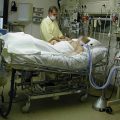
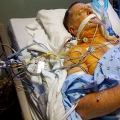
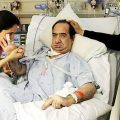
Hi, it’s Patrik Hutzel from INTENSIVECAREHOTLINE.COM where we instantly improve the lives for Families of critically ill Patients in Intensive Care, so that you can make informed decisions, have PEACE OF MIND, real power, real control and so that you can influence decision making fast, even if you’re not a doctor or a nurse in Intensive Care!
This is another episode of “YOUR QUESTIONS ANSWERED“ and in last week’s episode I answered another question from our readers and the question was
How to Have Power and Control Whilst My Ventilated Daughter is Critically Ill in the ICU?
You can check out last week’s question by clicking on the link here.
In this week’s episode of “YOUR QUESTIONS ANSWERED” I want to answer questions from one of my clients Romeo, as part of my 1:1 consulting and advocacy. Romeo’s daughter is with a breathing tube and on a ventilator in the ICU. Romeo is asking will it be safe for his daughter to undergo tracheostomy procedure even with a low hemoglobin level in the ICU.
Is it Safe for my Daughter to Undergo Tracheostomy Even with a Low Hemoglobin level in the ICU?
“You can also check out previous 1:1 consulting and advocacy sessions with me and Romeo here.”
Patrik: Hi Tess!
Tess: Hi Patrik! My daughter’s hemoglobin now is so low.
Patrik: Okay. I would be very curious to know why her hemoglobin is so low. That’s a bit of a worry for me. If people have surgery, the hemoglobin can drop. But she didn’t have surgery.
Tess: Yes, but maybe a salient, a very important point that maybe we may have missed telling you is that she’s skinny.
Patrik: Yes, that could be a reason why.
Tess: And because she has very little fat on her body at present.
Patrik: Yes.
Tess: And also, the musculature is not very well developed, especially in her upper torso and wasn’t going out very much over the period between the beginning of COVID in 2021 May when she discovered the matter in her fungal issue in her private area, which then basically set her on a path to try and sort out what she believed could potentially be diabetes or the beginning of onset diabetes through diet. And then her weight dramatically went down from 6 months after the point of her actually endeavoring on this whole journey to try and get better into 2021. So ultimately, we have Sarah in a pretty frail state, and yet still fighting for life.
Recommended:
Patrik: I see.
Tess: And she was being fed, she had access to whatever we could give her, whatever she so wished, and she still seemed to be losing weight. I don’t know whether this is incorrect rationale, but it’s almost like her metabolic system went into an overdrive.
Patrik: Yeah.
Tess: And she was fine in certain respects. Mentally, absolutely spot, real acuity, very, very clever, high-speed gamer. Extremely intelligent, focused and she was that up until about five days before the incident of the heart attack.
Patrik: Okay.
Tess: But she wasn’t as mobile as she could otherwise be, and I did encourage her to be. And as I mentioned, her gait, she was insecure about her walking, which was understandable because obviously, she didn’t have the muscle mass on her gluteus maximus and her thigh muscles.
Patrik: Yeah. Look, it’s not my area of expertise to speculate what happened prior to the event. That’s not my area of expertise. What does stand out to me is that hemoglobin is so low, considering she didn’t have surgery and I believe you may want to seek some answers there.
Tess: How could that be potentially assisted other than with the… The blood transfusions were given and they seem to think that they actually assisted. At least, that’s what I’ve gathered from the nurses.
Patrik: Oh, absolutely. In the short term, that helps. But I do believe they need to get to the bottom of it.
Tess: Right.
Patrik: So they need to find out why her hemoglobin is low in the first place. She could be anemic.
Tess: I suggested that and that wasn’t necessarily taken on board by one of the nurses anywhere at the time when I mentioned it.
Patrik: I think it’s a question for the doctors. I think it’s a question for the doctors.
Tess: So that would necessarily mean what? Low iron count?
Patrik: Low iron count. Maybe bone marrow isn’t producing. Again, that is not sort of my area of expertise.
Tess: Okay.
Patrik: But I do wonder about such a low hemoglobin without her having had surgery.
Tess: Yes and indeed. Is it even safe for her to be having a tracheostomy with that low hemoglobin count?
