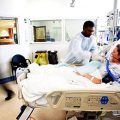
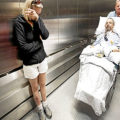
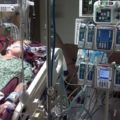
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
Why is My Loved One Prone to Develop Depression after a Long Stay in the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Jay, as part of my 1:1 consulting and advocacy service! Jay’s wife is with a breathing tube and diagnosed with ARDS in ICU. Jay is asking why the ICU team is saying that his wife is not a candidate for ECMO in the ICU.
Why is the ICU Team Saying That My 54-yr old Wife is Not a Candidate for ECMO?
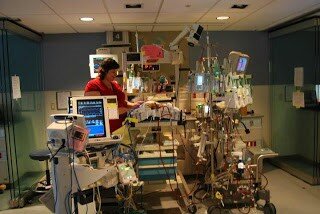
Jay: Hello Doctor. How are you?
Dr. Tom: Hello. I’m very well. Thank you.
Jay: So Dr. Tom, here with me is a family friend who is a critical care nurse. His name is Patrik.
Dr. Tom: Hi Patrik.
Patrik: Hello Doctor.
Jay: So Dr. Tom can you give us a summary of what transpired during my wife’s admission.
Dr. Tom: Alright. The events that transpired. It was the 13th, 14th, 15th of last month. And also spoke with the physician who did the ECMO or Extracorporeal membrane oxygenation. It sounds like although she was very sick after she was intubated, for those couple of days as we were escalating care… However, she was very, very sick and with severe ARDS or Acute Respiratory Distress Syndrome she was still meeting our targets with the plateau pressure and meeting lung protective strategies and ventilating.
Dr. Tom: And even though she was very sick and had a very poor trajectory, she did not require ECMO support until about yesterday, was when we had everything maxed out and she was continuing to fail. So yesterday was the first day that ECMO was even part of the conversation from her management. It was determined that just, pretty straightforward, was not on the table as an option for treatment because of her platelet count. And then I came on service this morning and sort of tried to piece it all together. Does that make sense?
Patrik: Well kind of does and it doesn’t. When was she intubated? Did you say on the 13th?
Dr. Tom: She was intubated on the 13th.
Patrik: 13th. Sure. If someone, I mean, if someone does go on ECMO, I mean, they end up on high doses of heparin. There’s a high risk of bleeding. If she’s got low platelets. I mean, what’s the difference?
Dr. Tom: I’m sorry, sir?
RECOMMENDED:
Patrik: If someone goes on ECMO, they end up on high doses of heparin.
Dr. Tom: Yeah. We anti-coagulate patients who are on ECMO.
Patrik: Of course, and there’s a high risk of bleeding if someone is on ECMO and I mean, people bleed from their cannulas all the time, if they’re on ECMO and on heparin. So if she’s got low platelets that might eliminate the need for heparin.
Dr. Tom: Well, it doesn’t, sir.
Patrik: I still…
Jay: That’s why she’s not on heparin..
Patrik: I still would like…
Dr. Tom: There’s a baseline level of knowledge of blood clots, and bleeding risk, and venous clots with different protein factors versus arterial clots of platelets. It is complex. I am just telling you that she is not a candidate for ECMO, with her platelets where they are. Plain and simple. She’s not a candidate.
Suggested links:
Jay: I have a question. So at what point, doctor, on the day before, or the day, the morning of intubation when they were asking me… “Karla’s tired, we think this is the route to go.” If her platelets were good, she had proning for more than 7 days. Because she had been actually doing it before that, she had ARDS. Then at that point before we intubated, her oxygen number was up from 81, which it had been 2 days before at 97. At that point if her platelets were still in range, then at that point, why was ECMO not offered as a… Before intubation.
Dr. Tom: I address that. That’s what I led with. My conversation that I’d started with was the answer to that question. She was sick. She is very sick, but she did not… There’s certain criteria on the ventilator that we look at to see if ECMO is needed and it has to do with whether or not we’re causing barotrauma and volume trauma, which is then causing harm with the ventilator. Or whether we’re meeting certain safety parameters based on the plateau pressure and the driving pressure and whether not we’re ventilating her with the pCO2. There’s a lot of numbers and factors that go into who needs ECMO.
