Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED” and in last week’s episode I answered another question from our readers and the question was
The Difference Between Real and Perceived End-of-Life Situations in Intensive Care! Live Stream!
You can check out last week’s question by clicking on the link here.
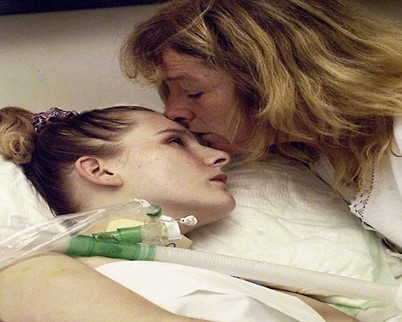
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Tess, as part of my 1:1 consulting and advocacy service! Tess’s daughter is post tracheostomy and still ventilated. Tess is asking what is the next step for her daughter in the ICU.
What is the Next Step for My Ventilated Daughter After Tracheostomy in the ICU?
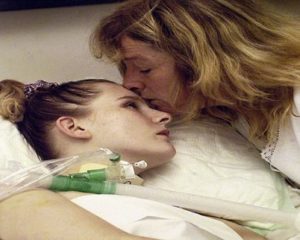
“You can also check out previous 1:1 consulting and advocacy sessions with me and Tess here.”
Patrik: Hi Tess!
Tess: Hi, Patrik. I want to ask, is there a possibility that my daughter can be weaned off the ventilator?
Patrik: Oh, absolutely.
Tess: Oh, wonderful. I’m so glad that you say that.
Patrik: If she’s opening her eyes, if she’s got a tracheostomy, a lot of it comes back to… Do you remember last week I asked you about the Glasgow Coma Scale? You said it was a 3.
RECOMMENDED:
Tess: Back then, yes. But that might be at the point when the paramedics initially assessed her.
Patrik: With the Glasgow Coma Scale, they should be doing this multiple times a day. So ask them about the Glasgow Coma Scale.
Tess: Okay.
Patrik: With the Keppra, the phenytoin, the valproic acid, they are normal anti-seizure medications. The good news is this. The good news is that they’re probably keeping some seizures at bay if she has any. The bad news is unfortunately anything in ICU comes with side effects. With the ventilator, it would be great if you could send me a picture.
Tess: I can’t because I’ve disallowed from taking any photographs or anything. I will try.
Patrik: Okay. I would never ask anyone for permission unless it’s something illegal. Taking a picture is not illegal, is it?
Tess: No, of course not. Actually, just take a shot of… Oh, actually on the Zoom call, we did take a screenshot of Sara.
Patrik: Right. Send it to me.
Tess: Okay. No. Where would the ventilator be? You’re not talking about the tracheostomy equipment itself, are you, on her neck?
Patrik: No. I’m talking about the ventilator.
Tess: On which side would that be?
Patrik: I wouldn’t know.
Tess: On the right or the left.
Patrik: Depending on where they put it.
Tess: Okay. So I’ve got to get a shot from the end of the bed, you’re saying?
Patrik: If you can send me a picture of the ventilator, a picture of the monitor, a picture of any infusions that are going in, that would be helpful. When you take a picture of the ventilator, make sure I can see all the numbers.
Tess: Okay. I’ll do the best that I can.
Patrik: Of course. The devil is in the detail, but let’s just go through your message. She’s already having time off the ventilator and that’s good. The question to me really is all of it, especially from a neurological point of view will come back to, what’s her Glasgow Coma Scale like? Does she have seizures? And what happens if they took off the Keppra and the valproic acid? So the phenytoin is off?
Tess: Yes, as of the 26th.
Patrik: Right. So it all comes down to what happens if they took the seizure medication away. Is she having seizures or not? That’s what it comes down to. If she’s not having any seizures, they might as well reduce it. They might as well take it off.
Patrik: I can see why they’re taking it conservatively. You got to keep in mind, if she does have seizures, that there could be some further brain damage from that.
Tess: Yeah.
Patrik: Every time she has a seizure, that’s…
Tess: Okay. Excuse me. Yes, Patrik, as Rey rightly says, one thing that they have ruled out that she’s not actually experiencing seizures. Epilepsy, excuse me, epileptic seizures, grand mal or anything like that. It’s mild chronic specific.