Recommended:
Patrik: Yes, because what they might do, they might give her another unit of blood pre-tracheostomy. They might.
Tess: So just put that down, ask about whether there’ll be another blood through transfusion.
Patrik: I’m making notes as we speak as well. I’ll send that in Skype in a minute.
Tess: I don’t worry. I was mentioning it to Rey because he can hear through the split of the same conversation that we’re having.
Patrik: Okay, great. So, the other thing is, let’s just quickly focus on the brain for a moment and what I can see happening. The Glasgow Coma Scale is 3. She is on Keppra, Phenytoin and Clobazam, which have some sedative effect. As I said, please get the doses.
Tess: Yeah. Write that down please. Doses for the Keppra.
Patrik: Doses for all of them.
Tess: Yeah.
Patrik: I am worried that she’s not coughing. I am worried about that.
Tess: Oh, she had a low coughing reflex prior to when she was in the process. Because apparently it might be esophageal related. But for simple fact is that there were particulates of food that they found and that could have precipitated the lung infection in the first place. She may have had an issue in her esophagus. And because of her low weight, that may mean that they could be interrelated the weakness of the muscle.
Patrik: Yeah. I see. Yeah. Definitely.
Tess: With all the tubing could be prohibitory to her actually doing it.
Patrik: No. I’ll tell you why.
Tess: No? Okay.
Patrik: I’ll tell you why I’m worried. So, if someone gets a breathing tube in the throat and they’re in an induced coma and then you take them out of the induced coma, assuming they don’t have a brain injury. That the first thing they do is cough because it’s so uncomfortable.
Tess: Unpleasant, yeah.
Patrik: All right. Now they’re telling you the brain stem is intact. They’re telling you that there is a significant hypoxic brain injury, but the cough reflex is the last thing to go, or it should be the last thing to go. It should be one of the first things to come back.
Tess: Right.
Recommended:
Patrik: It’s we can’t live without a cough. We just can’t. Because we would all be aspirating.
Tess: Yes.
Patrik: Right. So that is a concern to me. And you know, it may, or it may not come back. Have you seen them suction her? Have you seen that?
Tess: Yes, I have. Yes.
Patrik: Is she coughing then?
Tess: No.
Patrik: Right. That’s certainly a worry there. Because if someone shoves a suction catheter down your throat, you should definitely start coughing, you know?
Tess: But they say it seems as if he can feel discomfort when it’s going on.
Patrik: Yeah.
Tess: That was mentioned, but no coughing reflex.
Patrik: But okay. Picture this. Someone shoving a suction catheter down your throat. I mean, it’s almost impossible not to cough.
Tess: Yes.
Patrik: Look, it’s a question that needs to be raised. Where is this cough reflex? It’s a question that I think you should be asking.
Tess: Yes.
Patrik: The other thing is sort of outlook. The ventilator settings are really low, right.
Tess: Yes.
Patrik: If her blood gases are good, I would argue that if she’s hopefully getting a little bit more awake, she has a very good chance that she might be off the ventilator at least for a few hours in a few days, once she’s got the tracheostomy. I think that could be realistic. That would be a good step.
Suggested links:
Tess: Even if there isn’t necessarily tracking? Or at least there wasn’t-
Patrik: No, no. It sounds to me like she’s breathing.
Tess: Yes. Oh definitely.
Patrik: Right.
Tess: She’s triggering the machine.
Patrik: That’s right. So, that’s good. And then once she has the tracheostomy, I think there’s a waiting game.
Tess: Yes. What can I do myself whenever I can get access to her? How would be the best way other than obviously giving her as much physical contact or like stroking her hands, manipulating her hands, speaking to her directly, looking into her eyes, stroking her feet. Is there any other way you can suggest that I interact with her?
Patrik: Yep, absolutely. I would suggest that when you’re not there. I mean, when you’re there do all of what you’ve just mentioned.
Tess: Yeah.
Patrik: When, when you’re not there, you could play some music. They could put up an iPad or whatever, play some music. Maybe she could listen to your voice when you’re not there. Maybe you record something, all sorts of things.
Tess: Right. On headphones do you think? On loose headphones placed on her head, with maybe an MP3 player with some of her favorite music.
Patrik: Exactly.