Jay: But the morning before, Tuesday morning at 11:00 I got a phone call that they were considering to intubate her. Why wasn’t it introduced before that? She wasn’t in cardiac arrest, she was not in…
Dr. Tom: Are you talking about ECMO?
Jay: I’m asking, the day of intubation, before they intubated her… I’m asking because they didn’t need to do an emergency intubation. Why was ECMO not an avenue that morning…
Dr. Tom: That would not have been appropriate? There’s about 6 steps or more between needing to be intubated and needing ECMO, which is what we did. You get intubated, then you look at the blood gas and then you prone, and then you sedate, and then you paralyze and then you optimize the PEEP (Positive end-expiratory pressure) and you optimize the driving pressure and that’s what we’ve been doing. This is very complex, there is a lot of moving parts. We don’t just do ECMO on everyone who has ARDS. You don’t even do ECMO on everyone who has severe ARDS.
Jay: I do understand. It’s just… Patrik, go ahead and finish the conversation for me please. And we will let you go.
Patrik: Can I just ask a couple more questions, doctor? What’s the arterial blood gas (ABG) at the moment, what are we looking at partial pressure of oxygen (PaO2) and carbon dioxide (PaCO2)?
Dr. Tom: She’s on a 100% FiO2 (fraction of inspired oxygen), when she was proned this morning, her PaO2 was 55. So that’s a P to F ratio of 55. Which is… anything less than 150 is severe ARDS.
Patrik: And with that PaO2 of 55, what are we looking at in terms of oxygen saturation?
Dr. Tom: So it varies on her position while doing nursing care. She’s proned, and then we supined her for a couple of hours to help prevent skin sores and skin breakdown, and as part of our normal proning protocol. And then different positions desaturates anywhere from the mid-80s to the mid-90s, on a hundred percent FiO2.
Patrik: Sure. And sort of with severe ARDS… Are you doing things like, some units I’ve seen nitric oxide, epoprostenol.
Dr. Tom: Yes she’s on Flolan, I forgot to mention that.
Patrik: She’s on Flolan.
Dr. Tom: Yes, she’s on a pulmonary vasodilator.
Patrik: Right. I see. And for how long has she been on a 100% FiO2?
Dr. Tom: I believe yesterday was when she had ended up needing to go to 100%. To maintain our goal saturation.
Patrik: Sure. And proning, head down, doesn’t make any difference at the moment.
Dr. Tom: I think it makes a difference, I’ll have to go back and review it but, yeah. It certainly isn’t bringing her P to F ratio up above 60 or 65.
Patrik: Okay. And kidneys are working?
Dr. Tom: Yes.
Patrik: Right. There’s no need for dialysis. So she’s still making urine. She’s…
Dr. Tom: We’re giving her a little bit of diuresis. I’m trying maintain an even to slightly net negative fluid balance today. But her renal function has been… Her creatinine has been less than one for the last 2 or 3 days.
Recommended:
- YOU DON’T KNOW WHAT YOU DON’T KNOW WHEN YOUR LOVED ONE IS CRITICALLY ILL IN INTENSIVE CARE! (PART 1)
Patrik: Okay. And her blood work besides the platelets, I would imagine her white cell count would be high and her hemoglobin is stable or has she had any blood transfusions or…
Dr. Tom: She’s not had any blood transfusions. She has a slowly down trending hemoglobin as you would expect with critical illness.
Patrik: Right. And with the platelets being low, is that something that came up in the last few days? Is there a specific reason for that, that you…
Dr. Tom: Yes. Yesterday platelets… Today’s platelet count is 13. Yesterday’s was 24. The day before that was 38, and the day before that was 79, the day before that was 88, the day before that was 95. It’s just been down trending steadily for the last week.
Patrik: Okay. And obviously, you mentioned sepsis earlier. I would imagine she’s on… I don’t know what you do for the COVID, the Remdesivir, or is there any…
Dr. Tom: She is on our standard treatment. She’s received Remdesivir, let me get my note up. She’s received our standard therapy, which is… There are varying… She’s on high dose IV corticosteroid. She received Remdesivir and Baricitinib.