Patrik: Okay. How do they know that? Have they done an EEG (electroencephalograph)?
Tess: They must have done it at some point in the past, yes. And an ECG (electrocardiogram) . Does that make sense?
Patrik: Yeah, sure. That does make sense.
Tess: But I recollect that happening in the previous hospital before she even got transferred to this hospital. I saw it just prior to my entry into the room, the man was taking off the electrodes. But it didn’t look like many electrodes were being performed at the bedside. What looked like a simplistic electrode setup because I’ve seen ones that got really loads of them all over the head.
Patrik: Right. Yeah, sure. That’s an EEG. Yeah.
Suggested Links:
Patrik: Okay. Fair enough. When you say she’s making eye contact, you think she’s making eye contact because you’re talking to her and she’s looking you in the eye.
Tess: Yeah, definitely. When I was close by her and also over the Zoom call with other people, myself and Romeo the other day.
Patrik: That’s great.
Tess: But then today she wasn’t very good at all. Her eyes were more dazed and looking and all over the gaff.
Patrik: Sure. Today you were able to see her only on Zoom or in person?
Tess: In person.
Patrik: Okay. That’s great. She’s opening her eyes spontaneously or only when you talk to her?
Tess: She has her eyes open all the time today. Yeah.
Patrik: Okay, that’s great.
Tess: When you say spontaneously, previously, she was in a sort of half-sleep state. Then I said, “Sara,” I gave her a quite loud voice and said, “It’s Tess. It’s Tess.” And she just woke up like that. She came to and was looking at me.
Patrik: Okay, great. Great. Okay. But she’s not in a position yet where she can squeeze your hand?
Tess: No, very, very mildly. Yeah. I must admit that it was a few days ago, I experienced that. But not really today. As I said, the right foot was jerking somewhat. I assume that’s probably maybe the gaba..
Patrik: Gabapentin?
Tess: Not in the phenytoin, no. The other, the sodium… The changeover maybe. Because…
Rey: It’s the first time it happened.
Tess: Yeah. It’s the first time I’ve ever seen her foot behaving like that.
Patrik: Okay. But she’s off fentanyl. What other medications is she on? Do you know?
Tess: Something for the fact that she’s still, and they don’t want her to have knee thrombosis.
Patrik: Oh. Some either some Clexane, Lovenox or heparin. Okay. Yep. Fair enough.
Tess: Yep. The insulin, the Actrapid or something. That’s the only insulin that she’s on. But I was a bit just perturbed to hear from the doctor that they’ve come to that conclusion for the simple factors. I thought that Sara, for the best part, I mean when she initially went in, they were saying, “No, there’s nothing wrong with her kidneys when we are at the previous hospital in the cardiology department. They said, “No, we’re not worried about the rest of her body. It’s just about her brain.”
Patrik: Right. That’s still what it looks like to me, that most of the issue is around her brain. That’s what it looks like to me.
Tess: Sorry.
Patrik: Yeah, go on.
Tess: Yeah. Rey found out that the sodium valproate and the Keppra can be used together for the mild chronic seizures. So that correlates with what you’ve just said.
Patrik: Yeah, I would…
Tess: Sorry, as you’re saying.
Patrik: I would ask them, “What do they think happens when they stop it? What would be the consequences of that?” I would imagine the answer to that is that they would be worried about regular either myotonic seizures or grand mal seizures. That’s what I think would be the answer.
Tess: Yeah. Either grand mal which are very serious, yeah?
Patrik: Would be very serious, for sure. They would be trying to manage this very conservatively at the moment because the last thing they would want is stopping the Keppra and stopping the valproic acid and then she would have seizure. That could set her back. So I can see why they’re taking it conservatively.
Recommended:
Tess: Okay. If she goes out of intensive care with the tracheostomy in place and it’s being used, obviously, it’s going to need maintenance. Do you have any idea of what would the setup be in this country? Or would the options be open to them if they weren’t prepared to send her at this time to a rehabilitation hospital?
Patrik: Yep. I think there’s two sides to this, Tess. It depends on whether she can be weaned off the ventilator. If she can be weaned off the ventilator, she’ll “only have a tracheostomy”, to begin with. If she can’t be weaned off the ventilator and she needs ventilation and tracheostomy, it depends on whether she can be weaned off the ventilator or not. So if she can be weaned off the ventilator, I argue going to a ward area is an option. If she can’t be weaned off the ventilator, it’ll be difficult for her to leave intensive care, not impossible but difficult.
