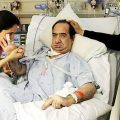
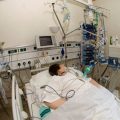
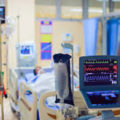
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
My Mother is on Life Support in Intensive Care! What is Actually Considered Life Support in ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Romeo, as part of my 1:1 consulting and advocacy. Romeo’s daughter is with a breathing tube and on a ventilator in the ICU. Romeo is asking how long before his daughter recovers from an induced coma and cardiac arrest in the ICU.
How Long Before My Daughter Recovers from An Induced Coma and Cardiac Arrest in the ICU?
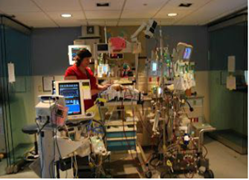
“You can also check out previous 1:1 consulting and advocacy sessions with me and Tess here.”
Patrik: Again, Tess, you’re overthinking things. Any questions that you have, you ask her. You’re overthinking. If you have questions, ask her.
Tess: Okay. Right. So, my task now is to… I’m assuming that it would be you calling the number that I relay to you, yes? And then I’m on the phone at the same time?
Patrik: Yes. And how do you think you want to introduce me to this woman? Do you want to go about it like we did with the nurse, or do you want to go about it…
RECOMMENDED:
Tess: I suspect that they already know. They have everything recorded, especially on the ward, the conversations. I would imagine so, anyway. They would have known that you had spoken to the nurse in the morning.
Patrik: Right. No, they would, they would.
Tess: And they would have probably already overheard your voice anyway.
Patrik: Why would they..
Tess: Because they may have listened back to it, Patrik. I’m just saying.
Patrik: If they are recording a phone call, they would have to, I believe, inform you.
Tess: But I don’t know about that.
Patrik: I would think they would have to inform you.
Tess: Okay.
Patrik: I also don’t think they have the time to listen to phone recordings. I don’t think they have the time for that.
Tess: Okay.
Patrik: I’ve worked in enough ICUs to know what’s priority, and potentially recording phone calls or listening, nobody has time for any of that.
Tess: My concern coming back to Sarah also, is that these myoclonic seizures, whatever they are, seizures, twitching, she didn’t mention EEG. She didn’t mention anything of knowing whether… I was stroking her head. I did feel a bit of glue in her hair. She may have had an EEG yesterday and it wasn’t mentioned to me. I forgot to ask about it, but the point being is, if she’s had an EEG to establish what’s going on with these myoclonic seizures. That’s extremely important, because whatever medication she’s on, it’s made her a lot more distant and less focused.
Recommended:
Patrik: Yeah.
Tess: And given that that’s the only real way that she can communicate at the moment, other than her plasticity helps her to be able to get back online with moving her arms in due course, I don’t know, Patrik. It’s tricky because she can’t speak for herself.
Patrik: For sure.
Tess: The Glasgow Coma scale is going to be low, anyway.
Patrik: Just remind me, how many days since the cardiac arrest?
Tess: The 31st of October.
Patrik: So, we’re almost a month. Okay. It’s not a long time, you know. It’s not a long time. I think she’s tracking well in terms of ventilation. It’s not a long time in terms of her recovery. She will probably need months.
Tess: I know. Especially given how underweight she is.
Patrik: Right.
Tess: That’s a major concern in all of this.
Patrik: Yeah, for sure.
Tess: But I got to see her frame and she’s pretty thin at the moment, you know.
Patrik: Yeah.
Tess: And I suspect that she may… what if she had had an adverse reaction to the fentanyl? Is that possible? Could she have been allergic to something she’s been given?
Patrik: Did she have fentanyl before the cardiac arrest?
Tess: She had an induced coma after the cardiac arrest.
Patrik: Yeah, no. Look, there is a small risk for that, for any allergies, of course. But the picture you are painting to me, and also the picture that the nurse painted to me, is a picture that I’ve seen before in after cardiac arrests. So, I’ve seen it many times.
Tess: Right. But to give my daughter the greatest opportunity to have at least some kind of quality of existence, I need to do everything in my power to ensure that she actually gets proper, consistent and very good care.
Suggested links:
Patrik: Yeah.
Tess: Yeah.
Patrik: And you really need to stop worrying about what they’re thinking. You ask for what you want. Stop overthinking.
Tess: Okay. I’ll try to do that but I’ve obviously been very perplexed and concerned about the whole situation.
Patrik: Of course.
Tess: … what I’ve gathered from you, it’s a minefield.
Patrik: It’s a minefield. There’s no question about that. It’s a minefield. But just like with medical records, for example, you just let them know you want access to medical records by tomorrow, 3 o’clock, you know. Just approach it that way. You never ask for permission for anything. You’re not doing anything illegal.