Patrik: Right.
Jay: Doctor, what is the hospital policy about veering outside of standard therapy in situations where…
Dr. Tom: I’m not going to discuss those interventions.
Jay: Wow.
Patrik: Well, if Jay is asking for a hospital policy, I mean, surely you can be transparent around that. Surely there’s nothing to hide from a hospital perspective.
Dr. Tom: No way. I do not wish to discuss changing the dosage of the budesonide. And I do not wish to discuss Ivermectin. Those issues are settled. I can discuss other things if you would like to.
Suggested links:
Jay: I was just asking, thank you, what your policy was. I mean, in general, that’s all. Patrik, do you have any more questions at this point?
Patrik: Well, I don’t have any more clinical questions. All I have to say is if we are asking questions that make things transparent, it’s disappointing that you don’t want to make transparent. I would really want to know how many ECMO beds you have there. I would really want to know. I’m sure there’s lots of patients needing ECMO at the moment.
Dr. Tom: I’m not at liberty to discuss our ECMO resources. Our hospital is a site, that’s the limit we will be discussing.
Jay: Doctor, how would I get a hold of the doctor’s notes on MyChart, I’ve noticed those have not been included. How do I get a hold of the doctor’s notes over the last few weeks?
Dr. Tom: I’m not sure, I can share my notes today, but I can’t speak to what was done with the prior physician’s notes. But I have the “share with patient” button on mine. You can read my note from today.
Jay: That’s wonderful. Do you know who I would talk to?
Dr. Tom: I don’t. Maybe I would start with patient advocates. I’m not entirely sure. So, that’s a relatively new thing for us that families can read the daily progress notes. I actually don’t know much about the details of that, but it’s the default button that the note is shared with the patient. I haven’t changed that for my note.
Jay: Perfect, I appreciate that. I will call patient’s advocates for that. Patrik, anything else? Can we let the doctor go?
Patrik: No, I think that’s it. Thank you so much for your help.
Jay: Thank you, doctor.
Dr. Tom: Just one thing. Earlier on the phone call, you started to ask a question. I think you started to ask a question and we kind of got a little bit sidetracked, in the weeds. Correct me if I’m wrong, you were waiting, or about to ask “Where do we go from here?” Or something along those lines.
Patrik: Yeah, probably. Yeah.
Dr. Tom: Is that true?
Jay: Yeah, that’s a great question, and I… Yeah.
Recommended:
Dr. Tom: To not get into too much of detail… Like not only details, but look. She’s either going to get better on her own with our current level of support or she is not. She is very, very sick. Her chances of dying are very high. We are going to continue doing everything we are doing, which is maximum support and if new issues come up that we can treat or look into, we’ll certainly communicate that with you but from a, sort of a big picture, 10,000 foot view of everything, she’s probably not going to make it. She might, and we’re pulling for her and we’re doing everything, but some of it is kind of out of our hands right now. She’s either going to get better or she’s not.
Patrik: I disagree that you’re doing everything. I disagree. You’re not offering her ECMO. I disagree.
Dr. Tom: Okay.
Jay: Can we… I have a couple questions about this because obviously, in the next few days I understand what’s going to happen one way or another. Can you please have a candid conversation with me, Patrik? I want to know some of the questions as far as it is too invasive to bring her out of sedation so that my family can say goodbye to their mom and their daughter and my wife too. Is that too dangerous? Is that something that can happen so that we could say our goodbyes?
Dr. Tom: I cannot imagine how difficult this could be for you and your family. I’ve been the doctor for situations like this, but I’ve not been on the other side of the phone for anyone close to me. I cannot, in good conscience, wake her up. One, for one reason, I think she would die if I did that. But also right now the intubation is alleviating her suffering. And to turn that off would stop alleviating her suffering.
Suggested links:
Jay: Okay. So, and… Patrik, tell me if you agree with her.
Patrik: I agree with that, Jay. I agree with that. That lowering sedation would not be beneficial for her. I understand your concern of course Jay, but I agree that lowering sedation would not be in her interest.