Tess: Okay. So it’s potentially, it could be done either on Friday, depending. Now I’m going there. Obviously, I’ll be going there tomorrow. Do you think I should try to speak to this neurological specialist and ask her that point about the cough reflex and also the dosages as you’ve suggested and what is possible about the hemoglobin and if they’re going to do another infusion prior to..
Patrik: Yeah. I think you should be asking all of those questions for sure.
Recommended:
Tess: Yeah. And is there anything else that does occur to you that could potentially be..
Patrik: Yes. Do you know, when you’re there are they seating her up?
Tess: Yes, invariably is. And I think that given that when she was in the MRI scan, it was mentioned that she didn’t particularly like to be in a prone state. They had to up the oxygen a bit. It suggests to me that she favors that position, but they’ve got to avoid her getting bed sores, yeah. Because the lack of gluteus maximus muscle and obviously pressure on the coccyx area, which she was bearing with before the incident, but it was obviously getting a bit much at times. Prolonged sitting at the computer and everything. I imagine that they have that under control because about, I think 3days, 2 days ago, at least I verified that there weren’t any sores as such, but they’ve got that under control.
Patrik: Right. What else can you… Do you know?
Tess: I couldn’t take any photographs today because I couldn’t get to see her.
Patrik: Yeah, sure. Do you know if she’s getting any physical therapy or physiotherapy?
Tess: Yeah, none whatsoever at the moment we were going to actually say… I actually mentioned that it obviously it would be incredibly important for Sarah to get as much possible physical therapy, so that the whole thing of this potentiality for a thrombosis or something through lack of activity could be avoided. And evidently, I assume that anticoagulants, yeah. Anti what deep vein thrombosis prophylaxis that they would be used only for that purpose. And as the specialists explained, being in the position where you are not utilizing your muscles, obviously I said, yes, your lymphatic system is not being moved and it can lead to potential complications. So, movement is in incredibly important in this equation.
Patrik: This very important, very important.
Tess: When do you think that might be part of the picture in terms of.
Patrik: Well, it should be part of the picture.
Tess: Right now, as we speak?
Patrik: Absolutely.
Tess: Okay. I will mention this tomorrow as well, ask about that. Would that mean that an actual physiotherapist would come to her bedside and actually give her some form of movement, you know?
Patrik: Very much so.
Tess: And how much would you suggest on a daily basis?
Recommended:
- Quick tip for families in ICU: Cardiac arrest & hypoxic brain injury, should a tracheostomy be next?
Patrik: Well, the more the better. There’s nothing, you know. The more the better. Well, when I say the more the better, I’d say 2x a day. Morning, afternoon.
Tess: Okay. Morning, afternoon. And if that’s not actually occurring. Yeah. And I haven’t yet.
Patrik: Well, I’ll tell you what happens if it’s not occurring. Her joints will get stiff and she’ll end up with contractions.
Tess: You mean contortion of the body?
Patrik: Contractions. So basically, if you’re not moving the joints, it’s like they’re rusting.
Tess: Okay.
Patrik: It’s critically important. Picture this, picture this. You’re lying-in bed for 2 weeks, 3 weeks. And nobody’s moving your joints.
Tess: Yeah.
Patrik: There’s going to be some damage from that.
Tess: Okay. Well, I’ll be on the case on that tomorrow, and I’ll try and ascertain what is actually going on there.
Patrik: Yeah.
Tess: And if anything, actually insist that something be done if it turns out that she’s just being moved. Because you see prior to say about 5, 6 days ago, she was unstable at times from just being turned and that discouraged them.
Patrik: Yeah. It might have. It might have.
Tess: Although stability has been attained more recently.
Patrik: Yeah.
Tess: And she’s more stable than she has ever been.
Patrik: Yeah, absolutely. But there’s a difference between turning her on the side and wash her back and change linen and her lying on her back and moving her arms and legs. There’s a big difference there.
Tess: Yes. Yes. Okay. Okay. I’ll definitely be onto that tomorrow.
Patrik: Yeah.
Tess: How long after the tracheostomy, if everything goes all right with it, how long is it possible that they will maybe go through the process of trying to wean her do you think after the actual surgery?
Patrik: Just repeat, can you please repeat to me what her ventilator settings are again? So, she is in pressure support?
