensure that she is all right. They didn’t want to handle it as a final thought. They decided they didn’t want to handle it on the ward where she meant to be. That’s why they sent her to the ICU to make sure she’s monitored, he’s done very good consideration, do you know what I mean?
Patrik: Right.
Tess: So it doesn’t take the fact that they’ve still got her DNR (Do Not Resuscitate) on her, and she won’t escalate … she will not allow anything to escalate. That is, they won’t do anything to help her other than what they’re doing to help her now.
Tess: And they weren’t even going to do that until Romeo pushed. Now, fortunately she’s stable. That’s the most important thing, and I believe, although I sensed from talking to her, she got a little bit suppressed uppity with me, because I’m asking important questions. I’m making important points. It’s like, sometimes the experts they don’t want to be … they don’t want to explain themselves, do they?
Suggested Links:
Patrik: Of course not.
Tess: They take that sort of higher ground. But I was civil and kind to her in the way I communicated, and I tried to be as intelligent in my questioning, so this person is extremely accomplished in my own mind already. They’re bit on the right thing by getting her looked after, but the whole matter of this mistake that may have occurred, that’s not through no fault of Sarah’s, is it?
Patrik: No, look-
Tess: She was doing all right.
Patrik: The fault, it may have occurred. Other things that may have happened is maybe she hasn’t had her bowels opened for a few days. That could also lead to aspiration. Those are all questions we can ask.
Tess: Maybe, not open the bowels for a couple of days?
Patrik: Well, I’m just talking from experience here what I’ve seen over the years. That’s all.
Tess: Okay.
Patrik: Look, if someone aspirates, that would be one of the first things … there’s often something going on in the bowels. It could also be as simply as maybe they did stop the feeds hours before the tracheostomy change, maybe they had her lying flat. I don’t know. Those are all the questions that can be asked.
Tess: Yes. I suppose for that matter they can’t necessarily answer, they’re actually on the notes, and readily available to the doctor and it should be to ascertain those facts, but at the moment I’m getting slightly mixed messages in that I know that this mishap has occurred from the other end. I extensively believe them when they say, I do believe them when they say that it’s not their fault. Not that those words have been used.
Patrik: Can I just ask, Emma, who has the power of attorney if you are not the power of attorney?
Tess: I don’t have the answer for that.
Patrik: You should urgently seek a family lawyer for this, because I think, you or Romeo not being the power of attorney could become a big issue in this. I think you should urgently seek a family lawyer to sort this out.
Tess: I don’t have a family lawyer.
Patrik: Look, it’s outside of my area of expertise. What I will say is you or your husband need to become the power of attorney as a matter of urgency, and the person that will help you with that is a family lawyer.
Tess: Okay, so we’ve got to liaise to find a family lawyer. Do you know how to get one?
Patrik: The reason, and I’ll tell you why. As I said, how to get it, I don’t know. That is not my area of expertise, but the reason I am telling you that is, I’ll give you a worst-case scenario that I’ve seen over and over again.
Patrik: Let’s just say there is ongoing dispute about the DNR (Do Not Resuscitate). Let’s just say there is ongoing dispute about access to the medical records. The hospital already argues that the DNR is in her best interest. I have seen that if there is dispute about those things, the hospital will try and get power of attorney. The way they do that is they go to court and they say that you as parents are not acting in his best interests, which is ridiculous, but I’ve seen it, and if the court is lending them an ear, and the hospitals are doing this over and over again, because they think that not having a DNR is “in the best interest for Sarah “. By you becoming the power of attorney, it’ll be much more difficult for them to make such attempts.
Suggested Links:
Tess: Right. Okay.
Patrik: I don’t think it’s a hurdle, it’s just a process that you need to go through. A family lawyer should be able to help you with that.
Tess: Sarah doesn’t have ability to give her consent for me to be her power of attorney.
Patrik: No she doesn’t, and that’s why you need a family lawyer.
Tess: I don’t have a family lawyer.
Patrik: You have to find. As I said, how to go about it is not my area of expertise, but I will tell you, you need to get power … you or your husband or both, you need to get power of attorney as quickly as possible.
Tess: Yeah, okay. Will it actually work out? I mean, it’s probably … yeah, go on.
Patrik: I believe that when we spoke last year, I’m pretty sure that I sent you some questions, haven’t I?
Tess: Are you talking about all the specific questions to ask?
Patrik: Yes, yes.
Tess: Yes. That I need to-
Patrik: They haven’t really changed. Now that she’s back in ICU, those questions are still applicable. You need to ask them the right questions for your daughter.
Tess: Which is what I’ve depended on, and what I’ve quoted back to you using those questions that are originally from you-
Patrik: Yes, I’m just looking them up here.
Recommended:
Patrik: I would be very surprised if she hasn’t been on Clexane or Heparin, at least on small doses. I’d be very surprised.
Tess: Yeah, of course, because he’s been-
Patrik: Immobile.
Tess: Immobile for so long, good point. Okay, yeah. Heparin, I forgot to ask that, and the central line. Okay. I think that … what do you suggest we do going forward, Patrik?
Patrik: Can you visit?
Tess: I was saying, we’ve been advised that we’d be too much stimulation. She needs to rest. That’s what they’ve been telling there.
Patrik: I think you should put your foot down with the DNR (Do Not Resuscitate). I think you should be asking for the hospital policy. I also believe that you should be potentially threatening them with a lawyer about the DNR, and that is often enough to get them off your back, because they don’t want to be dealing with a lawyer.