Jay: Okay, I wasn’t sure. So I guess, I don’t know. I mean, I guess maybe I need to know… At some point will her family… I mean, in situations like this I know you only allow two people. I understand, but I mean, what are… I mean, surely if this is happening, I… Tell me, what do you allow? What you don’t. I mean, because I have four children.
Dr. Tom: So we’re going to get our lead nurse or our charge nurse who’s going to be able to talk to you about what our current regulations are regarding that. But I did want to tell you that I’m not in any way pushing you to make a decision like that, right now. I mean, if that’s what you and your family want to go, I can walk with you there but that’s not part of my plan right now.
Jay: No. Okay. I mean, I don’t know how this happened. Did her heart quit working? I mean, are we waiting for her organs to shut down or are we waiting for her to get better?
Dr. Tom: So she’s very sick and there are any number of things that if they got worse could be life-threatening. Bleeding is a very large concern, but also yes, you’re right. The amount of stress that her body is under and the low oxygen levels. It’s vague and grey, it’s just very hard on the heart. As days click off, there’s more and more stress on the heart. And it just sort of starts to give out. It’s not very scientific. That’s the way we see these things happen.
Dr. Tom: So sometimes it happens fast. Something bad happens really fast, other times it’s just more of a gradual… The blood pressure starts going down, the heart rate starts going up, and we see sort of arrhythmias and different things with the telemetry. And you can just kind of get a feel for it. It’s not really anything specific. But like I said, right now, that’s not, that really wasn’t a conversation I was even like… That’s not where we’re at today. Yeah, I mean, she is very much ticking up to die, but that’s not what we’re really… Those signs are imminent or impending death, we’re not seeing. A lot of grey area here. Patrik, you said you’re a critical care nurse?
Patrik: Yes, yes.
Dr. Tom: Yeah. So you can kind of… Can you understand kind of where I’m coming at with that?
Patrik: Yeah. I agree with some of the things you are saying. What I’m lacking here is transparency. What’s your decision making process around ECMO? I feel like you’re not transparent with us and that’s disappointing because there are decision making… There’s policies in hospitals, how you make decisions around who you offer ECMO. And what’s your problem with making that transparent with us? You’re just keep on saying, “Oh, she’s not a candidate for ECMO.” That’s not good enough. That is not good enough to make such a statement. Make it transparent. What’s your flow chart, who you put on ECMO, who you don’t put on ECMO, tell us how many ECMO beds you have, make it transparent. What do you have to hide? Tell me what you have to hide about your decision making process here.
RECOMMENDED:
Dr. Tom: The current… I believe I’ve addressed these things.
Patrik: No you haven’t. No, you haven’t. Send us the policy around your decision making process, who you put on ECMO and who you don’t. What do you have to hide around that? What’s so difficult…
Dr. Tom: It’s not that algorithmic, sir. The decisions on who can go on ECMO is a clinical judgement, based on our ECMO physician reviewing the case. There are not hard and fast… I think I’ve said what I’d like to say on this topic.
Patrik: Yeah, what you’d like to say. Not what we need to know to make…
Dr. Tom: No, I said what I’m going to say. She is not a candidate because of her platelet count.
Patrik: Plenty of people going on ECMO with low platelet count. That’s fine. You say what you want to say. It would be good to have those discussions that you had with your team in writing. So we can see that you are making decisions that are in the best interest of Jay’s wife. We’re talking about a 54 year old. We’re talking about a 54 year old woman.
Dr. Tom: I’m very aware of that. So I feel like you think I’m trying to keep something from you.
Patrik: Yeah, absolutely. Absolutely. Tell me how many ECMO beds do you have and how big is your ICU and many COVID patients do you have on with ARDS? Make those numbers transparent. What do you have to hide?
Dr. Tom: So I’m not the head of our ECMO program. And I don’t know that that is information that is public knowledge. Well
Patrik: Well, maybe… Well…
Dr. Tom: No matter what those numbers are… So I’m not trying to keep it secret. I just also don’t want to divulge information that I’m not able to. I’m certainly not the right person. Even if we were going to share that information, I’m not the right person to do that. No matter what the answers to those questions are, she is not a candidate for ECMO based on her medical picture, her clinical picture.
Jay: Patrik, perhaps that’s a conversation that we could get with the gentleman that made that decision.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!