Podcast: Play in new window | Download
Subscribe: Apple Podcasts | RSS
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Loved ones in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
Is a Meaningful Recovery Possible for my Critically Ill Sister in ICU with Acute Pancreatitis?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions that we get quite frequently as part of my 1:1 consulting and advocacy service!
How Can My Loved One Prevent Aspiration Pneumonia in ICU?
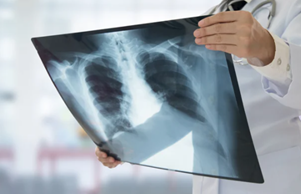
Aspiration is defined as the inhalation of either oropharyngeal or gastric contents into the lower airways, that is, the act of taking foreign material into the lungs. This can cause a number of syndromes determined by the quantity and nature of the aspirated material, the frequency of aspiration, and the host factors that predispose the patient to aspiration and modify the response.
Aspiration pneumonia is a type of pneumonia caused by the accidental infiltration of food or other substances from the mouth or stomach into the lungs. The condition can be caused by bacteria that normally reside in the mouth or nasal passages, or triggered by non-infectious toxins that damage lung tissue.
Pulmonary aspiration with subsequent pneumonia is a serious complication frequently encountered in the intensive care unit (ICU). Aspiration pneumonia is caused by the inhalation of colonized oropharyngeal and gastric secretions and is, therefore, an infectious process. The problem is complex for aspiration pneumonia: 20–30% of patients in the ICU presenting with gastric content aspiration eventually develop a secondary infection. Techniques to avoid or reduce aspiration are important in preventing pneumonia and pneumonitis.
What causes aspiration pneumonia?
Aspiration pneumonia is characterized by a failure of the physiological mechanisms that prevent food and other substances from entering the trachea (windpipe) and lungs. The aspiration (drawing in) of these substances can cause inflammation, infection, or airway obstruction.
Healthy people will commonly aspirate small amounts of food and other substances into the lungs, but the body’s natural reflexes (gagging, coughing) will usually clear them without difficulty. Problems only occur if larger amounts are inhaled or the impairment of the lungs or nervous system weakens these pharyngeal reflexes.
Many cases of aspiration pneumonia are linked to either a neurological condition or an episode of impaired consciousness that disables this reflex.
Examples of conditions that would impair this reflex and potentially lead to aspiration pneumonia include:
- neurological conditions like stroke, Parkinson’s disease, Alzheimer’s disease, multiple sclerosis, cerebral palsy, amyotrophic lateral sclerosis (ALS), myasthenia gravis, and brain trauma injury for which dysphagia (difficulty swallowing) is a characteristic
- vomiting, during which the severe spasms can allow food to slip from the esophagus (feeding tube) into the trachea
- alcohol, sedatives or illegal drugs, which can alter your level of consciousness and disable the normal gag reflex
- critical patients on induced coma and coming out of the induced coma/sedation
- seizures in which involuntary spasms can promote aspiration
- general anesthesia, which also disables the swallowing reflex
- dental procedures in which anesthesia and oral manipulation can enable aspiration
- gastric tubes and endotracheal tube which provide a ready route of access from the stomach to the lungs
- gastroesophageal reflux disease (GERD), characterized by acid reflux and the increased risk of chemical pneumonia
Aspiration pneumonia is also associated with the following mechanical conditions:
- Upper gastrointestinal endoscopy
- Gastrostomy or postpyloric feeding tubes
Other types of associated conditions are as follows:
- Protracted vomiting
- Prolonged recumbency
- General deconditioning and debility
- Critical illness
How is aspiration pneumonia diagnosed?
The doctor will look for signs of pneumonia during a physical exam, such as a decreased flow of air, rapid heart rate, and a crackling sound in your loved one’s lungs and the doctor may also run a series of tests to confirm pneumonia. These may include:
- sputum culture
- complete blood count (CBC)
- bronchoscopy
- computed tomography (CT) scan of your chest area
- blood culture
How to prevent aspiration pneumonia in ICU?
Aspiration pneumonia is an infectious process caused by the inhalation of colonized oropharyngeal- and gastric-secretions.
It often occurs in patients receiving mechanical ventilation and can be considered as ventilator-associated pneumonia.
A small subgroup of patients without endotracheal tubes develop aspiration pneumonia as a consequence of neurological dysfunction related to stroke, altered swallowing reflexes, weak cough reflex, or excessive sedation.
Preventive treatment mostly relies on factors described below and all measures related to the prevention of ventilator-associated pneumonia:
- Avoid Excessive Sedation
Coma or altered levels of consciousness are known to contribute to the development of pneumonia. When a patient is sedated, they may be less likely to clear their own airway by coughing or gagging. Avoiding excessive sedation in ICU patients can be accomplished with the use of a sedation score and drug titration.
- Reintubation
Reintubation is associated with an increased risk of aspiration and pneumonia, so care must be taken to avoid unscheduled extubation. More importantly, weaning procedures and timing need to be selected very strictly to maximize chances of success. Clearing of tracheal and oral secretions prior to extubation is highly recommended.
- Secretion Drainage
An endotracheal tube plays a major role in the pathogenesis of ventilator-associated pneumonia, it predisposes the patient to aspiration by eliminating the cough reflex and pooling of contaminated secretion above the endotracheal tube cuff. So timely and routine suctioning plays a vital role here.