Tess: Yeah, but they’ve got a safeguarding thing. They had that right at the beginning when she first went to the cardiology department and the doctor approached me and asked me to… and I got a bit funny attitude from them back then. And I was by Sarah’s bedside and I was asked to withdraw and then, the doctor said, “Oh well, there’s a safeguarding, I’m sorry. I’m afraid you’ll have go through a team to be assessed.” And that distressed me big time in that moment.
Patrik: Sure. What did they..
Tess: Because I’m being almost like put under suspicion as if I’d done something wrong. I’ve done nothing wrong. I tried to save my daughter’s life.
Patrik: So what do they mean by safeguarding? What do they mean by that?
Tess: Well, safeguarding… I don’t know what the full implications of that are, other than that the head nurse at the time reassured me that it’s procedure, and that was back then. That was in the first, say, week of this whole episode, or whole situation.
Patrik: I’ll tell you another thing..
Tess: I’ve never been prevented since. Sorry to interrupt you, but I’ve never been prevented since. I actually get in to see her going forward.
Patrik: I’ll tell you what you need to do. Anything they’re throwing at you, whatever that may be, always ask for a policies and procedures, because nothing in a hospital happens without policies and procedures. So, if they’re talking about safeguarding and you are unsure about what they mean, ask them for the policy and procedure.
Tess: Okay.
Patrik: Right. Because that’ll give you the answers to that. I know it’s easier said than done. They’re trying to intimidate you, but if you give in to that intimidation, they will walk all over you.
Tess: Yes. Yes, it’s pretty self-evident in the situation.
Recommended:
Patrik: Right. So, you need to start standing up. And you do not ask for permission for anything. You’re not doing anything illegal.
Tess: Okay. So, I have to keep on insisting that the ultimate goal is for Sarah to be there in proper care, consistent care.
Patrik: Absolutely.
Tess: … which is, in that hospital, it’s not private. There are private aspects to it, but in a certain aspect, every right to be able to be cared within that environment. So, they can give second opinions, because at the moment, I haven’t even seen any visual proof, again, of the brain damage that apparently has occurred.
Patrik: Right.
Tess: The hypoxia to the brain.
Patrik: Right.
Tess: So, one doctor said in front of me, and Romeo and I, that it’s not good. The neurological consultant said the situation wasn’t good. And then we basically… we’ve not poo-pahed it, we’re fighting it mentally because we don’t know, we’re not being shown nothing. We believe that given the chance, our daughter has got potentiality to get a better life.
Patrik: Yeah, absolutely. So do you remember, do you recall that I mentioned on one of our last calls, they will be negative until the cows come home.
Tess: Yeah.
Patrik: Right. Sarah could walk out of ICU and they would still be negative. So you can’t take that..
Tess: Take that as the gospel.
Patrik: You can’t take that as gospel, and they will be negative until the cows come home. The reason for that is A, trying to protect their downside. Okay, so not making any promises that they can’t keep. Because if they were promising you only the slightest, and it wouldn’t come into a reality, you could potentially sue them. That’s the main reason why they always will be negative, always. Okay? The other thing is this. God forbid, if she was to deteriorate, they will tell you, “Oh, I’ve told you so.”
Tess: Yeah.
Patrik: That gives them the option to do whatever they want, what they think, whatever they want, you know.
Tess: Yeah. And with this sort of secretion problem in her lungs, they can use that as a viable excuse for deterioration. Goodness forbid it would happen, but the fact that she’s not actually actively being able to cough anything up at the moment.
Patrik: Yeah, but there are… again, like I said before, you got to watch what they do, not what they say. You’ve got to watch both, but even more so what they do, and what they have done, obviously, is they’ve done the tracheostomy, which was the right thing, so that gives her time. And now she’s moving off the ventilator slowly, so that’s all positive. That’s all positive.
RECOMMENDED:
Tess: So, to cut this short, because obviously you’re very busy Patrik, what I’m going to suggest is this. I try to make a fixed appointment for myself to be able to have a conversation over the telephone with this doctor. Okay. And I’ll try my best to do that. And because there’s so many difficulties with the internet at the moment, I will do my best to update you, yes, about going forward.
Patrik: Sure.
Tess: … of the situation via Skype. And if, for any reason, I don’t get through to you, would you please give me a call anyway?
Patrik: I can give you a call at 1:00 PM your time.
Tess: Yes.
Patrik: Okay, let’s go from there.
Tess: That would be helpful.
Patrik: Yeah.
Tess: Or just shortly before it.
Patrik: Yeah.
Tess: You want to say quarter to one or something?
Patrik: Yeah, let’s do that.
Tess: Yes? Thank you very much, Patrik.
Patrik: It’s a pleasure.
Tess: And I really appreciate your support. We really do.
Patrik: It’s a pleasure.
Tess: And I’ll speak to you then.
Patrik: Yeah, talk then. Thank you so much.
Tess: Okay. Thank you very much-
Patrik: Thank you.
Tess: … Patrik.
Patrik: Thank you. Bye.
Tess: Thanks. Bye-bye.
Patrik: Bye.
Tess: Bye.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!