Tess: Okay. So it’s all dependent upon her ability to do so.
Patrik: Very much, so. Very much so. I tell you what I think needs and please don’t misunderstand me. I know you want to look into the future. I know that. I would argue, you need to take one day at a time.
Tess: Yes.
Patrik: You need to take one day at a time. You need to expect setbacks.
Tess: Which is what I gather from what you’ve previously said, yes.
Patrik: Right. Two steps forward, one step back. Compared to last week, there has already been some improvements. She’s got a tracheostomy tube, she’s opening her eyes. Right?
Tess: Exactly.
Patrik: You look at the positives, not at the negatives. Don’t look too far in the future. We don’t have a crystal ball. We don’t.
Tess: Yes. Indeed, this whole matter, because I’ve been doing a lot of research with Rey as well. We gather that with neuroplasticity, there is enormous amount of possibility potentially for her in the future, because she’s young and that. But as you rightly say, I do appreciate your point of view. It’s on a day to day basis. We have to take it on that level.
Tess: But the possibility of her being able to get a breakthrough in terms of actually regaining consciousness and being able to eventually speak for herself, I don’t rule that out at all. I’m very much of the belief that is possible in spite of what they’re saying. I must hasten to add that to this point, even though I’ve asked for, I haven’t seen any actual visual evidence of what is being claimed in terms of MRI (magnetic resonance imaging) scans or anything.
Patrik: Yeah. I’m not ruling out that she can talk one day and that she can get back to a better quality of life. But again, it’ll be very difficult to put a timeline on that. It could be weeks. It could be months. It could be years. That’s out of your hands and out of my hands to put a timeline on that.
Tess: Is it fair to say that from what I’ve told you and also from your understanding of similar situations, that the way they’re actually treating her is more positive and more in the right direction in terms of them viewing her as potentially being able to be assisted out of this predicament. Or do you think that they could actually be trying to-
Rey: Send her in the other direction.
Tess: …send her in the other direction and make it really difficult for Sara to get out of the situation? What do you reckon?
Patrik: I tell you what the ICU’s ultimate goal is. The ICU’s ultimate goal is to get her out. Now, how can ICU get a patient out? They can either get a patient out by improving the situation to a point where she can get out or they want to move her towards end-of-life. With everything that you’ve shared so far, I can’t see that they’re moving towards end-of-life. I can’t see that at the moment.
Tess: Good. Okay. That’s a relief.
Patrik: That’s not to say it can’t come, for whatever reasons it might be. They can move toward…
Tess: Yeah
Patrik: That’s not to say they may not do that, but there are no signs at the moment. Do you remember last week? I told you, “Watch what they do, not what they say.”
Tess: Yes. Okay.
Patrik: Right. You should be paying attention to both, but you should put more weight on what they do, not what they say.
Tess: Okay. Now, with the prospect of them actually wanting to talk to me about the fact that this doctor, who in all honesty was quite pompous with me, in front of some other students or maybe younger interns. I don’t know. But the point being, she was very perfunctory. She didn’t spend much time with the nurse at all. Basically said the insulin was a necessity. When I broached the topic of the sodium valproate and the potentiality for liver toxicity, she said, “No, I think this is the one helping.”
Tess: Also, as I said, in my message to you that it’s a case of, we wish to talk to you sometime this week because we are wanting to know where it’s going to go next sort of thing.
Patrik: Yeah. I’ll tell you where I think it’s going to go. Maybe looking into the future, the goal is to get out of ICU first and foremost. The goal is to get off the ventilator. The goal is to have that tracheostomy tube removed. I can’t tell you at the moment whether that’s possible at all. I will tell you that her having a tracheostomy tube and a ventilator is an obstacle for her to go to rehab. It’s an obstacle.
Suggested Links:
Rey: But the newer hospital does say…
Tess: But the newer hospital does say in the admission, like the form…
Rey: Basically we found a form here the…
RECOMMENDED:
Tess: Yeah. Bear with me. I’m just going to pass you to Rey.
Rey: Yeah. Okay. Hello.
The 1:1 consulting session will continue in next week’s episode.
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!