- Maintain the head of the bed at 30-45° unless contraindicated
It is now widely recognized that maintaining the head of the bed at 30-45° is critical in prevention of aspiration in non-mechanically, as well as mechanically-ventilated patients. In 1997, the Centers for Disease Control (CDC) recommended that these patients should remain in a semi-recumbent, rather than a supine, position. This recommendation was based on numerous studies showing a decrease of VAP incidence.
- Surveillance of enteral feeding
Besides maintaining the head of the bed at 30-45°, a critical measure to prevent aspiration of gastric content is based on a very strict surveillance of enteral feeding. The presence of a nasogastric tube is commonly described as a risk factor for developing pneumonia because the nasogastric tube is believed to promote a reflux of gastric contents with subsequent pulmonary aspiration.
The CDC recommends early removal of feeding tubes, routine verification of their placement, and regular assessment of the intestinal mobility with an adjustment of the administered volume to avoid regurgitation.
- Assess for signs of feeding intolerance every 4 hours in tube-fed patients
Regularly checking gastric residuals (the amount of a tube feeding that has not been digested), gastric distention, and complaints of gastric pain are all good indicators of how well a patient is tolerating feedings. Intolerance can lead to vomiting and possible aspiration.
- Use of promotility agents
Gastrointestinal dysmotility is frequently encountered in critically ill patients and this culminates in delayed gastric emptying that leads to increased gastric residual volume and increased risk of aspiration. Prokinetic agents such as metoclopramide and erythromycin are commonly used to improve gastrointestinal motility in these patients.
- Good oral hygiene
It has been shown that the amount of dental plaque increased during the ICU stay and was either present at admission or acquired during the ICU stay in 40% of patients. Moreover, a positive dental plaque culture was significantly associated with subsequent nosocomial infections.
Poor oral and dental hygiene is associated with a higher incidence of aspiration pneumonia. Oral/dental decontamination in general with 0.2% chlorhexidine gel, three times daily during the ICU stay, and dental plaque antiseptic decontamination more specifically, are very promising effective procedures for the prevention of aspiration pneumonia.
How to treat aspiration pneumonia?
To manage aspiration pneumonia, would therefore, first recommend obtaining quantitative cultures taken either from endotracheal aspirate or protected brush specimen depending on local protocols.
Treatment of aspiration pneumonia requires diligent surveillance for the clinical signs of pneumonia. Treatment decisions are based on 3 factors: [5]
- Clinical diagnostic certainly (definite versus probable)
- Time of onset [early (< 5 days) versus late (> or = 5 days)]
- Host factors (high risk versus low risk)
Antibiotics are commonly used to treat aspiration pneumonia. Even if the cause is neurologic or chemical, a course of antibiotics will still be prescribed. This is because it is often difficult to exclude bacterial infection as a primary or contributing cause.
Invasive diagnostic techniques (such as bronchoalveolar lavage) should be used when the diagnosis is not certain. Antibiotic coverage should be narrowed once sputum culture results become available.
Aspiration pneumonia are frequently encountered in the ICU. Many studies have been performed to evaluate the effect of preventive measures, and many among these were successful. It is now established that aspiration-related syndromes can be prevented by placing the patient in a semi-recumbent position, close monitoring of the stomach residual volume, providing minimal sedation, and maintaining good oral hygiene.
Additionally, the health care team, especially the nurses, plays a very crucial role in preventing aspiration pneumonia in critically ill/ventilated or with tracheostomy patients. Therefore, critical care nurses should recognize the importance of and advocate for the prevention & for the best possible treatment for their patients in the ICU.
Reducing the prevalence of aspiration pneumonia will lead to shorter hospital stays, less use of antibiotics, and a decreased mortality for their patients.
On the other hand, in cases where your loved one needs to go home ventilated with a tracheostomy, and on nasogastric tube/gastrostomy tube feedings, your loved one is at high risk for aspiration pneumonia so they need to be looked after by critical care nurses 24/7, like what we do at Intensive Care at Home where we employ hundreds of years of intensive care nursing experience who can manage your loved ones safely at home especially during emergencies.
You can check out intensivecareathome.com for more information about our services.
REFERENCES:
- Prevention and Treatment of Aspiration Pneumonia in Intensive Care Units
https://link.springer.com/article/10.2165/00151829-200504050-00003
- An Overview of Aspiration Pneumonia: The Accidental Infiltration of Food or Bacteria Into the Lungs
https://www.verywellhealth.com/aspiration-pneumonia-4178835
- Aspiration
https://www.webmd.com/lung/what-is-aspiration
- The Critical Care Nurse’s Guide to Aspiration Pneumonia Prevention
https://blog.sscor.com/the-critical-care-nurses-guide-to-aspiration-pneumonia-prevention
- Prevention and treatment of aspiration pneumonia in intensive care units
https://pubmed.ncbi.nlm.nih.gov/16137189/
- Aspiration Pneumonitis and Pneumonia
https://emedicine.medscape.com/article/296198-overview#a2
- Management of pneumonia in intensive care
https://jeccm.amegroups.com/article/view/4830/html
- WHAT IS VENTILATOR ASSOCIATED PNEUMONIA (VAP)?
https://intensivecarehotline.com/questions/what-is-a-ventilator-associated-pneumonia-vap/
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!