Tess: But won’t that then trigger them to actually act against them, and they’ll get their own lawyer to then try to secure power of attorney before I can?
Patrik: There’s a risk in everything that you do. There’s a risk in not taking action. There’s a risk in taking action.
Tess: Okay, well we’ve got to make a joint decision on that.
Patrik: No, and I agree you shouldn’t make a decision on the fly. I’m just sort of trying to explain what you can do. And maybe when you do talk with the family lawyer, maybe they also have some ideas around the DNR. Most of them don’t, but you never know.
Patrik: Most of them, when you talk to a family lawyer, maybe you can ask him whether they have any thoughts about how to challenge the DNR. I can tell you from experience, most of those lawyers have no clue, but you never know. You might come across one who does have insights into that space. You never know. But I doubt it.
Tess: Yeah, my decision is that as well. Oh boy. It’s like trying to find a needle in a haystack, essentially being able to talk to a lawyer. Okay, well Romeo knows a lawyer. Well, we will try to seek out somebody, and see what they have to say, and then he knows the right person to then approach. It’s a long shot but we will take that route first.
Patrik: And the other thing is you should be very repetitive in your demands, because your daughter is very young and my argument would be how can a DNR be in the best interest of someone with her young age, and they will be saying, “On yeah, she won’t have any quality of life.” Well, what is quality of life? That’s not up to the doctors to make that call. That’s up to you, and hopefully to Sarah one day, when she’s more aware, of what she wants.
Suggested links:
Tess: Well my argument is that they … you said watch what they do, not what they say. They wouldn’t have taken her on for rehabilitation unless she had good prospects. This matter, we could be all on a windup, because in a certain aspect, Sarah has already encountered these problems previously, and they were at the ward in the other hospital able to actually keep her stable to the point she actually to be saturated and they would just give her extra oxygen on the odd occasion, but on the whole she was all right, to the point where she could actually breathe ambient air. The cuff matters. It’s the cuff, that sort of T-shaped thing that goes over the actual trach hole, underneath the mask when there’s that nebulizing, that’s what should be replaced upon the end of the nebulization process, isn’t it?
Patrik: Yes.
Tess: Well it was missing. The nurse forgot to do it in my presence. And I went and told her, “You forgot. You know that cap? You need to put it on.” It was only for a very minuscule amount of time, and the nebulizer mask was still over the actual end of the trach, the open trach.
Patrik: Right. No surprises there. Once she’s outside of ICU, she’s almost in no man’s land when it comes to someone looking after a tracheostomy. No surprises there.
Tess: Okay. I think just to be … because there was a changeover, with the woman I spoke to, there would have been a change to a new doctor in the ICU situation, I think it’d be a good idea for me to ascertain the situation, but at the same time I don’t want to do the consultant’s head in, thinking that I’m not trusting her opinion in the situation, because she’s abreast of her wellbeing as of just prior to this conversation. And she’s going to be in charge as well. She’s still got the DNR sort of thinking maybe.
Patrik: Again, there are different schools of thought. Like with anything, you need respect for other people, but I don’t think you should be intimidated by other people, and it’s a fine line, I agree with that. But the way I look at these things, and it might be unique to me, you track what you fear. If you fear that she’s doing X, Y and Z, she might. Fear is never a good guide I believe.
Tess: Yes, fear is never a good guide. You’re right.
Patrik: You know what fear stands for? False appearances … false … hang on. False appearances appearing real, or something like that.
Tess: False appearances appearing real.
Patrik: Appearing real. It’s not correct, but there is a synonym for it, something along those lines, and I do believe you either stand up for her, or you don’t. I don’t think you can be half-hearted about it, because-
Tess: Why not?
Patrik: Well, you are to a degree, because you’re worried about what is she going to do if I stand up for her. With all criticism that I have for the system, I do not believe that she would deliberately do any harm to her because you are challenging her.
Tess: Yes, so with that said, we’ve got to stay strong, we’ve got to stand against the DNR in Patrik’s opinion, and I’m just relaying to the family-
Patrik: Sorry, say that again please, it’s a bit faint. Say that again please.
Tess: I’m just relaying a little bit of what you just said to Romeo yes?
Patrik: Yes.
Tess: And we’ll not be fearful and basically override and keep them on their toes.
Patrik: You absolutely have to keep them on their toes. They need to know in no uncertain terms that you are challenging the DNR on every level.
Tess: They need to know that we are challenging the DNR on every level.
Patrik: And I’ll tell you why as well. As you know by now, they’re walking all over people. They’re not used to people challenging them. They’re not used to that.
RECOMMENDED:
Tess: They’re not used to people challenging them.
Patrik: No, they’re not.
Tess: They’re walking over a lot of people at the moment.
Patrik: So by you making a stand, they will ignore you to begin with, but that’s also why I believe you need to do it over and over again so that they understand there’s no messing around with you.
Tess: Yes, the DNR, they must be very active with the DNR. The DNR needs to be taken off, and that we shouldn’t be giving any impression that we’ll potentially mess around with Sarah’s survival. Yeah. We’ll do that now then, speak to the … can I give you the number for the ICU and see if we can do a three-way call, and see how that goes?
Patrik: I just need a few minutes, and then we can set this up.
Tess: Brilliant. Thank you so much, Patrik, for your patience-
Patrik: Thank you, thank you, I’ll call you back. Thank you.
Tess: Okay, thank you, Patrik-
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!