Rey: Ventilator settings.
Tess: Ventilator settings.
Patrik: You mentioned it earlier, pressure support of 12 or something like that. PEEP of 8.
Tess: Oh yeah. Pressure of 10. PEEP 8, 35% oxygen.
Patrik: PEEP 8, hang on. Just making some notes. Pressure support 10.
Tess: Yes.
Patrik: And oxygen 30%?
Tess: 35%. Ever so slightly risen because of the MRI situation, but it was 30.
Patrik: So that’s pretty good. So, I tell you what needs to happen, her PEEP (Peak Expiratory End Pressure) should come down to 5 ideally. Her pressure support 10, 8. What it comes down to is her volumes. What that means is her volume.
Tess: Pressure support 10.
Patrik: When she breathes in her volume should be around 400 or 500 mls.
Tess: It was at 500 mls.
Patrik: Okay.
RECOMMENDED:
Tess: Oh, that maybe that’s to do with her urine, excuse me.
Patrik: No volumes. I’m talking about breathing volumes, not talking about.
Tess: Oh, breathing volumes.
Patrik: Breathing volumes. Talking about breathing per breath with 56 kilos tissue she should be breathing 350 to 500 mil. If she’s doing that and her breathing rate is not above 30 breaths per minute. And if her gases are fine, the candidate for having time off the ventilator. So, I think it’s actually fairly close.
Tess: Okay.
Patrik: I think so.
Tess: They’re actually basically got it in hand, and they are doing the right thing. You suspect.
Patrik: That’s what I’m saying. Yeah. I do believe they’re doing the right things. The only concern is obviously the.
Tess: Hemoglobin.
The 1:1 consulting session will continue in next week’s episode
How can you become the best advocate for your critically ill loved one, make informed decisions, get peace of mind, control, power and influence quickly, whilst your loved one is critically ill in Intensive Care?
You get to that all important feeling of making informed decisions, get PEACE OF MIND, CONTROL, POWER AND INFLUENCE when you download your FREE “INSTANT IMPACT” report NOW by entering your email below!
In Your FREE “INSTANT IMPACT” report you’ll learn quickly how to make informed decisions, get PEACE OF MIND, real power and real control and how you can influence decision making fast, whilst your loved one is critically ill in Intensive Care! Your FREE “INSTANT IMPACT” Report gives you in-depth insight that you must know whilst your loved one is critically ill or is even dying in Intensive Care!
Sign up and download your FREE “INSTANT IMPACT” REPORT now by entering your email below! In your FREE “INSTANT IMPACT” REPORT you’ll learn how to speak the “secret” Intensive Care language so that the doctors and the nurses know straight away that you are an insider and that you know and understand what’s really happening in Intensive Care! In your FREE report you’ll also discover
- How to ask the doctors and the nurses the right questions
- Discover the many competing interests in Intensive Care and how your critically ill loved one’s treatment may depend on those competing interests
- How to Eliminate fear, frustration, stress, struggle and vulnerability even if your loved one is dying
- 5 mind blowing tips & strategies helping you to get on the right path to making informed decisions, get PEACE OF MIND, control, power and influence in your situation
- You’ll get real world examples that you can easily adapt to you and your critically ill loved one’s situation
- How to stop being intimidated by the Intensive Care team and how you will be seen as equals
- You’ll get crucial ‘behind the scenes’ insight so that you know and understand what is really happening in Intensive Care
- How you need to manage doctors and nurses in Intensive Care (it’s not what you think)
Thank you for tuning into this week’s YOUR QUESTIONS ANSWERED episode and I’ll see you again in another update next week!
Make sure you also check out our “blog” section for more tips and strategies or send me an email to [email protected] with your questions!
Also, have a look at our membership site INTENSIVECARESUPPORT.ORG for families of critically ill Patients in Intensive Care here.
Or you can call us! Find phone numbers on our contact tab.
If you want a medical record review, please click on the link here.
Also check out our Ebook section where you get more Ebooks, Videos and Audio recordings and where you can also get 1:1 counselling/consulting with me via Skype, over the phone or via email by clicking on the products tab!
This is Patrik Hutzel from INTENSIVECAREHOTLINE.COM and I’ll see you again next week with another update!